Published on
Urgent message: The patient punctured his hand with a power screwdriver. It turned out to be the least of his problems.
Frank Fannin, MD, EMT-P
Introduction
Hand Injuries are common and a major concern in urgent care settings as a source of potential significant disability and liability. A detailed history and focused exam are paramount to appropriate treatment and disposition. In the following case, a potentially devastating finding turns out not to be all that is seems. A good assessment and use of resources in this case helps avoid the need for costly and potentially invasive treatment.1,2
Case Presentation
BS is a 62-year-old male who presented to the urgent care with pain in his non-dominant hand after a minor injury. The event occurred about 7 hours earlier while he was at home using a power screwdriver. The bit over-penetrated and managed to pass through a hole in BS’ glove and into his hand. He stated that he continued to work after the injury, but the discomfort and swelling has increased since then and now extended up into this arm. BS described the feeling as “tight” but with no significant pain per se. There were no concerns with the patient as a historian or in his representation of events. The remainder of the history was found to be unremarkable.
Observations/Findings
Evaluation of the patient revealed the following:
- T: 98.7° F
- R: 16
- P: 72
- BP: 131/86
Physical exam revealed a healthy-appearing male in no apparent acute distress or discomfort. His vital signs were noted to be normal and there were no other significant findings outside the area of concern.
The site of injury was noted to be at the base of the first digit and just medial from the midline (Figure 1). The wound was small, with a flap noted. There was no significant bleeding and BS related that he never had significant bleeding. Diffuse edema of the hand was obvious (Figure 2). BS had good active range of motion with no complaints of numbness or weakness. Upon palpation of his hand, there was mild tenderness, with normal skin appearance and temperature. Gross subcutaneous emphysema was noted over the entire dorsum of the hand extending up into the forearm to just proximal to the antecubital fossa. There was no gross tenderness on palpation of the arm or noted discomfort with use of extremity. No other signs of injury or trauma were appreciated.

Diagnostic Studies
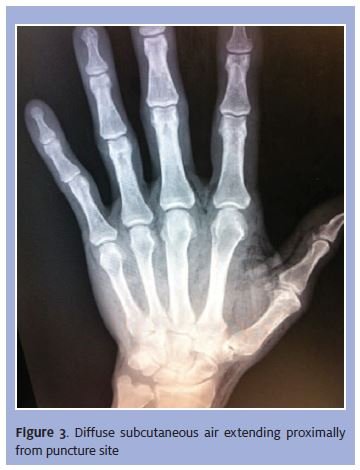
Imaging of the hand revealed neither fractures nor foreign bodies (Figure 3). A diffuse pattern of subcutaneous air was noted throughout the hand and proximal wrist. The film was read by radiology as being consistent with significant cellulitis.
Diagnosis
Traumatic subcutaneous emphysema.
Course and Treatment
BS’s concerning exam and x-ray findings did not fit with his history and overall presentation. The differential for this wound included infectious process and high-pressure injury. The ability to trust in a solid history of events and exam gave us reassurance. It was hypothesized that the wound was a port with the flap acting as a ball valve to allow in and trap air within the compartment of the hand.
The case was discussed with the surgeon on call for hand services, who agreed with our premise. A plan to apply a petroleum-based dressing to the site and wrap with a compressive dressing was undertaken. BS was to follow up in 12 hours with explicit instructions to monitor for spread of crepitus and erythema. He was to go to the emergency department with any concerning changes. His tetanus vaccination was updated and a prophylactic antibiotic regimen was initiated.
BS presented the next day with marked improvement in edema and crepitus, with none noted in the arm and minimal affliction in his hand. By day 3, his symptoms had completely resolved and he was able to return to work without issue, as noted on a follow-up call 2 weeks later.
Discussion
The finding of subcutaneous air in association with injury should always raise concerns for serious pathology, and if needed, aggressive surgical treatment at an appropriate facility.3,4 A thorough history and focused exam play an important role in directing care of these patients and ensuring the appropriate disposition.
In this case, the definitive time of injury and mechanism type, coupled with the absence of systemic symptoms suggestive of an infectious process, helped eliminate the major concerns on our differential. This left our hypothesis about the ball valve mechanism. Even in light of this, an abundance of precaution and education was undertaken because of the nature of the complaint.
In general, hand injuries require a high level of suspicion, as in most such presentations, the history can have a significant impact on the direction of care. Failure to build a complete picture or to use appropriate resources could have led to a potentially devastating outcome. for BS.
References
- Constantine T, Umayya M, Rammal A, et al. Non-infectious subcutaneous emphysema of the hand: a case report and review of literature. Emerg Med J 2010; 27(5): 383-386.
- van der Molen AB, Birndorf M, et al. Subcutaneous tissue emphysema of the hand secondary to noninfectious etiology: a report of two cases. J Hand Surg AM. 1999; 24(3): 638-641.
- Stevens D. Necrotizing infections of the skin and fascia. UpToDate website. Available at: http://www.uptodate.com/contents/necrotizing-infections-of-the-skin-and-fascia?source=search_result&search=Necrotizing+nfections+of+the+skin+and+fascia&selectedTitle=1-150. Accessed December 1, 2011.
- Stevens D, Bryant A. Clostridial myonecrosis. UpToDate website. Available at: http://www.uptodate.com/contents/clostridial-myonecrosis?source=search_result&search=Clostridial+myonecrosis&selectedTitle=1-150. Accessed December 1, 2011.
