Published on
Urgent message: Unmanaged hyperthyroidism can cause any number of acute conditions that would drive a patient to visit an urgent care center. Further, thyroid storm can mimic several life-threatening events. Early recognition of the correct diagnosis is essential to raising the likelihood of a positive outcome—and protecting the patient from self-harm.
Amrita Mahajan, BA and Lindsey Fish, MD
INTRODUCTION
Thyroid storm is a rare, life-threatening complication of thyrotoxicosis, a condition caused by excess thyroid hormone. It is an endocrine emergency characterized by an acute exacerbation of hyperthyroidism.1 In the United States, about 16% of patients in the inpatient setting with thyrotoxicosis are diagnosed with thyroid storm.2
Thyroid storm can occur in patients with chronic untreated hyperthyroidism. While factors such as surgery (thyroid or non-thyroid), diabetic ketoacidosis, trauma, infection, or parturition can trigger or precipitate an event, the mechanism of why these factors result in thyroid storm remains unclear. Treatment includes specific therapy directed against the overactive thyroid along with supportive care in the ICU. Recognition and treatment are vital due to the sizeable rate of mortality, ranging from 10% to 30%.3
CASE PRESENTATION
A 25-year-old female with past medical history remarkable for Graves’ disease presented to an urgent care clinic with a chief complaint of malaise for 4 weeks. She reported feeling poorly with symptoms of anorexia, fatigue, myalgias, and weakness during this time. She endorsed suicidal ideation. All other reviews of symptoms were negative. She also denied any factors that alleviated or aggravated her symptoms. Other than Graves’ disease, the patient had no other relevant past medical history and was not taking any medications. Patient was a nonsmoker, did not drink, and had no recreational drug use.
Physical Examination
Temperature 37.8°C
BP 148/90
HR 186
RR 28
SpO2 95% on RA
Patient was oriented to person, place, and time. HEENT exam was remarkable for proptosis and thyromegaly. On cardiovascular exam, patient was tachycardic and regular. Neuro exam was within normal limits and patient had normal mood and affect. Skin exam disclosed warm and dry skin with no diaphoresis.
Labs/Diagnostic Studies
Electrocardiogram (Figure 1) showed sinus tachycardia and prolonged QT interval (533 msec).
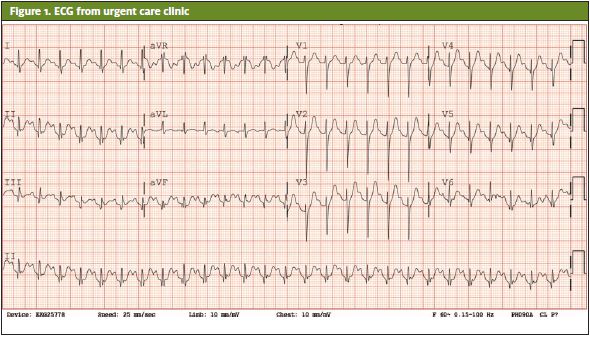
BMP and CBC were unremarkable, and troponin levels were within normal limits. Free T4 was elevated at >8 ng/dL with a TSH of <0.01. Patient had a normal lactate level. Other labs to note were an elevated alkaline phosphatase (152), total bilirubin (1.5), and elevated urobilinogen on urinalysis.
COURSE AND TREATMENT
Patient was transferred to ED via emergent ambulance. She was confirmed to be in thyroid storm (Burch-Wartofsky score 55), and treated with IV propranolol and methimazole in the ED which improved her heart rate and associated symptoms. Her elevated bilirubin and alkaline phosphatase were considered secondary to the thyroid storm and improved over time. The patient’s suicidal ideation was evaluated and treated by psychiatry. Her discharge plan included management of Graves’ disease and depression, and further work-up for the incidental finding of a ventricular-septal defect.
DISCUSSION
Thyroid storm has various presentations. Clinical features typically are an exaggeration of classic hyperthyroid symptoms, including tachycardia exceeding 140 beats per minute, congestive heart failure, hyperpyrexia (104⁰-106⁰F), and altered mental status. Encephalopathy is a known neurological manifestation of hyperthyroidism that can be exacerbated during thyroid storm and is associated with poor outcomes.4,5 Presentation of encephalopathy may include confusion, dementia, psychosis, and suicidal ideation which may be seen in up to twenty percent of patients.6-10 A list of commonly encountered symptoms with associated incidence can be found in Table 1.
Table 1. Common Symptoms of Patients with Thyroid Storm and Associated Incidence Data
| Symptoms | Incidence, percent11,12 |
| Body temperature >38°C | 66.7% |
| HR ≥ 120 bpm | 76.2% |
| HR ≥ 130 bpm | 60.8% |
| CNS manifestations | 53.5% (Glasgow Coma Scale), 62.6% (Japan Coma Scale) |
| Congestive heart failure (CHF) | 40% |
| Atrial fibrillation | 33.8%-39.3% |
| GI/hepatic manifestations | 68.3% |
While it is imperative to not miss this diagnosis, a comprehensive differential must be considered. For a young individual presenting with constitutional symptoms and tachycardia, other possibilities include:
- Arrythmia such as atrial fibrillation
- Drug use (cocaine, methamphetamines, opioid withdrawal)
- Panic disorder or attack depending on the duration of symptoms
- CNS infection
- Hypertensive encephalitis
- Heart failure
- Pheochromocytoma
Due to the broad possibilities, an urgent care provider must be vigilant about getting a thorough history and physical exam to guide the next steps in management.
Diagnosis is made based on clinical presentation and biochemical evidence of hyperthyroidism with elevation of free T3 and/or T4 and suppression of TSH. Physical examination may show goiter, lid lag, hand tremor, and Graves’ ophthalmopathy. Labs frequently demonstrate low TSH and increased free T4 +/- T3 concentrations.
Other nonspecific findings include mild hyperglycemia, hypercalcemia, abnormal LFTs, leukocytosis, or leukopenia. While there are no widely accepted criteria or clinical tools for making the diagnosis, some scoring systems have been established to assist in this. These include the Burch-Wartofsky Point Scale (BWPS) and Japanese Thyroid Association (JTA) scoring system.
The BWPS is a quantitative diagnostic tool established in 1993 used to distinguish uncomplicated thyrotoxicosis from active or impending thyroid storm.13 It is based on three observations—evidence of end-organ dysfunction, variability of signs and symptoms, and high risk of mortality if undiagnosed and subsequentially untreated—and assigns points to symptoms such as body temperature, CNS dysfunction, tachycardia, presence of atrial fibrillation, heart failure, and GI dysfunction. A score of >45 is highly suggestive of thyroid storm, while one of 25-44 points supports the diagnosis .14
The JTA scoring system is somewhat more recent (2006) and based on similar findings with thyrotoxicosis, or elevation of free T3 and/or free T4 as a prerequisite.11
In the JTA system, a combination of CNS manifestations (restlessness, delirium, psychosis, lethargy, coma), fever >38°C/100.4°F, HR >130, evidence of CHF (pulmonary edema, cardiogenic shock, or NYHA class IV), and/or GI/hepatic symptoms (nausea, emesis, diarrhea, total bilirubin >3 mg/dL) is required.
A patient with thyrotoxicosis with at least one CNS manifestation plus >1 other symptom or a combination of at least features among fever, GI/hepatic manifestations, CHF, or tachycardia is diagnosed with definite thyroid storm (TS1), while suspected thyroid storm (TS2) is defined by thyrotoxicosis plus a combination of at least two features from tachycardia, CHF, GI/hepatic manifestation, and/or fever or a patient with a previous history of thyroid disease and presence of goiter and exophthalmos on physical exam who meets TS1 criteria but has no thyroid function test values available.
While it has its uses, pitfalls include false positives due to its liberal criteria and potential for missed diagnoses due to atypical presentation in pediatric and elderly patient populations. These tools are not substitutes for a keen eye and sound clinical judgement, but they can be utilized as a resource to assist with diagnosis while recognizing their strengths and limitations.
Initial treatment of thyroid storm involves a therapeutic regimen of multiple medications and supportive therapy (IV fluids, cooling blankets, and glucose). Medications include beta blockers, thionamides, iodine solution, glucocorticoids, and possibly bile acid sequestrants. The intent of a beta blocker is to control symptoms secondary to increased adrenergic tone, while glucocorticoids reduce conversion of T4 to T3 and an iodine solution can block the release of thyroid hormone. Thionamides block the synthesis of new hormone and are indicated for treatment of hyperthyroidism. While they are incorporated in initial treatment, thionamides alone are unable to control thyroid storm due to their inability to act on previously formed T4 and T3 and needing at least 3 to 8 weeks to lower circulating T4 and T3.9
Long-term management of hyperthyroidism involves discontinuing most of the acute therapies (iodine, glucocorticoid, beta blocker) and titration of the thionamide to an appropriate level once thyroid function tests return to normal. Patients should also be monitored regularly. Should medical therapy fail to manage symptoms, options such as radioiodine therapy and surgery can be considered.
CONCLUSION
In summary, thyroid storm is a very rare yet life-threatening endocrine emergency seen in patients with hyperthyroidism. Thyroid storm has variable presentations but often they are exaggerations of typical hyperthyroidism features, such as tachycardia, hyperpyrexia, weight loss, and altered mental status with possible physical exam findings of goiter, lid lag, hand tremor, and Graves’ ophthalmopathy. Diagnosis is primarily clinical and can be further supported by thyroid function tests. Due to its considerable mortality rate (10%-30%), immediate identification and treatment of thyroid storm are crucial. Initial treatment involves a beta blocker, glucocorticoids, and a thionamide (the latter carrying over to long-term management), with supportive therapy such as IV fluids and cooling blankets. Upon improvement of clinical symptoms and normalization of thyroid function tests, long-term therapy and routine monitoring are indicated.
REFERENCES
- Sarlis NJ, Gourgiotis L. Thyroid emergencies. Rev Endocr Metab Disord. 2003;4(2):129-136.
- Swee du S, Chng CL, Lim A. Clinical characteristics and outcome of thyroid storm: a case series and review of neuropsychiatric derangements in thyrotoxicosis. Endocr Pract. 2015;21(2):182-189.
- Angell TE, Lechner MG, Nguyen CT, et al. Clinical features and hospital outcomes in thyroid storm: a retrospective cohort study. J Clin Endocrinol Metab. 2015;100(2):451-459.
- Ono Y, Ono S, Yasunaga H, et al. Factors associated with mortality of thyroid storm: analysis using a national inpatient database in Japan. Medicine (Baltimore). 2016;95:e2848.
- Angell TE, Lechner MG, Nguyen CT, Salvato VL, Nicoloff JT, LoPresti JS. Clinical features and hospital outcomes in thyroid storm: a retrospective cohort study. J Clin Endocrinol Metab. 2015;100(2):451-459.
- Joo SH, Jeong JH, Hong SC. A case report of suicidal behavior related to subclinical hyperthyroidism. Neuropsychiatr Dis Treat. 2014;10:641-643.
- Lu Y-Y, Hu K-W, Foo N-P. Psychotic appearances in a young girl: thyroid storm. J Acute Med. 2013;3(1):14-16.
- Cota E, Lentz J. Gland new psychosis: new onset adult psychosis with suicidal ideation and attempt in the setting of thyroid storm. Case Rep Psychiatry. 2017;2017:7402923.
- Martin FI, Deam DR. Hyperthyroidism in elderly hospitalised patients. Clinical features and treatment outcomes. Med J Aust. 1996;164(4):200-203.
- Fukui T, Hasegawa Y, Takenaka H. Hyperthyroid dementia: clinicoradiological findings and response to treatment. J Neurol Sci. 2001;184(1):81-88.
- Akamizu T, Satoh T, Isozaki O, et al. Japan Thyroid Association. Diagnostic criteria, clinical features, and incidence of thyroid storm based on nationwide surveys. Thyroid. 2012;22(7):661-679.
- Akamizu T. Thyroid storm: a Japanese perspective. Thyroid. 2018;28(1):32-40.
- Bacuzzi A, Dionigi G, Guzzetti L, et al. Predictive features associated with thyrotoxic storm and management. Gland Surg. 2017;6(5):546-551.
- Burch HB, Wartofsky L. Life-threatening thyrotoxicosis. Thyroid storm. Endocrinol Metab Clin North Am. 1993;22(2):263-277.
Author affiliations: Amrita Mahajan, BA, University of Colorado Anschutz Medical Campus. Lindsey Fish, MD, Federico F. Peña Southwest Urgent Care Clinic, Denver Health and Hospital; University of Colorado School of Medicine. The authors have no relevant financial relationships with any commercial interests.

