Published on
Urgent message: Patients with imminently life-threatening conditions can present to an urgent care appearing to be in good health or even with a viable alternative explanation for their symptoms. It is important to be vigilant for red flags of serious illness.
ARASH MIRZAIE, MS4, and MICHAEL WEINSTOCK, MD
Headache is one of the most common presenting complaints in ambulatory settings. Urgent care providers must rapidly evaluate and diagnose a variety headache types in a time-limited environment. Subarachnoid hemorrhage (SAH), a potentially life-threatening condition, can simply present as a sudden-onset headache without abnormal vital signs or neurologic deficit, and thus misdiagnosis is not uncommon. Failure to be on the lookout for such an insidious condition can lead to devastating consequences.
Case Presentation
A 34-year-old healthy-appearing woman presents to the urgent care center, accompanied by her husband, and says that she has had an allergic reaction to chocolate. She reports that an hour earlier, she and her friends were playing volleyball. After the game, she ate a small piece of chocolate, and soon after, she developed severe nausea, vomiting, and a “bad headache” at the base of her skull. She has associated photophobia. There are no significant findings in the review of systems. Her past medical history reveals that she has had migraines. She has no history of allergies to medicines or foods, and she takes no chronic medications. She reports that she does not smoke and does not drink alcohol.
Physical Examination
At initial presentation, the patient’s vital signs are as follows:
- Blood pressure: 138/84 mm Hg
- Respiratory rate: 16 breaths/min
- Temperature: 99.3°F (37.4°C)
- Pulse: 98 beats/min
- Body mass index: 24 kg/m2
The patient lies on the examination table in the fetal position and asks that the room lights be dimmed. Findings on examination of her head, eyes, ears, nose, and throat are normal. A neurologic examination shows that she is alert and oriented to person, place, and time, and that function for cranial nerves III through XII are within normal limits. Her muscular strength is normal for flexion and extension in all extremities.
Urgent Care Course
Intramuscular administration of 8 mg of ondansetron was ordered. After 15 minutes, however, the patient still had severe nausea and periodically gagged and vomited. The patient was advised that further imaging studies were necessary because the cause of her illness was unknown. She consented to transportation to a local emergency department (ED) by paramedics.
Emergency Department Course
After providing her medical history and undergoing a physical examination and initial blood tests, the patient underwent a noncontrast computed tomography (CT) brain scan, which revealed SAH. Magnetic resonance angiography was performed to localize the source of bleeding, but findings were inconclusive. The patient did not undergo lumbar puncture. She was given nifedipine to prevent cerebral vasospasm. She underwent repeat brain-imaging studies, which showed resolution of her bleeding. After 5 days, she was discharged home in stable condition without any pain or headache. She did not develop any disabilities as a result of her SAH.
Discussion
Anatomy and Definition
The organs of the central nervous system are covered by three protective membranes referred to as meninges. The order of the meningeal membranes, from deep to superficial, is pia mater, arachnoid mater, and dura mater. The space between the pia and the arachnoid mater is referred to as subarachnoid space, which is the location of the interface between the cerebrospinal fluid and the blood vessels. SAH is usually due to rupture of a saccular aneurysm, causing hemorrhaging in this space. SAH leads to mixture of blood with cerebrospinal fluid.
Epidemiology
Headache is one of the most commonly reported symptoms in EDs, accounting for approximately 2% of chief symptoms. SAH, a potentially life-threatening and disabling condition, has been identified as a cause of headache in 1% of patients whose chief presenting symptom to EDs is headache. Almost 50% of patients with SAH will have normal findings on examination and normal vital signs at initial presentation. SAH has a high mortality rate; between 25% and 50% of patients with this condition die within 6 months of diagnosis, and about 25% of patients who live end up with a neurologic deficit.1 That is why prompt diagnosis and awareness of the limitations of diagnosis are so important.
Clinical Presentation
SAH commonly presents as a sudden-onset headache that may or may not be accompanied by nausea, vomiting, and neck stiffness. In a prospective study of 109 patients with sudden-onset headache, SAH was the cause in 25%, of which 23% reported only headache without nausea, vomiting, or neck stiffness.2 Many patients with SAH will have an altered level of consciousness; seizures occur during the first 24 hours in about 10% of these patients. Coma is uncommon; about 10% to 15% of patients die before reaching a hospital.3
The four strongest independent risk factors for SAH are4
- Smoking
- A family history of SAH
- Hypertension
- Hypercholesterolemia
The risk factors of genetic origin affect blood vessel walls, commonly associated with autosomal-dominant polycystic kidney disease and Ehlers-Danlos syndrome.4
Diagnosis
It is easy to determine the need for further work-up when a patient presents with headache and a new neurologic deficit. However, when the only presenting symptom is headache, without neurologic deficit, as occurs in half of all patients with SAH, solving the mystery is much more difficult.5 If the diagnosis is missed in such patients, they are highly likely to have a poor outcome. A history of sudden-onset headache or a report of “the worst headache of my life,” regardless of headache severity, should be enough cause for a clinician to suspect SAH and to seek a more detailed history and physical examination, specifically targeted for signs and symptoms of SAH, such as nausea, vomiting, mental status change, seizure, and a history of loss of consciousness.
Because nearly half of all patients with SAH will have normal examination findings and normal vital signs on initial presentation, misdiagnosis of SAH is not uncommon. Other reasons for misdiagnosis include
- Failure to recognize the wide spectrum of clinical presentations of SAH6
- Failure to obtain a CT scan or to understand its limitations in the diagnosis of SAH
- Failure to perform a lumbar puncture or, if the procedure is performed, failure to correctly interpret its results
In a hospital-based series of 482 patients admitted with SAH, initial misdiagnosis occurred in 12% and was mostly associated with small-volume SAH and normal mental status at presentation. Failure to obtain a head CT scan was the most common factor leading to misdiagnosis, accounting for 73% of patients with misdiagnoses and leading to a fourfold increase in mortality rate for those with SAH.6
Diagnostic Modalities
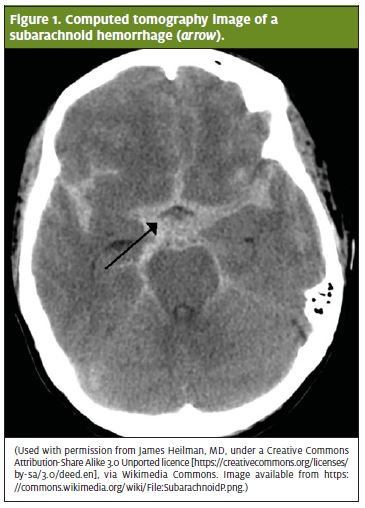
When SAH is suspected, the first test most commonly done is a noncontrast CT scan of the brain. If findings are negative, a lumbar puncture is performed to evaluate for the presence of red blood cells or xanthochromia. Lumbar punctures, however, are painful and may extend the duration of stay in the ED or can even lead to a post-procedure headache. The sensitivity of modern CT for identifying SAH in neurologically intact patients in the ED was evaluated in a recent prospective cohort study. The authors found that a CT scan performed within 6 hours of headache onset had a sensitivity of 100% and specificity of 92.9% for pinpointing SAH.1 Figure 1 shows a CT scan of SAH (obtained for another case).
 The American College of Emergency Physicians recommends that “in patients presenting to the ED with sudden-onset, severe headache and a negative noncontrast head CT scan result, lumbar puncture should be performed to rule out subarachnoid hemorrhage.”7 This is a level B recommendation. The sensitivity of CT at 5 days after headache onset falls precipitously, to just over 50% in early studies.7
The American College of Emergency Physicians recommends that “in patients presenting to the ED with sudden-onset, severe headache and a negative noncontrast head CT scan result, lumbar puncture should be performed to rule out subarachnoid hemorrhage.”7 This is a level B recommendation. The sensitivity of CT at 5 days after headache onset falls precipitously, to just over 50% in early studies.7
Urgent Care Evaluation
The case reported here was tricky, with the patient initially attributing her headache to an allergic reaction. The urgent care provider did not fall prey to anchoring bias8 and thus continued the evaluation in search of other causes.
Proper diagnosis is crucial because well-appearing patients sent home after a sentinel bleed have a high incidence of poor outcomes. About 50% of patients with SAH die within 6 months, and more than one third who live have a major residual deficit.9
Take-Home Points
- Nearly half of patients with SAH will have normal findings on physical examination and normal vital signs on initial presentation.
- SAH is commonly misdiagnosed, most often because the clinician fails to obtain a CT scan of the brain or fails to understand the limitations of CT in the diagnosis of SAH.
- SAH is the cause of headache in 1% of patients whose chief presenting symptom is headache.
- The sensitivity at 6 hours of modern third-generation CT scanners in ED patients is reported to be 100%.1
References
- Perry JJ, Stiell IG, Sivilotti ML, et al. Sensitivity of computed tomography performed within six hours of onset of headache for diagnosis of subarachnoid haemorrhage: prospective cohort study. BMJ. 2011;343:d4277.
- Fontanarosa PB. Recognition of subarachnoid hemorrhage. Ann Emerg Med. 1989;18:1199–1205.
- Butzkueven H, Evans AH, Pitman A, et al. Onset seizures independently predict poor outcome after subarachnoid hemorrhage. Neurology. 2000;55:1315–20.
- Vlak MH, Rinkel GJ, Greebe P, Greving JP, Algra A. Lifetime risks for aneurysmal subarachnoidhaemorrhage: multivariable risk stratification. J Neurol Neurosurg Psychiatry. 2013;84:619–23.
- Perry JJ, Stiell IG, Sivilotti MLA, et al. Clinical decision rules to rule out subarachnoid hemorrhage for acute headache. JAMA. 2013;310:1248–55.
- Edlow JA, Caplan LR. Avoiding pitfalls in the diagnosis of subarachnoid hemorrhage. N Engl J Med. 2000;342:29–36.
- Edlow JA, Panagos PD, Godwin SA, et al; American College of Emergency Physicians. Clinical policy: critical issues in the evaluation and management of adult patients presenting to the emergency department with acute headache. Ann Emerg Med. 2008;52:407–36.
- Croskerry P. Achieving quality in clinical decision making: cognitive strategies and detection of bias. Acad Emerg Med. 2002;9:1184–1204.
- Hackman JL, Johnson MD, Ma OJ. Spontaneous subarachnoid and intracerebral hemorrhage.In: Tintinalli JE, Stapczynski JS, Ma OJ, et al, eds. Tintinalli’s Emergency Medicine: A Comprehensive Study Guide. 7th edition. New York, NY: McGraw-Hill Medical; 2011.

