Published on
Urgent message: Given that x-ray is a differentiating feature of “urgent care” and the current challenges in recruiting and retaining licensed RTs, a logical question for urgent care operators is the extent to which x-ray tasks can be delegated.
Alan A. Ayers, MBA, MAcc is President of Experity Consulting and is Practice Management Editor of The Journal of Urgent Care Medicine.
“The only people who can touch an x-ray machine are those who are certified to do so….”
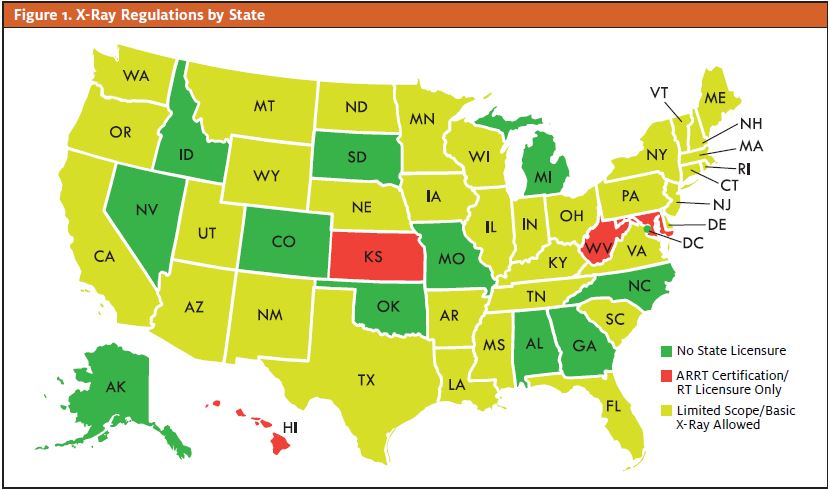
That’s what some states say to the question of who may take an x-ray at a medical facility, including an urgent care center. As a result, a physician may not delegate their certification or qualifications to a noncertified person. Nearly all states require a licensed radiologic technologist (RT) to take x-rays and prohibit others from doing so.1 In fact, only a handful of states (see Figure 1) do not impose any regulatory restrictions in this area.2
Here, we explore the rules concerning who may use an x-ray machine to take images, as well as some thoughts on common sense solutions to the issue.
BACKGROUND
To obtain a license, a prospective RT must have a 2-year (Associate’s) degree (prescribed curricula) and pass the American Registry of Radiologic Technologists’ national certification exam.3
RTs learn multiple modalities, including CT, MRI, fluoroscopy, and mammography; however, in urgent care, they only utilize basic x-ray.3 Radiographers must also maintain a high degree of accuracy in radiographic positioning and exposure technique, and maintain knowledge of radiation protection and safety. Due to the fact that only about 10% to 15% of urgent care patients require an x-ray, there’s an insufficient amount of volume to keep an RT busy full-time. As a consequence, RTs are expected to also serve as medical assistants. Medical assisting is a lower skill at a lower wage. It’s a physically demanding job that many RTs do not care to do. A trained RT would rather work in a facility, such as a hospital, where their entire skillset can be utilized.
THE ISSUE
The limited number of x-rays taken in urgent care facilities creates high turnover and hinders the operator’s ability to easily hire RTs. A shortage of RTs that predated the pandemic has exacerbated the problem.4
Because of this, many urgent care centers are put in a situation where they’re unable to offer x-rays altogether or on certain days of the week, which strips them of their “value add” of keeping patients out of the ED as well as their competitive differentiation over a primary care office or a retail clinic—neither of which typically have x-ray capabilities. Lack of x-ray capability can also delay important diagnoses, inconvenience the patient, and diminish the provider’s diagnostic confidence.
LOGICAL SOLUTIONS
Physicians are permitted to take x-rays in many states, which is the best solution for the independent, physician-owned urgent care. But increasingly, urgent care centers are staffed by physician assistants and nurse practitioners. Because of this, the most logical solution would be to allow PAs and NPs to take x-rays. It stands to reason that if a physician can take x-rays, and if a PA or NP can practice within the scope of the supervising physician’s practice (or, in some states, independently), with appropriate training, an NP or PA should likewise be allowed to take x-rays.
At this point, states have said that a PA or NP can perform whatever procedures a physician can do unless otherwise prescribed. Therefore, if a state, such as New York, states that “only licensed practitioners or licensed radiologic technologists, may position patients, set techniques or apply radiation to patients,” a PA or NP cannot take an x-ray.5 In fact, New York state regulations provide:
Nurses, nurse practitioners, secretaries, receptionists, physician assistants, medical assistants, or respiratory therapists may NOT position patients, move the x-ray source, set techniques, or expose patients unless they are licensed and currently registered as radiologic technologists with this Department.5
Limited Scope X-Ray
Many states provide for a “limited scope x-ray technician” or “basic x-ray machine operator” certification with lesser requirements than a fully certified RT. The American Society of Radiologic Technologists defines limited x-ray machine operator (LXMO) as “an individual other than a radiologic technologist who performs diagnostic x-ray procedures on selected anatomic sites. LXMOs have a different scope of function in radiology and the types of exams they are permitted to perform.6 This person could satisfy the need in urgent care centers. Owners could staff an LXMO and pay the person less than a licensed RT. This person could also assist with other functions in the urgent care.
However, some states, such as Illinois, an LXMO may require an RT to work under a physician’s supervision.7 This restricts their use in centers that are staffed by PAs and NPs. In addition, some states limit the parts of the body of which a limited radiologic technologist can take an image.8
Video Supervision and Telemedicine
Another solution is that an RT could oversee a medical assistant by video. In effect, the medical assistant would be the “hands” of the remote RT.9 Such a model has been considered, and was used in some circumstances during the pandemic.
The American College of Radiology’s CT and MR Accreditation Program requirements specify that the supervising physician is responsible for ensuring that a physician is present and immediately available when intravascular contrast material is administered to patients. However, on March 31, 2020 CMS issued an Interim Final Rule that, among other provisions, temporarily modified CMS direct supervision requirements in certain circumstances. The rule stated that “the virtual presence of the physician through audio/video real-time communications technology will be allowed during this emergency period when use of such technology is indicated to reduce exposure risks for the beneficiary or health care provider,” provided the administration is done in communication with an immediately available technologist, nurse, or advanced practice provider.10
It is possible to configure an x-ray machine remotely. However, as a matter of safety and to limit radiologic over-exposure, manufacturers install a manual switch to create the actual x-ray exposure. As a result, even if a medical assistant could position a patient based on the remote RT’s instruction, the MA would still be required to operate the machine. But again, states lay out the duties of the RT which involve physical (hands-on) positioning of the patient, and these duties cannot be delegated and cannot be performed over video.11
This “TeleRT” model would allow performing remote x-ray procedures with the licensed technologist off site and the medical assistant being directed via video link by the x-ray technician.12 As one author noted:
“The delivery of medical services through digital devices is increasing during the novel coronavirus pandemic as doctors, patients and insurers embrace the opportunity to deliver and receive healthcare remotely. With widespread adoption, we can expect that telehealth is now a bedrock of medical care.’’13
REGULATORY CHANGES
The most obvious answer to this issue is to change the laws and regulations to allow limited scope x-ray technicians to work in urgent care centers without direct physician supervision.
There is precedent for relaxed standards in the COVID-19 pandemic. In fact, such action has been contemplated for decades.14
The National Institutes of Health noted that regulators and payers rapidly lowered implementation barriers to telemedicine-related services during the pandemic.14 A New York court said “[s]ome latitude may be accorded an administrative agency in areas where scientific or other specialized knowledge is required for action.”15
Legislative advocacy can bring about a change in lawmakers’ perspective. Education and greater awareness of the issue can help lawmakers understand this important issue.
CONCLUSION
A specific change for urgent care scenarios would be significant, and yet it is not a great departure from what has been allowed in the past in particular circumstances. Given the success of telemedicine during the pandemic, there are really no obstacles to instituting this change for x-rays in urgent care centers.
For More Information on the Logistics of X-Ray in Urgent Care
In the December issue of JUCM we will present a detailed analysis of Limited Scope X-Ray Certification in the context of urgent care. In addition, our website will feature a state-by-state summary specifying respective regulatory authorities and the status of full RT licensing requirements, as well as Limited Scope procedures and licensing requirements. Watch for more on that in JUCM News.
REFERENCES
- See Buchanan v. Dept of Health, 322 So. 3d 238, 239 (Fla. DCA 2021). Commonwealth v. Kattupalli, 221 A.3d 238 (Pa. Super. Ct. 2019).
- American Society of Radiologic Technologists. Individual state licensure information. Available at: at https://www.asrt.org/main/standards-and-regulations/legislation-regulations-and-advocacy/individual-state-licensure. Accessed October 5, 2022.
- American Society of Radiologic Technologists. Education requirement. Available at: https://www.Arrt.Org/Pages/Earn-Arrt-Credentials/Initial-Requirements/Education-Requirement. Accessed October 5, 2022.
- Carestream. Filling the gaps in radiographer staffing shortages. Carestream. October 19, 2021. Available at: https://www.carestream.com/blog/2021/10/19/filling-the-gaps-in-radiographer-staffing-hortages/#:~:text=There%20was%20a%20shortage%20of,and%20Staffing%20Survey%20(1). Accessed October 5, 2022.
- Snyder R. Unlicensed operators of x-ray equipment.New York Bureau of Environmental Radiation Protection, New York Department of Health. December 1, 2021. Available at: https://www.health.ny.gov/environmental/radiological/radiation_safety_guides/docs/unlicensed_operator.pdf. Accessed October 5, 2022.
- Modern Technology School. Find out why the limited scope x-ray technician program at modern technology school offers the most value for your tuition! Available at: https://mtschool.edu/limited-scope-x-ray-technician-program/. Accessed October 5, 2022.
- Ill. Admin. Code § 401.20.
- Iowa Department of Public Health, Bureau of Radiological Health. Limited Radiography Training Manual. 2022. Available at: https://idph.iowa.gov/Portals/1/userfiles/249/Limited_Training_Manual_2022.pdf. Accessed October 5, 2022.
- Reed Smith. Will virtual direct supervision continue beyond the end of 2022? Available at: https://viewpoints.reedsmith.com/post/102hbl2/will-virtual-direct-supervision-continue-beyond-the-end-of-2022. Accessed October 5, 2022.
- American College of Radiology. Direct supervision for contrast studies. Available at: https://www.acraccreditation.org/-/media/ACRAccreditation/Documents/MRI/COVID—MR-CT-SUPERVISION-MSD-4-9-2020.pdf. Accessed October 5, 2022.
- National Institutes of Health. Telemedicine: progress made during pandemic offers chance for widespread adoption. Available at: https://heal.nih.gov/news/stories/telemedicine. Accessed October 5, 2022.
- Mills EC, Savage E, Lieder J, Chiu ES. Telemedicine and the COVID-19 Pandemic: Are We Ready to Go Live? Adv Skin Wound Care. August 2020. Available at: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC7342801/. Accessed October 5, 2022.
- Dubauskas J. What is telemedicine, and how has it evolved during the pandemic? Forbes. December 7, 2020. Available at: https://www.forbes.com/sites/forbesbusinessdevelopmentcouncil/2020/12/07/what-is-telemedicine-and-how-has-it-evolved-during-the-pandemic/?sh=4120dfa62deb. Accessed October 5, 2022.
- Avadhanula S. Telemedicine during the COVID-19 pandemic – and beyond. U.S. News. July 2, 2020. Available at: https://health.usnews.com/health-care/for-better/articles/telemedicine-during-the-covid-19-pandemic-and-beyond. Accessed October 5, 2022.
- See Chiropractic Assn. of N.Y. v Hilleboe, 12 NY2d 109, 187 NE2d 756, 237 NYS2d 289 1962).
Acknowledgment: This article was reviewed by Ron Boucher, MD, FACR, Chief Medical Officer, Experity Teleradiology.
Alan A. Ayers, MBA, MAcc is President of Experity Consulting and is Practice Management Editor of The Journal of Urgent Care Medicine.
View More Articles
- What Qualifies Someone to Take X-Rays in the Urgent Care Center? It Depends on Where You’re Located – RT Table
- The Implementation Of Nurse-Intiated Ankle And Foot X-Rays In An Urgent Care Setting

