Published on
Urgent message: PRICE (protection, rest, ice, compression and elevation) treatment is often advised to patients as part of sports soft tissue injuries; however, incorrect use of cryotherapy may lead to complications.
Amitesh Kumar, MD
Introduction
Cryotherapy involves application of ice on acute soft tissue injuries in the form of ice cubes, ice packs, ice towels, ice massage, frozen gel packs, ethyl chloride, and other chemical devices. The goal is temperature reduction of 10-15⁰ C1 to decrease pain and swelling, accomplished by localized inhibition of nerve conduction and vasoconstriction with reduced metabolic need. Cryotherapy burns are uncommon,2,3 with most occurring due to prolonged exposure to cold or a thin barrier covering the ice or cool packs.
Case Discussion
A 55-year-old male was playing soccer, and after sudden burst felt pain on the back of his right calf. He was limping and had difficulty in weight bearing. There was tender medial head of gastrocnemius with normal Achilles tendon. He had no drug allergies, and significant past medical history included ischemic heart disease, psoriasis, rosacea, and colon polyps. Regular medications consisted of atorvastatin, aspirin, ACE inhibitor, metoprolol, hydrocortisone ointment, and moisturizers. He was treated for a gastrocnemius sprain with PRICE, diclofenac, physiotherapy, and follow-up later in the week.
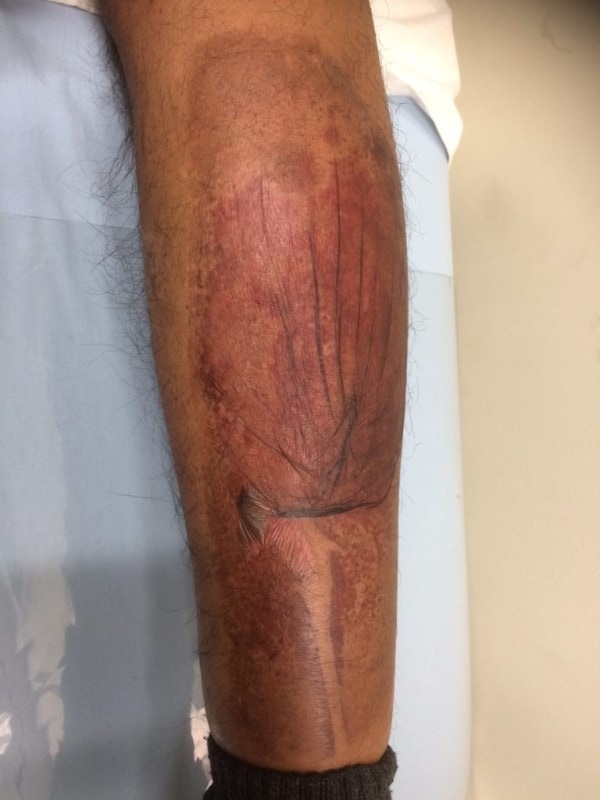
He returned to the clinic the next day with superficial blisters up to 6 x 6 cm surrounded by dark pigmentation on the right calf, thought to be due to direct application of ice for about 4 hours. (See Figure 1.)
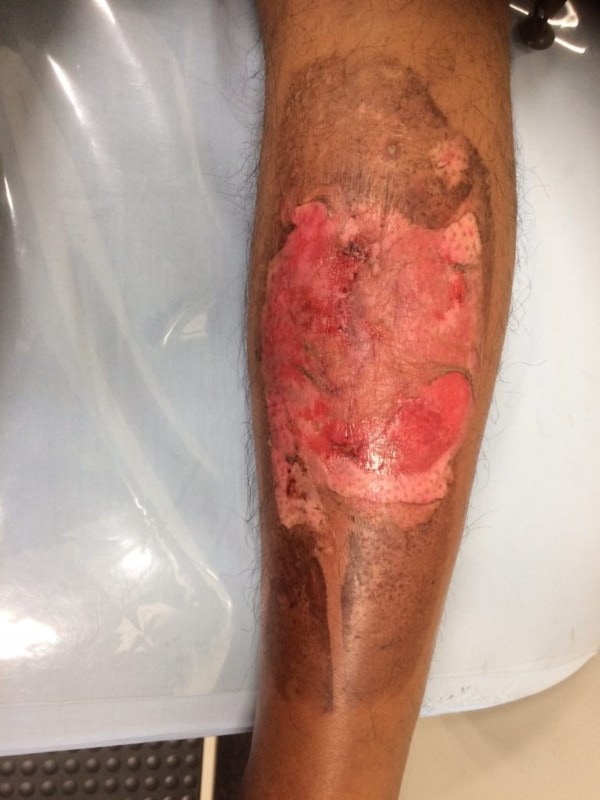
Education on cryotherapy treatment was provided and he was advised to return in 2 days for a wound check, at which time his limping had worsened and the blister size increased to 10 x 11 cm with fluid collection. The bullous lesion was drained, yielding 180 mL of serous fluid. The wound was cleaned with normal saline and dressed with sterile dressing. Regular dressing changes and follow-up were advised. (See Figure 2.)

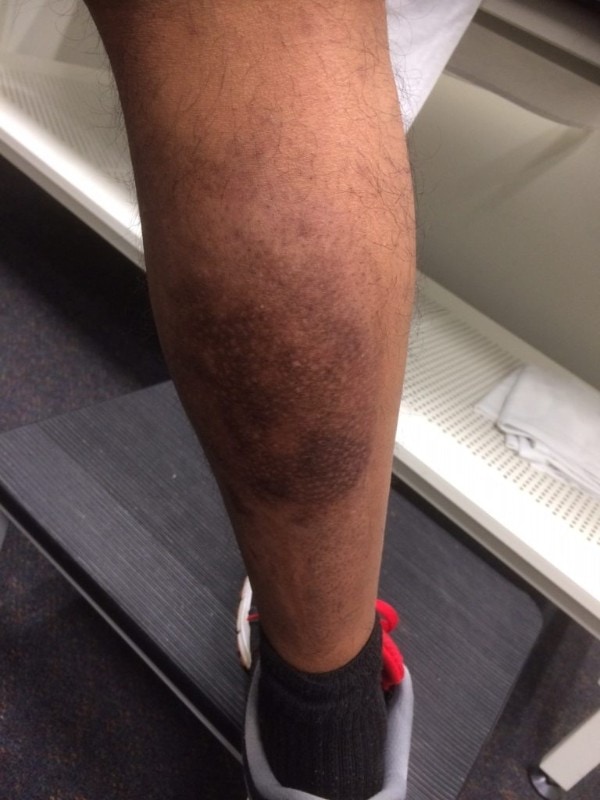
After a week of alternate day dressing in the clinic, he improved considerably, with only a residual small distal blister on calf. He has been walking without a limp but some pain. During the second week of injury, the superficial burn site increased to 17 x 10 cm, but there was no sign of infection and hence dressing continued. (See Figure 3). He improved within the next 2 weeks and continued his physiotherapy for calf strain. (See Figure 4.)
Discussion
Cryotherapy is common and widely accepted with orthopedic injuries. Though cryotherapy injuries may occur from home use, 42% of the complications occur in patients working with athletic trainers, of which 18% are burn related.4
Prolonged application and direct contact of ice on the skin are detrimental and could lead to burns, which further delays the rehabilitation of the injured soft tissue. Scenarios could be more challenging if burns occur on joints, which can lead to contractures and further hinder rehabilitation of the injured soft tissue. Cryotherapy leads to reduced blood flow and metabolism and prolonged exposure causes tissue necrosis and resultant burn.
Effectiveness of Cryotherapy
Though commonly practiced, a systemic review of 22 randomized controlled trials found marginal benefit of cryotherapy after soft tissue injuries.5,6 Few of those studies had good methodology, and further well-controlled trials are necessary for better guidelines on cryotherapy with various types of injuries. Cryokinetics, which is cryotherapy plus exercise, has been gaining momentum. It has shown to be more effective than cryotherapy alone in treating soft tissue injuries.
There are various cryotherapy guidelines,7 generally recommending use in acute setting for 3-10 days. Commercial ice packs are available. If using homemade ice packs, they should be well wrapped to avoid direct contact on skin. Recommend use for 10-20 minutes, 3–4 times per day.8
Burns from such a common treatment modality signify that better education and awareness of PRICE and cryotherapy are needed. In busy urgent care clinics, face-to-face counseling can be further emphasized with written information.
Take-Home Points
Proper use and application of cryotherapy should be explained to patients as to minimize the risks of adverse events like burns.
Kumar A. Post sports injury burn due to inappropriate use of cryotherapy. J Urgent Care Med. November 2018. Available at: https://www.jucm.com/post-sports-injury-burn-due-to-inappropriate-use-of-cryotherapy/.
References
- Bleakley CM, O’Connor S, Tully MA, et al. The PRICE study (protection rest ice compression elevation): design of a randomised controlled trial comparing standard versus cryokinetic ice applications in the management of acute ankle sprain BMC Musculoskelet Disord. 2007;8:125.
- Oksuz S, Eren F, Sever C, Ulkur E. Frostbite injury of the breast: a case report. Ann Burns Fire Disasters. 2014;27(2):105-106.
- O’Toole G, Rayatt S. Frostbite at the gym: a case report of an ice pack burn. Br J Sports Med. 1999;33(4):278-279.
- Nadler SF, Prybicien M, Malanga GA, Sicher D. Complications from therapeutic modalities: results of a national survey of athletic trainers. Arch Phys Med Rehabil. 2003;84(6):849-853.
- Bleakley C, McDonough S, MacAuley D. The use of ice in the treatment of acute soft-tissue injury: a systematic review of randomized controlled trials. Am J Sports Med. 2004;32(1):251-261.
- Hubbard TJ, Denegar CR. Does cryotherapy improve outcomes with soft tissue injury? J Athl Train. 2004;39(3):278-279.
- Mac Auley DC. Ice therapy: how good is the evidence? Int J Sports Med. 2001;22(5):379-384.
- Galiuto L. The use of cryotherapy in acute sports injuries. Ann Sports Med Res. 2016;3(2):1060.
Dr. Amitesh Kumar is a General Practitioner at Bakerfield Medical and Urgent Care in Manukau, Auckland, New Zealand.

