Published on
Urgent message: While skin-related complaints are not uncommon in the urgent care setting, with psoriasis being a relatively common source, evaluation and diagnosis of a rash can be challenging. This is especially true in the case of a rare variant like guttate psoriasis.
Chasity L. Falls, MS, PA-C
INTRODUCTION
Psoriasis is a common condition. However, the guttate variant is rarer, commonly affecting children and young adults less than 40 years of age and accounting for 4% of all clinical types of psoriasis.1,2 Other phenotypes of psoriasis include psoriatic arthritis, plaque-type psoriasis, and pustular psoriasis.3
The etiology of guttate psoriasis includes a genetic predisposition, predominantly in children and young adults. It is commonly preceded by a streptococcal infection and may develop within 2-3 weeks with or without treatment. It manifests with multiple small round papules and scaly plaques, usually located on the trunk and extremities. Here, we present the etiology, clinical findings, and treatment recommendations for guttate psoriasis and discuss the importance of a thorough history and physical for diagnosis of guttate psoriasis.
CASE PRESENTATION
A 28-year-old male with no past medical history presented to urgent care with a complaint of a rash that began 3 weeks prior. He noticed it first on his face, shortly after swimming in a lake. A week later he saw an area of redness to his right groin; at 2 weeks it developed on his hands and arms, followed by both knees and lower extremities. These lesions were described as looking similar to those on his face, which was different from those on the right groin region. It was mildly pruritic but without pain, fevers, sore throat, cough or drainage.
The patient did admit to an upper respiratory infection just before the onset of symptoms; he said it resolved spontaneously and he had not sought previous evaluation or treatment. There was no contact with any new items, food, or medications. The patient’s sexual history was positive for chlamydia, for which he received treatment 2 years prior, and his family medical history was noncontributory.
Exam
- Temperature: 99.6℉
- Respiratory rate: 18
- Heart rate: 63
- Blood pressure: 108/68
- Pulse oxygen: 99% on room air
Physical exam revealed an alert and well-developed male in no acute distress. Evaluation of his oropharynx revealed erythema to the peritonsillar region bilaterally without tonsillar edema or exudates. There was no uvula erythema or edema and no intraoral lesions on the exam. Dermatological findings were significant for numerous disseminated erythematous, round papules ranging from 1 mm to 15 mm in size on the face with sparing of the palms and soles. Silvery plaques covered the face, as well as bilateral hands and knees. There was a sizeable erythematous plaque noted to the right groin. The exam did not demonstrate lymphadenopathy or signs of a secondary bacterial infection.
Differential Diagnosis/Decision Making
The differential diagnosis included secondary syphilis, pityriasis rosea, tinea corpus, and psoriasis. The patient did have a remote history of a treated sexually transmitted infection (STI); however, he is sexually monogamous and utilizes protection. The presentation of his rash did not involve the palmar or plantar surfaces; therefore, secondary syphilis was less likely. Pityriasis rosea generally presents with a recent upper respiratory infection, resembling the patient’s history. However, pityriasis rosea has a salmon-colored herald patch that presents first, followed by a pattern of macules and papules in the shape of a Christmas tree and typically spares the face, hands, and feet, and the patient presented otherwise. Tinea corporis is an erythematous and scaly plaque; unlike our patient, tinea presents with usually one large annular lesion and central clearing.
Tests
A rapid strep test was positive.
Diagnosis
Streptococcal pharyngitis and guttate psoriasis.
Treatment
Treatment for the patient included a 10-day course of amoxicillin for streptococcal pharyngitis, as well as triamcinolone topical cream for guttate psoriasis. Amoxicillin is the current recommended standard-of-care treatment for a streptococcal infection. Topical corticosteroid cream is useful in guttate psoriasis by providing anti-inflammatory, antiproliferative, immunosuppressive, and vasoconstrictive effects.
Follow-Up
Upon follow-up, the patient stated that he had completed the course of amoxicillin and continued with the triamcinolone cream with clearing of the rash.
DISCUSSION
Guttate psoriasis commonly affects children and young adults less than 40 years of age and is uncommon in the United States, accounting for 4% of psoriasis cases; however, it is the second most common variant of psoriasis in children.1,2 It occurs in genetically susceptible patients and usually is preceded by a trigger that includes streptococcal pharyngitis, a life stressor, skin injury, drugs, or exposure to ultraviolet light.3 Sixty-three percent of guttate psoriasis cases are known to have been preceded by group A beta-hemolytic streptococcal infection within 1 week, and up to 1 month.1,2 One-third of patients diagnosed with guttate psoriasis have a family history of psoriasis in a first-degree relative.2
Classic characteristics include an acute onset in those without psoriasis or in patients with a known history of chronic plaque psoriasis. Guttate psoriasis appears as multiple scaling round “tear-drop” papules and tends to favor the trunk and extremities.4 It has been noted that in children guttate psoriasis will appear in uncommon locations such as the face and genital-anal region.4
| Differences Among Phenotypes of Psoriasis | ||
| Phenotype | Prevalence in psoriasis cases | Characteristics |
| Guttate psoriasis | 4%1,2 | Presents on the trunk initially and frequently presents 2-3 weeks after URI with group A beta-hemolytic streptococci; more likely to be pruritic |
| Psoriatic arthritis | 25% of those with psoriasis skin symptoms3 | Associated with plaque-type psoriasis; an erosive, polyarticular disease with joint dysfunction and loss of movement; usually hands and feet |
| Plaque-type psoriasis | 90%3 | A higher degree of scaling compared with guttate psoriasis2; affects the extensor surfaces of the knees, elbows, scalp and trunk |
| Pustular psoriasis | Uncommon in the U.S. | Blisters and pustules located on the palms and soles or diffusely over the body3,4 |
Treatment is based on the site and extent of the disease. Providers need to take into account the patient’s motivation level, health insurance status, availability of specialized treatment centers, age, and overall health. The first step is removing triggers and treating infections. Topical corticosteroids are beneficial; however, depending on the distribution and extent of the lesions, this may be difficult.2 Topical emollients can be used to help retain moisture in patients with pruritus.2
First-line treatment for widespread guttate psoriasis (>5% total body surface) is a dermatology referral for UV therapy.1,2 Ultraviolet-B, is recommended for extensive and nonresponsive rashes, but natural light exposure is beneficial and more economical.1 Topical vitamin D topical analogs may also be used.
Outcomes are variable; in some patients, the rash in guttate psoriasis may progress into chronic plaque psoriasis, while others will spontaneously resolve at the 3-month mark with long term remission.1,5 One-third of children diagnosed with guttate psoriasis will develop chronic plaque psoriasis later in life.4
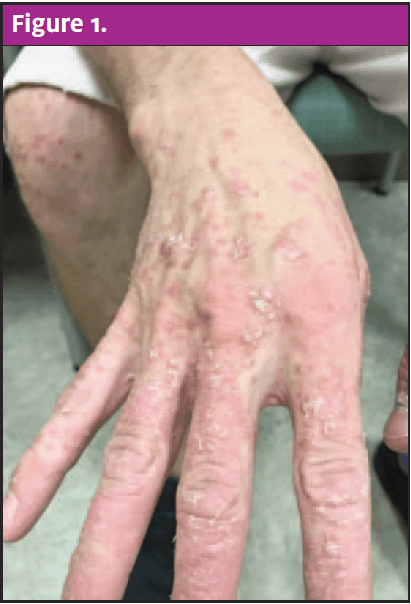
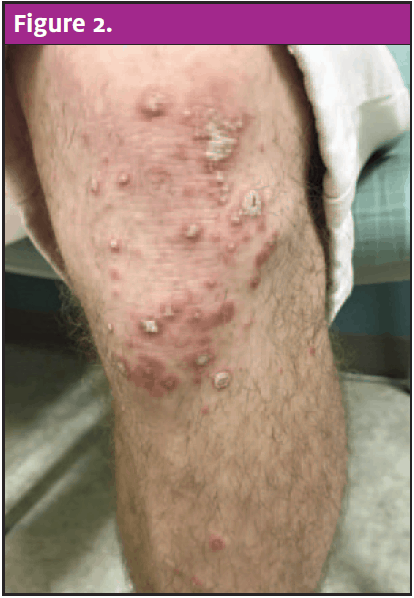
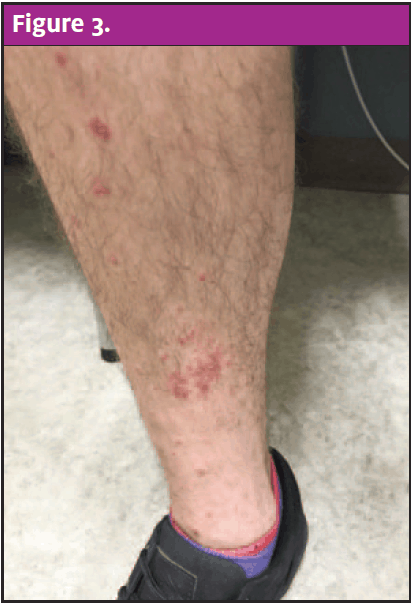
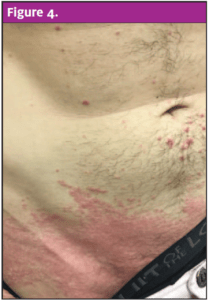
Conclusion
Guttate psoriasis often follows a trigger such as an infection and is managed by treating the underlying process as well as topical steroids and light therapy.

