Published on
Urgent message: No definitive treatment is available for this condition but diagnosis is important to reassure patients and avoid unnecessary care.
SHAILENDRA K. SAXENA, MD, PHD, MIKAYLA SPANGLER, PHARMD, BCPS, and ARCHANA MIKKILINENI, MD
Rashes are a common reason for patients to present to the urgent care clinic. Many require treatment but some do not. Schamberg’s disease is one such rash.
Case Presentation
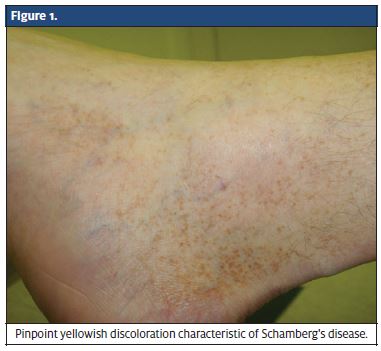
A 42-year-old male presented to our clinic with a chief complaint of bilateral lower extremity rash, which he had been experiencing for the past 3 months. The rash was erythematous, mildly pruritic, hyperpigmented and associated with pinpoint yellowish discoloration of the skin (Figure 1). There was no associated edema or stasis dermatitis of the skin. The patient did not have any other associated symptoms including fever, excoriation, blistering, or sharp pain around the site.
Definition
Schamberg’s disease was named after Jay Frank Schamberg, who first described it in 1901.1 It is also commonly known as “progressive pigmentary dermatosis of Schamberg,” “purpura pigmentosa progressiva,” or “Schamberg’s purpura.”1 It is characterized by chronic discoloration of the skin and is seen predominantly in the lower extremities. Although Schamberg’s disease is more common in males, it can present across all age groups, including both adult and pediatric patients.2, 3
Pathogenesis
Schamberg’s disease is caused by extravasation of red blood cells from the blood vessels near the surface of the skin.2 These cells penetrate through the capillary membrane and deposit in the skin and subcutaneous tissue. Degradation of hemoglobin to hemosiderin is responsible for the yellow-brown, pinpoint rash-like appearance.2 The causes of this type of capillaritis include medications, food additive allergies, viral infections and exercise.2
Medications associated with Schamberg’s disease There is no definitive medication-related cause of Schamberg’s disease. However, there have been case reports detailing possible causative medications. Nishoika and colleagues 4 identified many potential agents that could be responsible for the development of the condition, including vitamin B3 and chlordiazepoxide. In these cases, removal of the offending agent usu- ally resulted in an improvement in the appearance of the skin.4 Although medications are not commonly the cause of Schamberg’s disease, providers should rule out medication-related instances by implementing a drug holiday.
Symptoms
The symptoms of Schamberg’s disease include irregular yellow-brown, rust-colored flat patches on the skin, with reddish pinpoint lesions along the border of the discoloration, which are often described as Cayenne pepper spots.1 New spots appear within and along the edges of old lesions. These lesions are usually present on the lower extremities (around the ankles), but can be seen on any part of the body, including the hands. The patches are usually not bothersome, but can occasionally cause some pruritis. The eruption can persist for many years, although the pattern of eruption can change with slow extension and clearing of lesions.5
Differential diagnosis
Differential diagnoses of Schamberg’s disease include purpura annularis telangiectodes (Majocci’s Disease),5 which is characterized by annular telangiectasias along with Cayenne pepper spots. Pigmented purpuric dermatosis of Gougerot and Blum is another possible diagnosis and is characterized by lichenoid papules.1 Diagnosis of Schamberg’s disease is made when microscopic examination of a skin biopsy shows perivascular lymphocytic superficial dermal infiltrate with mild hemorrhage and hemosiderin deposition. The biopsy may also show red.
Treatment
There is no known definitive treatment for Schamberg’s disease. Cosmetic imperfections, rather than heath-related issues, are the main concern for patients with this disease. The discoloration of the flat, smooth patches resembling Cayenne pepper may be cause for embarrassment. Various strategies for controlling the rash include discontinuing or changing the offending medication, avoiding food preservatives and artificial coloring agents, and wearing support stockings to counteract abnormal vein function. Taking vita- mins such as vitamin C has helped individuals in some cases. Topical steroids, such as cortisone, may be used if there is an itching component to the rash, but this rarely cures the capillaritis, which is the predominant cause of the disease. Some patients have reported successful treatment with pentoxifylline, but that does not work in every case.6 Laser therapy is being considered as a treatment option, but further research must be performed before it can be considered as a definitive treatment option.6
Discussion
Schamberg’s disease is usually characterized by pinpoint petechiae with a brown or yellow base. This dis- tinct rash is easy to recognize in clinical practice but other diagnoses should also be considered, including Pigmented purpuric dermatosis of Gougerot and Blum,1 drug-induced eruptions,3 Majocci’s Disease,5 and leuko- cytoclastic vasculitis.7 The purpura is usually harmless. However, localized lichinifications, scaling, and atrophy may present with rash.1 The treatment of Schamberg’s disease has not been well established. Making a correct diagnosis is imperative to reassure patients and to avoid further costly referrals and unnecessary treatment. ■
References
- Tristani-Firouzi P, Meadows KP, Vanderhooft Pigmented purpuric eruptions of child- hood: a series of cases and review of literature. Pediatr Dermatol. 2001;18:299-304.
- Gibson Schamberg Purpura. Mayo Clin Proc. 2004;79:1070.
- Draelos ZK, Hansen RC. Schamberg’s purpura in children: case study and literature review. Clin Pediatr (Phila). 1987;26:659-661.
- Nishoika K, Katayama I, Masuzawa M, Yokozeki H, Nishiyama Drug-induced chronic pigmented purpura. J Dermatol. 1989;16:220-222.
- Nichamin S and Brough Chronic Progressive Pigmentary Purpura: Purpura Annu- lares Telangiectodes of Majocchi-Schamberg. Am J Dis Child. 1968;116:429-433.
- Kano Y, Hiroyama K, Shiohra Successful treatment of Schamberg’s disease with pen- toxifylline. J Am Acad Dermatol. 1997;36:827-830.
- Wheeler B, Shah D, Saxena Mystery ash: Acute leukocytoclastic vasculitis. Consult- ant. 2010;50:22-24.

