Published on
The Role of Ultrasound for Soft Tissue Infections in the Urgent Care Setting
Urgent Message: Abscess evaluation is one of many diagnostic applications of ultrasound that could improve patient care in the urgent care setting.
Authors: Staci Shepard, MS-4, and John Shufeldt, MD, JD, MBA, FACEP
Staci Shephard is a fourth-year medical student at Creighton University School of Medicine.
John Shufeldt, MD, JD, MBA, FACEP, is CEO of Urgent Care Integrated Network and sits on the Editorial Board of JUCM.
Consider this case scenario:
A 34-year old-man presents to the urgent care center with the complaint of an expanding, painful rash on his left arm. He states that 5 days ago he noticed a large pimple on his arm that he was not able to pop, so he decided to try to lance it with his pocket knife. He proceeded to “sterilize the blade” with rubbing alcohol and ran it over the flame of a lighter before cutting the lesion. There was blood but no purulent material expressed when the lesion was incised. The patient reports he has no past medical history. In particular, he is not a diabetic and to his knowledge, is not HIV-positive.
The man is afebrile, has a pulse of 88 and a blood pressure of 136/86. At present, the left arm has erythema surrounding a 1-cm laceration on the left forearm. This area is warm to touch and very tender to palpation, with no apparent loculations appreciated, however, the exam is limited by pain.
The challenge in this case is trying to determine whether the patient simply has increasing cellulitis or a deeper abscess that needs to be incised.
Patients often present to urgent care centers with soft tissue infections in the form of cellulitis or abscess. In these cases, hematologic markers such as white blood cell count and tests such as plain radiography contribute minimally to diagnosis, and providers are left to rely on physical exam and history for diagnosis. Differentiating between cellulitis and abscess is very important because their medical management differs. Cellulitis is treated with antibiotics alone, whereas abscess is treated with incision and drainage (I&D) of the infected site generally without antibiotics.1 Further, misdiagnosis could lead to delayed or lack of incision of an abscess, or conversely, subjecting a patient who does not have a collection of pus to an unnecessary procedure with no benefit.
Recent investigations of the diagnostic role of ultrasound (US) in differentiating between abscess and cellulitis have found that US has a higher sensitivity and specificity than physical exam alone in identifying abscesses. In addition, practitioners participating in these studies were physicians who had minimal specific training in US before using the tool for diagnosis, demonstrating that the skills can be acquired relatively easily with specific training.2,3
Abscess and Cellulitis
A number of studies have looked at the diagnostic utility of US in differentiating cellulitis from abscess formation. In an observational prospective study, Squire et al looked at 135 patients who presented with soft tissue infection and in whom both physical exam and subsequently US were used to determine presence of an abscess. The outcome measure for positive abscess was obtaining pus on incision and drainage (I&D). Of the 76 patients determined to have abscess based on physical exam, 14 had no signs of abscess on US. In eight of these 14 cases, the physician decided to change medical management to antibiotic treatment; three patients improved and five were lost to follow-up. In six patients, I&D was performed and in all those cases, no pus was extracted from the site. Four patients in that subgroup were determined to have an abscess based on physical exam and US findings but no pus was extracted. It was further noted that in three of these cases a hematoma was present. In the Squire et al. study, 59 patients that were diagnosed with cellulitis based on physical exam alone, of whom 10 showed signs of abscess on US with a negative physical exam. I&D was performed on nine of the 10 patients with discordant exam results and in eight patients, pus was expressed. Overall, this study demonstrated that US has a greater sensitivity and specificity (98% and 88% respectively), compared to physical exam (86% and 70% respectively). Moreover, all the physicians that participated in this study only had 30 minutes of US didactic training for abscess diagnosis with US and used an 8.0MHz or 10.0 MHz US probe.2
Similar results were also reproduced in an observational prospective study focusing on pediatric soft tissue infection by Iverson et al. in which the sensitivity and specificity were determined to be 97.5% and 69.2% for the US exam compared with 78.7% and 66.7% for physical exam alone. Further, in that study, when the US results were made known to the treating physician, I&D was averted in five of 43 patients who were determined to need I&D based on physical exam. This is of particular importance in the pediatric population, because in this group, I&D is usually done under conscious sedation, which represents an increased risk to a child. Again, in this study, the diagnosing physician was only given brief specific US training before using the tool for diagnosis.3
Further, it has been shown that when US is used as a diagnostic tool, the findings change medical management 48% to 73% of the time. This leads to fewer unnecessary painful I&D procedures as well as yielding fewer missed abscess.4,5 Multiple studies also have demonstrated that use of US is a skill that novice physicians can obtain.2,3,6 Another rare benefit of the technology is the ability to visualize complicating factors that necessitate transfer of care for abscess drainage. Hernia of bowel, pseudo-aneurysm and arterial blood flow all have been characterized on US in what clinically was a simple cutaneous abscess, demonstrating another utility for this type of exam.7
Diagnosing Abscess with Ultrasound
 Diagnosis of a superficial soft tissue abscess with US is very straightforward. It is best to use a high-frequency linear probe (8-12 MHz) and to lightly place the probe on the affected skin to visualize the superficial structures. At times it is hard to visualize structures that are very superficial, and therefore, too close to the probe. This can be corrected with an acoustic stand-off pad, which will produce an extra medium for the US waves to go through and helps focus an image that is very close to the surface of the skin. An air-free intravenous (IV) fluid bag can serve as a reasonable substitute for this purpose.8
Diagnosis of a superficial soft tissue abscess with US is very straightforward. It is best to use a high-frequency linear probe (8-12 MHz) and to lightly place the probe on the affected skin to visualize the superficial structures. At times it is hard to visualize structures that are very superficial, and therefore, too close to the probe. This can be corrected with an acoustic stand-off pad, which will produce an extra medium for the US waves to go through and helps focus an image that is very close to the surface of the skin. An air-free intravenous (IV) fluid bag can serve as a reasonable substitute for this purpose.8
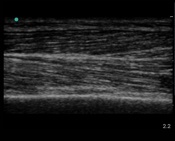
 On an US image, normal skin appears as a very organized structure, with the dermis and epidermis presenting as a bright hyperechoic lines separated by dark hypoechoic subcutaneous tissue (Figure 1).8,9
On an US image, normal skin appears as a very organized structure, with the dermis and epidermis presenting as a bright hyperechoic lines separated by dark hypoechoic subcutaneous tissue (Figure 1).8,9
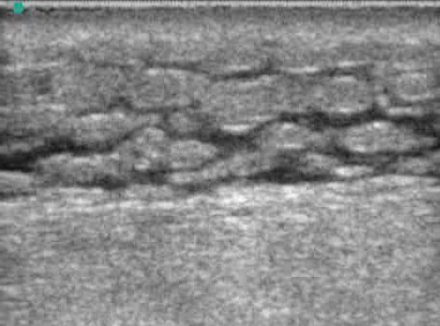
When cellulitis is present, the subcutaneous area will appear thicker than the contralateral normal skin. Often this thickening will begin to consolidate and produce “cobblestoning.” This sign is produced by stranding in the subcutaneous fat that appears on US as hypoechoic or anechoic lines. At the same time, the subcutaneous fat will become brighter and more echogenic (Figure 2). 8,10
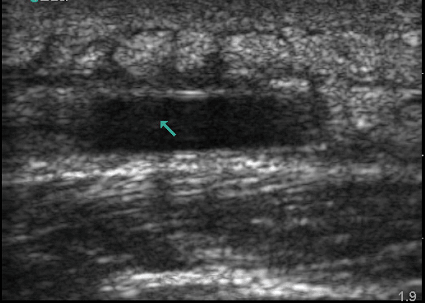 The usual US finding for abscess is a spherical or elliptical collection of dark anechoic or hypoechoic fluid. The fluid can either be uniform throughout or have areas with internal echoes producing a heterogeneous collection (Figure 3).10 Eliciting movement of the fluid pocket by gently compressing the skin with the US probe also helps facilitate diagnosis. The surrounding subcutaneous tissue of the collection will often appear hyperechoic and bright. When an abscess is identified, it is important to scan through it in two perpendicular planes to ensure that it is, in fact, an abscess and not a vessel. A vessel will be round in one plane and linear in another; conversely, an abscess will be round in both planes.11
The usual US finding for abscess is a spherical or elliptical collection of dark anechoic or hypoechoic fluid. The fluid can either be uniform throughout or have areas with internal echoes producing a heterogeneous collection (Figure 3).10 Eliciting movement of the fluid pocket by gently compressing the skin with the US probe also helps facilitate diagnosis. The surrounding subcutaneous tissue of the collection will often appear hyperechoic and bright. When an abscess is identified, it is important to scan through it in two perpendicular planes to ensure that it is, in fact, an abscess and not a vessel. A vessel will be round in one plane and linear in another; conversely, an abscess will be round in both planes.11
Ultrasound Training
The strong interuser variability in using US for diagnosis is well established but that should not discourage practitioners from integrating the technology into their practices. When looking at diagnosis of soft tissue infection specifically, studies have demonstrated the diagnostic utility of US in the hands of practitioners who received only 30 minutes to 2 hours of specific training.2,3,6 A number of recent studies have assessed the ability of medical students, residents, and practicing physicians to effectively learn and utilize focused US exams for a variety of organs with limited training.12 For example, in Croft LB et al. first-year medical students were able to accurately interpret focused echocardiograms over 80% of the time with handheld US devices after only 30 hours of didactic training.13 Although the echocardiographic exam does not directly relate to soft tissue infection, this demonstrates that focused US skills can be obtained with focused training. Further training in ultrasound can be obtained through a variety of CME courses. The American Institute of Ultrasound in Medicine has a variety of online and DVD educational materials that can be used for CME credit and the organization hosts an annual conference that provides hands-on training. More information can be obtained at www.aium.org. In addition, a variety of universities offer CME seminars directed at hands-on US training for physicians.14
US Devices and Other Applications
Handheld US devices are on the market starting at $8,000 new; quality used devices are available starting at $2,500. Multiple studies have investigated the utility of handheld sonography in a variety of clinical scenarios. Clinical applications include but are not limited to cardiac, abdomen, obstetric, and thoracic US.
Evaluation of first-trimester vaginal bleeding is another US application in the urgent care setting. In such cases, when US identifies an intrauterine pregnancy (IUP) and a fetal heart rate (FHR), referral can safely be made for outpatient follow-up with obstetrics. Further, the rate of concordance between emergency physicians and obstetricians for diagnosis of a viable IUP on US is 92%. The finding is also highly specific for absence of ectopic pregnancy. 15 In urgent care, the transabdominal US is preferrable to transvaginal US for viable IUP diagnosis because the exam is less invasive, does not require specialized probes, and requires less training to interpret. The disadvantage is that transabdominal US identifies 71.7% of IUPs with FHR compared with 93.5% found with transvaginal US exam.16 Although the detection rate is significantly less with the transabdominal approach, this modality can be easily implemented and will identify a large number of women that can be directly referred to obstetrics without evaluation in the emergency department (ED).
US-guided IV access can also benefit urgent care centers. One report found that the technology increases nursing staff’s ability to obtain peripheral access, resulting in obtaining access more quickly and with fewer attempts.17 It also enables technicians to gain proficiency in difficult IV placement with minimal training, freeing nursing staff for other tasks.18 US further enables the brachiocephalic vein to be accessed by the physician in patients with very difficult vasculature, preventing the need for transfer to the ED for line placement.
Conclusion
Soft tissue infections can often be misdiagnosed based on physical exam alone, resulting in incorrect treatment. That may lead to worsening infection and repeat visits by patients. It has been demonstrated in a number of studies that US is a reliable method for differentiating cellulitis from abscess and it performs notably better than physical exam alone.2-5 US is also beneficial for IV access and assessment of first-trimester vaginal bleeding with minimal provider education required for implementation. The technical skills required to perform such US exams can be quickly acquired and multiple options exist to obtain necessary skills through CME courses.14 This technology brings added benefit to patient care, with minimal provider education necessary for implementation, and therefore, should be considered for integration into the urgent care setting.
References
- Melton C. Soft Tissue Infection. in Tintinalli’s Emergency Medicine Manual. Eds. Cline D, Ma JO, Cydulka R et al. (McGraw-Hill, 2012) ed. 7 ch 90.
- Squire BT, Fox JC, Anderson C. Abscess: applied bedside sonography for convenient evaluation of superficial soft tissue infections. ACAD Emerg Med. 2005;12(7):601-606.
- Iverson K, Haritos D, Thomas R et al. The effect of bedside ultrasound on diagnosis and management of soft tissue infections in a pediatric ED. Am J Emerg Med. 2012;30: 1347-1351.
- Adhikari S and Blaivas M. Sonography first for subcutaneous abscess and cellulitis
evaluation. J Ultrasound Med. 2012;31:1509-1512. - Tayal VS, Hasan N, Norton J et al. The effect of soft-tissue ultrasound on the management of cellulitis in the emergency department. Acad Emerg Med. 2006; 13(4):384-388.
- Berger T, Garrido F, Green J et al. Bedside ultrasound performed by novices for the detection of abscess in ED patients with soft tissue infections. Am J Emerg Med. 2012;30:1569-1573.
- Blaivas M and Adhikari S. Unexpected findings of point-of-care superficial ultrasound imaging before incision and drainage. J Ultrasound Med. 2011;30:1425-1430.
- Ramirez-Schrempp D, Dorfman DH, Baker WE et al. Ultrasound soft tissue application in the pediatric emergency department: to drain or not to drain? Ped Emerg Care. 2009;25(1):44-48.
- Euerle M. (2008) Soft Tissue. Ultrasound Guide for Emergency Physicians. Retrieved March 28th, 2014, from http://www.sonoguide.com/soft_tissue.html.
- Soft-tissue Abscess. SinaiEm.us Retrieved March 28th, 2014, from http://new.sinaiem.us/tutorials/soft-tissue-abscess/
- Robben SG. Ultrasonography of musculoskeletal infections in children. Eur Radiol.
2004;14(suppl 4): L65-77. - Wong F, Franco Z, Phelan MB et al. Development of a pilot family medicine hand-carried ultrasound course. WMJ. 2013;112(6):257-261.
- Croft LB, Cohen LB, Dorantes TM et al. The echo-stethoscope: Is it ready for prime-time with medical students? J Am Coll Cardio. 2002;39:448A.
- CME. The American Institute of Ultrasound in Medicine. Retrieved March 28th, 2014, from www.aium.org
- Wong TW, Lau CC, Yeung A, et al. Efficacy of transabdominal ultrasound examination in the diagnosis of early pregnancy complications in an emergency department. J Accid Emerg Med. 1998;15:155-158.
- Kaur A, Kaur A. Transvaginal ultrasonography in first trimester of pregnancy and its comparison with transabdominal ultrasonography. J Pharm Bioallied Sci. 2011;3(3): 329–338.
- Blaivas M, Lyon M. The effect of ultrasound guidance on the perceived difficulty of emergency nurse-obtained peripheral IV access. J Emerg Med. 2006; 31(4):407-410.
- Bauman M, Braude D, Crandall C. Ultrasound-guidance vs. standard technique in difficult vascular access patients by ED technicians. Am J Emerg Med. 2009;27(2):135-140.
[taq_review]

