Published on
Urgent message: Gastritis and peptic ulcer disease are a spectrum of diseases that can range from mild to serious; urgent care providers must be on the alert for these conditions. Early diagnosis and treatment, along with recommendations for follow-up care with appropriate specialists, can help prevent long-term sequelae.
TRACEY Q. DAVIDOFF, MD
Gastritis and peptic ulcer disease (PUD) represent a continuum along a path of inflammation of the gastric mucosa, from superficial irritation of the stomach lining to full-blown ulceration with perforation or penetration. They are caused by varying degrees of disruption of the aggressive and defensive factors that maintain the integrity of the mucosa. Aggressive factors include gastric acid and pepsin, and defensive factors include mucus and bicarbonate. For the urgent care practitioner, it is imperative to recognize the alarm symptoms that may represent more serious disease progression. Identifying patients who are less ill and may benefit from treatment, starting that treatment, and suggesting appropriate follow-up measures are the keys to urgent care management of these conditions.
Gastritis
The term gastritis encompasses a broad spectrum of entities caused by inflammatory changes in the gastric mucosa. The clinical presentation is similar for many of them, but it differs histologically when samples of inflamed tissue are viewed under the microscope. The inflammation may involve the entire stomach or only specific regions. Gastritis may be erosive (superficial, deep, or hemorrhagic) or non-erosive; the latter type is mostly caused by infection with Helicobacter pylori.
Gastritis is common in the United States, accounting for approximately 2 million physician visits annually. Patients older than 60 years are more likely than younger patients to have gastritis. The disease affects all age groups and both sexes. Although patients with H. pylori are more
likely to have gastritis, not all patients with gastritis will have positive test findings for H. pylori.1
Many factors can cause erosive gastritis (Table 1), although nonsteroidal anti-inflammatory drugs (NSAIDs) and aspirin are the most common agents. Both oral and systemic administration of these drugs at any dosage, either therapeutic or supratherapeutic, may cause gastritis. The gastric mucosa exhibits hemorrhages, erosions, and ulcerations when viewed on endoscopy.
Long-term effects include fibrosis and stricture.
| Table 1. Causes of Gastritis | |
Drugs
|
Ischemia Acute stress Infection
Radiation |
| Data from Soll AH, Vakil NB. Unusual causes of peptic ulcer disease. Waltham (MA): Wolters Kluwer Health, UpToDate. © 2015 [updated 2014 June 11; cited 2015 January]. Available from: http://www.uptodate.com/contents/unusual-causes-of-peptic-ulcerdisease? source=search_result&search=peptic+ulcer+disease&selectedTitle=6~150, and from Wehbi M. Acute gastritis. New York (NY): WebMD Health Professional Network, Medscape. © 2015 [updated 2014 September 18; cited 2015 January 8]. Available from: http://emedicine.medscape.com/article/175909-overview. NSAID = nonsteroidal anti-inflammatory drug; SSRI = selective serotonin reuptake inhibitor. |
|
The effect of H. pylori results from chronic rather than acute infection. It is usually acquired in childhood, and the percentage of infected individuals increases with age. It is found in 20% of those younger than 40 years with gastritis or PUD and in 50% of those older than 60 years. Transmission is thought to be from person to person through the oral–fecal route or through the ingestion of contaminated water or food. This explains the increased prevalence in lower socioeconomic groups. H. pylori infection is asymptomatic unless the patient has developed gastritis or PUD.
The acute symptoms of uncomplicated gastritis include abdominal pain, epigastric discomfort, nausea, vomiting, loss of appetite, belching, and bloating. Fever, chills, and hiccups may also be present. Symptoms may be indistinguishable from peptic ulcer disease, and no specific symptom makes one more likely than the other.2 Oddly enough, however, most patients with histologic evidence of acute gastritis are asymptomatic.1 The diagnosis is frequently made during endoscopy that is being performed for other indications.
History of Present Illness
In obtaining a thorough history of the current illness, ask about the following:
- Gnawing or burning epigastric discomfort that may be described as aching, as a hungry feeling, or as an empty feeling
- Nausea and/or vomiting
- Pain that awakens the patient at night
- Symptoms relief achieved with food, milk, or antacids
- Specific food intolerances, although no specific food is pathognomonic
- Previous history of gastritis, PUD, or H. pylori
- History of eating raw fish
- Exposure to aggravating drugs or chemicals such as NSAIDs or steroids, even a single dose
- Routine use of aspirin or NSAIDs
- Alcohol use, which may cause gastritis, generally considered a separate disease process (beyond the scope of this article)
- Alarm symptoms signifying more serious disease; these are the same as for peptic ulcer disease (Table 2)
Physical Examination
Be aware of the following points when conducting a physical examination:
- Normal findings are most likely
- Mild midepigastric abdominal tenderness
- More abnormalities may develop if the patient develops complications such as gastrointestinal (GI) bleeding, perforation, and penetration.
- Alarm findings on examination
- Hypotension
- Pallor
- GI bleeding or heme-positive stools
- Severe abdominal tenderness, rebound, guarding, or other signs of acute abdomen
Differential Diagnoses for Both Gastritis and
Peptic Ulcer Disease
Gastritis and PUD can be mistaken for quite a few entities:
- Dyspepsia
- Irritable bowel disorder
- PUD
- Cholelithiasis
- Crohn disease
- Gastric cancer
- Viral gastroenteritis
- Lymphoma
- Pregnancy
- Sarcoidosis
- Pancreatitis1,3
No work-up may be necessary in the urgent care center if the provider has a high index of suspicion and no alarm symptoms are present (Table 2). In the acutely ill patient, it may be helpful to rule out other disease processes with a complete blood count, liver and kidney function tests, amylase and lipase tests, pregnancy test, and stool test for occult blood. Tests for H. pylori (see the section “Testing for Helicobacter pylori”) may be indicated. Radiographic studies are generally not useful in an urgent care center unless it is suspected that the patient has a perforation. In that case, an upright chest radiograph will suffice to document the presence or absence of free air. Barium radiography may be of use diagnostically but should generally be ordered by the primary-care physician or gastroenterologist. The American Society for Gastrointestinal Endoscopy guidelines recommend endoscopy for patients older than 50 years with suspected gastritis or PUD with alarm features, such as weight loss and anemia (Table 2). Endoscopy should be considered in symptomatic patients who have negative findings for H. pylori, regardless of age.
Treatment of gastritis alone is strictly supportive, unless the disease is caused by H. pylori.4
NSAIDs, if being used, should be discontinued. When H. pylori is present, the patient should be treated for it. Fluids and electrolytes should be replaced if the patient is dehydrated, vomiting, and/or unable to take fluids by mouth. Acid blocking either with H2-blockers or proton pump inhibitors (PPIs) may be of benefit in patients in whom it is difficult to treat H. pylori, or in those patients suspected of having PUD.
H2-blockers provide competitive inhibition of histamine at the histamine-2 (H2) receptor, thereby decreasing gastric acid secretion. This effect suppresses basal gastric acid output as well as acid output stimulated by food and the neurologic system.
PPIs inhibit the proton (acid) pump in the secretory membrane of the parietal cells, thus completely inhibiting acid secretion. They have a long duration of action and are the most effective acid blockers. If cost is a concern, it is helpful to know that PPIs are more expensive than H2-blockers.
Practitioners should be aware that there is growing concern over the interaction between PPIs and clopidogrel and other antiplatelet agents. A decrease in the antiplatelet activity and increase in adverse cardiac events is possible because of an interaction between these 2 classes of drugs. Pantoprazole seems to be the safest choice in these cases.1 Consultation with the patient’s cardiologist is necessary if treatment with a PPI is unavoidable, as would be the case for a patient with gastritis with newly placed cardiac stents.
Peptic Ulcer Disease
PUD occurs most commonly in the stomach and proximal duodenum, and less commonly in the lower esophagus, distal duodenum, and jejunum. It is more common in patients with hyper secretory states such as Zollinger-Ellison syndrome, in patients with hiatal hernias, and in areas of ectopic gastric mucosa such as Meckel diverticulum. Approximately 500,000 persons in the United States are affected with PUD annually, and 70% of them are between the ages of 25 and 64 years. The direct and indirect health-care costs total over $10 billion annually. Fortunately the incidence is declining, likely due to the increased use of PPIs and the decreasing rate of H. pylori infection.3 Improving American diets and the decreasing incidence of smoking may also play a role.
Untreated ulcers may heal spontaneously, and then may recur within a few months. Some are highly symptomatic, and some are asymptomatic. Some ulcers are prone to complications, and some remain refractory to treatment. Prior ulcer history tends to predict future behavior.
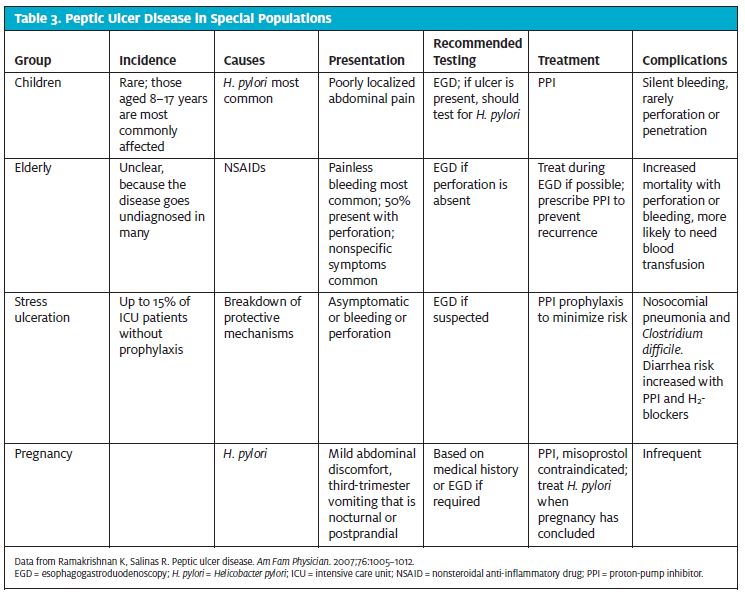
More than 48% of cases of PUD can be related to H. pylori infection, and 24% of the remaining cases can be related to NSAID use. Other less common causes include steroids, bisphosphonates, 5-flourourocil, stress, and malignancy. Comorbidities that increase the incidence of PUD include cytomegalovirus or tuberculosis, Crohn disease, cirrhosis, chronic renal failure, sarcoidosis, myeloproliferative disorders, critical illness, a stay in an intensive care unit, surgery, and hypovolemia causing hypoperfusion of the gastric mucosa.5 Smoking increases the risk of recurrence of PUD and slows the healing process in established ulcers. Table 3 outlines concerns of special populations with PUD.
Helicobacter pylori
Most patients with duodenal ulcers have documented H.pylori in their gastroduodenal mucosa; however, only 10% to 15% of patients with H. pylori infection actually develop PUD. It is believed that these patients are infected with a variety of H. pylori that has a chromosomal variance that increases its virulence and ulcerogenic potential. Persons with H. pylori have increased resting and meal-stimulated gastrin levels as well as decreased gastric mucus production and duodenal mucosal bicarbonate secretion, which contributes to ulcer formation. Eradication of H. pylori decreases risk of ulcer recurrence from 67% to 6% in duodenal ulcers and from 59% to 4% in patients with gastric ulcers.3 Relapse is generally the rule if H. pylori is not treated.
Nonsteroidal Anti-inflammatory Drugs
NSAIDs are the second most common cause of PUD. They cause peptic ulcer disease in two ways, first by direct contact, which causes submucosal erosions, and second, systemically by inhibiting cyclooxygenase, which decreases mucosal protection, bicarbonate secretion, epithelial cell proliferation, and mucosal blood flow. For this reason parenteral NSAIDs may be as deleterious as oral NSAIDs. H. pylori increases the intensity of NSAID damage. In chronic NSAID users, the annual risk of a life-threatening ulcer complication is 1% to 4%. Older patients are at highest risk. NSAID use is thought to be responsible for more than half of all perforated ulcers. PPIs and misoprostol minimize the ulcerogenic potential of NSAIDs and reduce ulcer recurrence in these patients.
Diagnosis
Diagnosis of PUD is usually based on clinical features and testing either with contrast radiographic studies or endoscopy. Signs and symptoms alone are generally unreliable, especially when differentiating gastric ulcers from duodenal ulcers.
The clinical features of PUD include episodic midepigastric pain described as gnawing or burning that occurs 2 to 5 hours after eating or when the stomach is empty. Pain may occur at night and awaken the patient from sleep. It may be relieved by food or antacids; this is the most specific finding for PUD and may help make the diagnosis. Other symptoms may include indigestion, vomiting, anorexia, fatty-food intolerance, a sensation of heartburn, and a family history of PUD. The physical examination is often nonspecific and may or may not include epigastric or left upper quadrant tenderness. Abdominal findings such as tenderness, including guarding and rebound, may be prominent in the case of perforation or penetration of the ulcer.
Older patients with PUD are more likely to have abdominal pain. Patients with duodenal ulcers are more likely to have pain relieved by food or antacids than are patients with gastric ulcers. Weight loss due to fear that eating will cause recurrent pain is more common in those who have gastric ulcers than in those with duodenal ulcers.
If the clinical presentation is consistent with PUD, assess the patient for alarm symptoms (Table 2). Any alarm symptoms should prompt further evaluation. Patients older than 55 years who have alarm symptoms should be referred to a gastroenterologist for urgent esophagogastroduodenoscopy (EGD). EGD is more sensitive than a radiologic contrast procedure and biopsy, and treatment can be performed during the test, essentially saving time and procedures. It is also more sensitive and specific. Patients younger than 55 years without alarm symptoms should be tested for H. pylori; NSAIDs should be discontinued for these patients, and so should use of alcohol and illicit drugs. In addition, the patient should start a trial of PPIs. Patients with positive test findings for H. pylori should be treated for infection and treated with a PPI for at least 4 weeks. Patients with persistent symptoms should undergo EGD at that point to rule out refractory ulcers and malignancy. Patients with gastric ulcers are at increased risk of developing gastric malignancy. Duodenal ulcers, however, are not at increased risk of malignancy.6
Testing for Helicobacter pylori
- pylori testing should be done in all patients suspected or confirmed to have PUD or gastritis. In most cases, this testing is not necessary in the urgent care center and can be left to the primary-care provider, unless it is the case that the patient is using an urgent care center for primary care, that they will not be seeing their primary-care provider before treatment must be instituted, or that blood is being drawn for another reason. Serum ELISA testing is the least accurate and should only be used for initial infection, but it is the most practical for urgent care use. Serum tests for H. pylori are useful only in patients who have never been treated before, because serum antibodies can remain positive for up to 3 years after eradication (Table 4). The urea breath test uses radiolabeled 13C or 14C urea taken orally. The bacteria then split the urea, which can be quantified in breath samples. This test is best used to confirm that treatment has successfully eradicated H. pylori. The stool antigen test for H. pylori is highly accurate, but it too is best used to confirm eradication. Endoscopic biopsy and staining is the first-line test for H. pylori. PPIs, bismuth, many antibiotics, and upper GI bleeding may lead to falsenegative test results. When a high index of suspicion is present, 2 negative sets of test findings are required to rule out H. pylori infection.5
| Table 4. Testing for Helicobacter pylori | ||||
| Test | Used For | Sensitivity (%) | Specificity (%) | Comment |
| Serologic ELISA | Initial testing | 85 | 79 | Cannot confirm eradication |
| Urea breath test | Confirm eradication | 95–100 | 91–981 | Expensive; must stop PPIs 2 weeks before test |
| Stool antigen test | Confirm eradication | 91–98 | 94–99 | Inconvenient |
| Urine-based ELISA/rapid urine test |
Initial testing | 70–96 | 70–96 | Convenient; cannot confirm eradication |
| Endoscopic biopsy, culture |
Both | 70–80 | 100 | |
| Endoscopic biopsy, histology |
Both | >95 | 100 | |
| Endoscopic biopsy, rapid urease (CLO) test |
Both | 93–97 | 100 | |
| Data from Data from Ramakrishnan K, Salinas R. Peptic ulcer disease. Am Fam Physician. 2007;76:1005–1012, and from Wehbi M. Acute gastritis. New York (NY): WebMD Health Professional Network, Medscape. © 2015 [updated 2014 September 18; cited 2015 January 8]. Available from: http://emedicine.medscape.com/article/175909-overview. Both = initial testing and confirm eradication; CLO = Campylobacter-like organism; ELISA = enzyme-linked immunosorbent assay; PPI = proton pump inhibitor. |
||||
The most common cause of H. pylori–negative ulcers are false negative test results for H. pylori and undiscovered NSAID consumption.5 In patients who are at high risk for H. pylori, positive findings on a single test confirms infection, whereas negative findings on 2 tests are required to rule out H. pylori infection. Treatment of Peptic Ulcer Disease Treatment of PUD is first focused at treating the underlying cause. NSAIDs or other inciting factors should be discontinued if possible. H. pylori should be treated for 10 to 14 days.
Treatment for Helicobacter pylori
Table 5 outlines standard treatments for H. pylori.
Adjunct treatments with prebiotics and probiotics may be helpful in increasing eradication rates and decreasing the side effects of treatment. Treatment failures are largely due to antibiotic resistance and patient noncompliance because of intolerable side effects.6
Testing for H. pylori eradication may be performed at 4 weeks after completion of therapy using either the rapid urease breath test or the stool antigen test. It may not be cost-effective and thus may be omitted in patients with uncomplicated gastritis whose condition improves with treatment. Patients with ulcers or cancer and those whose condition does not improve after treatment must be checked for resolution. Antibiotics and PPIs must be discontinued for 2 weeks prior to testing.
Other Treatment
H2-blockers or PPIs should be continued for 4 weeks because they induce healing in most duodenal ulcers.3 PPIs have superior acid suppression, healing rates, and symptom relief compared with H2-blockers and are recommended as first-line treatment for most patients. PPIs heal duodenal ulcers in more than 95% of patients by 4 weeks, and gastric ulcers in 80% to 90% of patients in 8 weeks. Maintenance therapy with either H2-blockers or PPIs is recommended to prevent recurrence in high-risk patients: those with a history of complications, frequent recurrences, negative test findings for H. pylori, refractory giant ulcers, or severely fibrosed ulcers. If H. pylori has been eradicated and the patient is no longer taking NSAIDs, no maintenance treatment is required.
| Table 5. Standard Treatments for Helicobacter pylori |
First-line therapy
Or
Second-line therapy for treatment failures
Or
Initial treatment in the penicillin-allergic patient
Or
Second-line therapy for treatment failures in the penicillin-allergic patient
Third-line treatment for when therapy has failed
|
| PPI = proton pump inhibitor. |
Antacids and sucralfate are superior to placebo in healing NSAID induced duodenal ulcers, but neither has been established as treatment for any other variety of ulcers. Because H2-blockers and PPIs are superior, sucralfate cannot be recommended as treatment.5 Antacids may be useful for symptom reduction.
Misoprostol is better than placebo for treatment of PUD, but has no advantage over H2-blockers and PPIs. It may be useful in non-menstruating patients who must take NSAIDs to prevent recurrent gastritis or ulceration. It is available in a combination NSAID product mixed with diclo fenac. It is contraindicated in pregnancy (category X) because it is an abortion-inducing agent.5
Gastritis and Peptic Ulcer Disease in Pregnancy
In a pregnant patient who develops PUD, treatment should be aimed at acid suppression. All of the PPIs are low risk in pregnancy, and are therefore category C. Most obstetricians will recommend them. Pregnant patients with positive test findings for H. pylori should be treated after delivery unless they are experiencing severe nausea and vomiting. There is some evidence that H. pylori contributes to hyperemesis gravidarum. Treatment with anti–H. pylori drugs, with the exception of tetracycline and bismuth, is generally safe in pregnancy, especially after 14 weeks’ gestation. Conversely, bismuth and metronidazole are unsafe in breastfeeding infants.5
Refractory Ulcers
Refractory PUD is defined as disease that fails to heal after 8 to 12 weeks of therapy. This may be due to persistent or resistant H. pylori infection, continued NSAID use, giant ulcers, cancer, tolerance of or resistance to medications, or hypersecretory states. The underlying cause should be addressed, and treatment should continue for longer than 8 weeks if required. These patients should be evaluated by a gastroenterologist.3,5
Surgery
Surgery may be required for patients who are intolerant of medications, do not comply with medication instructions, or are at high risk of complications, such as transplant patients, chronic steroid or NSAID users, those with giant gastric or duodenal ulcers, or those whose disease fails to heal with adequate treatment. Patients who experience relapse after multiple courses of medication should also be considered for surgery.3
Complications
About 25% of patients with PUD will have a serious complication such as hemorrhage, perforation, or gastric outlet obstruction (GOO). Silent ulcers and complications are more prevalent in older patients and in patients taking NSAIDs. Upper GI bleeding, which occurs in
12% to 20% of patients with PUD, is the most common cause of death and the most common reason for surgery.3 Patients may present with bright-red or coffee-ground hematemesis, melena, fatigue due to anemia, orthostasis, or syncope. Most patients in an urgent care center with documented GI bleeding should be transferred to an emergency department for further evaluation.
In stable patients with GI bleeding, ulcerogenic medications should be discontinued and a PPI should be administered. EGD should be performed as soon as possible. Testing and subsequent treatment for H. pylori should be done to prevent recurrent bleeding. If the patient must continue to take aspirin or NSAIDs, misoprostol or a PPI administered concurrently should be considered.
Perforation may occur in 2% to 10% of patients with peptic ulcers. It is usually found in the anterior wall of the duodenum (60%), the antral wall of the stomach (20%), or the lesser curvature of the stomach (20%).3 Perforation of ulcers in children is rare. Perforation into the peritoneum and resulting peritonitis constitute a surgical emergency. Perforation is characterized by sudden and rapidly spreading severe upper abdominal pain exacerbated by movement. It may radiate to the right lower abdomen or to both shoulders. Fever, hypotension, and oliguria suggest sepsis syndrome. Generalized abdominal tenderness, rebound tenderness, board like abdominal wall rigidity, and hypoactive bowel sounds may be masked in older patients and those patients taking steroids, immunosuppressants, or chronic narcotics. Upright or lateral decubitus radiographs or an erect chest radiograph may show pneumoperitoneum; however, its absence does not rule out perforation. Further testing with sonography, CT scanning, or gastroduodenography may be required.
GOO may occur from PUD, but it is the underlying cause in less than 5% to 8% of patients.3 Patients with recurrent duodenal or pyloric channel ulcers may develop pyloric stenosis because of inflammation, spasm, edema, or scarring and fibrosis. Symptoms of GOO include recurrent episodes of emesis with large volumes of vomit containing undigested food, bloating, fullness after eating, and early satiety. Weight loss, dehydration, and hypochloremic hypokalemic metabolic alkalosis may result. EGD or gastroduodenography is recommended to determine the site, cause, and degree of obstruction. Malignancy is responsible for more than 50% of GOO and should be ruled out. Other causes of GOO include acute inflammation or edema of the gastric mucosa due to H. pylori. No firm dietary recommendations are necessary; however, it should be noted that patients should avoid any foods that are known to precipitate their symptoms.5
Conclusion
Gastritis and PUD are due to an imbalance of the acid balance and the protective factors in the stomach. The most common causes are NSAID use and infection with H. pylori. The health-care provider should be aware of alarm symptoms that can point to more serious complications such as cancer, perforation, bleeding, and penetration. Treatment is aimed at removing the inciting factors, eradicating H. pylori if present, and acid suppression with H2-blockers or PPIs. Refractory or complicated cases should be evaluated by a gastroenterologist. Part 2 of this series will discuss gallbladder disease and acute pancreatitis.
References
- Wehbi M. Acute gastritis. New York (NY): WebMD Health Professional Network, Medscape. © 2015 [updated 2014 September 18; cited 2015 January 8]. Available from: http://emedicine.medscape.com/article/175909-overview
- Gratton MD. Peptic ulcer disease and gastritis. In: Tintinalli JE, Stapczynski JS, Cline DM, et al, editors. Tintinalli’s Emergency Medicine, 7th ed. New York, New York: McGraw-Hill Professional. 2010:554–557.
- Ramakrishnan K, Salinas R. Peptic ulcer disease. Am Fam Physician. 2007;76:1005–1012.
- Gratton MD. Peptic ulcer disease and gastritis. In: Tintinalli JE, Stapczynski JS, Cline DM, et al, editors. Tintinalli’s Emergency Medicine, 7th ed. New York, New York: McGraw-Hill Professional. 2010:554–557.
- Soll AH, Vakil NB. Unusual causes of peptic ulcer disease. Waltham (MA): Wolters Kluwer Health, UpToDate. © 2015 [updated 2014 June 11; cited 2015 January 5]. Available from: http://www.uptodate.com/contents/unusual-causes-of-peptic-ulcer-disease?source=search_result&search=peptic+ulcer+disease& selected Title=6~150
- Anand BS. Peptic ulcer disease. Medscape [website]. New York, New York: Medscape, LLC [accessed 2015 January 11]. Available from: http://emedicine.medscape.com/article/ 181753-overview#showall
- University of Texas at Austin, School of Nursing Family Nurse Practitioner Program. Recommendations in primary care for the most efficacious and cost effective pharmacologic treatment for Helicobacter pylori in non-pregnant adults. Austin, Texas: University of Texas at Austin, School of Nursing; 2013 May 17. Available from: http://www.guideline.gov/content.aspx?id=46427

