Published on
Urgent message: ‘Fresh eyes’ may be needed to reconsider an initial diagnosis or re-evaluate treatment in patients who present with unresolved symptoms.
Joseph Toscano, MD
The Case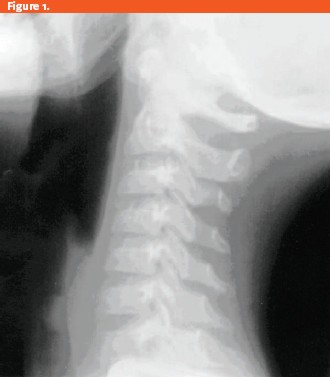
A 9-year-old boy presented to an urgent care clinic with a several-day history of dry cough and intermittently noisy and difficult breathing, especially at night.
He had no fever or chest pain, no nasal discharge or headache, and no rash or pruritis.
His past medical history included no prior diagnosis or suspicion of allergies, asthma, or other chronic respiratory problem, and no history of similar or other significant acute problems.
The boy was taking only over-the-counter cough syrup and had no medication allergies. Family history was significant for mild childhood asthma in his mother. He is not exposed to second-hand smoke.
Review of systems was negative for GI symptoms, joint pain, and weight loss.
A presumptive diagnosis of new-onset asthma was made on his first visit, and he was started on an albuterol inhaler and spacer.
He was seen several more times for persistent symptoms. Each time, the diagnosis was the same. Inhaled, then oral, steroids were added.
At the last visit four days ago, azithromycin was prescribed.
Now, he presents with a total of two weeks of slowly worsening but similar symptoms. None of the prescribed treatment has seemed to work, according to his parents.
At this visit, personal medical history, family history, social history, and review of symptoms are unchanged from above.
Upon exam, you find:
- T 98.2
- P 90
- R 20
- BP 104/62
- O2 sat 97% on room air
- General: WDWN, NAD, though mild inspiratory breath sounds are audible in general
- Head: Normocephalic, no visible abnormalities or sinus tenderness
- Eyes: Clear conjunctivae and sclerae, EOMI, PERRL
- Ears: Normal pinnae, canals, and TMs bilaterally
- Nose: No significant congestion and no FB or discharge
- Throat: No mass, infection, exudate, swelling, or erythema
- Neck: Inspiratory retractions visible across the neck and into the supraclavicular areas, but no lymphadenopathy or other masses are felt; no meningismus
- Chest: Airmovement normal bilaterally, but there are diffuse airway sounds with inspiration; no crackles or expiratory sounds
- Heart: Regular rate and rhythm without gallop, murmur, or rub
- Abdomen: No distension; soft without masses, tenderness, or hepatosplenomegaly
- Skin: No urticaria, petechiae, purpura, or other rashes
- Extremities:Warmwith good color and pulses; no joint swelling or edema
The clinician ordered a lateral soft tissue neck x-ray (Figure 1), which showed a normal epiglottis and laryngeal air column, but there was a soft-tissuemass on the anterior trachea below the larynx occupying approximately 85% of the AP diameter of the tracheal air column.
Subsequently, the patient went on to have an uncomplicated resection of the tumor, which proved to be a tracheal hamartoma.
Discussion
The purpose of this case report is not somuch to recount the clinical presentation of a fairly rare airway tumor, but to emphasize two very important issues that arise much more commonly in urgent care practice:
- The first important issue regards the often crucial physical examination distinction between whether additional respiratory sounds are occurring during inspiration or expiration.Beyond the pure semantics of the terms “stridor” and “wheezing” — they are sometimes used interchangeably — this distinction has important implications.
Due to the airway mechanics of unassisted ventilation, inspiratory sounds — usually, but not uniformly referred to as stridor — typically suggest extrathoracic airway obstruction (naso-, oro- or hypo-pharynx, larynx, trachea above the sternal notch).
On the other hand, expiratory sounds — usually, but not uniformly referred to as wheezing — typically suggest intrathoracic obstruction (lower trachea, bronchi, bronchioli).
Each engenders a separate differential diagnosis and approach to treatment and evaluation.
Wheezing is much more commonly seen and can often be treated empirically with a bronchodilator. With arranged follow-up, it is not absolutely necessary to distinguish, at the initial visit, between new onset reactive airways disease, acute infectious or allergic bronchitis, or bronchiolitis, though each should be borne in mind and discussed with the patient.However, even in the absence of respiratory distress, stridor requires definitive identification as to its cause (parapharyngeal mass or edema, allergic reaction, airway foreign body, croup, epiglottitis, etc.) to allow appropriate treatment and disposition of the patient. The degree of airway obstruction can change quickly with time, positioning, or respiratory effort and with the exception ofmost cases of croup, the causes of stridor require prompt emergency department or specialty referral.
- The second important issue involves patients who return for the evaluation of a recently diagnosed and treated complaint.In many cases, the diagnosis is indeed the same and all that’s needed is a change or intensification in treatment, but sometimes the return is due to an entirely incorrect initial diagnosis. In these situations, one should start fromt he beginning (even if he or she was the initial provider!) and focus on the chief complaint rather than any existing diagnoses.
Take-home Lesson
Every returning patient with the same complaints should be approached with extra attention rather than being considered a “slam-dunk.”

