Published on
Urgent message: Patients who have had recent surgical procedures may present to urgent care centers for reasons ranging from seeking reassurance to presentation of life-threatening complications.
Tracey Quail Davidoff, MD
Introduction
Patients often experience complications—or, at least as often, fear they’re experiencing complications—after a surgical procedure. While the surgeon is often the best person for them to consult, this may not be possible for a variety of reasons. Outpatient surgical centers are opening almost at the same rate as urgent care centers,1 but may not be well prepared to handle complications after hours. Patients in rural areas may need to travel to distant facilities for cosmetic or specialized procedures, making bedside reassessment with the surgeon difficult. Medical tourism, where patients travel outside the country for procedures, also makes follow-up with the actual surgeon impractical if not impossible. Patients who have just been discharged from the hospital may not wish to return if they have a complication, fearing long emergency room wait times and large bills, opting instead to present to urgent care.
Surgical complications likely to present to an urgent care center can be divided into acute, subacute, and late.
ACUTE COMPLICATIONS
Complications defined as acute occur as a direct result of the surgery itself, side effects of anesthesia, bleeding, or side effects of the medications prescribed, such as pain medications and antibiotics. These may include:
- Injury to anatomic structures or expected postsurgical effects. Some concerns may be condition-specific (eg, hematuria from lithotripsy, inability to void after prostatectomy, or vaginal bleeding after gynecologic procedures). Patients who have had laparoscopy may complain of abdominal pain or bloating or even shoulder pain from the insufflated gas. These concerns need to be addressed on a case by case basis, with consultation with the surgeon or referral to the ED if the concern cannot be addressed by the urgent care provider.
- Postoperative pain. This is one of the major reasons a patient will seek urgent care following surgery. In the current climate of narcotic abuse, surgeons rely less on postoperative narcotics and more on local blocks for postoperative pain control. These blocks generally lose their effectiveness after 16-18 hours. If NSAIDs are not strong enough or contraindicated, the patient does not wish to take the narcotics, or they were not prescribed, the patient may present seeking pain control. If the patient contacted the surgeon and he or she refused to prescribe narcotics, the urgent care provider should be cautious about dispensing them. If narcotics are prescribed, no more than a 5-day supply should be offered. Be sure to follow your state regulations when prescribing narcotics.
- Postoperative fever is most commonly an acute complication but can occur at any point in the postoperative period. Fever is defined as temperature higher than 38°C or 100.4° See Table 1 for differential diagnoses.
Causes of Postoperative Fever
| Acuity | Immediate | Acute | Subacute | Late |
| Time span | Within hours of surgery | Within 1 week of surgery | 1-4 weeks following surgery | >1 month after surgery |
| Condition/
complication |
Medications | Nosocomial infections | Surgical site infection | Recurrent infection |
| Blood products | Infections obtained prior to surgery | Central venous catheter infection | Postpericardiotomy syndrome (if open heart surgery) | |
| Infections obtained prior to surgery | Early surgical site infections (GAS, Clostridium perfringens) | Antibiotic associated diarrhea (Clostridium difficile) | Viral infections related to blood products | |
| Inflammation due to surgery itself | Vascular access related infections | Febrile drug reaction
(b-lactam antibiotics, sulfa-containing medications) |
Surgical site infections due to indolent organisms (Coagulase-negative Staphylococcus) | |
| Malignant hyperthermia (rare but deadly) | · Aspiration
· Ventilator-acquired pneumonia (VAP) · Catheter-related UTI · Pancreatitis · Myocardial infarction · Pulmonary embolus · Thrombophlebitis · Alcohol withdrawal · Acute gout |
· Thrombophlebitis, especially if patient is less mobile
· Post─CU-related infections |
SUBACUTE AND LATE COMPLICATIONS
Subacute complications present several days postoperatively. “Late” complications can occur anytime after that in the post-op period, and are discussed here accordingly.
- Allergic reactions should prompt a careful review of any medications given intra- or postoperatively as well as latex and glue or tape allergies from bandages. Antibiotic ointments may also cause contact dermatitis and allergy. Dressings should be removed and the area inspected. Betadine may not have been washed off, causing itching. Some patients may also have a contact reaction from tincture of benzoin used to adhere surgical tape and bandages.
- Dystonic reactions may occur from medications prescribed for nausea and vomiting, presenting with muscle spasms including fixed upward gaze, neck twisting, grimacing, clenched jaw, and difficulty speaking. It is usually painful and frightening. Treatment with parenteral diphenhydramine, diazepam, or benztropine is usually curative.
- Spinal or postdural puncture headaches occur as a complication of accidental puncture of the dura during epidural anesthesia or failure of the puncture to seal following spinal anesthesia. Patients will complain of headache that is positional; worse when upright and better when lying flat. The headache may be accompanied by neck stiffness, photophobia, nausea, tinnitus, or phonophobia. Risk factors include female sex, young but not pediatric age, pregnancy, history of prior headaches, and a low BMI.2 Mild symptoms may be treated with fluids, caffeine, bed rest and analgesia. Severe cases may require an epidural blood patch, which will likely require transfer to the ED and consultation with an anesthesiologist.
- Nausea and vomiting may occur immediately after surgery or several days post-op. Early vomiting is usually due to the aftermath of anesthesia, though it can also be caused by narcotic pain medications including codeine, morphine, and oxycodone; or antibiotics. The patient should be evaluated for dehydration, and if necessary, fluids should be replaced. Antiemetics such as ondansetron, metoclopramide, promethazine, or prochlorperazine can be given or prescribed for outpatient use. Changing from one narcotic to another may alleviate vomiting. Other structural causes may include ileus or obstruction. With significant pain or vomiting, or consideration of severe dehydration, intractable emesis, or an organic cause, emergent evaluation in the ED is advisable.
One frequent cause of nausea and vomiting, as well as diarrhea, is antibiotics. Vomiting may present as an early side effect, and diarrhea as a late effect. Most diarrhea from antibiotics is self-limited and will resolve when the antibiotic is discontinued, but if the diarrhea is severe, associated with abdominal pain, fever, or marked cramping, consider Clostridium difficile. Antibiotics may also cause yeast infections in the form of thrush or vaginitis in females.
- Constipation is common following abdominal procedures. Etiologies may include medications, bowel inactivity, decreased postoperative activity, and dietary changes. Treatment with suppositories or enemas may be trialed first, and if limited results, oral agents such as granular bulking agents or citrate of magnesium can be tried. Granular bulking agents should be avoided if bariatric or bowel surgery has been performed as they may cause obstruction. Severe cases may require manual disimpaction of stool from the rectum. Before making a diagnosis of constipation, consider consultation with the surgeon, as constipation may be a symptom of obstruction.
- Sore throats are common following endotracheal intubation for general anesthesia. Evaluate for stridor and drooling. If stable, a careful exam of the oral cavity to inspect for trauma, swelling, and injury to the teeth should be performed to rule out any serious complications. If these are not present, the patient should be reassured. With persistent or significant symptoms, the patient may need referral to an otolaryngologist for an endoscopic procedure to detect occult injury.
- Cough is also common following general anesthesia; this may be self-limited but may indicate more serious concerns such as pneumonia, aspiration, and atelectasis. Assess for fever, elevated respiratory rate, tachycardia, hypoxia, and abnormal breath sounds. A chest radiograph may be indicated for abnormal findings.
- Chest pain is worrisome in the postoperative patient. Pulmonary embolus (PE) and deep venous thrombosis (DVT) may follow major procedures, lower extremity procedures, and patients who have had in-patient surgery. Patients who have had a personal or family history of venous thromboembolic disease, obese patients, and cancer patients also have an elevated risk. Patients should be referred to the ED with consideration of DVT or PE.
Myocardial infarction may occur in the postoperative period; these patients should be evaluated in the ED.
- Urinary symptoms. Patients who have had gynecologic, urologic, or other surgeries requiring a Foley catheter may present with urinary symptoms such as dysuria, urgency or frequency. Side effects of anesthetics, narcotics, antiemetics and antihistamines may also cause urinary retention. Patients may also develop candida vaginitis as a result of antibiotics that may cause urinary symptoms. Unless there are urologic complicating factors, treatment is often the same as non-postoperative patients. Contacting the patient’s gynecologist or urologist may be advised for further direction in complicated cases.
- Bleeding or drainage from the wound may be distressing for patients prompting them to seek urgent care. Although medical personnel are accustomed to seeing blood or serous fluid soaking through bandages, patients may see this as a potential complication. Removing the bandage and inspecting the area, with reassurance and a bandage change may be all that is required, but the patient should be evaluated for hematoma, seroma, or infection.
A hematoma is a collection of blood, in this case beneath a surgical incision. It is due to the failure of primary homeostasis to be achieved during the time of the procedure, or a failure of the clotting mechanism of the patient due to a bleeding diathesis, causing pain, swelling and oozing from the suture line, which can then predispose to separation of the wound and infection.
A seroma is a collection of serum beneath the surgical incision. A seroma forms due to dead space remaining between the skin and the deep tissues at the time of wound closure. This allows the accumulation of serous fluid to form in the dead space. This can be site specific or due to failure of the surgeon to adequately close the dead space. Obesity is the main risk factor and can be mitigated by drain placement. Higher risk surgical sites include breast, abdominal wall surgeries, especially ventral hernia repairs. Seromas cause swelling and oozing from the suture line, but compared to a hematoma, are usually painless. They rarely become infected but add to wound healing time.3 The drainage can be quite copious and distressing.
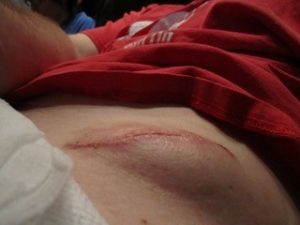
Seroma following a hernia repair. (Photo courtesy of Tracey Quail Davidoff, MD.)
The diagnosis of either is by inspection and palpation of the wound. If the diagnosis is in question, ultrasound or CT scan may be useful to delineate the extent of the area or distinguish between hematoma, seroma, infection, and the dreaded complication of necrotizing fasciitis. Small hematomas and seromas can safely be observed, but large ones should be drained. The wound may be opened partially along the suture or staple line after consultation with the surgeon. If a seroma is suspected, needle aspiration may be all that is required.4 The wound should be packed until granulation tissue is present at the base allowing healing by secondary intention. If there is any suspicion of infection or if it appears that deeper tissues are exposed or disrupted, the patient should be evaluated urgently by a surgeon.
- Fascial dehiscence may occur when the incision breaks down due to tissue breakdown, suture failure, or knot failure. This may occur early or late in the course of healing. The wound may dehisce partially or completely.5 Abdominal wounds are at risk for evisceration. Fascial dehiscence that is not repaired may result in hernia formation.
Suspect dehiscence if the patient complains of a serosanguinous drainage from the wound. There may be an incisional bulge which is exacerbated by a Valsalva maneuver. Most fascial dehiscence occurs 4-14 days after the surgical procedure. The diagnosis is clinical. Complete fascial dehiscence is a surgical emergency for which mortality and morbidity may be significant. If the bowel is exposed the wound should be gently covered with saline soaked gauze and the patient transferred to the ED.
- Surgical-site infection (SSI) occurs in 4% of all clean surgical wounds and 35% of grossly contaminated wounds (characterized as being grossly purulent, with a retained foreign body [trauma], devitalized tissue, or fecal contamination).6 Risk factors include obesity, immunosuppression, cardiovascular disease, smoking, cancer, previous surgery at the same site, malnutrition, and prior irradiation in the field of surgery. The diagnosis is clinical, with erythema, induration, warmth, pain, and purulent wound drainage present. Separation of the incision may occur, as well as fever, and leukocytosis. Deep tissue infection extending to the fascia, or necrotizing fasciitis, is a surgical emergency. These patients will have copious, dishwater like drainage from the wound and the skin will be dusky with pale and devitalized, even necrotic tissue beneath. The surrounding tissue will be friable. Treatment is emergent surgery.
SSIs with cellulitis can be treated with oral antibiotics or, in select patients, topical mupirocin. Topical antibacterial preparations such as povidone-iodine, sodium hypochlorite, and hydrogen peroxide should be avoided as they are toxic to fibroblasts and impede wound healing. Cleaning with soap and water may be done daily.. Swabs of the wound are often polymicrobial and cannot distinguish colonization from active infection and are not helpful. Antibiotics should cover gram-positive cocci from skin (eg, cephalexin). If a methicillin-resistant staph aureus (MRSA) abscess is a consideration, incision and drainage should be performed with possible prescription of antibiotics which cover the MRSA (such as trimethoprim-sulfamethoxazole).
Infected wounds with fluctuance and evidence of abscess formation should be opened, explored, drained, and irrigated with sterile normal saline. If fascial disruption is suspected or discovered the procedure should be done in an operating room under sterile conditions. Mechanical debridement with forceps, scissors, or scalpel and removal of all foreign bodies should be done.7 Superficial wounds can be covered with sterile dressings, deeper wounds should be packed with wet, saline soaked gauze and changed twice daily until a bed of healthy granulation tissue is present. There are many commercial dressings available, one should be selected that allows for maintenance of warmth and moisture and encouragement of granulation tissue.8 Antibiotics are not required if the wound is open and draining and the patient has no signs of systemic infection. The patient should be referred back to the surgeon if possible, if not, a wound center.
- Drains and sutures. Patients may present to the urgent care center for removal of drains or sutures. Drains are generally removed when there has been no fluid output for 24 hours. Any suture should be removed first. The tubing should be “milked” from the skin to the bulb until as much liquid as possible is collected from the tube. The drain should then be removed in a continuous unidirectional pull. A dressing to collect any further drainage should be applied. Patients should be warned that some drainage from the opening is to be expected.
A late presentation postsurgery may be for suture removal if the patient has had their procedure in a distal location. Before removing any sutures, the wound should appear to be well healed, similar to a laceration, and “ready” to have the sutures removed. If in doubt, a few or every other suture can be removed and reassessed before removing all the sutures. If it appears more time is needed, surgical tape strips can be applied to maintain approximation.
Abdominal wounds require longer healing periods to prevent dehiscence, especially in the obese. Some cases require 2-3 weeks or more. Early removal can contribute to dehiscence, hypertrophic scaring, and hernia by increasing the tension on the underlying deep sutures. If there is any question as to the timing of removal, a surgeon, preferably the one who did the procedure should be consulted prior to removal of any sutures or staples.
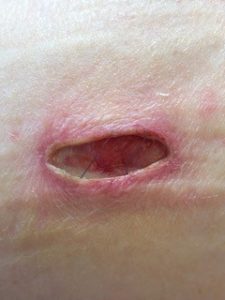
Dehiscence of a laparoscopy incision. Note the ruptured sutures in the wound bed. (Photo courtesy of Tracey Quail Davidoff, MD.)
- Itching is common following any surgical wound and is a normal part of the healing processes. Inspect the wound for any evidence of infection or rash. Contact dermatitis from bandages or topical ointments is common. The patient should be questioned what they are putting on the wound. If no evidence of rash or infection is present, the patient can be reassured that itching is normal. Petroleum jelly can be used to provide barrier protection and alleviate itch. If the wound is completely closed, topical scar creams, Vitamin E oil, or cocoa butter can be used.
- Neuropathic symptoms. Cutaneous nerves are frequently disrupted during surgery and may result in neuropathic symptoms such as numbness, burning, itching or paresthesia in and around the wound. These symptoms may partially resolve over time but are frequently permanent. They can be quite distressing for the patient. Deeper nerve injuries may cause pain, numbness, weakness, and ultimately neuroma.9 If reassurance is not sufficient the patient should be referred back to the surgeon and in some cases a pain and symptom management specialist.
- Keloids and hypertrophic scars can occur from any injury to the skin in susceptible persons. Topical silicone sheets or gel may be helpful if used for 3-6 months in new and established scars.10,11 Other treatments such as steroid injection, laser therapy, and resection are best left to a dermatologist or plastic surgeon. Treatment of these complications is often less than satisfactory.11
- Hernias occur when the abdominal wall tension overcomes the suture or knot strength of the fascial layer of an abdominal wound. It may be partial or complete and occur in any abdominal incision including laparoscopic sites. This may occur at any point in the healing process. It is more likely to occur in males, obese patients, patients with chronic coughs, wound infections, patients on chronic glucocorticoids, and patients with poor nutritional status. Following abdominal surgeries patients should avoid heavy lifting of >13 pounds from the floor for four to six weeks following the procedure.12 Once the hernia has occurred, the only option is surgical repair. Hernia belts or abdominal compressive garments may minimize symptoms but are not curative. Patients should be evaluated for incarceration, and if present, should be sent to ED for evaluation. If incarceration is not present, outpatient referral for surgical evaluation and potential repair is recommended. Patients should be warned about the signs of incarceration such as significant pain, vomiting, or fever. Larger hernias are less likely to become incarcerated than smaller as the abdominal contents flows freely from the hernia sack to the abdomen.
Conclusion
Postoperative complications are common, and it is not always possible for the patient to be evaluated by the operating surgeon. As patients are more and more looking for immediate solutions to their medical concerns, they may seek care for these complications in your urgent care center. A thorough evaluation is key in determining if an emergency condition exists and if transfer to the hospital is required. Consultation with the performing surgeon should be accomplished if possible. Frequently, gentle reassurance and patient education is all that is required.
Citation: Davidoff TQ. Postoperative complications in the urgent care setting. J Urgent Care Med. February 2019. Available at: https://www.jucm.com/postoperative-complications-in-the-urgent-care-setting/.
References
- Fields R. 25 statistics on surgery center growth. Becker’s ASC Review. July 14,2011. Available at: https://www.beckersasc.com/asc-turnarounds-ideas-to-improve-performance/25-statistics-on-surgery-center-growth.html. Accessed September 29, 2018.
- Khlebtovsky A, Weitzen S, Steiner I, et al. Risk factors for post-lumbar puncture headache. Clin Neurol Neruosurg. 2015;131:78-81.
- Aho JM, Nickerson TP, Thiels CA, et al. Prevention of postoperative seroma with dead space obliteration. Int J Surg. 2016;29:70-73.
- Lehr S, Schuricht A. A minimally invasive approach for treating post-operative seromas after incisional hernia repair. JSLS. 2001;Jul-Sep:5(3):267-271.
- Carlson MA. Acute wound failure. Surg Clin North Am. 1997;77(3):607-636.
- Campbell B. Complications of abdominal incisions: a review of prevention, diagnosis, and treatment. Grand Rounds. KUMC – Wichita Department of OBGYN. May 10, 2017. Available at: https://www.wesleyobgyn.com/pdf/lectures/2017.05.10_Abdominal%20wound%20complications.pdf. Accessed January 10, 2019.
- Steed DL. Debridement. Am J Surg. 2004;187(5A):71S.
- Vermeulen H, Ubbink D, Goossens A, et al. Dressings and topical agents for surgical wounds healing by secondary intention. Cochrane Database Syst Rev. 2004.
- Kehlet H, Jensen TS, Woolf CJ. Persistent postsurgical pain: risk factors and prevention. Lancet. 2006;367(9522):1618-1625.
- Gold MH. Topical silicone gel sheeting in the treatment of hypertrophic scars and keloids. A dermatologic experience. J Dermatol Surg Oncol. 1993;19(10):912-916.
- Fulton JE Jr. Silicone gel sheeting for the prevention and management of evolving hypertrophic and keloid scars. Dermatol Surg. 1995;21(11):947-951.
- Gerten KA, Richter HE, Wheeler TL 2nd, et al. Intraabdominal pressure changes associated with lifting: Implications for postoperative activity restrictions. Am J Obstet Gynecol. 2008; 98(3):306.e1-5. Epub 2008 Feb 20.
Tracey Davidoff, MD is an attending physician at Rochester Regional Health Immediatecare in Rochester, NY. The author has no relevant financial relationships with any commercial interests.

