Published on
Urgent message: Tattoos and piercings are becoming commonplace, but patients who experience complications with these forms of body art may present to urgent care centers, as access to dermatology and plastics specialists frequently requires a referral or extended wait periods. The urgent care provider should possess a working knowledge about how tattoos and piercings are performed, how to recognize the complications, and how to treat them appropriately.
Tracey Quail Davidoff, MD
TATTOOS
Introduction
The term tattoo is derived from the Tahitian word tattau, which translates “to mark.”1 Tattoos occur when pigment granules are embedded into the skin either purposefully or accidentally. Purposeful tattoos have been performed for thousands of years to identify individuals, associate them with groups, for protection, and for artistic expression. Accidental tattoos occur when pigment, such as graphite, dirt, or other substances are ground into the skin during an injury. This article will focus on purposeful tattoos.
Previously in the Western world, decorative tattoos were primarily seen in men, especially in members of the armed forces or other groups to inspire solidarity. Beginning in the 1990s, tattooing gained more popularity and is now quite common in young people of both sexes, including professionals.
“Cosmetic” tattoos are tattoos performed in areas where makeup is typically applied. Also called permanent makeup, common sites include eye brows, eye liner, lip liner, and lip stick. Some may have birthmarks tattooed on their skin.
Reconstructive tattoos are done after cancer treatments to replace lost hair and pigmentation, either by surgical removal or loss due to chemotherapy. Examples include areola, brows, and eyelashes. Tattoos may also be used to mark areas undergoing radiation treatment.
A tattoo is created by using a pointed object to introduce particles of pigment into the dermis. In the most basic of forms, this is done by placing the pigment on the skin and using a pin or other sharp object to pierce the skin, allowing the pigment to enter the dermis and remain there permanently; examples include prison tattoos and self-made tattoos in adolescents, gangs, and persons who cannot afford a professional tattoo. Pigments used include the ink from a pen or graphite from a pencil, or mascara. On the other hand, professional tattoo artists use electric needles to inject the colored particles into the dermis.
Henna is a form of tattoo that does not require use of needles. Instead, temporary stains are applied to the skin (Figure 1); these wear off in days to weeks. Also called mehndi, henna is made from a vegetable dye made from hina, or the henna tree. This practice originated in the middle east and expanded to Asia and Africa. It is used to stain skin, hair and fingernails, as well as fabrics and leather. Henna pigment is applied as a wet paste to the skin and allowed to dry. The crusted pigment is then brushed off and the skin remains stained in the design applied.

Although there are generally few complications, in some cases the henna is mixed with p-phenylenediamine (PPD) to produce a blacker color. This can cause an acute allergic contact dermatitis which may even be associated with systemic reactions, such as generalized lymphadenopathy and fever.1 Experienced artists will not use PPD, and will make their own henna to be sure PPD is not present in the product.
Complications
The most common complication of tattooing is regret and dissatisfaction—for example, tattooing the name of a romantic interest with eventual termination of the relationship. Younger persons may tattoo images such as cartoon characters, musicians, or reflecting other interests that change as they age. Tattoos placed in areas such as the neck, face, or hands cannot be covered and may prevent job advancement; tattoo artists call these “career enders.” Sometimes the image does not turn out as the person intended, is off center or crooked, or was poorly done. Most tattoos will fade or stretch over time, especially if the person gains weight. The only corrections for these problems are modification of the original tattoo (by tattooing over the original tattoo) or removal.
Medical complications from decorative tattooing in the developed world are surprisingly rare, but as the incidence of tattooing increases, so do the complications. In most countries, there are few regulations promoting safe tattooing, making complications more common.1 The introduction of foreign substances into the skin can result in toxic or immunologic reactions to the pigment, transmission of infections in the event of improper sterilization, and the localization of skin disease within the tattoo. Immunologic reactions include acute inflammatory reactions and allergic hypersensitivity.
Acute inflammatory reactions can occur due to the physical tissue injury of the skin, or reaction to the dyes or metals used to produce the pigment. These reactions usually resolve spontaneously in about 2-3 weeks and are expected adverse events of the tattooing process. (See Figure 2 and Figure 3.)


Infection can occur due to a break in the skin, as in any other skin injury. This can result in cellulitis, fasciitis, and even sepsis. The most common pathogens are Staphylococcal and Streptococcal species, including MRSA. Improper disinfection of the skin prior to tattooing, as well as improper aftercare, can contribute to infection.1 There have been reports of Vibrio vulnificus infection causing sepsis and death from swimming in ocean water with a recent, unhealed tattoo.2 Transmission of blood-borne diseases such as tuberculosis, syphilis, hepatitis B and C, and HIV have also been reported from tattooing, most likely from using improperly sterilized needles; occurrence of these events is unknown. In some areas, persons with recent tattoos are prohibited from giving blood for fear of transmitting hepatitis and HIV. Person-to-person transmission of viruses such as vaccinia and HPV have also been reported.3 Infectious agents may also be present in ink; it is estimated that approximately 10% of new inks are contaminated with pathogenic bacteria.4 Trauma to the skin can also reactivate infections such as HSV and VZV.1 Leprosy has been reported related to tattooing in India.1
Later reactions include an allergic sensitivity to the elements of the pigment in the tattoo. Red pigments are a common offender. This results in acute or chronic contact dermatitis or a photoallergic dermatitis. This can manifest as localized eczematous eruptions or as an exfoliative dermatitis. Photoaggravated reactions are most commonly caused by yellow pigment, which contains cadmium sulfide, a chemical used in photoelectric cells. Reactions to green, blue, and black pigments are much less common. Green tattoos have been linked to eczema at the site of the pigment, as well as more generalized eczematous reactions.5 Blue pigments containing cobalt aluminate may cause a localized hypersensitivity, and rarely uveitis. Allergic reactions to black pigment are very rare, and presumably due to a sensitivity to carbon.

Granulomatous reactions can occur due to any pigment, and in rare cases can be linked to sarcoidosis. Such cases may warrant further investigation for systemic sarcoid. Lichenoid reactions are even less common and may be related to a delayed hypersensitivity, similar to a graft-vs-host reaction, with mercury found in red pigment the most common offending agent. The area of red in the tattoo is usually affected, but warty papules or plaques may be more generalized.6 Pseudolymphoma-like lesions may also occur as red nodules in or around the tattooed area.
Several generalized cutaneous disorders also show affinity for tattooed skin. Lichen planus, psoriasis, sarcoidosis, and lupus erythematosus have all been shown to localize to tattooed skin. Other trauma-related lesions may occur (eg, keratoacanthoma, squamous carcinoma, basal cell carcinoma, and melanoma). Primary melanomas may be difficult to see if they lie within a tattooed area, preventing timely diagnosis. The carcinogenic effects of the deposited metal in the pigments are unknown.
Newly tattooed skin should be covered with petroleum jelly to prevent oozing of serosanguinous fluid if this has not already been done by the tattoo artist or the patient. The area should be cleaned twice daily with a gentle antimicrobial soap and the petroleum jelly reapplied. The patient should avoid contact with the tattoo except for cleaning. Tattoos generally take about 2 weeks to heal. Patients should be instructed to avoid baths, swimming, and sun exposure, and to wear loose clothing that will not stick to the tattoo.
| Table 1. Tattoo Pigments | |
| Black | Carbon (India Ink), iron oxide, logwood |
| Blue | Cobalt aluminate |
| Brown | Ferric oxide, silica |
| Green | Chromic oxide, lead chromate, phthalocyanine dyes, malachite |
| Purple | Manganese, aluminum |
| Red | Mercuric sulfide (cinnabar), sienna (ferric hydrate), sandalwood, brazilwood, organic pigment, cadmium red |
| White | Titanium oxide, zinc oxide, lead white |
| Yellow | Cadmium sulfide |

Treatment of Complications
Infections should be treated as any other skin infection (eg, abscess and cellulitis). Incision and drainage may be necessary. Wound cultures may be helpful to guide treatment. Cellulitis may require IV antibiotics in severe cases or disseminated infection. Empiric antibiotic choices in accord with local recommendations and antibiograms should be aimed at the usual suspects: Staphylococcus, Streptococcus, and MRSA.
Topical, intralesional, and, rarely, systemic steroids may be useful in inflammatory cases. Remember, nothing stronger than 1% hydrocortisone should be used on the face, and for the shortest time possible.
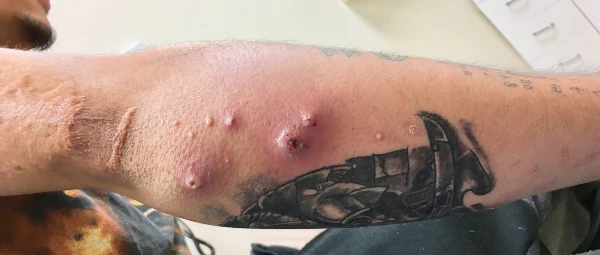
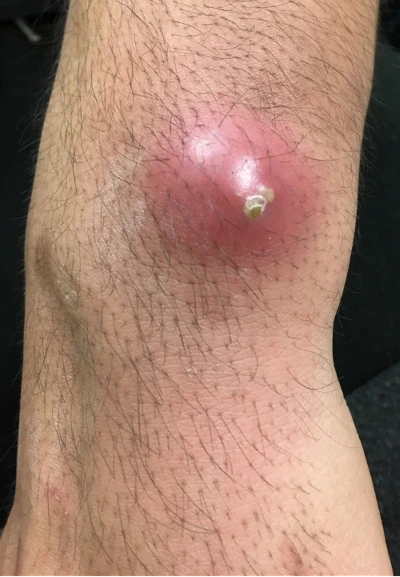
Figure 6. Right elbow with multiple abscesses 1 week after tattooing. The patient had abscesses at distant sites (Figure 7), indicating bacteremia. Cultures from the abscess, as well as blood, were positive for CA-MRSA.
Tattoo Removal
Removal is usually sought for social or aesthetic reasons, regret being the most common. Although a variety of treatments to remove tattoos has been described in the past, the Q-switched ruby laser has been the most successful. Multiple treatments are required, and complete resolution of color may not be achieved in all cases. Some scarring or “ghost” of the previous pigment may remain. Recently developed picosecond lasers have been showing more promise. In both cases, the laser causes the pigments to become extracellular, and then drained through the lymphatic system or by formation of a scale-crust. Rarely after removal, tattoo pigments can be found in lymph nodes and be confused with metastatic changes.1
Special tattoo inks can be more easily destroyed during laser treatments. These are bioresorbable dyes encapsulated in beads with pigments specially designed to permit targeting of the tattoo by specific laser wavelengths.1 They are easier to remove than standard tattoo ink.
Acute complications of laser tattoo removal include pain, blistering, crusting, and pinpoint hemorrhage. Rarely, laser removal attempts may cause permanent darkening of the tattoo. Localized reactions may become more generalized. Scarring may occur. Amateur tattoos are easier to remove than professional tattoos,1 as they are not placed as deep in the dermis. Cosmetic tattoos are more difficult to remove because they contain iron or titanium oxide, which becomes darker when exposed to the laser.
PIERCINGS
Introduction
The trend of piercing areas other than the ear lobe has increased in the last 2 decades and is now commonplace. Between 25% and 35% of adolescents and young adults between the ages of 13 and 29 have body piercings at a site other than the ear lobe,7 including the tongue, lips, nose, eyebrows, nipples, navel, and genitals. Complications can include local and systemic infections, poor cosmesis, and foreign body rejection. Swelling and bleeding (generally, site-specific) can occur with complications. Patients who present with complications, or who inquire in advance of piercings, should be counseled so they can make informed decisions before undertaking piercings in the future.
The jewelry used to pierce varies by site, and may include hoops, studs, and barbell-shaped devices that may be straight or curved. Tongues are usually pierced with straight barbells, umbilical piercings use curved barbells, noses may be studs or hoops in the nostril, and curved barbells or rings in the nasal septum. Genitals and nipples may be rings or barbells. Options for ears are many, based on patient preference and location.
Jewelry is usually made from stainless steel, gold, niobium, titanium, or various other alloys. Contact allergies are common when alloys containing nickel are used. Rarely, plastic is used. Some may have a mechanism to keep them in place, such as screw backs, and others are more easily removed (eg, spirals, hooks, or rings). Jewelry with locking backs is recommended for piercings in small children to prevent aspiration, choking, or loss.
No reliable estimates are available for the number of persons who have experienced complications related to body piercing.8 Patients who are vulnerable to infection and susceptible to hemorrhage are at greater risk of complications from piercing.
Site-Specific Concerns
Ear
Traditionally, a single piercing in the lobe was the only socially acceptable piercing in Western society. Multiple piercings within the lobe are now common, as are “high” ear piercing in the chondral cartilage. Up to 35% of pierced ears may have complications; 77% would be considered minor infections, 43% allergic reactions, 2.5% keloid formation, and 2.5% traumatic tearing.8 Stretching of the hole is also common, especially when large, heavy earrings are worn; this increases the risk of tearing.
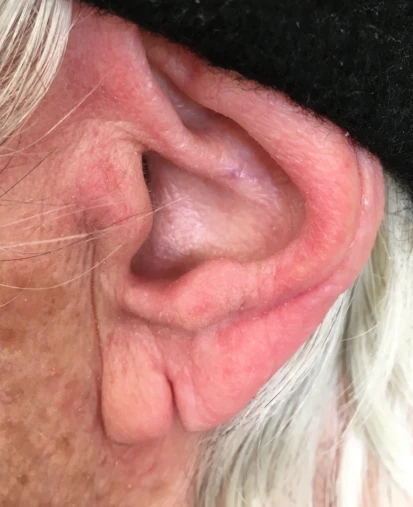
High piercings are associated with poor healing and infection due to the avascular nature of the chondral cartilage. More serious infections may result in disfigurement from perichondritis, causing some degree of cauliflower ear. Patients with perichondral infection, as opposed to a superficial infection, will have pain with deflection of the ear. The most common pathogens are the usual skin suspects, including Staphylococcus aureus and Streptococcus pyogenes, but the high piercings are also prone to Pseudomonas aeruginosa. Antibiotic choices should be tailored to location, with ciprofloxacin or another skin fluoroquinolone being used if chondral infection is suspected. Abscesses should be incised and drained. If an abscess develops in the upper ear, scarring and perichondritis may result in a poor cosmetic outcome.
Earrings and their backings can become embedded in the skin, especially the fleshy ear lobe, either due to inflammation, from trauma, or if the patient is careless when removing the jewelry; this may also be a complication of using piercing guns.8 Using longer earring posts when piercing can prevent this. Gentle probing may facilitate removal of the embedded jewelry, but in some cases local lidocaine and a small incision may be required to locate and remove embedded object.8
Patients with atopic dermatitis or a history of contact dermatitis are more likely to develop minor skin infections related to piercings, but it may be difficult to differentiate contact dermatitis from superficial infection.
Superficial infections may be treated with local cleaning, moist packs, and over-the-counter antibiotic ointment or mupriocin. Contact dermatitis should be “treated” with switching the jewelry to a different metal that is less allergenic, and topical steroids. The skin surrounding silver jewelry may develop argyria, a greyish discoloration, which should also resolve when the jewelry is removed.
Tongue and oral
The infection rate of oral piercings is surprisingly low, despite the number of bacteria in the mouth. Rinsing with dilute antiseptic mouthwash or carbamide peroxide oral rinse can reduce the rate of infection while the fresh piercing heals. Ludwig’s angina, a rare type of deep tissue infection in the submandibular space, is a possible complication and may be life threatening if not identified and treated aggressively. Airway compromise is possible with spread to the mediastinum; surgical debridement and IV antibiotics are urgently required.8 However, tongue piercings can initially result in swelling that can be uncomfortable and make eating and drinking difficult. Ice and a soft diet may be advised. Experienced piercers will use a longer barbell for piercing and switch to a shorter one when the swelling subsides. Rarely, tongue swelling can cause airway compromise. Tooth chipping from the piercing is so common it should be expected.
Nose
Nose piercings can be either at the lateral nares or the base of the cartilaginous septum. Piercing of the cartilage can cause a fair amount of bleeding, a septal hematoma, and infection. Perichondritis can also occur in this location and should be treated for possible Pseudomonas infection. Aspiration and embedding of the jewelry may also occur in this location. (See Figure 10.)
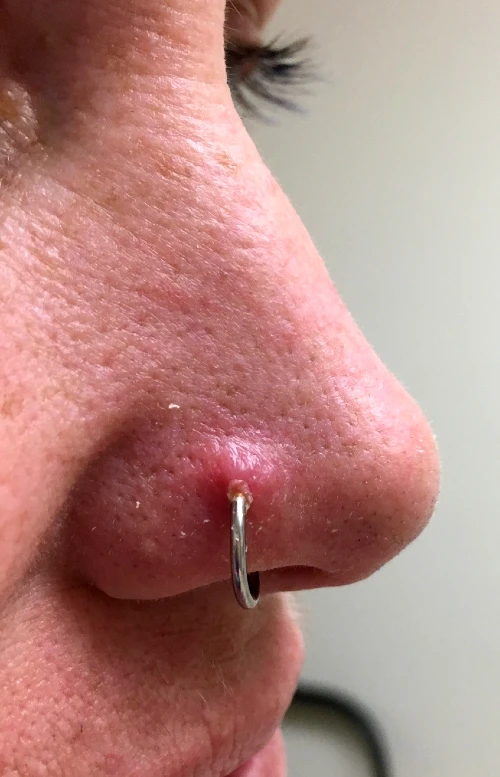
Navel
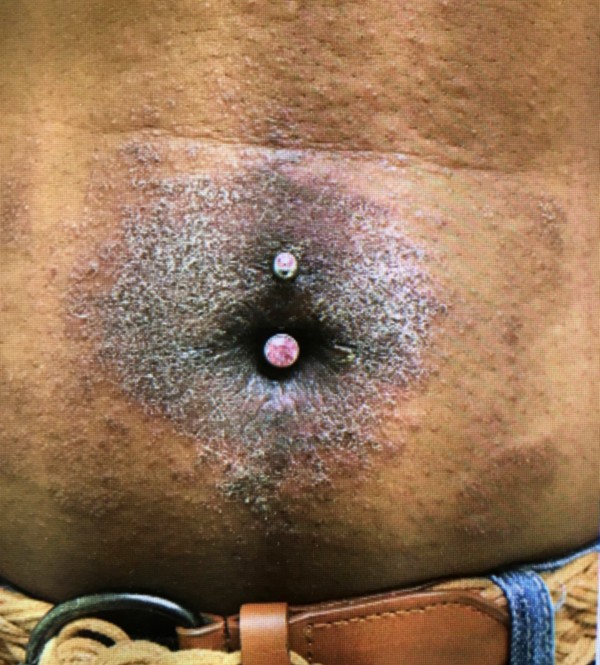
The navel is a popular site of piercing in young girls, and is often pierced unprofessionally, either by the patient or their friend. The jewelry may rub on clothing or be compressed in tight clothing and is prone to trauma from the waistband. If placed too superficially, the jewelry may migrate to the skin surface. Weight gain and pregnancy can contribute to this problem. Curved barbells are less likely to migrate.
Nipple
Nipple piercings may take 2-4 months to heal properly. Patients should be prepared for this. Infection including abscess formation and cellulitis is possible. There is no information about piercing nipples of breasts that have had augmentation. Scar tissue could impair latching or milk flow when attempting to breast feed.8
Genitals
The purpose of genital piercing is to enhance sexual sensitivity. Sites in men include the glans, foreskin, and scrotum. In women the clitoral prepuce or body, labia minora or majora, and perineum may all be pierced. Genital piercings may take several months to heal.
Concerns common to all sites
Hypertrophic scarring and keloid formation may occur; the ear lobe is a common site for this. The keloid may itch or hurt. Treatment includes intralesional steroid injections and surgical excision, but the keloid frequently recurs. Patients who are predisposed to keloids (eg, those of African descent and patients who have had keloids in the past) should be aware of this complication before piercing.
If inflammation and infection are severe, the jewelry should be removed. If the patient wishes to maintain the piercing, a 20 g Teflon IV catheter can be used to thread surgical silicone into the opening. Nylon suture material can also be used to keep the opening patent while healing occurs.8 If the patient no longer desires the piercing, the jewelry can be removed, and the hole allowed to close. If the piercing is then again desired, it can be re-pierced when healing is complete (in ≥6-8 weeks, depending on location).
Mild infections can be treated with diligent cleaning and topical antibiotics such as bacitracin or mupirocin. If oral antibiotics are required, they should have good Staph and Strep coverage, including MRSA coverage, if it is prevalent in the area. Choices may include a first-generation cephalosporin such as cephalexin or cefadroxil, clindamycin for those who are allergic, and either trimethoprim/sulfamethoxazole or doxycycline if MRSA coverage is desired.
Trauma to a piercing site is common and can result from falls, accidents, contact sports, violence, or accidental pulling. The area should be cleaned and repaired as soon as possible. If the provider is not comfortable repairing the area, the patient should be referred to the emergency department or a plastic surgeon. If the opening is damaged, the area can be re-pierced after healing, in about 6-8 weeks.
| Table 2. Common Complications of Piercings, by Site | |
| Site | Complication |
| Ear | Allergic reaction, embedded earrings, infection, keloid, traumatic tear |
| High ear | Auricular perichondritis, perichondral abscess, pain |
| Female genitals | Allergic reaction, compromise of barrier contraception, infection, keloid formation |
| Male genitals | Frictional irritation, infection, paraphimosis, penile engorgement, priapism, condyloma, urethral rupture, urethral stricture, urinary flow interruption |
| Mouth | Airway compromise, alteration in eating, gingival trauma, hematoma formation, increased salivation, infection, injury to salivary glands, loss of taste, Ludwig’s angina, pain, permanent numbness, speech impediments, tooth chipping or fracture, uncontrolled drooling |
| Navel | Bacterial endocarditis, frictional irritation, infection, jewelry migration and rejection |
| Nipples | Abscess formation, bacterial endocarditis, breastfeeding impairment, infection |
| Nose | Infection, jewelry swallowing or aspiration, perichondritis, and necrosis of nasal wall, septal hematoma formation |
Other Types of Piercings
Gauges
Gauges are another type of piercing—usually in the ear lobe, in which larger and larger jewelry is introduced into the hole, gradually increasing the size. This is usually done every 4 to 6 weeks. Large discs or rings are then inserted into the hole to hold the shape. Some of these can be quite large, as this skin has great potential to be stretched over time. Infection is very uncommon after the initial piercing because increasing the size does not produce a break in the skin. When the gauge is no longer desired, a large hole with stretched out skin remains; surgical repair is necessary to restore the ear lobe to its normal size. (See Figure 11.)

Dermal implants
Dermal implants are another type of piercing in which a tool is used to place a backing under the dermis, then a post-type stud can be screwed into the backing. These can be introduced anywhere. Complications include infection, migration, scarring, granuloma formation, pain, and chronic irritation, depending on location. (See Figure 12 and Figure 13.) The stud can be unscrewed and removed, but the backing remains under the skin, requiring a minor procedure to remove it. The area can be field blocked with lidocaine, a small incision made with a scalpel, and then the back can be pulled out with forceps. Blunt dissection may be required, as may a suture or two to close the skin following removal. Infection may require skin-specific antibiotics.
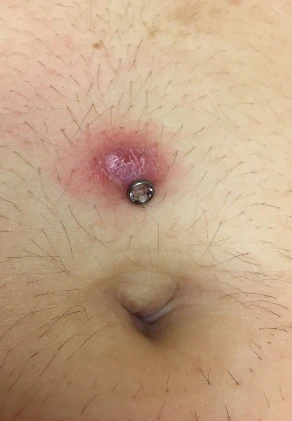
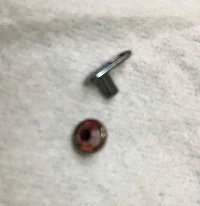
Fins, spikes, and horns can all be added as deep dermal implants and are generally not removable; these are beyond the scope of this article.
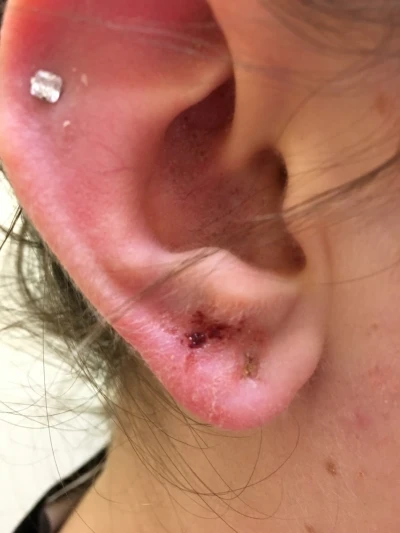
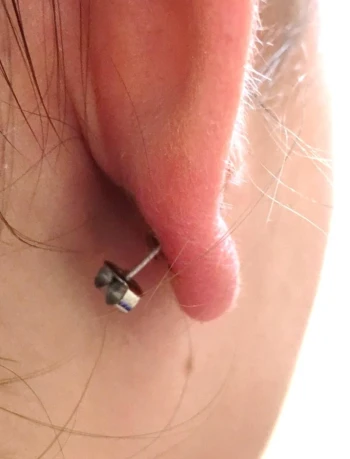
Figure 14 and Figure 15. Cartilage piercing; stud type earring embedded in ear lobe.
Patients should have been counseled at the time of piercing that the skin should be cleaned twice daily with antimicrobial soap and water, and that contact with the freshly pierced site should be avoided except for cleaning. Ask if they’ve used commercial products sold at piercing and jewelry shops. Generally, these are to be avoided because they contain benzalkonium chloride, which does not have activity against Pseudomonas sp, and may be contaminated.7
Most patients will know how their jewelry is removed, but may need instruction if it is new, or if they had inadequate education after the procedure. The process varies according to the type of jewelry. For example:
- Studs have backings that are simply pulled off, or screwed on and off.
- The ends of barbells usually screw off, allowing the jewelry to be removed.
- Hoops bend, revealing the opening, similar to a keyring.
- Gauges are removed by stretching the earlobe.
- Spirals are removed by rotating and pulling the jewelry until it is removed.
- Embedded and bent jewelry may need to be manipulated, cut with wire cutters, bent using pliers or needle drivers, or disassembled to be fully removed.
Rarely, dissection similar to removing a splinter or other foreign body is necessary. Topical or local anesthesia may facilitate removal. Some creativity may be required.
Summary
Urgent care providers will likely encounter patients presenting for management of the complications associated with body art. Patients should be counselled about the potential health risks of piercings and tattoos. The urgent care provider needs to be aware of the complications that can occur and how to treat them. Familiarity with the specific jewelry and how to remove it, how to treat infections, and recommending cleaning procedures is good practice.
Additional Resources
- Alliance of Professional Tattooists, Inc.; www.safe-tattoos.com.
- Association of Professional Piercers; www.safepiercing.org.
- S. National Library of Medicine. Piercing and tattoos. Available at: www.nlm.nih.gov.
Take-home points
- Acute inflammatory reactions such as redness, oozing, and swelling are expected results of the tattooing process and do not require treatment other than local care.
- Careful hygiene, including washing with antibacterial soap and water, and applying petroleum jelly twice daily can prevent infectious complications of tattooing.
- Infections related to tattooing and piercing should be treated as any other skin infection, with coverage for Staphylococcal and Streptococcal species, including MRSA.
- Tooth chipping is an expected complication of tongue piercing.
- Piercing-related trauma should be repaired as soon as possible.
- Infections in sites of cartilage piercings should be treated with a skin fluoroquinolone such as ciprofloxacin. Deformities are common following the treatment of such infections.
References
- Khunger N, Molpariya A, Khunger A. Complications of tattoos and tattoo removal: stop and think before you ink. J Cutan Aesthet Surg. 2015; 8(1):30-36.
- Hendren N, Sukumar S, Glazer CS. Vibrio vulnificus septic shock due to a contaminated tattoo. BMJ Case Rep. 2017 May 27. 2017:[Medline].
- Baxter SY, Deck DH. Tattoo-acquired verruca plana. Am Fam Physician. 1993;47(4):732.
- Serup J. Tattoo infections, persona resistance, and contagious exposure through tattooing. Curr Probl Dermatol. 2017;52:30-41.
- Jacob SE, Castanedo-Tardan MP, Blyumin ML. Inflammation in green (chromium) tattoos during patch testing. Dermatitis. 2008;19(5):E33-4.
- Taafe A, Wyatt EH. The red tattoo and lichen planus. Int J Dermatol. 1980;19(7):394-396.
- Desai N. Body piercing in adolescents and young adults. UpToDate. Available at: https://www.uptodate.com/contents/body-piercing-in-adolescents-and-young-adults?search=piercing&source=search_result&selectedTitle=1~53. Accessed January 9, 2018.
- Meltzer DI. Complications of body piercing. Am Fam Physician. 2005;72(10):2029-2034.
Citation: Davidoff TQ. Tattoos and piercings: what the urgent care provider needs to know. J Urgent Care Med. April 2018. Available at: https://www.jucm.com/tattoos-and-piercings-what-the-urgent-care-provider-needs-to-know/.

