Published on
Improving antibiotic stewardship was an industry-wide mandate even before a 2018 study indicated that urgent care appeared to be more likely than other settings to overprescribe for common infections. While the methodologies could be questioned, especially in their take on the nature of urgent care visits, the point was well taken. Since then, urgent care as a whole has sought to improve providers’ prescribing habits more aggressively than ever.
The initial awareness campaigns did a great job of raising the profile of the issue, but actually seeing results has taken more time—and, more to the point, focus. Really making an effort to get urgent care providers to take note requires a concentrated effort. Emerging data suggest that it may not take much more than that to change the curve.
A study published by JAMA Network Open is an excellent, and very timely, example.1 Researchers found, at baseline that 48% of 493,724 urgent care encounters with patients who
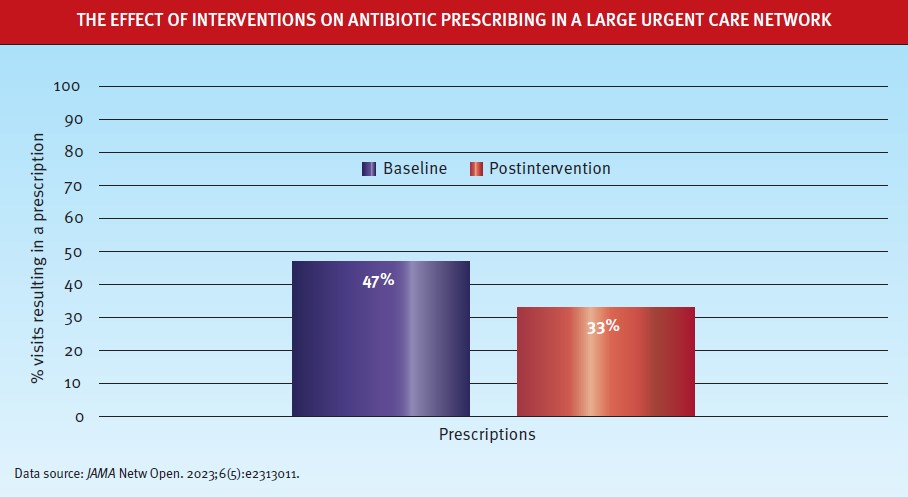
had a respiratory condition resulted in an antibiotic prescription. As the figure below illustrates, over the following year, interventions (provider and patient education; electronic health record tools; a transparent clinician benchmarking dashboard; and media) succeeded in lowering that figure to 33%. Perhaps most impressive is how quickly, prescribing behavior was changed: Prescription rates fell 22% early on and continued to fall 5% per month throughout the 1-year intervention period.
As the authors wrote: “This study’s findings suggest that a multifaceted antibiotic stewardship initiative was associated with reduced antibiotic prescribing for UC respiratory conditions, and that such initiatives in large UC networks may decrease inappropriate antibiotic prescribing.”
Reference
- Stenehjem E, Wallin A, Willis P, et al. Implementation of an antibiotic stewardship initiative in a large urgent care network. JAMA Netw Open. 2023;6(5):22313011.