Published on
Upon returning home from a busy urgent care shift, you notice a certified letter with a law firm’s return address. You open the letter and realize you are being sued in the case of a 26-year-old woman you saw almost a year ago. As your heart beats harder, you think about returning to the urgent care to pull up the chart. You wonder who you should call (the medical director, the insurance company…?) Should you put an addendum on the chart more completely detailing your memory of the case? While you remain frozen with fear racing through your mind, you hear your children’s voices calling from the TV room. “Mommy’s home!”
Many medical providers fear receiving notice of malpractice litigation.1 Even in states with low relative risk of malpractice paid claims, high levels of worry among providers persist. Regardless of the ultimate outcome of a lawsuit, the personal impact of malpractice litigation itself on the individual provider is often significant.2
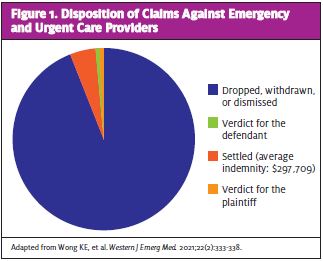
Malpractice litigation is exceedingly common. Research suggests that by the age of 65, over 75% of physicians in low-risk specialties, and 99% in high-risk specialties, had faced a malpractice claim at least once in their careers.3 The majority of claims do not result in any payment to the plaintiff, and only a small minority of cases proceed to trial. In one study, 68% of claims that closed in a single calendar year were dropped, dismissed, or withdrawn; out of the 7% of claims that were decided by a trial verdict, 88% resulted in the provider prevailing.4 In another recent study by Wong, et al, out of 6,779 closed medical professional liability claims originating from ED or urgent care centers over a 15-year period, 65.9% were dropped, withdrawn, or dismissed; 22.8% were settled for an average indemnity of $297,709; and 7.6% went to trial. Of the cases that went to trial and jury verdict, defendants prevailed 92.6% of the time.5
Despite the frequency and fear of litigation, many providers are not well-versed in how litigation unfolds once a lawsuit is initiated. In this article, we focus on the details of what a provider might expect when they find the “letter in the mail,” as well as some general principles the provider should adhere to during the early stages of litigation.
BACKGROUND
“Getting served” or “receiving notice” are the informal terms used to describe how most providers are notified that a lawsuit is being filed against them. This “service of process,” as it is known legally, is part of the right to procedural due process as guaranteed in the fifth and 14th Amendments to the United States Constitutional. This step in initiating a lawsuit is essential. If it is not executed properly and within the rules of that particular jurisdiction, the case cannot proceed.
Service of process gives the defendant provider a formal notice that the lawsuit is starting, and it is typically accompanied by the “complaint” (the stated grounds for the lawsuit). It also establishes that the court hearing the lawsuit has jurisdiction over the defendant.
A provider may be served by a certified letter in some places, but in others it may happen in person, delivered by a “process server” (an agent of the court who may deliver official documents) or even by a sheriff in uniform. There is generally no advance notice that someone is coming to serve papers, and the element of surprise unfortunately adds to the traumatic nature of the encounter.
Service of process may occur at home or work. One can imagine the impact of being served papers by a sheriff in uniform in front of colleagues or patients at work, or at home in front of family. Physicians have even described being served by a sheriff in uniform in front of extended family during Thanksgiving dinner.6
As you may surmise, this moment is sometimes leveraged by plaintiff’s attorneys as an opportunity to distress the defendant at the very start of the case. It is an opening move in a long, strategic process. Understanding that these methods are tactical, engineered to elicit an emotional response from the defendant, may be somewhat helpful in minimizing the intended effect.
The manner of service of process notwithstanding, the accompanying written complaint itself is typically quite distressing to the provider. Written in formal, legal language, it usually describes the defendant’s alleged malpractice and negligence in a very forceful and emphatic manner, again crafted for impact. An emotional response is natural—and intended.
The traumatic impact of litigation on the provider starts at the very beginning, with receiving notice. The accusation of malpractice, whether or not substandard care was rendered, often creates a cascade of responses in the defendant that may have significant psychological, cognitive, spiritual, and physical effects, known collectively as litigation stress.7 Understanding the strategy behind service of process, as well as knowing what concrete steps to take and to avoid during this time, can help mitigate the litigation stress.
FIRST STEPS: DO’S
Contact your Malpractice Insurance Carrier
The first step after receiving notice of litigation is to contact your medical malpractice insurance carrier, as they will give you further instruction on how to proceed. They will typically assign you a representative who will oversee the claim and answer any questions. They will also often assist you in the next crucial step, which is obtaining a defense attorney.
Obtain an attorney
Your insurer will be paying the attorney’s fees, and typically will determine which attorneys you may work with. If you have an attorney in mind, they may oblige you. They may assign you a particular attorney or provide you with a list of possible choices. Keep in mind that your attorney will be ushering you through a process that is foreign to you. You will be relying on them heavily, so it is helpful to have an attorney who is experienced with medical malpractice rather than personal injury law in general. Having a senior partner advising on your case is also helpful.
Your attorney will help with some crucial next steps, such as officially responding to the complaint in a timely manner, which is required by the court. They will also assist you in answering “interrogatories,” introductory questions you will likely be sent by the plaintiff’s team. This begins what is known as the “discovery phase,” in which the attorneys on each side start building their cases, filing record requests, doing research, and obtaining external case reviews and deposition testimony. In due time, your attorney will prepare you for your own deposition.
In some states, the filing of the lawsuit will automatically trigger involvement of the state Department of Health and Licensure. Your attorney can help you with whatever is required in this case as well.
Seek support
Although providers are often admonished by their insurer and attorney to avoid talking to others about the case, this refers to the medical details and case events. It is absolutely fine to talk with trusted and discreet people in your life, such as your significant other or family, about the fact that you are being sued and how it impacts you. Talking about traumatizing events is a key element in processing and recovery.5 Seeking out peer supporters may be particularly helpful, as they have a baseline understanding of the stress of malpractice litigation that laypeople may not. It may also be helpful to speak confidentially with a mental health clinician during this time.
Learn More About the Process
Several books about medical malpractice litigation are available from online vendors and have information on both the practical aspects of litigation as well as managing its psychological impact. Professional societies, malpractice insurers and attorneys may have resources, as well. Online legal reference sources can also give you an overview of the civil litigation process. Knowledge about the process and your role in it may serve to mitigate your overall anxiety.
Practice Self-Care
Healthcare providers are notorious for neglecting self-care, and the culture of medicine does not inherently encourage us to prioritize our personal needs. However, malpractice litigation is an abnormal, longitudinal stressor, uniquely designed to erode provider well-being. Being sued adds on to the already significant daily challenges of practicing medicine; combating this extra stress requires a thoughtful and strategic intervention.
Though it may at times feel difficult, establishing a routine with attention to exercise, nutrition, sleep, and personal relationships is helpful. Scheduling time for enjoyable activities and relaxation is also important, even if this means saying no to extra professional responsibilities.
Professional help from a well-trained mental health clinician can also help. As in the case of provider burnout,8 techniques exist that may help you reframe the litigation events in a more constructive way. Research-based resilience training, cognitive behavioral therapy techniques, and acceptance commitment therapy may all also arm you with valuable tools to help you cope. Litigation is unfortunately a high-risk time for burnout, anxiety, depression, substance use, post-traumatic stress disorder symptoms, and even suicide.7 Taking early, proactive steps to protect your physical and mental health is important. Give yourself permission to make your well-being a priority.
THINGS TO AVOID DURING THIS TIME: DON’TS
Do Not Alter the EMR
Do not alter the medical record in any way after receiving notice of litigation. The electronic medical record (EMR) keeps an audit trail with easily discoverable data indicating who entered the record, when they viewed it, and from what computer or terminal. It records if a chart was viewed or altered in any way, and all changes are discoverable. It is increasingly common for attorneys to hire digital forensics experts who will reveal any alteration attempts, and the optics of such attempts will spell devastation for your case. There have been many cases lost after an EMR audit in the last several years. If possible, avoid accessing the chart at all to avoiding any hint of impropriety. You will have a chance to review the records once obtained by risk management, your insurer, or your attorney.
Do Not Attempt to Contact the Plaintiff or Their Family
Occasionally, the urge to personally communicate with the plaintiff or their family is very strong. You may wish to explain what happened, or apologize for their loss, or just connect to them on a human level. However, once litigation is initiated, this could easily be seen as intimidation and is absolutely forbidden. All communication from this point further is limited to the attorneys.
Do Not Keep Your Own Notes or Do Research
Do not write notes or do any research about the case without the knowledge of your attorney. It is important that all of this is kept within the protection of attorney-client privilege. Classifying any notes as attorney-client work product is protective to you. When you are deposed, you will be asked about any notes, research, or records you have kept, and it is important that you can answer honestly under oath that you have only done this in conjunction with your attorney.
Do Not Despair
The initiation of a lawsuit is an intensely stressful time. Recognize that malpractice litigation is very common, and many of your peers and role models have weathered it. Being prepared for the challenges of litigation and taking care of your mental and physical health are of paramount importance. There are resources to help you better understand the practical aspects of litigation and its psychological impact. Understanding what steps to take, as well as the need for support and guidance during this time, will minimize the anxiety associated with the process.
CONCLUSION/TEACHING POINTS
- Most physicians will face a lawsuit at some point in their career. Less than half result in payments, and only a small number proceed to trial.
- Of cases which do go to trial, roughly 90% result in a defense verdict.
- If you are involved in a malpractice action, do not alter the chart or take notes without the advice of an attorney, as there is an easily discovered audit trail in the EMR metadata.
- Though you should not discuss the details of the case with anyone other than legal counsel, you can discuss your feelings about being involved in a malpractice action.
REFERENCES
1. Carrier ER, Reschovsky JD, Mello MM, et al. Physicians’ fears of malpractice lawsuits are not assuaged by tort reforms. Health Aff (Millwood). 2010;29(9):1585-1592.
2. Bookman K, Zane RD. Surviving a medical malpractice lawsuit. Emerg Med Clin North Am. 2020;38(2):539-548.
3. Jena AB, Seabury S, Lakdawalla D, Chandra A. Malpractice risk according to physician specialty. N Engl J Med. 2011;365(7):629–636.
4. Guardado JR. Medical liability claim frequency among US physicians. AMA Policy Research Perspectives. 2017.
5. Wong KE, Parikh PD, Miller KC, Zonfrillo MR. Emergency department and urgent care medical malpractice claims 2001–15. Western J Emerg Med. 2021;22(2):333-338.
6. Brenner IR. How to Survive a Medical Malpractice Lawsuit: A Physician’s Roadmap for Success. Hoboken, NJ: Wiley-Blackwell; 2010.
7. Charles S, Frisch P. Adverse Events, Stress and Litigation. Oxford University Press: Oxford, UK; 2005.
8. Nedrow A, Steckler NA, Hardman J. Physician resilience and burnout: can you make the switch? Fam Pract Manag. 2013;20(1):25-30.
Author affiliations: Gita Pensa, MD, FAAEM, The Warren Alpert Medical School of Brown University; The George Washington University School of Medicine. The author has no relevant financial relationships with any commercial interests.
View Similar Articles
- A Better Way To Settle Malpractice Suits?
- What To Do When You Get Named In A Malpractice Suit
- How To Get Sued For Malpractice: Four Studies In Self-Destruction

