Published on
Urgent message: Acanthosis nigricans has a strong association with obesity and insulin resistance. Assessment involves a thorough physical exam to differentiate from other dermatosis, as well as full workup for insulin resistance. Early diagnosis in the urgent care setting, and treatment, will improve the appearance of acanthosis nigricans, but also the patient’s overall morbidity.
Shailendra Saxena, MD, PhD and Bao Chau Nguyen, BS
Introduction
A 21-year-old Caucasian male presented for a circumferential hyperpigmented rash around the neck that began several months ago.
History
Past medical history was significant for morbid obesity and bipolar disorder. Previous medications included quetiapine fumarate (Seroquel) and bupropion (Wellbutrin). Family history was significant for diabetes in maternal grandmother and negative for gastrointestinal cancers.
Physical Examination
Physical examination was negative for constitutional symptoms. Cardiac exam revealed regular rate and sinus rhythm with no extra heart sounds, murmurs, rubs, or gallops. Pulmonary exam showed clear auscultation bilaterally without rhonchi, rales, or wheezes.
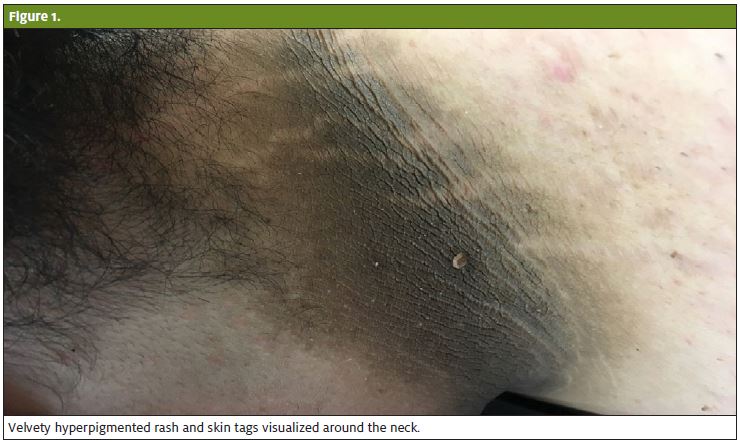
Physical inspection of the neck area revealed circumferential velvety, papular, hyperpigmented rash and skin tags. Areas of rash did not blanch with pressure palpation and were not associated with pruritus or discomfort. The rest of physical inspection was within normal limits.
Differential Diagnosis
- Linear epidermal nevus – benign, linear hyperpigmented plaques that can become more prominent over time
- Confluent and reticulated papillomatosis – hyperpigmented and scaly plaques that occur on the neck, chest, and upper back, often seen in young adults
- Granular parakeratosis – pruritic brown-red plaques that often involve the axilla
Workup
Physical exam suggested the neck rash being acanthosis nigricans due to its chronic nature, as well as the velvety, unblanching characteristics with no pruritus. Patient was also worked up for insulin resistance with fasting serum glucose and hemoglobin A1C. No malignancy workup was done due to his young age, absence of family history, and no signs and symptoms aside from the neck rash.
Diagnosis
His neck rash was determined to be acanthosis nigricans secondary to insulin resistance.
Management
As acanthosis nigricans is associated with diabetes, it was not surprising the patient’s lab results revealed insulin resistance, with fasting serum glucose of 110 mg/dL (normal 70-100 mg/dL) and HbA1C of 6.6% (normal <5.7%). He was started on oral metformin extended-release 750 mg once daily and counseled on lifestyle changes and exercise.
Treatment
Due to the benign and asymptomatic nature of acanthosis nigricans, cosmetic concerns are the focus of available treatments. Methods are divided into three categories: treatment of the underlying disorders, skin-directed treatments, and systemic treatments. These are detailed further in Table 1.
| Table 1. Treatment options for acanthosis nigricans as well as their potential side effects | ||
| Categories | Treatment Types | Outcomes and/or Side Effects |
| Treatment of underlying disorders (preferred method) | · Obesity: encourage weight loss · Insulin resistance: agents that improve insulin sensitivity, such as Metformin · Malignancy: treatment of underlying malignancy |
· Moderate improvement when associated with obesity and malignancy1,2 · Uncertain improvement with insulin resistance3,4 |
| Skin-directed treatments (for those who remained dissatisfied with improvement) | Topical retinoids | Moderate success with 2-week course with few side effects5 |
| Topical vitamin D analogs: reduce keratinocyte proliferation | Moderate success in some patients6 | |
| Other topical agents: urea, salicylic acid, glycolic peels | Moderate improvement after multiple sessions with few side effects7 | |
| Laser therapy | Marked improvement after multiple sessions with few side effects8 | |
| Systemic treatments (reserved for very severe and refractory cases) | Systemic isotretinoin and acitretin | · Moderate success in patients with severe acanthosis nigricans9 · Wide range of potential side effects, such as scaling of the skin and cheilitis5 |
Discussion
Acanthosis nigricans is a benign, asymptomatic dermatosis characterized by velvety, hyperpigmented plaques most commonly found on surfaces of the neck and axilla. A thorough physical exam will differentiate acanthosis nigricans from its dermatosis counterparts, mainly through physical appearance and the absence of pruritis in acanthosis nigricans.
Acanthosis nigricans is closely associated with obesity and insulin resistance. This case study demonstrates the importance of a systemic approach to treating dermatosis in an acute setting. In patients with no history of insulin resistance but who are obese and have acanthosis nigricans, a full workup for diabetes mellitus should be performed. If a diagnosis of diabetes is reached, patients should be counseled on weight loss and started on agents that improve insulin sensitivity.
Rarely, acanthosis nigricans can also be linked with adenocarcinomas of the gastrointestinal (GI) tract.10 A malignancy workup is warranted in patients with GI signs and symptoms. Treatment of underlying malignancy is the preferred therapy for those with malignancy-associated acanthosis nigricans.
In this case, this patient’s presentation of a circumferential neck rash required more than just a topical hydrocortisone treatment; a full workup revealed diabetes mellitus-associated acanthosis nigricans. GI malignancies were ruled out based on the absence of GI symptoms and a negative family history.
With the rising incidence of obesity and insulin resistance in the U.S. population, especially in younger age groups, it is vital for all acute care clinicians to diagnose and treat associated systemic diseases such as diabetes mellitus in cases of suspicious acanthosis nigricans.
Citation: Saxena S, Nguyen BC. Neck rash on a 21-year-old male. J Urgent Care Med. February 2018. Available at: https://www.jucm.com/clearing-up-the-confusion-in-covid-19-testing/.
References
- Kuroki R, Sadamoto Y, Imamura M, et al. Acanthosis nigricans with severe obesity, insulin resistance and hypothyroidism: improvement by diet control. Dermatology. 1999;198(2):164–166.
- Anderson SH, Hudson-Peacock M, Muller AF. Malignant acanthosis nigricans: potential role of chemotherapy. Br J Dermatol. 1999;141(4):714-716.
- Bellot-Rojas P, Posadas-Sanchez R, Caracas-Portilla N, et al. Comparison of metformin versus rosiglitazone in patients with Acanthosis nigricans: a pilot study. J Drugs Dermatol. 2006;5(9):884-889.
- Tankova T, Koev D, Dakovska L, Kirilov G. Therapeutic approach in insulin resistance with acanthosis nigricans. Int J Clin Pract. 2002;56(8):578-581.
- Darmstadt GL, Yokel BK, Horn TD. Treatment of acanthosis nigricans with tretinoin. Arch Dermatol. 1991;127(8):1139-1140.
- Gregoriou S, Anyfandakis V, Kontoleon P, et al. Acanthosis nigricans associated with primary hypogonadism: successful treatment with topical calcipotriol. J Dermatolog Treat. 2008;19(6):373-375.
- Ichiyama S, Funasaka Y, Otsuka Y, et al. Effective treatment by glycolic acid peeling for cutaneous manifestation of familial generalized acanthosis nigricans caused by FGFR3 mutation. J Eur Acad Dermatol Venereol. 2016;30(3):442-445.
- Rosenbach A, Ram R. Treatment of Acanthosis nigricans of the axillae using a long-pulsed (5-msec) alexandrite laser. Dermatol Surg. 2004;30(8):1158-1160.
- Katz RA. Treatment of acanthosis nigricans with oral isotretinoin. Arch Dermatol. 1980; 116(1):110-111.
- Lee SS, Jung NJ, Im M, et al. Acral-type Malignant Acanthosis Nigricans Associated with Gastric Adenocarcinoma. Ann Dermatol. 2011;23(Suppl 2):S208-S210.


