Published on
Urgent message: Pharyngitis is a common chief complaint in urgent care, but not all sore throats are streptococcal (strep) pharyngitis. Delayed diagnosis and treatment of some causes of sore throat can lead to catastrophic outcomes.
Epidemiology
Acute pharyngitis accounts for 1%-2% of all visits in the ambulatory setting.1 Most pharyngitis seen in urgent care is viral in etiology. The most common bacterial cause of pharyngitis is group A beta hemolytic Streptococcus (GABHS), which is responsible for 5%–15% of visits for sore throat in adults and 20%–30% in children.2
Case
An otherwise healthy 28-year-old man presented to urgent care after several days of fever and sore throat that worsened with swallowing, leading to decreased oral input. He denied any sick contacts. He was seen a few days prior and had a negative influenza and rapid strep test. He had been given a prescription for amoxicillin at the initial visit due to concern for strep pharyngitis but his symptoms did not improve.
Physical Exam
The patient was well appearing but visibly uncomfortable. His throat exam revealed erythema with tonsillar exudates bilaterally. The tonsils were swollen bilaterally, somewhat worse on the right. No uvular deviation was noted. He had no stridor, difficulty breathing, or drooling. The remainder of his exam was normal. Lungs were clear without wheezing, heart had a regular rate and rhythm without murmur, and abdomen was soft and nontender.
Urgent Care Management
The patient was referred to the local emergency department due to concerns for peritonsillar or retropharyngeal abscess based on the degree of swelling.
DIFFERENTIAL DIAGNOSIS FOR ACUTE PHARYNGITIS
Viral Pharyngitis
Viruses are the most common cause of pharyngitis. In addition to sore throat, patients commonly also experience cough, low-grade fever, conjunctivitis, and general malaise. Physical exam will often show an erythematous oropharynx.
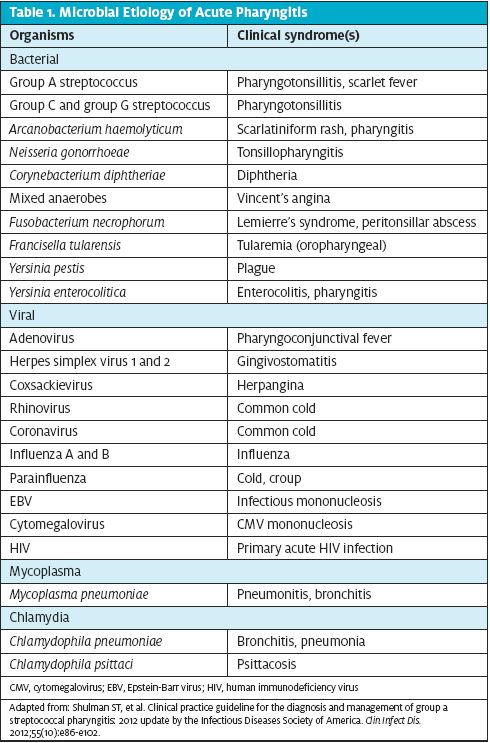
Viral pharyngitis is more likely if there is no tonsillar exudate, drooling, stridor, tonsillar asymmetry or palatine petechiae. Diagnosis is clinical. Common viruses causing pharyngitis include rhinovirus, adenovirus, and coronavirus. A more detailed list of viruses related to pharyngitis can be found in Table 1.2 No testing or antibiotics are necessary; however, GABHS testing is reasonable depending on severity of pharyngitis relative to other symptoms. The condition is self-limited with supportive care alone.
GABHS (ie, Strep Pharyngitis)
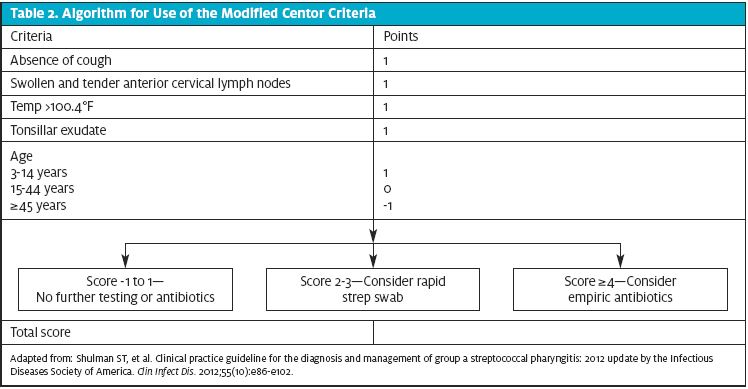
GABHS pharyngitis is most common in children and young adults. It is rare in children <3 years of age and adults >40 years of age. Signs and symptoms of strep pharyngitis include sore throat, fever, tonsillar swelling, tonsillar exudate, cervical lymphadenopathy, and lack of cough (known collectively as the Centor criteria). The modified Centor criteria includes the patient’s age. (An algorithm for use of the modified Centor criteria can be seen in Table 2.) Palatine petechiae are uncommon, but when present this finding is 95% specific for GABHS.3
A rapid antigen detection test (RADT) to confirm strep pharyngitis is recommended. RADTs have high specificity for group A strep. It is unnecessary to obtain throat culture on positive RADT due to their high specificity. In low- risk populations (ie, older adults), a negative RADT does not require confirmatory culture because the incidence of GABHS in adults is quite low.2 Pediatric patients less than 3 years of age are unlikely to have strep pharyngitis and have a low likelihood of complication if diagnosed. Thus, it is not recommended to routinely swab children younger than 3 unless they have direct contact with an individual who has been diagnosed with GABHS.
It is almost always appropriate to treat positive RADTs or throat cultures with antibiotics. Strep pharyngitis is most often benign and even more likely to be so if identified and treated. When left untreated, patients are at higher risk for certain complications such as peritonsillar abscess, retropharyngeal abscess, cervical lymphadenitis, and mastoiditis. Acute rheumatic fever and post-streptococcal glomerulonephritis can occur following resolution of the pharyngitis. While relatively rare, these conditions are thought to be secondary to immune response and not directly due to strep infection.4
Although most causes of pharyngitis in the urgent care center will be either viral or GABHS-related, the following etiologies should be included in the differential:
- Peritonsillar Abscess (PTA)
Peritonsillar abscesses occur most commonly in teenagers and young adults <40 years of age, with GABHS being the most common etiology. Signs and symptoms of PTA include unilateral sore throat, fever, painful swallowing, and when advanced, difficulty opening the mouth (ie, trismus), and voice changes. Physical exam findings can be similar to strep pharyngitis, but may be differentiated with the presence of drooling, muffled voice (AKA “hot potato voice”), and contralateral uvular deviation. PTA can generally be diagnosed clinically without imaging. When there is diagnostic uncertainty, imaging such as soft issue CT of the neck with IV contrast or ultrasound can help confirm the diagnosis and differentiate from other causes.5,6 The gold standard for confirmation (and treatment) is purulent fluid removal on needle aspiration.
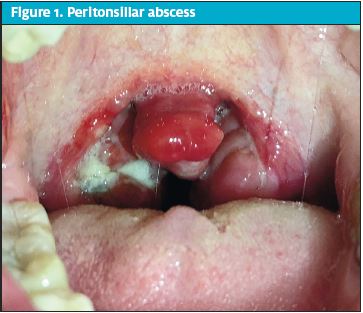
Left untreated, PTA can lead to respiratory compromise or hemorrhage from necrosis into the carotid sheath. Treatment is generally drainage of the PTA with either needle aspiration, incision and drainage, or immediate tonsillectomy. Patients should be treated with systemic corticosteroids such as prednisone and antibiotics such as amoxicillin/clavulanate, clindamycin, or second- or third-generation cephalosporins. Patients with mild symptoms, no trismus or airway compromise, or small abscesses may be able to be treated with only antibiotics.7
- Retropharyngeal Abscess (RPA)
Retropharyngeal abscesses develop in the potential space retropharyngeally in the posterior pharynx. Due to the location of these abscesses, RPA can be difficult to distinguish from other causes of a sore throat. Additionally, the physical exam on these patients may be completely normal other than subtle posterior pharyngeal bulging.
RPAs are most common in toddlers and school-age children. They are often preceded by a recent upper respiratory infection or trauma. The presentation of RPA is often similar to PTA. Unique findings on exam that should lead to concern for RPA include neck stiffness and muffled voice. Refusal to extend the neck is a concerning finding on exam and should heighten suspicion in an appropriately aged child for RPA.
CT scan of the neck with IV contrast is the preferred imaging modality for evaluation and diagnosis. As with PTA, early recognition and treatment are crucial. Patients who present with concern for airway compromise due to RPA may require a definitive airway. These patients should be emergently transferred to the ED by EMS, as management will require incision and drainage by an otolaryngologist. Consideration for starting antibiotics is reasonable but should not delay referral to a nearby ED.
Whereas the conventional thought has been that all peritonsillar abscess diagnoses should receive incision and drainage, several recent studies have shown that oral antibiotic therapy may be equally effective for small or early PTA.7
- Mononucleosis
Mononucleosis, more commonly known as “mono”, is usually caused by the Epstein-Barr virus. The spread is primarily through saliva. Mono is primarily a disease of adolescence.
Patients with mononucleosis typically present with fever, sore throat, lymphadenopathy, and significant fatigue. The presence of hepatosplenomegaly should be assessed on exam.
Diagnosis of mononucleosis is typically based on clinical evaluation and a heterophile antibody test (AKA Monospot). Treatment is supportive and antibiotics are not recommended.
Patients should be advised not to share drinkware or toothbrushes, or kiss others while symptomatic to prevent spread. Patients should also be advised to avoid contact sports or potentially injurious activities due to increased risk of splenic rupture.
Patients with mononucleosis started on antibiotics, such as amoxicillin, may present with a maculopapular rash due to hypersensitivity reaction, which generally starts a few days after initiating the antibiotics; this may occur up to 95% of the time.8 If this occurs, the antibiotics should be discontinued. The rash is self-limited.
- Epiglottitis
Epiglottitis describes a condition of inflammation and edema of the epiglottis. It was previously commonly caused by H influenza type B. Since the advent of the HiB vaccine it is now much rarer in children. Adults are now affected with epiglottitis more often than children.
In addition to sore throat, patients will commonly be leaning forward and drooling as swallowing becomes progressively more difficult. A muffled voice is also commonly observed.
Findings suggestive of epiglottitis can be seen on a lateral neck x-ray. However, CT scan or direct visualization of the epiglottis with laryngoscopy are more sensitive (although rarely feasible in urgent care).
Encouraging a patient with suspected epiglottitis to remain calm is important because agitation and anxiety can worsen airway obstruction. The patient may require intubation to ensure their airway stays patent; however, intubation should be performed in the most controlled setting possible to minimize risk of failure.9 Once an airway has been established, antibiotic therapy is the next priority. This is an emergent diagnosis and early recognition is extremely important to minimize risk of airway occlusion.
- Thrush
Thrush is a fungal infection of the oral cavity and/or the esophagus. It is most commonly caused by Candida species of yeast. Thrush most commonly affects patients with corticosteroid inhaler use, dentures, recent antibiotic use, HIV, diabetes other immunocompromised states.10 Patients may complain of a sore throat and difficulty swallowing, and may also notice white plaque on their tongue or posterior oropharynx. Thrush is primarily a clinical diagnosis. The exam will reveal white plaques on the tongue that can be scraped off. The mainstay of treatment is antifungals. For mild-to-moderate cases, antifungals, such as nystatin, can be applied to the oral cavity alone. For more severe cases or patients with esophageal candidiasis, systemic fluconazole is recommended.
- Gonococcal (GC) Pharyngitis
There are 820,000 cases of gonorrhea per year in the United States.11 It can be transmitted by different routes, including orally. GC pharyngitis is predominantly a disease affecting men who have sex with men (MSM) and is increasing,12 but it can occur in other individuals practicing receptive oral-genital sex. Patients may have mild or no symptoms and the presentation may be difficult to distinguish from other infections, such as GABHS. Signs of infection elsewhere including the rectum, vagina, or urethra with a suggestive sexual history of risk should raise suspicion for GC pharyngitis. Testing for GC pharyngitis involves swabbing the posterior pharynx and sending for PCR. Patients with concern for or confirmed GC pharyngitis should receive ceftriaxone 250 mg IM as well as azithromycin 1 g orally due to increasing GC resistance to cephalosporins.11 Patients should also be tested for chlamydia, syphilis, and HIV and counseled about safe sex practices.
- Diphtheria
Diphtheria is an extremely rare cause of pharyngitis in the United States with only two cases reported from 2004-2017,6 but occurs in other locations around the world with 7,100 cases reported in 2016. The mortality rate is significant (5-10%) and approaches 20% in those <5 years of age and the elderly.6 Diphtheria is characterized by fever, sore throat, cough, and development of pseudomembranous plaques on the posterior oropharynx which appear as a thick gray coating that can be extensive enough to create airway compromise. Treatment for diphtheria involves administration of Diphtheria antitoxin as soon as the diagnosis is suspected.13 The CDC recommendations for antibiotic therapy are erythromycin or penicillin.6
OUTCOME OF CASE
Upon arrival to the emergency department, the patient was given a dose of ampicillin/sulbactam and dexamethasone IV. A CT with IV contrast showed an early peritonsillar abscess. After discussion with ENT, He was discharged on amoxicillin/clavulanic acid.
CONCLUSION
When a patient presents to urgent care with a sore throat, the most likely etiologies are viral or GAS; however, it is important to maintain a broad differential including PTA, RPA, epiglottitis, mononucleosis, thrush, gonococcal pharyngitis, and diphtheria, as several of these causes can be life-threatening if the diagnosis is missed. Patients requiring imaging or emergent management should be referred to the ED; 911 should be activated if there are concerns for airway compromise. When indicated, antibiotic treatment should be geared toward reducing already-low risk for secondary infection and decreasing risk of spread and symptoms duration.
REFERENCES
- Schappert SM, Rechtsteiner EA. Ambulatory medical care utilization estimates for 2006. Natl Health Stat Report. 2008 Aug 6 (8):1-29.
- Shulman ST, Bisno AL, Clegg HW, et al. Clinical practice guideline for the diagnosis and management of group a streptococcal pharyngitis: 2012 update by the Infectious Diseases Society of America. Clin Infect Dis. 2012;55(10):e86-e102.
- Choby BA. Diagnosis and treatment of streptococcal pharyngitis. Am Fam Phys. 2009;79(5):383-390.
- Centers for Disease Control and Prevention. Group A Strep. Available at: https://www.cdc.gov/groupastrep/diseases-hcp/strep-throat.html. Accessed February 29, 2020.
- Steyer TE. Peritonsillar abscess: diagnosis and treatment. Am Fam Phys. 2002;65(1):93-97.
- Battaglia A, Burchette R, Hussman J, et al. Comparison of medical therapy alone to medical therapy with surgical treatment of peritonsillar abscess. Otolaryngol–Head Neck Surg. 2018;158(2):280–286.
- Souza DLS, Cabrera D, Gilani WI, et al. Comparison of medical versus surgical management of peritonsillar abscess: a retrospective observational study. Laryngoscope. 2016;126(7):1529-1534.
- Luzuriaga K, Sullivan J. Infectious mononucleosis. N Engl J Med. 2010;362:1993-2000.
- Epiglottitis: Airway management. OpenAnesthesia. Available at: https://www.openanesthesia.org/epiglottitis_airway_management/. Accessed May 1, 2020.
- Gonsalves WA, Chi AC, Neville BW. Common oral lesions: part I. Superficial mucosal lesions. Am Fam Phys. 2007;75(4):501-506.
- Centers for Disease Control and Prevention. Gonococcal infections in adolescents and adults. Available at: https://www.cdc.gov/std/tg2015/gonorrhea.htm. Accessed October 8, 2020.
- Hook EW 3rd, Bernstein K. Kissing, saliva exchange, and transmission of Neisseria gonorrhoeae. Lancet Infect Dis. 2019;19(10):e367-e369
- World Health Organization. Operational protocol for clinical management of diphtheria. Bangladesh, Cox’s Bazar. Version 10, Dec 2017.
Colin Johnson, DO, PGY-3 is an emergency medicine resident at Adena Regional Medical Center. Evan Johnson, OMS-III is a student at Des Moines University College of Osteopathic Medicine. The authors have no relevant financial relationships with any commercial interests.
