Published on
Urgent message: Complaints of ear pain in children are among the most common presentations in the urgent care setting. While acute otitis media and acute otitis externa are high on the list of possible causes, it is essential that the urgent care provider be prepared to differentiate these from other possible etiologies.
Elizabeth Flasch, MSN, APNP, PNP; Sadia Ansari, MD; Timothy Martin, MD
Citation: Flasch E, Ansari S, Martin T. If not otitis externa…then what? J Urgent Care Med. 2021;15(5):11-15.
INTRODUCTION
Ear pain is one of the most common presentations in urgent care, especially among pediatric patients. Further, acute otitis media (AOM) is the most common condition for which antibacterial agents are prescribed for children in the United States. Clinician visits make up 634 per 100 children during 2005-2006. It is imperative that clinicians differentiate AOM from new onset of otorrhea not due to acute otitis externa (AOE), the most common diagnoses made by clinicians with regional variations based on age and geography.1
The majority of AOE-related visits occur during the summer months (June through August); visits occur most commonly in the South and least commonly in the West.2-4
Rosenfeld, et al noted that data from ambulatory care centers suggest there are about 2.4 million visits for AOE, affecting 1 in 123 persons in the United States. Just less than half of all visits for AOE were for children 5 to 14 years of age. Direct costs are estimated at half a billion dollars annually, and ambulatory care providers spent about 600,000 hours treating AOE.2-4
Clearly, urgent care providers must be able to distinguish AOE and AOM from other causes of otalgia, otorrhea, and inflammation of the external auditory canal. “Ear infections” that do not present as AOE or AOM make for a difficult case in an urgent care setting. In such cases, the treatment and management differ from AOE and AOM. In addition, coordination with a subspecialist is often necessary.
Here, we offer three illustrative cases involving children who presented to Children’s Wisconsin Urgent Care facilities with chief complaints of “ear infection” or “ear pain.”
CASE 1
A 3-year-old female presents with a complaint of “left ear infection” and facial swelling. Symptoms started 36 hours prior to presentation. While cleaning her hair, parent noticed a swelling on outer left ear. The child had been diagnosed with right AOM one month prior and was treated with amoxicillin. Her right ear was not reassessed after completion of treatment. She had a past medical history significant for atopic dermatitis and shellfish allergy which were under good control with low-dose topical steroids as needed. Parent denied fever but stated presence of upper respiratory symptoms.
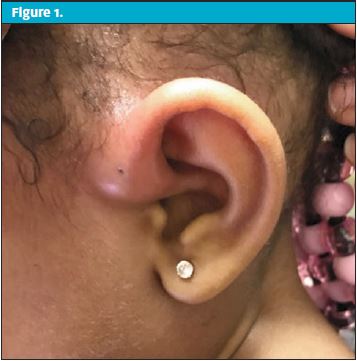
| Exam – Case 1 | |
| Vitals | AfebrileWithin normal limits for age |
| Physical exam findings | Left pinna with moderate-to-significant swelling and a visualized preauricular pitOn palpation, mild to moderate tenderness and mild fluctuance |
| Ear canal | No drainage with dry membranesTympanic membranes were clear bilaterally |
| Nares | Clear rhinorrhea bilaterallyRemainder of the exam was benignPrior to examination, the mother was unaware of the definition of a pre-auricular pit |
| Decision-making/diagnosis | Patient was diagnosed with an infected pre-auricular pit with clearance of the previous AOM |
Treatment
The patient was discharged home on high-dose amoxicillin clavulanate with outpatient referral to otolaryngology for evaluation and possible excision of the preauricular pit. Unfortunately, as you will read, this was likely the incorrect choice for this patient.
Follow-up
The ENT nurses phoned the family the next day to set up an appointment for follow-up. Due to tactile fever and increasing ear pain, as relayed by the parents, the child was referred to the emergency department, where incision-and-drainage (I&D) was performed under sedation by ENT. Bacterial culture was ordered and sent. The patient was discharged from ED with oral clindamycin with outpatient ENT follow-up to be scheduled in 7-10 days. Culture was positive for Serratia marcescens, Aggregatibacter, and coagulase negative Staphylococcus (CONS). The oral amoxicillin clavulanate was recommended to be stopped by the ENT specialist.
Three days later, the family contacted ENT via telephone and reported bloody drainage and “new white patches” on the ear. The patient was evaluated in the outpatient ENT clinic, then admitted immediately after for surgical drainage of the preauricular pit. After drainage of the pit, she was discharged on clindamycin PO (30 mg/kg/day dosed three times daily) for an additional 7 days. Per parent report, this course was completed.
The patient returned to the ENT clinic with continued drainage 3 weeks later. She was started on 10 days of oral ciprofloxacin (40 mg/kg/day dosed twice daily). Due to recurrent infections, the decision was made to excise the pre-auricular pit. She had surgery 2 months postpresentation, with successful resection of the pit.
Discussion
Preauricular sinuses are distinct from first branchial cleft anomalies and derive from ectodermal inclusions formed during development of the external ear. They are quite common in pediatric patients and may present in 1% of Caucasians, 5% of African-Americans, and 10% of Asians. Infants born with pre-auricular pits should have formal audiologic evaluation.
The preauricular sinuses may be the first indication of branchio-oto-renal (BOR) syndrome—one of the most common hereditary causes of hearing lose. BOR is an autosomal dominant syndrome characterized by preauricular pits, branchial cysts or tracts, malformed ears, and renal anomalies, including renal dysplasia and bifid renal pelvises. They may present as cysts and frequently become infected to form abscesses.5-10
First-line treatment of abscess is I&D with oral antibiotics. Following resolution of inflammation, the sinus should be excised to prevent recurrence. Pits are most commonly infected with Staphylococcus species. Edema, erythema, fluid drainage, and pain are common signs infection.
For this case presentation, Serratia species is likely from an exogenous environmental source—water, soil, plants, animals, insects. Serratia species are generally susceptible to fluoroquinolones, aminoglycosides, trimethoprim-sulfamethoxazole, Zosyn (piperacillin and tazobactam), Timentin (ticarcillin and clavulanate), fourth-generation cephalosporins, macrolides, tetracycline, nitrofurantoin, and colistin. CONSwas presumed to be a contaminant.
CASE 2
A 16-year-old female with an insignificant past medical history presents with chief complaint of ear pain, swelling, and “ear infection” for the last 10 days. Cartilage pierced 17 days prior to urgent care visit. Seen at another hospital 10 days prior with erythema and purulent drainage from the piercing site. She was started on high-dose amoxicillin clavulanate 875-125 mg twice daily. Seen again at same hospital, 6 days prior to the visit with worsening symptoms. The patient was referred to a general surgeon’s clinic immediately following her urgent care visit. There, I&D was performed and she was continued on amoxicillin clavulanate 875-125 mg twice daily. Instructions to follow up in 1 week provided. She continued to have worsening swelling, erythema, and purulent thick drainage and thus presented to our urgent care.
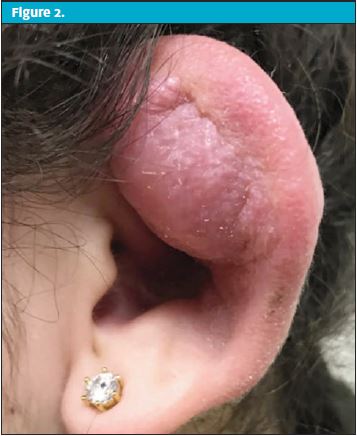
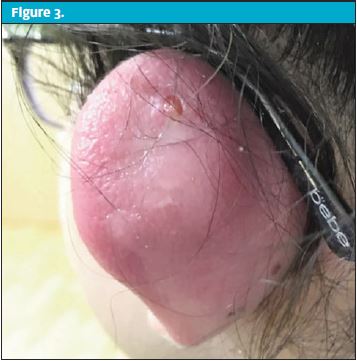
| Exam – Case 2 | |
| Vitals | Heart rate 64Respiratory rate 16Temperature 36.8⁰CWeight 108.2 kg |
| General | AfebrileMild distress with level of pain reportedPatient tearful with examiner |
| Ear | On inspection of left pinna: auricular erythema with significant swellingOn palpation, moderate to severe tenderness with fluctuance noted |
| Decision-making/diagnosis | Cellulitis of left ear with abscess, perichondritis of left earDigital images taken via Haiku into EPICENT phone consult done during urgent care visit. ENT recommended admission with intravenous antibioticsAfter admission, she was started on IV ciprofloxacin (400 mg every 12 hours) with plans for I&D in the operating room |
Follow-up
After successful I&D and short hospital stay (72 hours), the patient was discharged on 10 days of oral ciprofloxacin (500 mg every 12 hours). An aerobic and anaerobic culture was sent and grew few Pseudomonas aeruginosa which were susceptible to ciprofloxacin (pan-susceptible). She followed up in ENT clinic 2 weeks later. During that visit, her ear was noted to be healing well. Three months after the initial urgent care visit, the ear was healed with a residual defect in the cartilage.
Discussion
Auricular abscess/perichondritis complicating helical ear piercing is a frightening complication of the traumatized ear that can lead to a residual deformity. These piercings are associated with poor healing and more serious infection due to the avascular nature of auricular cartilage. Piercings are usually carried out by nonauthorized or untrained professionals with no consensus on asepsis techniques. The risk of developing infection is higher in the ear cartilage than in the lobe.11-17
Pathogens
The most common pathogen is Pseudomonas aeruginosa, followed by Staphylococcus aureus.17 Symptoms usually develop between 3 days and 4 weeks after the ear piercing and include pain, erythema, edema, and abscess formation. Diagnosis is clinical; wound culture with antibiogram must be performed. Fluoroquinolones are the treatment of choice since they show antipseudomonal activity in addition to anti staphylococcal effect. Once an abscess develops, surgical I&D is often necessary. Good cosmetic preservation of the cartilage is difficult to maintain.11-17
CASE 3
An 8-year-old female presented to urgent care with a 12-hour history of ear “redness.” She complained that her ear felt “thick” and warm to the touch. She had minimal pain. She denied drainage, difficulty hearing, fever, URI, or trauma. She had been swimming quite a bit in the days leading up to the visit. There was no known injury or trauma to the ear. Past medical history and surgical history were negative.
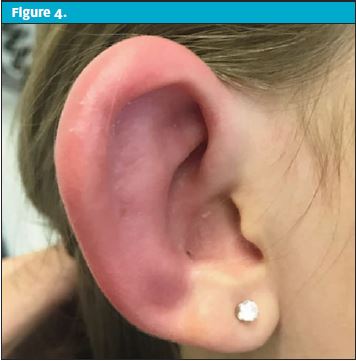
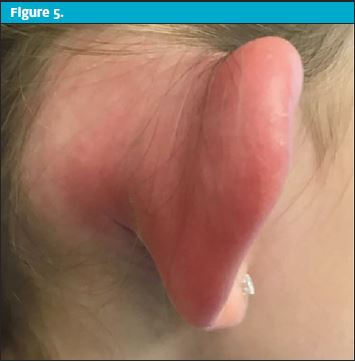
| Exam – Case 3 | |
| Vitals | Heart rate 80Respiratory rate 20Temperature 37.7⁰ CWeight 28.1 kg |
| Ear | Significant and well-demarcated erythemaNo pain to mastoid process or the entire helix |
| Decision-making/diagnosis | Digital images taken via Haiku into EPICENT consult via telephone during urgent care visitThe patient was admitted for IV antibiotics. The ENT resident initially started nafcillin for Staphylococcus coverage and was later changed to ceftazidimeDiagnosis of perichondritis thought to be caused by a previous injury/laceration to the ear that had gotten infectedAlthough the patient denied injury/trauma, the likely cause of the perichondritis was some injury with infection from her recent swimming |
Follow-up
The patient was discharged home after 1 day of IV antibiotics. She was switched to 10 days of ciprofloxacin (500 mg twice daily for 10 days) and clindamycin (300 mg every 8 hours for 10 days).
Discussion
Perichondritis is an infection of the pinna. Pseudomonas and Staphylococcus species are the most common pathogens6,13 (Staphylococcus species being the major pathogen in non-abscess perichondritis6). Pseudomonas is widespread in nature and thrives on most surfaces and is known to cause otitis externa, keratitis, hot tub folliculitis, postoperative abscesses and burn infections. Double antibiotic therapy is recommended with a penicillin and fluroquinolone.6,13
CONCLUSION
There is a broad differential for outer ear infections. Patients presenting with a chief complaint of “ear infection” or “ear pain” automatically prompt the clinician to consider AOM and AOE. However, a detailed history and thorough examination can aid in assessing for preauricular sinus infection, infected piercing site, or perichondritis on the differential diagnosis list.
In these conditions, implicating pathogens are more likely to include Pseudomonas and Staphylococcus species. Antibiotic resistance rates are high. Intravenous antibiotics, hospitalization, surgical I&D and culture may be necessary. Oral antibiotics may require double coverage. Augmentin is used often and is the incorrect choice. Consultation with ENT is often necessary to preserve the form and function of the ear.
References
- Lieberthan, A, Carroll, A., Chonmaitree, T, et. al (2013). The Diagnosis and Management of Acute Otitis Media. Pediatrics. 131 (3), e964-e999.
- Rosenfeld RM, Schwartz SR, Cannon CR, et al. (2014). Clinical practice guideline: acute otitis externa. Otolaryngology Head Neck Surgery. 150:S1.
- Rosenfeld RM, Singer M, Wasserman JM, Stinnett SS. (2006). Systematic review of topical antimicrobial therapy for acute otitis externa. Otolaryngology Head Neck Surgery. 134:S24.
- Rosenfeld RM, Brown L, Cannon CR, et al. (2006). Clinical practice guideline: acute otitis externa. Otolaryngology Head Neck Surgery. 134:S4.
- Bellini C, Piaggio G, Massocco D, et al. (2001). Branchio-Oto-renal syndrome: a report on nine family groups. American Journal of Kidney Disease. 37:505-509.
- Ehlers Klug, T., Holm, N., Greve, T., Ovesen, T. (2019). Perichondritis of the auricle: bacterial findings and clinical evaluation of different antibiotic regimens. European Archives of Oto-Rhino-Laryngology (276): 2199-2203
- Huang XY, Tay GS, Wansaicheong GK, Low WK.(2007)Preauricular sinus: clinical course and associations. Archives of Otolaryngology and Head & Neck Surgery. 133:65-68
- Kugelman A, Tubi A, Bader D, et al. (2002). Pre-auricular tags and pits in the newborn: the role of renal ultrasonography. The Journal of Pediatrics. 141:388-391.
- Roth DA, Hildesheimer M, Bardenstein S, et al. (2008). Preauricular skin tags and ear pits are associated with permanent hearing impairment in newborns. Pediatrics. 122:e884-890.
- Scheinfeld NS, Silverberg NB, Weinberg JM, Nozad V. (2004). The preauricular sinus: a review of its clinical presentation, treatment, and associations. Pediatric Dermatology. 21:191-196Isaacson, G. (2019). Comprehensive management of infected preauricular sinuses/cysts. International Journal of Pediatric Otorhinolaryngology (127).
- Keene WE, Markum AC, Samadpour M. (2004). Outbreak of Pseudomonas aeruginosa infections caused by commercial piercing of upper ear cartilage. Journal of the American Medical Association. 291:981-985.
- Lee TC, Gold WL. (2011). Necrotizing Pseudomonas chondritis after piercing of the upper ear. Canadian Medical Association Journal. 183:819-821.
- Mitchell, S., Ditta, K., Minhas, S., & Dezso, A. (2014). Pinna Abscesses: Can we manage them better? A case series and review of the literature. European archives of Oto-rhino-laryngology. 272, (11), 3163-3167.
- Rodriguez, J., Thone, N., Duque, J., Branes, R. (2019). Infected transcartilaginous ear piercings. A case report and review of the literature. Revista de Ciencias Medicas (44), 2, 23-25.
- Rowshan HH, Keith K, Baur D, Skidmore P. (2008). Pseudomonas aeruginosa infection of the auricular cartilage caused by “high ear piercing”: a case report and review of the literature. Journal of Oral Maxillofacial Surgery. 66:543.
- Sosin M, Weissler JM, Pulcrano M, Rodriguez ED. (2015). Transcartilaginous ear piercing and infectious complications: a systematic review and critical analysis of outcomes. Laryngoscope. 125:1827-1834.
- Stewart, G., Thorp, A., & Brown, L. (2006). Perichondritis-A Complication of High Ear Piercing. Pediatric Emergency Care. (22), 12, 804-806.
Author affiliations: Elizabeth Flasch, MSN, APNP, PNP, Department of Urgent Care, Division of Primary Care, Children’s Wisconsin; Marquette University College of Nursing. Sadia Ansari, MD, Department of Urgent Care, Division of Primary Care, Children’s Wisconsin. Timothy Martin, MD, Department of Otolaryngology, Children’s Wisconsin; Medical College of Wisconsin. The authors have no relevant financial relationships with any commercial interests.

