Published on
Physical Examination
On physical examination, the patient’s vital signs are as follows:
- Temperature: 97.8°F (37.1°C)
- Pulse: 112 beats/min
- Respiration: 20 breaths/min
- Blood pressure: 168/102 mm Hg
- Oxygen saturation: 99% on room air
The patient is alert and oriented, is in no acute distress, and is breathing comfortably but slightly faster than normal. His lungs are clear to auscultation. His heart rate and rhythm are regular, without murmur, rub, or gallop. His abdomen is soft and nontender; there is no rigidity, rebound, or guarding. The right foot has a normal skin color, but there is swelling over the mid-dorsal aspect of the foot. There is pain with palpation over the proximal aspect of the second metatarsal, but no palpable fracture. The dorsal pedal pulse is 2+, and sensation is grossly intact. The patient has no history of previous illnesses and does not take any medications. He reports that he smokes but does not drink alcohol.
Urgent Care Work-Up
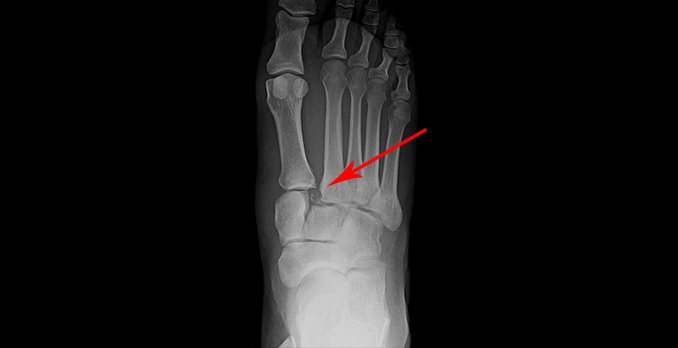
An x-ray is obtained that shows evidence of a Lisfranc injury (Figure 2). Note the widened space between the proximal aspect of the first and second metatarsal bones as well as presence of a fracture fragment.
Differential Diagnosis
- Cuboid fracture
- Cuneiform fracture
- Ankle dislocation
- Osteolytic lesion
- Osteomyelitis of the second metatarsal
Diagnosis
Lisfranc fracture.
Learnings
The key to understanding the importance of a Lisfranc fracture or dislocation is to understand the importance of the tarsometatarsal joint complex. The foot is divided into the hind foot (rear foot), midfoot (3 cuneiform bones, 1 cuboid bone, and 1 navicular bone), and the forefoot (starting from the proximal aspect of the metatarsals and extending distally). The division of the midfoot and the forefoot is called the Lisfranc joint. The proximal aspect of the 5 metatarsal bones approximate with the 3 cuneiform bones and the cuboid bone. The stability of the foot is determined by the bony approximations, the ligamentous attachments, and the arch configuration of the dorsal foot. The second metatarsal is attached to the medial cuneiform by the strong Lisfranc ligament.
Lisfranc injuries are relatively uncommon. Midfoot fractures overall represent 0.4% of all fractures in adults, but Lisfranc fractures are a subset of these, representing 0.2%. The presentation can be subtle, with 20% of injuries being missed initially, possibly resulting in chronic pain. The incidence of vascular complications has declined and is now typically present only with concomitant compartment syndrome.
Evaluation of foot pain should include questions as to the following:
- Mechanism of injury: The typical mechanism of a Lisfranc fracture or dislocation is a sudden impact to the foot, such as from a motor vehicle collision, a direct impact, or a fall from height. Injury may also occur from seemingly minor events such as twisting in athletes or the elderly.
- Onset: Was pain onset gradual or sudden?
- Location: The typical location of pain is dorsal over the tarsometatarsal junction.
- Duration
- Character
- Severity: Pain from a Lisfranc injury is typically severe.
- Associated symptoms: Inquire about symptoms of fever, redness, and weight loss, though the presence of gout, cancer (bone or metastatic), infection, or subacute bacterial endocarditis is unlikely with a typical mechanism of injury.
- Tetanus status: Inquire about tetanus status if there are cuts or breaks in the skin.
During the physical examination, it is important to do the following:
- Obtain vital signs: Check for fever, tachypnea, and tachycardia.
- Inspect the skin: Look for swelling, erythema, ecchymosis, and tenting of the skin.
- Palpate for the site of greatest pain: This will typically be located dorsally at the tarsometatarsal joint complex.
- Assess for swelling.
- Assess range of motion: Gently check range of motion at the toes and ankle.
- Assess the ability to bear weight.
- Assess for the presence of a crush injury: With a crush injury, there will typically be evidence of swelling, ecchymosis, and bruising, but with a noncrush injury, the foot will be pronated and abducted, which may cause pain and is specific for tarsometatarsal injury.
X-rays are the initial test of choice. The normal alignment of the proximal second metatarsal demonstrates the alignment of the medial aspect with the medial margin of the middle cuneiform bone. The appearance of a tarsometatarsal dislocation or fracture is as follows on radiographs:
- Loss of the normal anatomy, with displacement of the proximal metatarsal bones relative to the distal aspect of the 3 cuneiform bones and the cuboid bone bone
- Widening at the base of the first and second metatarsals (or the more lateral proximal metatarsals) that is >2.5 mm
- Widening between the middle and medial cuneiform bones
- Flake fracture (formerly called a fleck sign), which is a fracture at the base of the second metatarsal or cuneiform
- Impaction fractures of the cuboid, medial cuneiform, or navicular bones
- Apparent fracture or dislocation or both, or appearance of no injury
Treatment
Most patients with a Lisfranc fracture or dislocation will be sent to an emergency department for reduction, surgery, and/or orthopedic consultation. Patients with a good social support system can be transported by private automobile. Other indications for transfer include the following:
- Associated major trauma
- The possibility of neurovascular compromise
- The possibility of compartment syndrome (the “5 P’s”):
- Pain
- Paresthesia
- Pallor
- Pulselessness
- Paralysis
- Uncontrolled pain