Published on
Urgent message: Odontogenic infections can pose life-threatening risk when swelling occurs in close proximity to the airway. It is essential that the urgent care provider is able to differentiate cases of relatively straightforward infection that can be managed in the urgent care setting vs true airway emergencies.
Amandeep Kaur Bains, BDS(Hons) MFDS RCPS (Glasg); Awais Safdar Ali, BDS MJDF RCSEng; and Pavan Padaki, BDS, MFDS RCPS (Glasg), MBChB, MRCS, FRCS (OMFS)
INTRODUCTION
While odontogenic or “dental” infection is a subject scarcely covered in medical training, dental-related presentations worldwide are on the rise. In the U.S., for example, dental visits account for up to 3% of visits to emergency rooms.1 This paper aims to educate urgent care providers on the management of odontogenic infections which, although still relatively rare, can pose a life-threatening risk when in close proximity to the airway. Differentiating emergent cases requiring immediate consultation from those that are either non-odontogenic or that can be managed on an outpatient basis is a frequent challenge in all acute care settings.

PATHOPHYSIOLOGY
The majority of dental infections arise from dental caries which can penetrate the outside enamel and inner dentine to enter the blood supply in the pulp chamber, causing acute dental pain, called pulpitis. The patient will describe a severe throbbing ache which is difficult to locate. Commonly, the patient will not show systemic signs of spread such as swelling or sepsis symptoms; pain management will be sufficient in these cases.3 Paracetamol and nonsteroidal anti-inflammatory drugs will be the first line of treatment.
If not treated in short order, pulpitis can progress into the alveolar bone surrounding the tooth, forming a periapical abscess (Figure 1). The patient will find the tooth tender to bite on; the precise source of the pain becomes easy to locate due to the confined area in which the abscess resides.4 This phase can last from a few weeks to a few months.
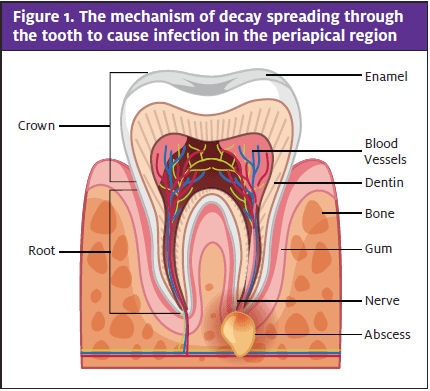
Left unresolved, the subsequent infection can break through the cortical plate of the jaw, allowing bacteria to enter the fascial planes. This is often when patients present with facial swelling and systemic signs.4
The extent and spread of infection depend on the source. Infections arising from the lower teeth can spread to the sublingual and submandibular/submental spaces, as well as to the parapharyngeal space and mediastinum. There is a risk of airway compromise with these infections due to the swelling of the parapharyngeal/paraglottic spaces leading to narrowing of the airway. Upper arch dental infections can lead to buccal space abscess, or canine space abscess, which can cause periorbital cellulitis. In rare cases, this can cause cavernous sinus thrombosis and visual loss.5
CLINICAL CASE
A middle-aged man presented with facial and neck swelling. He reported feeling unwell and was not talking in a coherent manner. His other chief complaint was a toothache of 2 days’ duration. He had not visited a dentist in over 3 years. His oxygen saturation had begun to deteriorate.
Immediate Assessment
As always, approach the patient with the ABCs. The airway may be threatened by the elevation and posterior displacement of the tongue, as well as parapharyngeal/paraglottic swelling and edema.
Airway compromise can be assumed when a patient situates himself in a sitting position with the face looking down, drooling saliva, using accessory muscles, and unable to form a single sentence in one breath. In addition to stabilization measures, this should prompt an immediate request for consultation due to the severity of the case. In cases of Ludwig’s angina, which is explained later, intubation may be required with aid from anaesthetics. At this point, a stat dose of dexamethasone 8 mg can aid in reducing the edematous swelling.
Dental abscesses can become septic. Often, treatment is IV antibiotics and IV fluids, with oxygen high flow to maintain target saturations. Taking blood cultures, lactate, FBC, urea and electrolytes, and C-reactive protein along with hourly urine output monitoring is strongly suggested.
TAKING THE HISTORY
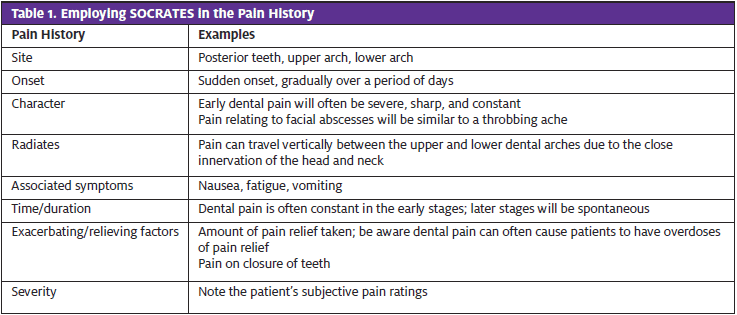
The history can help to determine the source of the pain and whether a collection has started to form. To begin, take a pain and swelling history; SOCRATES is a popular mnemonic that can be helpful for the pain history (Table 1). Patients presenting with dental pain will likely be able to locate the pain in the dental arch, but asking Where does it hurt to bite? can help locate the causative tooth.
A patient presenting with gradual-onset pain that suddenly worsens suggests an acute exacerbation of a chronic dental infection. Any patient presenting with sudden-onset toothache with no obvious swelling needs to seek help from an emergency dentist.
Facial swelling of <24 hours duration is likely to be edematous in nature, whereas longstanding facial swelling may have a collection of exudates which requires drainage.
Patients may be alarmed by sudden swelling upon waking; however, this edema may be due to the patient being supine for a long period of time. It is important to identify any history of previous treatment carried out on the dentition or oral cavity, including dental treatments, previous drainage, and prescription of antibiotics. Lastly, identifying the most recent dental visit and the patient’s ability and willingness to follow up with a dentist following their visit can help in determining the next steps.
Following a detailed history, the physician should have a good idea of whether the cause of infection is odontogenic, and thus initiate further assessment if needed.
CLINICAL ASSESSMENT
Begin with the extra-oral examination. Evaluate surrounding structures to detect the severity and, hopefully, rule out Ludwig’s angina.7 Look at the patient straight-on and assess for asymmetry and the location of the swelling. Then stand behind the patient and feel the border of the mandible down to the neck, assessing for unilateral/bilateral swelling and the border of the mandible.
Assessment of the facial swelling location and a relationship to any adjacent or affected structures should be noted. For example, inability to palpate the lower border of the mandible indicates a collection in the submandibular space. Closure of the eye due to swelling of the cheek is usually due to a canine space infection wherein the culprit tooth is located in the maxillary arch; very rarely, these can lead to vision compromise if the orbital septum is violated.
Often, especially to less-experienced providers, buccal space abscesses can masquerade as a submandibular abscess. If the swelling is above the border of the mandible, it is likely to be a buccal space abscess, as opposed to a submandibular abscess. Further examination of the swelling through bimanual palpation can aid in assessing the consistency and extent of the swelling. Swelling which indicates a collection of pus can be fluctuant in the early stages and progress to firm due to pressure.7,9 The site of swelling can also indicate the risk status, with those located in the submandibular and submental regions posing a greater risk due to proximity to the airway.
Evaluate the opening of the mouth. Trismus occurs due to submandibular, submasseteric, or medial pterygoid space abscesses as well as Ludwig’s angina. Differentiation between true and pain-related trismus through physical manipulation of the jaw adds to the clinical significance of the case. Any reduction in the normal range of the mouth opening (between 35 mm and 55 mm) may indicate fascial space infection.8
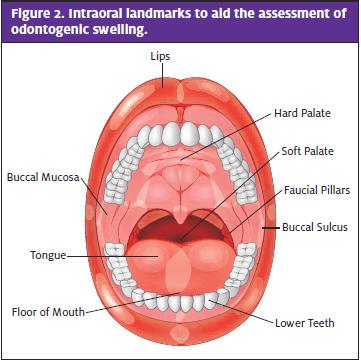
Through palpation of the floor of the mouth, tongue movements, swallowing difficulties, and drooling, the intra-oral examination offers vital information to aid the assessment of airway risk.9 This can be achieved with one digit, looking for tenderness, firmness, and swelling and comparing with the contralateral normal floor of the mouth. The buccal sulcus (the space between the teeth and the buccal mucosa) is assessed next for obliteration of the sulcus, as this in isolation indicates a buccal space abscess. Note if there is swelling of the faucial pillars, soft palate, and the uvula (Figure 2). The provider can often identify frank decay or broken teeth, which can be a strong indicator of odontogenic infection.
Initial Urgent Care Examination
In the absence of red flags, imaging with plain radiography is preferable to CT, which has been found to be overutilized in assessment of odontogenic infection.10 Radiolucency around the apices of the teeth can indicate accumulation of granulation tissue, thus clearly indicating an infection of odontogenic origin.11
RED FLAGS FOR EMERGENT REFERRAL
Any sign of sepsis, including pyrexia, tachycardia, tachypnoea, or increased white blood cell warrants a referral to maxillofacial surgeons.12 Dysphagia will also require a second opinion; a red flag for referral will be an inability to swallow liquids and drooling.7,9 Children with facial swelling will also warrant a second opinion, as infection in these patients can exacerbate quickly.
As mentioned previously, submandibular/submental abscesses in close proximity to the airway will need close review. In these cases, it is often preferable to surgically drain earlier. A warning sign will be the spread of infection past the midline; this will indicate the collection is spreading along the fascial planes. Immunocompromised patients will have a reduced ability to clear the dental infection and will often deteriorate faster and, therefore, may need admission.
Ludwig’s Angina
Ludwig’s angina is rapidly progressing cellulitis and bilateral edema of the submandibular, submental, and sublingual spaces. This poses an immediate risk for upper airway obstruction and requires immediate action.7,13 The primary site of origin is the submandibular fascial spaces, causing spread to the sublingual and submental spaces. Symptoms can include pain, swelling, elevation of the tongue, inability to swallow saliva, and “hot potato” voice.
While awaiting transfer it is vital to ensure the patient is cannulated with fluids, and IV antibiotics prescribed. Also recommended is a dose of IV dexamethasone to reduce laryngeal edema, ultimately buying time for all teams to assess the patient.14,15
MANAGEMENT OF DENTAL INFECTIONS REQUIRING FURTHER CONSULTATION FROM THE MAXILLOFACIAL TEAM
The primary question to answer in regard to odontogenic fascial swelling is, Does the patient require surgical drainage? Any patient with substantial swelling which has evidence of a collection or associated systemic signs of spreading infection as described above will likely require a second opinion from the maxillofacial team.
MANAGEMENT OF DENTAL INFECTION NOT REQUIRING ADMISSION
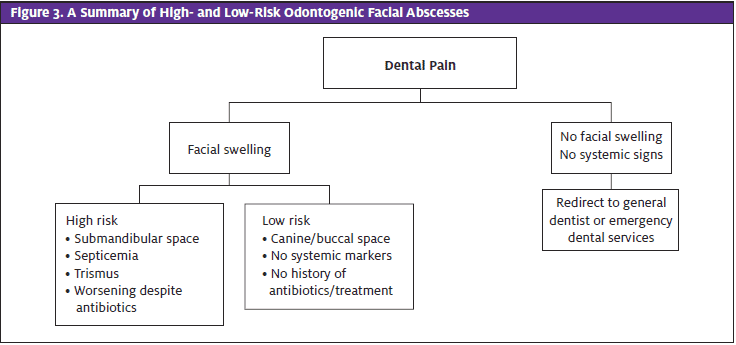
Nonemergent cases include those patients who present with swelling in low-risk regions or who do not show systemic signs of spreading infection (malaise, fever, rapid heart rate).
Pain Management
NSAIDs at regular intervals have been shown to be the best option for dental pain. Acetaminophen can be added to promote a synergetic effect.16 If this combination does not yield adequate pain relief, an opioid can be considered if deemed appropriate after reviewing the patient’s medical history. Opioids have no ceiling dose and therefore should be prescribed at a low dose initially and titrated to the effective dose.15
Antibiotics
Any systemic spread, such as swelling, raised inflammatory markers, temperature, or rigors will require antibiotics.17 Antibiotics should not be prescribed solely for dental pain. There are many sources of information for correct antibiotic prescribing including the Faculty of General Dental Practitioner guidelines or even the British National Formulary.18,19 Often, an appropriate regimen of amoxicillin and metronidazole in combination or co-amoxiclav may be considered in the first instance after consulting the patient’s allergy status. Patients with true penicillin allergy can be prescribed clindamycin and metronidazole.20
Encouragement to visit a dental practice is essential in all cases. Urgent care providers are advised to maintain contact information for emergency dentists, or even free dental care charities.
NON-ODONTOGENIC ETIOLOGIES
If panoramic radiography comes back inconclusive and the patient gives a history with no prior dental pain, there may be alternative causes. It is advisable to keep this in mind when assessing a facial swelling. One such cause could be inflammatory lesions of salivary glands, such as mumps, acute parotitis, or sialothiasis. In the submandibular region this can be submandibular sialadenitis. This can be investigated further with an ultrasound, or even an MRI of the salivary glands.21
Cellulitis can cause swelling in the deep layers of the facial tissues, often occurring on the cheek. This can be caused by broken areas of skin where bacteria can penetrate through the layers.
Another rare finding can be reactive hyperplasia of lymph nodes; this lymphadenopathy can progress into a submasseteric abscess which can mimic dental facial abscesses.21 For example, in children, lymphadenitis can masquerade as a submandibular abscess. Any progressive increase in swelling in the region of lymph nodes with no acute cause can raise suspicion of lymphoma.
It is important to keep these differentials in mind if a dental cause cannot be pinpointed easily.
CONCLUSION
It is essential to educate patients on symptoms that warrant further assessment or treatment. For example, a patient with only toothache in their first visit may progress to a facial abscess. Inform the patient of warning signs of spreading facial swelling toward the neck, eye, or associated systemic signs. This will also aid in conveying the importance of seeking appropriate dental care to the patient.
References
- Currie CC, Stone SJ, Connolly J, Durham J. Dental pain in the medical emergency department: a cross-sectional study. J Oral Rehabil. 2017;44(2):105-111.
- Multi-million pound price tag of toothache at A&E and GP practice. Available at: https://www.bmj.com/content/356/bmj.j98/rr. Accessed December 3, 2019.
- Practitioners TRAC of G. RACGP – Management of dental infections by medical practitioners. Available at: https://www.racgp.org.au/afp/2014/may/dental-infections/#8. Accessed December 3, 2019.
- Gonzalez-Beicos A, Nunez D. Imaging of acute head and neck infections. Radiol Clin North Am. 2012;50(1):73-83.
- Bridgeman A, Wiesenfeld D, Newland S. Anatomical considerations in the diagnosis and management of acute maxillofacial bacterial infections. Aust Dent J. 1996;41(4):238-245.
- Preventable deaths: an exploration of sepsis to develop clinical understanding and improve practice. Faculty Dental Journal. Available at: https://publishing.rcseng.ac.uk/doi/10.1308/rcsfdj.2018.145. Accessed December 3, 2019.
- Saifeldeen K, Evans R. Ludwig’s angina. Emerg Med J. 2004;21(2):242-243.
- Dhanrajani PJ, Jonaidel O. Trismus: aetiology, differential diagnosis and treatment. Dent Update. 2002;29:88-92, 94.
- Nyush A. Oral and Maxillofacial Medicine: The Basis of Diagnosis and Treatment. 3rd edition. Available at: https://www.academia.edu/36609700/Oral_and_Maxillofacial_Medicine_The_Basis_of_Diagnosis_and_Treatment_3e.pdf. Accessed December 3, 2019.
- Weyh A, Busby E, Smotherman C, et al. Overutilization of computed tomography for odontogenic infections. J Oral Maxillofac Surg. 2019;77(3):528-535.
- Sklavos A, Beteramia D, Delpachitra SN, Kumar R. The panoramic dental radiograph for emergency physicians. Emerg Med J. 2019;36(9):565-571.
- Sainuddin S, Hague R, Howson K, Clark S. New admission scoring criteria for patients with odontogenic infections: a pilot study. Br J Oral Maxillofac Surg. 2017;55(1):86-89.
- Uluibau IC, Jaunary T, Goss AN. Severe odontogenic infections. Aust Dent J. 2005;50(4 Suppl 2):S74-S81.
- Dowdy RAE, Emam HA, Cornelius BW. Ludwig’s angina: anesthetic management. Anesth Prog. 2019;66(2):103-110.
- Centers for Disease Control and Prevention. National Center for Health Statistics. Oral and dental health. Available at: https://www.cdc.gov/nchs/fastats/dental.htm. Accessed December 3, 2019.
- Becker DE. Pain management: part 1: managing acute and postoperative dental pain. Anesth Prog. 2010;57(2):67-79.
- Stein K, Farmer J, Singhal S, et al. The use and misuse of antibiotics in dentistry: a scoping review. J Am Dent Assoc. 2018;149(10):869-884.e5.
- National Institute for Health and Care Excellence. Excellence N-TNI for H and C. BNF: British National Formulary – NICE. Available at: https://bnf.nice.org.uk/dental-practitioners-formulary/. Accessed December 3, 2019.
- Faculty of General Dental Practice. Antimicrobial Prescribing. Available at: https://www.fgdp.org.uk/antimicrobial-prescribing. Accessed December 3, 2019.
- Oberoi SS, Dhingra C, Sharma G, Sardana D. Antibiotics in dental practice: how justified are we. Int Dent J. 2015;65(1):4-10.
- Agrawal A, Singh V, Kumar P, et al. Unilateral swelling of cheek. Natl J Maxillofac Surg. 2017;8(2):157-161.
Author affiliations: Amandeep Kaur Bains, BDS(Hons) MFDS RCPS (Glasg),Lancashire Teaching Hospitals NHS Trust, London, England. Awais Safdar Ali, BDS MJDF RCSEng, University of Manchester Dental Hospital, Manchester, England. Pavan Padaki, BDS, MFDS RCPS (Glasg), MBChB, MRCS, FRCS (OMFS), Lancashire Teaching Hospitals NHS Trust, Bolton, England.
