Published on
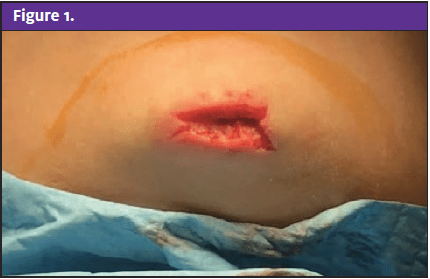
Urgent message: Adhesive repair for skin lacerations in pediatric patients is a viable (sometimes preferable) option—under the right circumstances. Careful consideration is warranted when the wound is to the chin.
Joshua Sherman, MD and David Mathison, MD, MBA
INTRODUCTION
The use of adhesive repair in lieu of sutures for the management of minor lacerations has become increasingly commonplace.1 When used correctly, cosmetic outcomes are similar and may be superior to suture repair in certain situations. For example, because it may be faster and less traumatic, adhesive repair is often the best option when working with younger children and those with developmental disorders or high anxiety.
However, as these techniques become more widely used, it is important to understand the situations and anatomic locations where adhesives may or may not be appropriate.
LITERATURE REVIEW
In the April 2019 issue of Injury, Lestage et al2 published an article entitled Complications Following Chin Laceration Repair Using Tissue Adhesive Compared to Suture in Children. This study was a retrospective chart review of children (median age 4.5 years) requiring facial laceration repair at a single tertiary care pediatric hospital in Montreal. The primary outcome was wound dehiscence in the first 30 days following the repair. A random sample of charts was reviewed in duplicate to ensure reliability of the chart review.
The authors found that among 2,044 children who presented with a facial laceration requiring intervention, 1,804 (88%) were repaired using tissue adhesive. Of the 360 chin lacerations, there were seven cases of dehiscence (2.2%) relative to 0 cases of dehiscence in all other facial laceration locations [odds ratio (OR) = 2.2]. All of these seven cases were closed with tissue adhesive. There were zero cases of dehiscence on chin lacerations that were sutured and zero cases of dehiscence on other facial lacerations closed with adhesives. When adjusting for other factors using logistic regression, the OR for location (chin vs other) being a predictor for complication was 3.84.
The authors concluded that the probability of dehiscence is greater in cases of chin lacerations versus other facial wounds.
DISCUSSION
This study offers a valuable assessment of tissue adhesive repair in more than 2,000 pediatric facial lacerations. This supports previous reports demonstrating a small but statistically significant increased rate of dehiscence with tissue adhesive3 and in this case highlights the chin as a particular area of caution.
From the perspective of a pediatric emergency medicine physician who works both in urgent care and the emergency department, this study highlights the importance of location when assessing wound integrity. The chin is not only a high-tension area, but it can be positionally difficult to repair in children if the patient flexes the neck (such as a reflex in fear of pain).
The authors’ approach is to lean towards suture repair in the vast majority of chin lacerations, and to not make this decision until the wound has been thoroughly irrigated since the irrigation process may expose a deeper or wider wound.
When using suture repair, it is advisable to employ both subcutaneous and cutaneous layer repair (when possible) to have the best cosmesis and to prevent dehiscence.
Adhesives are wonderful tools for wound repair in children, but they must be used with caution. Using adhesive is an option for chin lacerations, but only for very superficial wounds that do not further open with quality wound irrigation. Adhesives may also be a better option with chin lacerations that are more inferior and located more on neckline than the jawline.
There are obvious limitations to the Lestage paper. First, it was a retrospective chart review which lends to reporting bias, as well as incomplete documentation and follow-up. Also, this was performed at a single center where there was a very high rate (88%) of adhesive repair for facial lacerations. The outcome measure was dehiscence and not necessarily cosmetic appearance.
Working in urgent care, we balance speed and accuracy every day. We balance pain and anxiety with outcome on every shift. If we can be confident that using skin adhesive on chin laceration was as effective as using sutures it would save time, pain, anxiety, and cost while promoting patient satisfaction. However, we still must determine the level of tension, the location, the parental preference, and make an educated decision regarding route of closure when assessing every wound.
References
- Sniezek PJ, Walling HW, DeBloom JR 3rd, et al. A randomized controlled trial of high-viscosity 2-octyl cyanoacrylate tissue adhesive versus sutures in repairing facial wounds following Mohs micrographic surgery. Dermatol Surg. 2007;33(8):966–971.
- Ste-Marie-Lestage C, Adler S, St-Jean G, et al. Complications following chin laceration repair using tissue adhesive compared to suture in children. Injury. 2019;50(4) 903–907.
- Farion K, Osmond MH, Hartling L, et al. Tissue adhesives for traumatic lacerations in children and adults. Cochrane Database Syst Rev. 2002;(3):CD003326.
Author affiliations: Joshua Sherman, MD is Regional Medical Director, California, PM Pediatrics. David Mathison, MD, MBA is Vice President, Clinical Operations, PM Pediatrics.

