Published on
Bradley L. Laymon, PA-C, CPC, CEMC
PRESENTATION
A mother brings in her 4-year-old, who has never visited your urgent care center before, with complaints of fever and sore throat. The mother provides the HPI. She explains that the child’s symptoms have been present for 2 days. During that time, the patient’s temperature rose to a high of 101.5°F (38.6°C). Ibuprofen has been effective in reducing the fever. The girl was exposed to COVID-19 at daycare 3 days ago. The mother reports no other complaints. The child has no known allergies.
Current Outpatient Medications
Over-the-counter ibuprofen
Current Facility-Administered Medications
None
Physical Exam
- Blood pressure – not obtained
- Pulse 128
- Temperature 101.0° (38.3°C)
- Respiration 26
- SpO2 98%
- Weight 36 pounds
- General appearance: Alert child sitting in mom’s lap, no apparent distress, appears stated age
- Head: Normocephalic, without obvious abnormality, atraumatic
- Eyes: Conjunctivae/corneas clear; PERRLA; no discharge
- Ears: TMs clear, no erythema or discharge
- Mouth: oropharynx is erythematous with strawberry appearance. No exudates
- Neck: Nontender anterior cervical adenopathy
- Lungs: Clear to auscultation bilaterally. No rales, rhonchi, or wheezing
- Heart: Tachy rate and rhythm; S1, S2 normal; no murmur, click, rub, or gallop
- Skin: Color, texture, turgor normal. No rashes or lesions
Assessment
- Strep pharyngitis
- Exposure to COVID-19
The Plan
The mother was advised to give OTC acetaminophen or ibuprofen PRN for discomfort or fever.
ENCOUNTER SUMMARY
- Point-of-care group A beta-hemolytic streptococcal was positive. Prescribed amoxicillin 250/5mL, 1 tsp TID for 10 days
- Point-of-care COVID-19 nucleic acid test was negative
CODING CONSIDERATIONS
Previsit planning was completed via Snapshot and review of chart. I reviewed the patient instructions on the after-visit summary; the patient and family verbalized that they understood what the problem is, what they need to do about it, and why it is important that they do it.
The patient and family voiced understanding of all medications. No barriers to adherence were noted. Patient was taking and tolerating all medications. AVS was given to patient/MyChart.
Number and Complexity of Problems Addressed
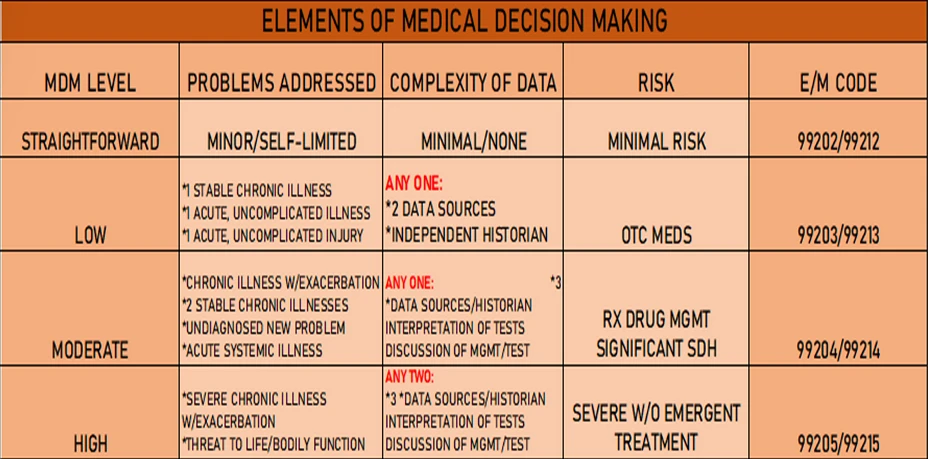
Patient complaint, per mother, was fever and sore throat. This would fall under “1 acute, uncomplicated illness or injury”—which is a “Low” medical decision-making or level 3.
Amount and/or Complexity of Data to Be Reviewed and Analyzed
In this case, the provider ordered a POCT strep and COVID. This would count toward two “ordering of each unique test” in Category 1. Since the provider received the HPI from the mother (“assessment requiring an independent historian(s)”), one point would be awarded. This would meet the criteria for Category 1 in the Moderate section, which is level 4.
Risk of Complications and/or Morbidity or Mortality of Patient Management
Amoxil was prescribed to treat strep pharyngitis. This would meet the criteria for level 4 – prescription drug management. Two of the three elements of MDM need to be met when choosing your level of service. We successfully met level 4 criteria in the Data and Risk categories, so this is a 99204.
CONCLUSION
What if the provider had not documented that they used an independent historian (mother) to gather the HPI? This would drop the LOS to a 99203 since the Complexity of Data Category 1 requirement would not be met. If the strep test were negative, this would lower the LOS to a 99203 because no prescription would be needed.