Published on
Urgent message: Upper abdominal pain is a common presentation in urgent care practice. Narrowing the differential diagnosis is sometimes difficult. Understanding the pathophysiology of each disease is the key to making the correct diagnosis and providing the proper treatment.
TRACEY Q. DAVIDOFF, MD
Part 1 of this series focused on disorders of the stomach—gastritis and peptic ulcer disease—on the left side of the upper abdomen. This article focuses on the right side and center of the upper abdomen: biliary tract disease and pancreatitis (Figure 1). Because these diseases are regularly encountered in the urgent care center, the urgent care provider must have a thorough understanding of them.
Biliary Tract Disease
The gallbladder’s main function is to concentrate bile by the absorption of water and sodium. Fasting retains and concentrates bile, and it is secreted into the duodenum by eating. Impaired gallbladder contraction is seen in pregnancy, obesity, rapid weight loss, diabetes mellitus, and patients receiving total parenteral nutrition (TPN).
About 10% to 15% of residents of developed nations will form gallstones in their lifetime.1 In the United States, approximately 6% of men and 9% of women have gallstones.2 Stones form when there is an imbalance in the chemical constituents of bile, resulting in precipitation of one or more of the components. It is unclear why this occurs in some patients and not others, although risk factors do exist. Gallstones can occur in all age groups, but the incidence increases with age. Everyone remembers the 4 F’s from medical school: “fat, fertile, female, and forty.” Estrogens cause more cholesterol to be excreted in bile, increasing risk. Obesity is certainly a factor, and family history is also contributory.
Biliary sludge is a mixture of particulate matter and bile that may turn into tiny gallstones. It is common in patients who are or have been pregnant or who are receiving TPN. Persistent sludge may become gallstones, or the sludge itself may cause cholecystitis. Most patients with sludge are asymptomatic. The majority of patients found to have incidental gallstones are asymptomatic and are not at risk for developing gallbladder disease. Less than 20% will develop symptoms over 15 years, and their illness will not be severe. The risk of developing a severe complication from these stones is much less than the risk of a complication from a cholecystectomy, and therefore it is not recommended that patients with asymptomatic gallstones undergo cholecystectomy. Once a patient develops symptoms, however, their subsequent risk of developing complications is much higher, and prophylactic cholecystectomy is advisable.2
Biliary tract disorders are the second most common surgical illness in pregnancy, with an incidence of symptomatic gallstones of about 0.1%.3 Surgical intervention should be delayed until after delivery if at all possible, although laparoscopic cholecystectomy has been proven safe in pregnancy.
Biliary Colic
The most common illness related to gallstones is biliary colic. The patient experiences right upper quadrant or midepigastric abdominal pain lasting for 2 to 6 hours, which then remits spontaneously. The pain is intense, sharp, and stabbing in nature and may be associated with nausea, vomiting, fever, and diaphoresis. It may radiate around (not through) to the back, specifically the right shoulder blade. It is not exacerbated by movement, and not relieved by position, movement, or passage of flatus or stool. Symptoms occur because of increasing intraluminal pressure and distention of the biliary tract as 1 or more stones migrate from the gallbladder into the cystic or common bile duct. Commonly the symptoms begin between 9 p.m. and 4 a.m. Dyspepsia, belching, and bloating are nonspecific symptoms that are just as common in people with gallstones as those without. A common trigger is a fatty meal, although association with meals is not universal. If the initial obstruction is not relieved by persistent contractions, or if the stone does not fall back into the gallbladder, an inflammatory response will occur by mechanical, chemical, or infectious means. If pain lasts more than 5 to 6 hours, think complications, such as acute cholecystitis or acute pancreatitis.
These patients look uncomfortable, but findings on the physical examination are usually benign. There may be some right upper quadrant tenderness, which is often underwhelming compared with the amount of pain the patient appears to be in. There are no peritoneal signs. There should be no jaundice. There may be some signs of dehydration, such as dry mouth or poor skin turgor if vomiting has been severe.
| Table 1. Complications of Gallstones | |
|
|
Although the diagnosis of biliary colic is frequently made by medical history, ultrasonography is necessary to identify the presence of stones and to rule out other illnesses or complications that may be occurring such as acute cholecystitis (see the section “Acute Cholecystitis”). It should be noted, however, that the absence of stones on ultrasonography does not rule out their existence; small stones and sludge may be missed,1 and the sensitivity of ultrasonography may be operator dependent.
Once a patient has developed symptoms related to gallstones, definitive treatment with surgery is recommended, because the risk of subsequent symptoms or complications is high.4 Stones can occur and become symptomatic even after the gallbladder has been removed, months to even years after cholecystectomy. Therefore, a history of cholecystectomy does not rule out the possibility of biliary colic. The incidence of this is unknown, but it is probably low.5 Stones occurring immediately after surgery are called retained stones, and those occurring months to years after are recurrent stones.
Patients with biliary colic should be treated for pain with opioids and nonsteroidal anti-inflammatory drugs: oral if possible, but parenteral if nausea and vomiting prevent the use of oral medications. All narcotics increase biliary pressure and spasm of the sphincter of Oddi and theoretically could make biliary obstruction worse; however, proof of this has never been reported in the literature.5 Pain relief is more important than any theoretical risk. Antiemetics may be required. Intravenous hydration should be given if dehydration is suspected. Patients having symptoms for more than 6 hours or who have evidence of complications should be referred to an emergency department (ED). Patients whose condition improves and who are asymptomatic after an episode of biliary colic can be referred to surgery for outpatient, elective cholecystectomy.
| Table 2. Laboratory Studies to Rule Out Complications of Biliary Colic | |
| Test | May Rule Out |
| Liver biochemical markers (AST, ALT, ALK, bilirubin) | Hepatitis, biliary tract obstruction, acute cholecystitis |
| Serum amylase and lipase | Acute pancreatitis |
| CBC count | Acute cholecystitis or acute cholangitis |
| Urinalysis | UTI, renal colic |
| Upper endoscopy | PUD, gastritis |
| Endoscopic ultrasonography | Chronic pancreatitis |
| ERCP with sphincter of Oddi manometry | Sphincter of Oddi dysfunction |
| Cholescintigraphy with or without CCK | Acute cholecystitis and functional gallbladder disorder |
| ECG | Ischemic heart disease |
| Esophageal manometry | Esophageal spasm |
| ALK = anaplastic lymphoma kinase; ALT = alanine aminotransferase; AST = aspartate aminotransferase; CBC = complete blood cell; CCK = cholecystokinin; ECG = electrocardiography; ERCP = endoscopic retrograde cholangiopancreatography; PUD = peptic ulcer disease; UTI = urinary tract infection. | |
Red-flag symptoms and signs indicating impending complications (Table 1) include pain lasting more than 6 to 8 hours, intractable vomiting, fever, jaundice, elevated white blood cell (WBC) count, elevated enzyme levels on liver function tests, and elevated amylase and/or lipase levels.2 Findings on all laboratory studies (Table 2) should be normal in patients with uncomplicated gallbladder disease or biliary colic. Patients suspected of having a complication, or in whom the diagnosis is unclear, should undergo ultrasonography, if available, or should be referred to the nearest ED for further evaluation.
| Table 3. Differential Diagnosis of Upper Abdominal Pain Not Related to Biliary or Pancreatic Disease |
| • Esophagitis or gastroesophageal reflux disease • Acute hepatitis • Peptic ulcer disease • Gastritis or duodenitis • Dyspepsia • Irritable bowel disease • Disorders of the right kidney, including renal colic • Right lower lobe pneumonia • Fitz-Hugh-Curtis syndrome • Subhepatic or intra-abdominal abscess • Perforated viscus • Cardiac ischemia • Black widow spider envenomation • Retrocecal appendicitis |
Atypical symptoms should prompt an investigation for other diagnoses (Table 3), even if the patient has known or documented gallstones. These include
- Chest pain
- Nonspecific abdominal pain
- Belching
- Fullness after meals or early satiety
- Fluid regurgitation
- Abdominal distention or bloating
- Epigastric or retrosternal burning sensation
- Nausea or vomiting without typical biliary colic pain
Acute Cholecystitis
Acute cholecystitis is an inflammation of the gallbladder most commonly caused by gallstones. Approximately 1% to 3% of patients with symptomatic gallstones will develop acute cholecystitis.3
In most cases, acute cholecystitis is caused by to obstruction of the cystic duct of the gallbladder by a stone or sludge that has impacted at the neck of the gallbladder. This obstruction causes the pressure in the gallbladder to build and, in combination with bile, causes an inflammatory response. Secondary bacterial infection may occur in up to 20% of patients,3 usually with enteric organisms such as Escherichia coli, Klebsiella, and Enterococcus faecalis. The overall mortality of a single episode of acute cholecystitis is approximately 3%, depending on the patient’s underlying health and surgical risk.
4
In acute cholecystitis, pain is localized to the right upper quadrant and lasts for more than 4 to 6 hours,6 as opposed to biliary colic, in which the pain is more intermittent. The pain may radiate to the right shoulder or around to the back. Nausea and vomiting are common. There is abdominal tenderness in the right upper quadrant, there is voluntary and involuntary guarding, and there will be positive findings for Murphy sign (pain with palpation on deep inspiration in the right upper quadrant with associated inspiratory arrest). The sensitivity and specificity of Murphy sign are 97% and 48%, respectively.6 If septicemia is present, there may be fever. Mild jaundice may be present.
Typically patients will have a leukocytosis with increased band cells. Liver enzymes and bilirubin levels will more than likely not be elevated, because the obstruction is limited to the gallbladder. Think complications if alkaline phosphatase and bilirubin levels are elevated.6 Amylase and lipase levels may be slightly elevated because of the passage of smaller stones or sludge prior to obstruction. It should be noted that laboratory findings are nonspecific and cannot definitively distinguish colic from cholecystitis.
All patients suspected of having acute cholecystitis should be referred to a hospital.3
The diagnosis of acute cholecystitis can be made on the basis of medical history, but it must be supported by the characteristic findings on ultrasonography, which is the test of choice. Typically there is pericholecystic fluid around the gallbladder, edema of the gallbladder wall, gallstones, and a sonographic Murphy sign. The sensitivity and specificity of ultrasonography for cholecystitis are 88% and 80%, respectively; for gallstones, the respective values are 84% and 99%.6 Distinguishing biliary colic from acute cholecystitis can be difficult. Murphy sign is the most sensitive (65%) and specific (87%) element of the history and physical that can distinguish the two. In the sonographic Murphy sign, the ultrasound probe is used for palpation and visualizing the stones during the test.
Plain abdominal films show gallstones in only 10% of cases.3 Gas within the gallbladder may be seen in emphysematous cholecystitis, which is rare. Plain films should not be routinely ordered for suspected gallbladder disease.
When the diagnosis remains in question after ultra sonography, biliary scintigraphy or a hydroxyiminodiacetic acid (HIDA) scan can be performed. The patient is injected with radiolabeled HIDA. In healthy gallbladders, uptake can be seen in 1 to 2 hours, but in inflamed gallbladders, there is no uptake seen. The sensitivity and specificity of HIDA scans for acute cholecystitis are approximately 97% and 90%, respectively.6
The treatment of acute cholecystitis is ultimately surgical. In most patients, the disease is managed initially with medical treatment, including fasting, rehydration, and pain medications. The impacted stone falls back into the gallbladder, and then it can be removed electively. If this does not happen, gangrenous cholecystitis, empyema, or perforation may result. Nonsteroidal anti-inflammatory drugs, specifically ketorolac,6 are recommended as first-line treatment for pain because they also provide an anti-inflammatory effect. Some patients may require narcotic pain medications as well. Antiemetics may also be required. If an infectious process is suspected, treatment with a second- or third-generation cephalosporin and metronidazole is also recommended.
Twenty percent of patients with acute cholecystitis need emergency surgery when peritonitis or emphysematous cholecystitis (air in the gallbladder) is present.3,4 The remaining 80% can be observed with medical management to have the inflammation “cool down,” and then laparoscopic cholecystectomy can be performed in several days, usually within 72 hours of presentation.3,4
Choledocholithiasis
A stone lodged in the common bile duct may cause typical biliary colic pain, however it will last longer and eventually lead to more complicated disease. Serum aspartate aminotransferase (AST) and alanine aminotransferase (ALT) levels are typically elevated. If the stone does not pass, serum anaplastic lymphoma kinase (ALK), bilirubin, and glutamyl transpeptidase (GGTP) levels may become elevated out of proportion to the ALT and AST levels. Acute cholangitis may subsequently develop causing fever, leukocytosis, and sepsis syndrome.
Ultrasonography may be helpful, but visualizing stones in the distal portion of the duct may be difficult. Magnetic resonance cholangiopancreatography, endoscopic ultrasonography, or ERCP may be useful in these cases.
Ascending Cholangitis
Ascending or acute cholangitis occurs as a result of infection and stasis of infected bile in the biliary tract. Its severity can range from mild to life-threatening. The patient will present with fever, abdominal pain, and jaundice (often called Charcot triad), then progress to confusion and hypotension. Septic shock can occur, progressing to multisystem organ failure. Patients taking glucocorticoids, especially the elderly, may have no symptoms until hypotension occurs. Laboratory findings include a cholestatic pattern of abnormal liver enzymes and an elevated WBC count.
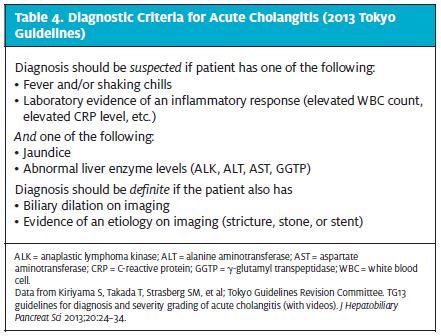
Bacteria enter the biliary tract because of gallstones, sludge, or manipulation of the sphincter of Oddi, usually as an iatrogenic effect of ERCP, stent placement, or percutaneous drainage, but bacterial ingress can be spontaneous. E. coli is the most common gram-negative bacteria, followed by Klebsiella and Enterobacter species. Enterococcus species may also be responsible. Occasionally a mixed picture with anaerobes occurs (Table 4). Ascending cholangitis is a medical emergency that requires immediate evaluation in an ED.
Pancreatitis
Acute Pancreatitis
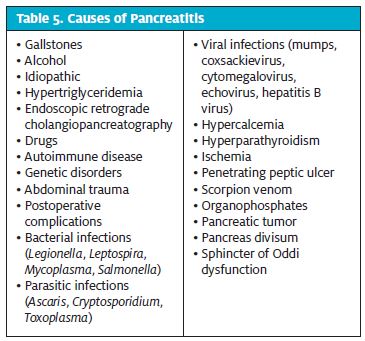
Acute pancreatitis is an inflammatory process that can range from mild to severe. Mild cases can resolve with minimum treatment and have a mortality rate of <1%, whereas severe cases can result in multiorgan system failure, with death rates of 20% to 30%. Gallstones are the leading cause cause (35%–40%) of pancreatitis (Table 5), followed by acute or chronic alcoholism (20%); idiopathic (15%–20%); ERCP (5%); elevated triglycerides (1%–4%); and drugs (1%–2%).
The incidence of pancreatitis has been increasing, perhaps because of the increasing incidence of obesity and, by extension, gallstones.7 Acute pancreatitis is responsible for $2.2 billion in U.S. health-care expenditures yearly.
The pathophysiology of pancreatitis relates to the unregulated activation of trypsin within the pancreatic acinar cells, as well as to a lack of elimination of excess trypsin. The trypsin spills into the interstitial and endothelial spaces, causing autodigestion of the gland and pancreatic injury. The result is inflammation, acinar necrosis, pseudocyst formation, and pancreatic abscess, or phlegmon. The inflammation and release of mediators may cause damage to surrounding as well as distant structures, initiating the systemic inflammatory response syndrome, multisystem organ failure, and death.
Gallstone pancreatitis is caused by passage of gallstones through the cystic duct into the distal common bile duct, where they obstruct the biliary and pancreatic ducts. This obstruction and resulting dilation of the ducts causes inflammation, which activates the process of pancreatitis.
Incidence is highest in patients with small gallstones or sludge because these materials are more likely to proceed as far as the common bile duct. Gallstone pancreatitis is more common in Caucasians, Hispanics, and American Indians. Obesity is not only a risk factor; obese patients are more likely to have more severe disease. Pregnancy is also a risk factor for gallstone pancreatitis.7
The incidence of alcohol-related acute pancreatitis peaks between the ages of 35 and 44 years. The risk of death is also higher in this group, perhaps because of poor baseline nutrition. Idiopathic pancreatitis is more common in patients of African heritage.
Pancreatitis occurring after ERCP, or iatrogenic pancreatitis, occurs in about 3.7% of patients undergoing the procedure, although individual risk factors also play a role. Iatrogenic pancreatitis may also occur after abdominal surgery, cardiac surgery, liver biopsy, and abdominal procedures performed by interventional radiologists. Hypercalcemia from TPN may also be an iatrogenic etiology of pancreatitis.
Elevated triglyceride levels can be seen in familial disorders, the third trimester of pregnancy, poorly controlled type 2 diabetes, alcoholism, and hypothyroidism. Triglyceride levels can be falsely elevated during an episode of acute pancreatitis, so levels should be tested again after the pancreatitis has resolved.
Hypercalcemia is also a recognized etiology of pancreatitis, and it can be seen in malignancy, TPN, sarcoidosis, vitamin D toxicity, and as a complication of cardiopulmonary bypass.
Because of the strong relation of drugs to pancreatitis, it is important to obtain a thorough medication history for all patients presenting with pancreatitis, especially those whose disease is of an unclear etiology (Table 6). To be considered drug-induced, the pancreatitis must occur while the patient is taking the drug and resolve when the drug is stopped.
| Table 6. Drugs Commonly Associated with Pancreatitis | |
|
|
Rare causes of pancreatitis include autoimmune disease, trauma, ampullary carcinoma, intraductal papillary mucinous neoplasm of the pancreas, pancreas divisum, and other congenital anomalies of the pancreas. If the underlying cause of pancreatitis is not identified and treated, the risk of recurrent pancreatitis within 6 years may be as high as 40%.7 If gallstone pancreatitis is recognized and the gallbladder is removed, the risk is reduced to 10%.
Patients presenting with pancreatitis will give a medical history that is based on the underlying disorder. For example, a patient with gallstone pancreatitis will present with symptoms of biliary colic. A patient with iatrogenic pancreatitis may present after having undergone ERCP the day before. A patient with drug-induced pancreatitis will have recently started taking a new medication or an increased dose. Alcoholic pancreatitis may be preceded by a binge or even a single alcoholic drink. Pancreatitis is heralded by a constant, boring5 midepigastric abdominal pain radiating through to the back, frequently accompanied by nausea and vomiting. The pain may radiate to other areas of the abdomen, and its intensity can vary from minor to severe. Abdominal distention or bloating is a common symptom, because patients can often develop ileus. Patients usually feel better sitting up with the knees bent than they do when lying flat.5
On examination, the patient may be in moderate distress from pain. Low-grade fever, tachycardia, and hypotension are often present. Midepigastric abdominal tenderness is usually present. Peritonitis, if present, is generally a late finding because of the retroperitoneal location of the organ. Bowel sounds may be diminished if ileus is present. Cullen sign is a traditional finding of bluish discoloration around the umbilicus, and Grey Turner sign is a bluish discoloration of the flanks rarely seen with hemorrhagic pancreatitis. As the patient becomes sicker, signs of multiorgan system failure, such as respiratory distress, third-spacing, and decreased urine output, may occur.
The mainstays of laboratory testing for pancreatitis are amylase and lipase levels. These are both digestive enzymes normally found in the pancreas whose serum levels increase as the pancreas becomes inflamed. Unfortunately, low levels of amylase may also be found in numerous other tissues and neoplasms, making a finding of an elevated amylase level less specific for pancreatitis. Amylase levels rise quickly and return to normal within 3 to 4 days of resolution of pancreatitis. Lipase level, however, is much more specific and more accurate in the diagnosis of pancreatitis. Its rise is also rapid, but it may take 7 to 14 days to return to baseline. It is the preferred test for pancreatitis. There is no benefit to ordering both tests when evaluating a patient for pancreatitis. It should be noted that the levels of amylase and lipase do not correlate to the severity of disease.
Plain radiographs in the setting of pancreatitis are useful only for excluding other disease processes that may be responsible for the patient’s symptoms. Ultrasonography is useful if it is thought that the pancreatitis is due to gallstones, whereas it is less useful in nonbiliary etiologies. Computed tomography scanning provides superior anatomic definition, especially when grading disease and when looking for abscess. It may be less useful in mild or early disease. ERCP may be useful in those patients in whom the etiology is unclear.
The Ranson criteria (Table 7) for determining the prognosis of pancreatitis have long been used to attempt to predict poor outcome, but research has shown them to have a poor predictive value that does not improve on clinical judgment.5 Many other scoring systems have been developed, but similar to Ranson, they have not shown any clinical usefulness.8

The majority of patients with suspected or confirmed pancreatitis seen in an urgent care center should be sent to an ED for further evaluation.
Ninety percent of all patients with pancreatitis recover without complications and with the use of only supportive measures. The mainstay of treatment is to rest the pancreas by withholding oral intake, although in mild cases, patients can be given clear liquids. Adequate intravenous hydration should be provided to keep urine output at about 100 mL/h. Patients in unstable condition should be treated with aggressive supportive measures and may require treatment in an intensive care unit. Adequate pain medication and antiemetics should be provided. Patients with biliary disease should be treated accordingly. Empiric antibiotics are not recommended except in severe disease.
Chronic Pancreatitis
Chronic pancreatitis is a relapsing and remitting disease process that in most cases is not a complication of acute pancreatitis. Alcohol abuse is the most common etiology, with an idiopathic etiology accounting for most of the remaining cases. Patients may present with acute exacerbation of chronic pain. The pain is similar to that in acute pancreatitis: midepigastric abdominal pain radiating to the back. Patients may have nausea and vomiting. The episode may be precipitated by alcohol ingestion. Patients who have had pancreatitis for some time may appear chronically ill, with wasting, clubbing, and possibly stigmata of chronic liver disease. Abdominal tenderness may be less prominent. Amylase and lipase levels may be elevated, but they may also be normal in long-term disease.
When patients with chronic pancreatitis present with abdominal pain, other conditions should first be ruled out, and exacerbation of chronic pancreatitis should be a diagnosis of exclusion. Patients should be assessed for hydration status and be given pain medication. If pain or emesis cannot be controlled orally, they may need assessment in an ED for possible admission.
Conclusion
Upper abdominal pain is a common presentation in urgent care centers. Assessing for and ruling out the more serious illnesses is the key to successful management. Patients with red-flag symptoms should be sent to an ED in a timely fashion. Pain management and hydration status are important in all causes and should be evaluated and treated accordingly.
References
- Sanders G, Kingsnorth AN. Gallstones. BMJ 2007;335:295–300.
- Zakko SF. Uncomplicated gallstone disease in adults. Waltham (MA): Wolters Kluwer Health, UpToDate. © 2015 [updated 2015 February 17; cited 2015 March 25]. Available from: http://www.uptodate.com/contents/uncomplicated-gallstone-disease-in-adults
- Indar AA, Beckingham IJ Acute cholecystitis. BMJ 2002;325:639–643.
- Vollmer CM, Zakko SF, Afdhal NH. Treatment of acute calculous cholecystitis. Waltham (MA): Wolters Kluwer Health, UpToDate. © 2015 [updated 2015 February 3; cited 2015 March 2]. Available from: http://www.uptodate.com/contents/treatment-of-acute-calculous-cholecystitis
- Atilla R, Oktay C. Pancreatitis and cholecystitis. In: Tintinalli J, Stapczynski JS, Cline DM, Ma OJ, Cydulka RK, Meckler GD, eds. Tintinalli’s Emergency Medicine: A Comprehensive Study Guide. 7th edition. New York, New York: McGraw-Hill; 2011:558–566.
- Zakko SF, Afdhal NH. Acute cholecystitis: pathogenesis, clinical features, and diagnosis. Waltham (MA): Wolters Kluwer Health, UpToDate. © 2015 [updated 2013 November 19; cited 2015 March 2]. Available from: http://www.uptodate.com/contents/acute-cholecystitis-pathogenesis-clinical-features-and-diagnosis
- VanWoerkom R, Adler DG. Acute pancreatitis: review and clinical update. Hospital Physician 2009;January:9–19. Available from: http://www.turner-white.com/memberfile. php?PubCode=hp_jan09_acute.pdf
- Ranson JH, Rifkind KM, Roses DF, et al. Prognostic signs and the role of operative management in acute pancreatitis. Surg Gynecol Obstet 1974;139:69–81.
- Kiriyama S, Takada T, Strasberg SM, et al; Tokyo Guidelines Revision Committee. TG13 guidelines for diagnosis and severity grading of acute cholangitis (with videos). J HepatobiliaryPancreat Sci 2013;20:24–34.