Published on
Urgent message: The high specificity but broad range of possible causes associated with a primary complaint of lower extremity edema poses a particular challenge to the urgent care clinician. Proper assessment of the differential diagnoses is the first step toward optimal outcomes, whether they be facilitated by treatment or referral.
Michael S. Miller, DO
Patients presenting to urgent care with a primary complaint of edema of the lower extremities of any duration can pose a particularly vexing challenge for the practitioner. While the symptom is quite specific, it could be indicative of any number of diagnoses; is the root cause chronic venous insufficiency, or a more emergent condition requiring immediate referral (e.g., deep vein thrombosis)?
Further, how do you differentiate between stasis dermatitis and cellulitis, thereby avoiding inappropriate antibiotic therapy?
Such determinations are essential preparation for choosing appropriate treatment or referring the patient to the appropriate setting for care.
Introduction
The word circulation is often misused by physicians or misunderstood by patients. While it is usually used in reference to the peripheral blood flow in the arteries, circulation more properly refers to the entire course of blood flow from the heart through the peripheral arteries of the distal tissues via the capillaries, all the way to its return via the venous system to the heart.
Patients may find it easier to grasp the true meaning if you explain that the word itself was derived from the Latin word circulare – to make a circle.Equally problematic is the diagnosis of “poor circulation” made by a simple visual inspection of the legs when, in fact, no arterial compromise exists. Consideration should always include both the arterial and the venous.
Arterial circulation can easily be assessed via a well-taken history (“How far can you walk? Does the pain make you stop walking? Do you have to rest – and for how long?”, etc.), palpation of the pulses, or Doppler signals (though the latter is unlikely to be employed in the urgent care setting). The venous system has been somewhat more diagnostically elusive, however, save for the presence of varicose veins.
The Peripheral Venous System
In fact, the peripheral venous system is itself fairly simple to assess. To review: The capillaries receive deoxygenated “dirty” blood from the tissues/cells, and transfer it to larger venules which combine into veins. While capillary filling is hydrostatic in nature, the propulsion of venous blood from distal to proximal involves a slightly more active system.
A cross section of the leg would show the outer layer of skin, a subcutaneous fat layer, a circumferential supporting fascial layer, and then the deeper structures of muscle, bone, arteries, veins, etc. In simplest terms, activation of the calf muscle squeezes the veins against the fascia, creating an internal pressure to move the venous blood. One-way valves allow the blood to go either distal to proximal or from superficial to deep to the larger veins (which then go distal to proximal). Each squeeze of the muscle actively promotes this flow.
Elevating the legs simply and passively allows the blood to follow the same flow course but at a much reduced rate since there is only gravity (and at an angle less than 90°) to move the blood. This is how venous return occurs.
Of course, it is easy to see how compromise can also occur. Pregnancy, obesity, trauma, genetics, and surgery of adjacent or proximal areas or on the veins themselves (such as removal for a bypass) can all increase the intravenous pressure, thus creating venous hypertension.
Early on, venous dilatation may present as either small spider veins or larger varicose veins. These occur when the superficial veins become engorged from venous hypertension and bulge through the superficial fascia. (If you take your finger and run it transversely across a varicose vein, you will feel the edges of the fascia it is bulging through.)
Continued hypertension damages the venous valves, which can deform, leak, and ultimately fail, allowing for retrograde venous blood flow that further exacerbates venous hypertension. This causes compromise to the venous walls, allowing for leakage of fluids and blood components, including fibrin.
It has been theorized that leakage of fibrin leads to formation of a cuff around the vein, which compromises the respiration of the venous walls. As this fibrin cuffing increases, damage to the vein walls allows for leakage of additional substances and fluids which can now reach the tissues from which they originated. This results in tissue injury and loss of the fascial integrity; venous return is worsened, leakage increases, and a various cycle commences.
Initially, hyperpigmentation and red-brown discoloration from red blood cell extravasation appear (hemosiderin deposition). Later, eczematous changes develop and manifest as erythema, scaling, weeping, and crusting, all of which can be made worse by bacterial superinfection or by contact dermatitis from the many topical antimicrobial treatments often applied inappropriately, based on the erroneous assumption of infection.
Stasis Dermatitis
As the disease progresses, episodes of diffuse inflammation of the leg, called stasis dermatitis, can develop acutely over hours or days. Symptoms include itching, scaling, and diffuse inflammation. Interestingly, this is not usually associated with pain, fevers, and abnormal lab studies such as elevated white blood cell count.
However, patients will frequently present with a history of multiple episodes and a misdiagnosis of cellulitis, in spite of the fact that their presentation, clinical findings, and work-up do not support this diagnosis. More interestingly, a review of their history does not reveal etiologies for these recurrent “infections.”
Thus, it is important to remember that this process is inflammatory, not infectious, in nature.
When chronic venous insufficiency and stasis dermatitis are bother treated inadequately, progression to frank skin ulcerations called venous insufficiency ulcers (in the past referred to as venous stasis ulcers) occurs. While this a relatively rare presentation in urgent care, it is important to remember that venous insufficiency may be part of the bigger clinical picture for many patients who do present.
This constant and/or recurrent inflammation and scarring gives the deeper tissues a “woody” feel with incompressible skin better known as lipodermatosclerosis (Figure 1). If untreated, this often gives the lower leg an “inverted Coke bottle” shape with enlargement of the calf and narrowing at the ankle (Figure 2). The skin itself may have a shiny appearance and becomes hairless.
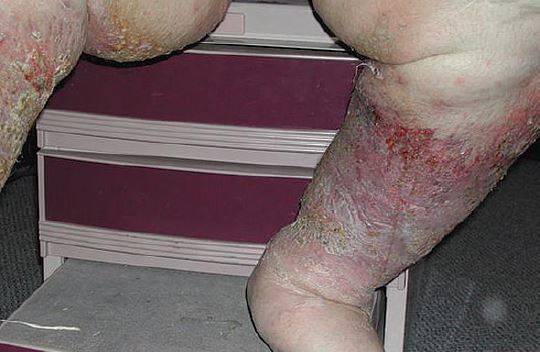
As these tissue injuries heal, they may leave a whitish scar called atrophie blanche at the site (Figure 3). This is a sign that the tissue did not heal normally, but was replaced by a more rigid, less elastic tissue more prone to injury.
Differential Diagnoses
It is imperative to consider and evaluate the differential diagnoses of chronic venous insufficiency, as several have serious consequences if not identified and treated.
Congestive heart failure
Congestive heart failure may mimic venous disease with the presentation of edema of the ankles and lower legs. However, one early but subtle symptom of congestive heart failure is fatigue; this can be so subtle that the patient may not even sense decrease in energy and may subconsciously reduce activities to accommodate this limitation.
As the heart failure progresses, bilateral swelling (edema) of the ankles and legs or abdomen may be noticed. Based on the pathophysiology of the disease, it rarely presents solely unilaterally, though one leg may be worse than the other. In addition, fluid may accumulate in the lungs, thereby causing shortness of breath, particularly during exercise and when lying flat. In some instances, patients awaken at night, gasping for air. Some may be unable to sleep unless sitting upright. The extra fluid in the body may cause increased urination, particularly at night.
These findings are uncommon in primary venous disease.

due to scarring and contraction of the lower leg.
Deep venous thrombosis
Due to its significant sequelae (specifically, pulmonary embolism), deep venous thrombosis (DVT) is another condition that must be ruled out when performing a work-up in the urgent care setting. Many patients later found to have DVT are asymptomatic. However, classic signs and symptoms are associated with obstruction to venous drainage. Pain and unilateral leg swelling can be seen. Nonspecific findings include warmth, erythema, a palpable cord in the tissues of the leg, pain upon dorsiflexion of the foot, and pain in the calf on forced dorsiflexion of the foot with knee straight (Homan’s sign).
When a patient presents with these symptoms, a diagnosis of DVT is strongly suggested. However, treatment should not be initiated base on clinical findings alone; even when a patient has a swollen, painful, congested leg, there is only a 50% chance that DVT is the correct diagnosis. Unfortunately, absence of these signs and symptoms does not rule out DVT.
Risk factors for DVT that can be ascertained by questioning the patient or family member include long periods of immobility, recent surgery or trauma to the lower body, obesity, heart attack, heart failure, recent childbirth, use of hormone therapy or oral contraceptives, and advanced age.
The presence of a DVT cannot be diagnosed or excluded based on clinical findings; thus, diagnostic tests must be performed whenever the diagnosis of DVT is being considered. Many of these, such a Doppler ultrasound and venography, are likely to be beyond the means of most urgent care centers. Hence, suspicion of DVT warrants immediate referral.

of the inferior wound on this. Posterior is a whitish scar from a previously
healed ulcer called atrophae blanche.
Cellulitis
Cellulitis is, primarily, a true infectious process that initiates with some type of traumatic event resulting in a break in the skin of the lower extremity. There is an identifiable progression from the skin and tissue injury to a diffuse inflammation, with associated findings of elevated temperatures, pain in the affected extremity, redness, and swelling.
In cellulitis, this usually follows the skin injury; in venous disease, there is usually an episode history of “cellulitis” prior to the acknowledgement of any skin trauma.
Other possibilities
Other possible causes of lower extremity edema include renal failure, endocrine abnormalities such as Crushing’s disease or hyperthyroidism, and use of medications such as corticosteroids, birth control pills, antibiotics with higher sodium content, and nonsteroidal anti-inflammatory drugs.
Lab Considerations
With any disease entity, the clinician could order every conceivable lab test to rule in/out every eventuality that may present with similar signs and symptoms. However, particularly in the urgent care setting, it is best to rely on the time-honored practice of ordering a lab test only if it will change your diagnosis and your decision to treat or refer.
If the patient has previous labs, reviewing them may give you a clue that their presentation has been previously evaluated and save you the time and cost of an unneeded work-up. In addition, the history and physical examination should provide sufficient guidelines as to what labs may be beneficial.
If you feel further evaluation and labs are warranted, referring the patient for further testing is a valid option. As always, it is important to document this recommendation and to ensure that the patient or family member understand the possible consequences of failing to follow through.
A Focused Approach to Treatment
Once you have considered differential diagnoses and understand that the etiology is based on valvular dysfunction and loss of the fascial integrity, you can focus on treatment likely to solve these problems.
It may also become more evident why frequently used treatments such as whirlpools, antibiotic creams, oral or intravenous antibiotics, silver sulfadiazine (Silvadene, Thermazene), wet-to-dry dressings, and topical or systemic steroids don’t work; they simply are not addressing the problem, which is threefold:
- dilatation of the veins
- separation of the valves
- damage to the fascia.
Appropriate treatments usually involve a commercially prepared multilayer wrap system of between two and four layers applied to the leg from the foot to the level of the knee, with each layer performing a distinct function:
- Layer 1 consists of cotton padding that absorbs moisture and shields the skin.
- Layer 2 is a short stretch wrap that provides low resting pressure and high working pressure.
- Layer 3, conversely, provides high resting pressure and low working pressure.
- Layer 4 – the layer furthest from the surface of the skin – surrounds the other three layers, ensuring that they work in concert.
Together, these provide both support to the fascia and compression to the valvular structures. In essence, the pressure is increased so the retrograde flow is corrected. In the two-layer system, layers 1 and 2 and layers 3 and 4 above are combined into two discrete layers which serve the same function.
Application of a skin cream may help ensure that the skin remains moist and healthy. I do not recommend the use of skin “lotions” as these have higher water content and are absorbed too quickly to provide long-term skin hydration.
These products are worn from three to seven days, depending on how much drainage there is from the legs. I do not recommend using Unna boots (zinc oxide paste wraps), particularly in an urgent care settings, since this product tends to stop working after eight hours and to dry out the skin. There also tends to be less compression; as the edema resolves, the zinc oxide layer does not shrink and thus, there is neither contact nor pressure from the wraps to the skin.
For patients unable to tolerate wearing wraps 24 hours a day for the prescribed period of time, or tolerate compression during nocturnal periods of sleep, other treatments can be applied every morning and removed prior to going to bed.
Clearly, some of these treatments options beg follow-up care likely to be administered by another clinician. Again, it is virtually important that the patient or caregiver understood this, and that you document any recommendation you make to that effect.
Compression stockings
Once active treatment with any of the aforementioned is completed and the venous insufficiency is well controlled, patients should be measured for a pair of compression stockings. This involves measuring the circumference at both the ankle and the calf. Elastic stockings are used to prevent the problem from recurring, but because they stretch and are not stiff, they only correct for the valve problem and not the fascial problem; therefore, they are inadequate for true “treatment.”
Practitioners must ensure that patients understand that even if they wear the stockings continuously, swelling may recur and the compression wraps will need to be replaced. Once the venous system and structures are damaged, it is unlikely they will ever be “normal” again. The key is to keep the veins functioning with compression.
We have found it effective to advise patients to think of the compression as they would medicine for a chronic condition (e.g., in the way that a patient with diabetes must continue taking insulin even if they feel better). Continuing treatment helps control the disease.
There are studies showing that pentoxifylline (Trental) is beneficial in reducing the risk of venous-related problems such as ulcers. This medicine works on the fibrin cuffing around the veins, allowing for better nutrient exchange. Use of other treatments such as nitroglycerine patches, phenytoin (Dilantin), or other compounds thought to improve peripheral circulation has not been shown to be effective in treating venous disease.
Conclusion
The presence of lower extremity edema should induce you to identify the etiologies. It is imperative to identify the cause prior to referral or initiation of treatment, as the varied causes preclude a “magic bullet” approach such as diuretics or leg elevation.
Indeed, the knee-jerk use of antibiotics as first-line treatment without a work-up subjects the patient to additional time untreated and to the potential untoward sequelae of their inappropriate use.

