Published on
Urgent message: Staphylococcus aureus is a common pathogen in the community—one that can lead to a range of infections, including abscess and sepsis. Invasive methicillin-resistant S aureus (MRSA) infections have decreased in the healthcare setting; however, at the same time, community-acquired infections have increased. Delayed treatment increases morbidity and mortality.
Jordan Miller, DO and Ari Leib, MD
AN ILLUSTRATIVE CASE
A 40-year-old female presented to an urgent care center with the chief complaint of a spider bite on her right foot. She states that she woke up to her foot itching and now had a small area of redness over the dorsal aspect with associated pain over the foot but no associated fevers, chills, or malaise. She denied seeing a spider. She denies a history of intravenous drug use, skin popping, or trauma to the area. She denies recent pedicures in unsanitary conditions or going barefoot; however, she did admit to taking a shower in a tub that had standing water backing up into it.
Physical exam revealed a well-nourished, well-developed female in no significant distress. Her exam revealed a small area of erythema over the lateral aspect of the fourth metatarsal with mild pain to palpation (See Figure 1). Neurovascular exam of the foot was benign.
Urgent Care Management
The patient was given amoxicillin/clavulanic acid and steroids from the urgent care and was discharged with return precautions.
Outcome
Over the next 2 days, the patient developed extensive swelling over the dorsum of the foot, with fevers and malaise. The erythema transitioned to necrosis with draining tracts. She subsequently presented to the emergency room where bedside incision and drainage revealed extensive purulent material. She was started on intravenous antibiotics (vancomycin and piperacillin-tazobactam).
The patient met one SIRS criteria on admission, for an elevated white blood cell count of 13k, but all other laboratory work was negative for acute abnormality. MRI was performed of the right lower extremity but it did not show osteomyelitis. Wound cultures returned positive for MRSA and blood cultures were negative. In addition, the patient was diagnosed with cellulitis secondary to MRSA in the emergency room after failed outpatient management; this was thought to be provoked by unsanitary water exposure. After 5 days of IV antibiotics she was discharged home with oral linezolid two times daily for 6 days.
DISCUSSION
Introduction
Staphylococcus aureus is a gram-positive, cocci-shaped bacterium that is catalase-positive, reduces nitrates, and is a facultative anaerobe. It can be a normal part of human flora, commonly found in the upper respiratory tract and on the skin; however, it can also be an opportunistic pathogen that is a common culprit in abscesses, respiratory tract infections (including sinusitis), and food poisoning, pneumonia, meningitis, osteomyelitis, endocarditis, toxic shock syndrome, bacteremia, and sepsis.
Though S aureus could be treated successfully with penicillin in the 1940s, two decades later resistance began to develop and methicillin emerged as the treatment of choice. The first human case of MRSA was discovered in 1968; the bacteria was found to be resistant to previously successful treatments including penicillin, methicillin, oxacillin, and amoxicillin.
Currently, intravenous vancomycin is the drug of choice for MRSA, although there have been 13 documented cases of vancomycin-resistant MRSA.1
Common symptoms of community-acquired MRSA include:
- A cluster of “pimples” or a large, tender lump that drains pus (a carbuncle)
- The area may form a central raised area that oozes purulent material
- Single raised red lump that may or may not be tender and, with many patients, report of a “spider bite,” without actually seeing the spider
Epidemiology
S aureus is implicated in many infections, and it can quickly become deadly.2 In one study, researchers cultured acute skin or soft tissue infections of 422 patients seen at 11 emergency rooms; 59% were found to be MRSA. Another study revealed that in perianal abscess 34.8% of cases were found to be MRSA positive.1 The initial area of infection spread hematogenously to the heart valves, bones, joints, lungs, pacemakers, IV lines, or prosthetic joints.
Risk Factors
Risk factors for community-acquired MRSA include skin trauma (burns, cuts, and sores), body hair removal, tattoos, piercings, and sharing of personal equipment (eg, razors, tweezers) that are not cleaned properly. The incidence of MRSA-related hospitalizations ranges from 11.5% to 60% across the nation.3 MRSA is considered a major pathogen in skin and soft tissue infections. Clinicians should suspect MRSA infection in the following situations:
- Contact with a prisoner or prison facility
- Recent treatment or report of a “spider bite”
- Recurring skin infections, including impetigo and furuncles
- The patient is involved in contact sports or spends time in a sports facility
Cellulitis vs MRSA
Misdiagnosing cellulitis is a common problem in our healthcare system. Inflammatory dermatoses of the lower extremity are often misdiagnosed as cellulitis and treated with antibiotics or hospitalization. One study found that 30.5% of patients were misdiagnosed with cellulitis; of those 259 patients, 52 were admitted for further treatment.4 Misdiagnosing cellulitis leads to 50,000 to 130,000 unnecessary hospitalizations and use of unneeded antibiotics, which can lead to nosocomial infections, including Clostridium difficile and adverse reactions to anaphylaxis. Correlating exam findings with patient presentation is an important task for physicians to avoid unwanted outcomes for the patient.4
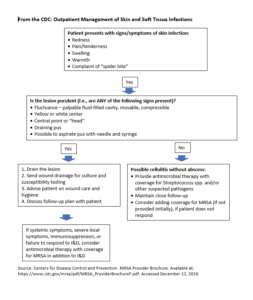
Treatment for simple cellulitis vs MRSA infection can be difficult to distinguish. Patients with simple cellulitis often present with redness, swelling, and pain around the site of the skin infection. Purulent lesions with palpable, fluid-filled cavities that are moveable or compressible are more likely to be MRSA. Lesions with draining pus are also more likely to be MRSA. Patients with a history of MRSA infection elsewhere on the body, penetrating trauma, or history of IV drug abuse are more likely to require MRSA coverage.
As streptococci species are also a common cause of cellulitis, many physicians choose to cover for both MRSA and streptococci. Options include using TMP-sulfamethoxazole (Bactrim) or doxycycline with a beta-lactam such as penicillin, cephalexin, or amoxicillin. Current studies have shown that in the absence of abscess, ulcer, or purulent drainage, beta-lactam monotherapy is recommended and that treatment with a beta-lactam such as cefazolin or oxacillin was successful in 96% of patients. Double-blinded studies showed that a combination of TMP-SMX plus cephalexin was no more efficacious than cephalexin alone in pure cellulitis.4
Patients with an increased mortality and morbidity due to MRSA include seniors, nursing home patients, and those with organ dysfunction. Patients with end-stage liver disease or renal dysfunction and those admitted to the ICU with MRSA infection have also been found to have increased mortality. Mortality rates range from 5% to 60%, dependent on the site of infection and patient population.1 In 2017, S aureus bloodstream infections accounted for 20,000 deaths in the United States.5
For patients discharged from the ED with a MRSA infection, outpatient follow-up in a timely period is important.
The CDC gives specific recommendations for outpatient MRSA follow-up and advises that patients should be clearly instructed to return promptly if they develop systemic symptoms or worsening local symptoms, or if their symptoms do not improve within 48 hours. Patient should have a follow-up visit scheduled within 48 hours of the initial visit to confirm adequate response to therapy.6
Management
Treatment includes antibiotics along with incision and drainage. If the patient is to be discharged home, options include a 7- to 10-day course of by mouth trimethoprim-sulfamethoxazole, doxycycline, clindamycin, or minocycline. For those with a history of sulfa allergy where sulfamethoxazole is contraindicated, doxycycline or clindamycin are acceptable options. (Using a local antibiogram can help guide clinicians to select the best empiric antimicrobial therapy in the event of a pending culture and susceptibility result.)
Doxycycline is excreted in fecal material and is also an acceptable option in outpatient treatment of patients with chronic kidney disease.
For children with sulfa allergy and MRSA infection, clindamycin and doxycycline are both suitable options. Avoiding tetracyclines in children is no longer a recommendation to protect against adverse effects or teeth discoloration.
In pregnant patients with a sulfa allergy, use clindamycin.
| Table 1. Management Options—a Comparison |
| · Trimethoprim-sulfamethoxazole ─ Mechanism of action: sulfamethoxazole inhibits bacterial synthesis of dihydrofolic acid; trimethoprim blocks the production of tetrahydrofolic acid from dihydrofolic acid ─ Pros: low cost ─ Cons: photosensitivity, hyperkalemia, renal tubule acidosis, hepatitis, Steven Johnson syndrome |
| · Doxycycline ─ Mechanism of action: bacterial protein synthesis inhibitor ─ Pros: fecal excretion (good antibiotic choice for ESRD patients) ─ Cons: chelation, teratogenic, photosensitivity |
| · Clindamycin ─ Mechanism of action: bacterial protein synthesis inhibitor ─ Pros: low cost ─ Cons: diarrhea, high risk for Clostridium difficile infection, potential source for inducible resistance |
Currently, according to the CDC, cultures are rarely obtained in cases of cellulitis where there is no purulent drainage or no abscess. Current recommendations include incision and drainage of simple abscesses and boils. In addition, there are insufficient data to suggest the necessity of antibiotics in these cases. Antibiotics should be given if there are multiple sites of infection or progression of associated cellulitis, signs and symptoms of systemic illness, associated comorbidities or immunosuppression, extremes of age, or in body areas where abscesses are difficult to drain.
Empiric therapy is recommended for 5 to 10 days; a culture should be obtained if there is purulent material. For nonpurulent cases, give 5 to 10 days of empiric therapy. In some departments, irrigation after an incision and drainage is standard of care. Irrigation increases the length of procedure and pain experienced by the patient.
Prevention
Following are tips to help prevent MRSA:7
- Avoid sharing personal items such as towels or washcloths
- Perform good handwashing with soap and water
- Clean all exercise machines at gyms
- Avoiding touching other’s wounds and sores
- Keeping cuts/scrapes clean and dry with a Band-Aid overtop
Colonization
Most patients who develop MRSA infection have been colonized prior to infection. Approximately 20% of the general population is colonized with S aureus, and most frequently it is found it in the anterior nares.8 In the general population, another 30% is intermittently colonized. Though the reasons are unclear, the remaining 50% don’t appear to be susceptible to S aureus carriage.9
Risk factors for colonization include previous admission to a hospital, the presence of chronic wounds or skin lesions, residing in a long-term care facility, and use of urinary or IV catheters.
One study showed that mupirocin appeared to only be cost-effective as a decolonization agent in patients that are proven nasal carriers. It was concluded that mupirocin as a decolonizing agent is effective in the short-term, and is helpful in decreasing risk for infection in select populations.1 Mupirocin is not systemically absorbed, which makes it a good choice for decolonization. There has been an increase in resistance to mupirocin when the agent is routinely used as a strategy to control endemic S aureus infection and transmission among general inpatient population.
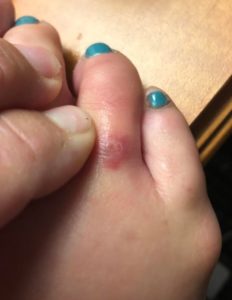
Figure 1. Patient’s foot after “spider bite.”
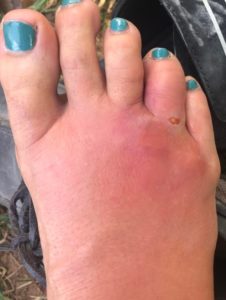
Figure 2. Patient foot prior to starting Augmentin with steroid taper.
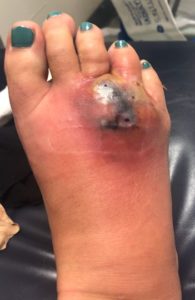
Figure 3. Patient foot on day of admission.
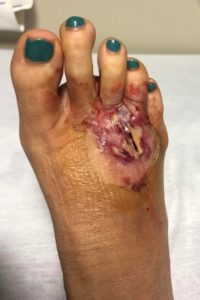
Figure 4. Patient foot after 4 days of IV antibiotics and incision and drainage.
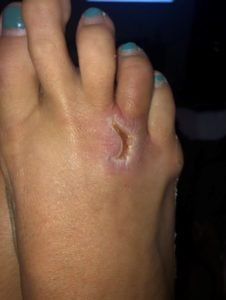
Figure 5. Patient foot 6 weeks after treatment.
Teaching Points
- MRSA infection can turn deadly quickly if not promptly identified and treated.
- Associated risk factors include contact with prisoners or a prison facility, recurring skin infections, contact sports, and reports of “spider bites” (although true spider bites are uncommon).
- MRSA-related mortality can be reduced by early identification and control of infectious source.
References
- MRSA most common cause of skin infections in nation’s emergency rooms.” ScienceDaily. Available at: www.sciencedaily.com/releases/2006/08/060819112256.htm. Accessed December 12, 2019.
- Lakhundi S, Zhang K. Methicillin-resistant Staphylococcus aureus: molecular characterization, evolution, and epidemiology. Clin Microbiol Rev. 2018;31(4).
- Miao J, Wang W, Xu W, et al. The fingerprint mapping and genotyping systems application on methicillin-resistant StaphylococcusMicrob Pathog. 2018;125:246-251.
- Moran GJ, Talan DA. Cellulitis commonly misdiagnosed or just misunderstood. JAMA. 2017;317(7):760-761.
- Kourtis AP, Hatfield K Baggs J, et al. Epidemiology and recent trends in methicillin-resistant and in methicillin-susceptible Staphylococcus aureus bloodstream infections—United States. MMWR. 2019;68(9)214-219.
- Centers for Disease Control and Prevention: Methicillin-resistant Staphylococcus aureus (MRSA). Centers for Disease Control and Prevention. Available at: https://www.cdc.gov/mrsa/healthcare/outpatient.html. Updated June 26, 2019. Accessed October 23, 2019.
- Farr BM. Prevention and control of methicillin-resistant Staphylococcus aureusCurr Opin Infect Dis. 2004;17(4):317–322.
- Williams RE. Healthy carriage of Staphylococcus aureus: its prevalence and importance. Bacteriol Rev. 1963;27:56–71.
- Khan TM, Kok YL, Bukhsh A, et al. Incidence of methicillin resistant Staphylococcus aureus(MRSA) in burn intensive care unit: a systematic review. Germs. 2018;8(3):113-125.


