Published on
Urgent message: Acute or chronic hallux pain is a common complaint in urgent care. Due to the structure, several diagnoses can have similar presentation on history and exam. With this discussion, we examine a sesamoid stress injury.
Sergio P. Ramoa, MD, MS
INTRODUCTION
The tibial (medial) and fibular (lateral) sesamoids are contained within the flexor hallucis brevis tendons along the metatarsal head.1 They have several roles such as absorbing weight, helping glide and reducing friction of the tendons, and improving flexion strength. X-rays of injuries can sometimes be nonconclusive. Approximately 13.5% of the population have bipartite sesamoids—a sesamoid bone that has not fused together, leaving two separate components.2 For those that have bipartite sesamoids, 90% of them involve the medial sesamoid.1 Most of the weight transmitted to the first metatarsal is bore by the tibial sesamoid; therefore, most sesamoid pathologies are involved with the tibial sesamoid.1
CASE PRESENTATION
A 39-year-old male runner presented with a 2-month history of intermittent right foot pain, worse at the right great toe. He stated that he has had similar issues in the past that would typically resolve with rest, but return when he resumed running. The most recent exacerbation started when the pain woke him up in the middle of the night. Patient denied any history of trauma, family history of joint pathologies, or recent dietary changes. He was a social drinker with 1-2 drinks per month. There were no known dietary restrictions, but he followed a low-fat diet while avoiding sugary snacks and frequent red meat consumption.
Physical exam
- Temperature: 97.2⁰, pulse 63, BP 100/62, O2 saturation: 98%, weight 180 lbs, height: 6’1”, BMI 23.7
- Worse with off-phase of walking
- Swelling and redness on plantar side only of the metatarsophalangeal joint (MTP). Tenderness with palpation. Skin is intact
- Full range of motion and sensation
- Strength 5/5
Differential and Decision-Making
With pain starting suddenly at night and without a distinct traumatic history, gout is a concern. On exam, he lacked uniform swelling and tenderness of the joint. He also denied family history and had no recent dietary changes. His pain was only on the plantar side of the MTP joint, with worse pain during the step-off phase of walking, which would increase concern for sesamoiditis. Due to the amount of redness and swelling, an x-ray was ordered. It showed a medial sesamoid with two components. This could represent a sesamoid variant like a bipartite sesamoid, stress injury, or a fracture.
Radiologic Results/Diagnosis
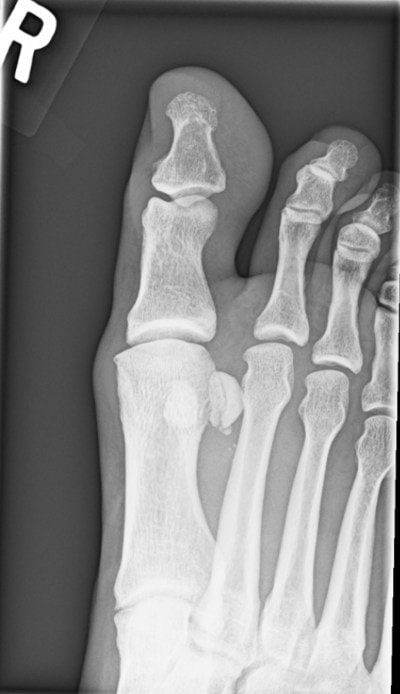
Treatment
Imaging for this patient is undiagnostic. In cases in which the exam, history, and radiology are not straightforward, MRI or isotope bone scan can better distinguish pathologies.1 Both can also determine if a sesamoid may be a bipartite vs a fracture, as a bipartite sesamoid may still present with pain due to sesamoiditis. An MRI can also differentiate between an acute and chronic stress fracture, or if diminished flow caused avascular necrosis.
Due to the patient’s history, an empiric approach was taken for stress fracture, but further imaging is still essential for determination of his pathogenesis. The first approach to an acute nondisplaced and chronic stress fracture can be conservative, nonoperative treatment. Given that the sesamoid bones’ function is to absorb weight, reduced weightbearing is an important goal. In chronic stress fractures, this can be done with orthotics displacing the weight towards the heel.3 In acute nondisplaced, immobilization and weightbearing need to be altered, such as with a cast and crutches. Activity should be modified from high- to low-impact exercises to prevent repetitive loading to the area, while maintaining physical conditioning. The stress fractures will typically heal in approximately 6 weeks, and a patient can return to normal activity only after complete healing to avoid a full fracture.4 Depending on practice type and the ability for the patient to follow up, an orthopedic referral may be reasonable at the beginning of management. With failed treatment or displaced fractures, referral to orthopedics is essential for surgical intervention. Preventive methods can also be implemented for runners (ie, decreasing total mileage, changes in terrain, avoiding hills, and replacing shoes every 6 months to maintain adequate shock absorption).4
DISCUSSION
It is important to gather information on other daily activities, new and previous shoe wear, and attempted treatments. Due to numerous pathologies of the hallux, diagnosis is not always straightforward even with an appropriate history gathered.
In this patient, the sudden pain onset did increase concern for gout, but location was solely on the base of the toe. He also tried to avoid red meats (relative risk (RR) 1.41) and fructose “sugary” snacks (RR 2.02) and drinks (RR 1.82), which would increase the risk of gout. Increased BMI can increase risk of gout, although his was within normal range.5 With these considerations from the history and exam, his risk of gout was low. Though not obtained from the patient during history, dairy and vitamin C consumption can decrease risk of gout (RR 0.56 and 0.55, respectively).5 The incidence of turf toe, or plantar capsular ligament sprain or tear, has increased with the introduction of lighter foot wears into athletic activity.2 With normal walking, the ligament complex can bear up to 60% of the body weight, increasing up to 3 times for athletic activity, and up to 8 times for running jumps.6 Hyperextension is the main cause of injury, and future arthritic changes are a greater likelihood in patients who have reduced dorsiflexion.6 Turf toe has different classifications; Table 1 presents common exam findings. Along with treatment-specific management noted in the table, initial treatment should include rest, ice, compression, and elevation.
Turf Toe Classes and Management6,7
| Classification | Findings | Management | |
|---|---|---|---|
| Class 1 | Acute sprain of the ligaments with micro-tears and without instability | Swelling Mild ecchymosis Full range of motion Able to bear weight | Heal in 1 to2 weeks Symptomatic treatment and return to play as tolerated |
| Class 2 | Partial tear of the capsular ligament | Moderate swelling Ecchymosis Restricted range of motion Painful movement Painful weight bearing | Heal in 4-6 weeks May need protected weightbearing, such as a walking boot Days 3-5, gentle range-of-motion exercises with passive plantar flexion to prevent adhesions |
| Class 3 | Complete tear of the capsule and instability | Moderate to severe swelling Ecchymosis Decreased range of motion Difficulty bearing weight Significant tenderness with palpation | Heal in 6-12 months 4-8 weeks of immobilization in a walking cast or CAM boot Progressive range-of-motion exercises after immobilization Protected ambulation with foot plate inserts or modified footwear If failed treatment, surgical intervention may be necessary |
Sesamoiditis could be a very likely cause to the patient’s symptoms, but should be a diagnosis of exclusion once other etiologies have been ruled out. He did not have a high risk of infection as his history lacked any trauma to the skin that would inoculate the sesamoids with bacteria. He also lacked a past medical history like diabetes which would increase the risk through immune suppression, poor vascularity, and peripheral neuropathy. Along the same line, no foreign body was suspected at this time due to lack of trauma, but further imaging with MRI may be able to better differentiate compared with x-ray. Due to frequent running, he could have increased risk of arthritis but x-ray did not suggest signs that would lead to an arthritic flare.
In cases in which the exam, history, and radiology are not straightforward, MRI or isotope bone scan can better distinguish pathologies.1 Compared with other etiologies for the hallux and sesamoid, which affect both sesamoids, stress fracture typically involves only one sesamoid.4 Few (0.4%) running injuries are due to sesamoid stress fractures.4
Sesamoids fractures fall into a high-risk category that can have increased complications such as: complete fracture, nonunion, delayed union, and higher likelihood of surgical intervention compared with other locations of the foot such as the 1st through4th metatarsal and calcaneus.4 Therefore, it is important to have continued monitoring for full healing of the stress injury, as well as reinforcing to the patient to not return to previous repetitive impact activities prematurely.
Take-Home Points
- First MTP pain is often not straightforward and can have several etiologies.
- MRI or isotopic bone can help differentiate among several pathogenesis of injury, as well as normal variants.
- First-step approach with fracture, stress injury, sesamoiditis, capsular injury, or arthritis is a conservative approach.
REFERENCES
- Sims AL, Kurup HV. Painful sesamoid of the great toe. World J Orthop. 2014;5(2):146-150.
- Lee DK, Mulder GD, Schwartz AK, et al. Hallux, sesamoid, and first metatarsal injuries. Clin Podiatr Med Surg. 2011;28(1):43-56.
- Silverman L. Sesamoid stress fractures. FootEducation. Available at: https://footeducation.com/sesamoid-stress-fractures/. Accessed August 4, 2021.
- Kahanov L, Eberman LE, Games KE, Wasik M. Diagnosis, treatment, and rehabilitation of stress fractures in the lower extremity in runners. Open Access J Sports Med. 2015;6:87-95.
- Roddy E, Choi HK. Epidemiology of gout. Rheum Dis Clin North Am. 2014;40(2):155-175.
- Najefi AA, Jeyaseelan L, Welck M. Turf toe: a clinical update. EFORT Open Rev. 2018;3(9):501-506.
- Aran F, Shamrock AG, Scott AT. Turf Toe. [Updated 2020 Aug 24]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; January 2020. Available at: https://www.ncbi.nlm.nih.gov/books/NBK507810/. Accessed August 4, 2021.
Author affiliation: Sergio P. Ramoa MD, MS, CareNow Urgent Care HealthONE Denver, CO.
