Published on
Urgent message: Sports-related concussions are particularly dangerous injuries due to their complex nature and difficulties associated with diagnostic and return-to-play decisions. Some of the most commonly employed assessment tools have been shown to be unreliable, leading to misdiagnoses. Guidelines for selecting more effective concussion assessment instruments and the use of such tests in urgent care settings are here suggested as an optimal framework for improved care.
Len Lecci, PhD, MA
Introduction
Millions of adults, adolescents, and children participate in sport-related activities that place them at risk for concussion. Among those who are inured in this way, the majority experience mild symptoms. Currently, the instruments that are most commonly used to assess sport-related concussions have been shown to be highly problematic with respect to reliability and validity, resulting in inaccurate diagnostic and return-to-play decisions. Here, we present tests that may be more effective, along with basic guidelines for selecting better concussion assessment instruments.
Each year, an estimated 38 million children and adolescents participate in organized sports in the United States; an additional 170 million adults participate in physical activities including sports. Many of these activities are associated with an increased risk of injury. One form of sports-related injury that has been the target of increased scrutiny is concussion, sometimes referred to as a traumatic brain injury (TBI). Approximately 1.7 million people seek medical attention for TBI every year in the United States, and approximately 75% of these injuries are considered mild in nature. These figures are in keeping with CDC estimates that between 1.6 and 3.8 million concussions occur in sports and recreational activities annually. Moreover, among children, injuries associated with participation in sports and recreational activities account for 21% of all traumatic brain injuries.1
Various guidelines that define the nature of a concussion have been published, with no single agreed-upon definition (eg, CDC; Veterans Affairs/Department of Defense Clinical Practice Guidelines; American Congress of Rehabilitation Medicine). However, what is common to all definitions is that the injury is induced from a direct or indirect impact to the head, face, neck, or elsewhere.
Concussed individuals can present with a wide range of clinical signs, including behavioral changes (eg, dizziness, change in gait, balance problems, loss of consciousness); cognitive changes (eg, slowed reaction times, amnesia, feeling “in a fog,”); sleep disturbance (eg, drowsiness or inability to sleep); somatic symptoms (eg, headaches); and/or emotional symptoms (eg, irritability, emotional lability). In many instances, milder forms of concussion (also referred to as mild traumatic brain injuries, or mTBIs) result in normal or “unremarkable” brain imaging, despite the reporting of subjective symptoms. Consequently, the known incidence of mTBIs likely underestimate the actual incidence of mTBIs because many individuals fail to seek medical care. This may be especially true when the symptoms appear to resolve or are less pronounced. A particularly dangerous aspect of concussions is that they compound, meaning that mild concussions, if untreated or otherwise ignored, can quickly and suddenly escalate with reinjury into categorically more serious and threatening conditions.
Because of the nature of recreational sports, a significant number of these activities (and the resulting injuries) occur in the evenings and on weekends when doctors’ offices are closed. This means that if the injured party chooses to seek medical attention, the viable options are the ED and urgent care. It is here proposed that a formal triage model is the best way to address concussions, such that the injured party or a third party can be used to determine when an ED visit is in order. ED visits are indicated when the more severe concussion symptoms are present, such as nausea, vomiting, loss of consciousness, balance problems/dizziness, confusion, light sensitivity, and pupil-size asymmetry. However, if a head injury occurs and the above-noted symptoms are not present, then there is still a need to evaluate the injured party for more subtle symptoms. The urgent care environment is best suited for this task.
The challenge is to establish best practices in urgent care that can detect subtle symptoms, increase the accuracy of return-to-play decisions, and interface with specialists (eg, neurology and neuropsychology) and general practitioners as needed. To accomplish this goal, urgent care facilities need to be equipped with the tools necessary to provide a thorough, sensitive, yet efficient screening assessment. In these next sections, we will outline what should constitute best practices.
Current limitations
Concussions affect numerous brain functions, including both neurocognitive processes and motor control. Failure to assess either of these domains will weaken the sensitivity of any assessment. Therefore, it is important to measure neurocognitive and neuromotor functioning with the best instruments available.
To select the best measures to support diagnostic decisions, it is important to consider: 1) reliability, which is the consistency of a test, and 2) validity, meaning the extent to which the test measures what it is supposed to measure.
Reliability and validity are related because a test can only be valid if it is first shown to be reliable. As an illustration, imagine you have a blood pressure measure on a healthy patient that provides the following readings three times over the span of 10 minutes; 120/80, 90/40, and 175/145. Assuming the machine was used correctly, the data suggest that the machine is producing inconsistent (ie, unreliable) blood pressure readings. Importantly, when reliability is poor, the values do not accurately inform us of the individual’s BP (ie, no validity). Moreover, when a test has low test-retest reliability, as would be the case in this illustration, knowing their score at one point in time (eg, 120/80) would not provide any information about what their score might be the next time it is measured (potentially ranging from 90/40 to 175/145). Thus, the measure is not clinically useful, as one would not intervene or make clinical decisions based on these unreliable estimates of blood pressure. The same is true for any test purporting to assess the consequences of a head injury.
ImPACT and SCAT
It is important to evaluate some of the most commonly used measures to assess sports concussions today. The two most prevalent tests used in recent years are the Immediate Post-Concussion Assessment and Cognitive Test (ImPACT) and the Sport Concussion Assessment Tool (SCAT). The ImPACT and SCAT test batteries have been instrumental in contributing to the greater standardization in concussion assessments, in that they introduced and proliferated methods for the measurement of multiple domains when concussions are suspected.
The cognitive and motor tests that are employed in these batteries are not fully appropriate for evaluating the functions impaired in concussion; as a result, they have been shown to have disturbingly poor reliability and validity. For example, ImPACT is highly variable in terms of its reliability, as most studies found values well below 0.7, which is considered the minimum accepted value for an assessment instrument. (Reliability coefficients range from 0, meaning no association between the two scores, and 1.0, meaning a perfect correspondence between repeated measurements). Moreover, some reviews have found the test-retest reliability to be as low as .15 to .22,2 indicating that an individual could take the test on two separate occasions and obtain widely differing scores. This would essentially make it impossible to know if the variation in scores reflects concussive symptoms in an injured individual or is simply due to the fluctuations of an unreliable measurement.
Poor reliability also undermines validity, which is likely why ImPACT scores do not effectively predict performance on other well-validated instruments assessing the same cognitive functions ImPACT is purported to measure.3 Additionally, ImPACT scores have been shown to not relate to, indicate, or account for concussion history.4 Critically, ImPACT has very high misclassification rates, as anywhere from 1 in 4 to almost 1 in 2 healthy individuals are misclassified as concussed.5 Cases in which ImPACT shows concussed individuals to not have symptoms have also been documented, with even more problematic outcomes. Indeed, the danger of relying on insensitive, unreliable methods to monitor concussion and recovery was illustrated in the case of Kenny Bui,6 who died in 2015 after being cleared to play football just weeks after suffering a concussion. The same Wall Street Journal article also highlights a recent large-scale, 3-year longitudinal study tracking 28,000 athletes showing that many individuals are similarly being returned to play prematurely based on what appears to be inaccurate information from ImPACT. Given these problems, it is not surprising that medical researchers have concluded that ImPACT is not sufficiently accurate to support important medical decisions, including timing for return-to-play.7
The SCAT is slightly better than ImPACT with respect to reliability, but even its values might be deemed unacceptable. In a recent study examining 164 healthy professional athletes, the Standardized Assessment of Concussion component of the SCAT3, which ostensibly measures orientation, immediate memory, concentration, and delayed recall, obtained an overall reliability score of .34, with some subcomponents yielding values as low as .03.8
In the same study, the motor control, balance, and gait tests of the SCAT3 were found to all exhibit reliability scores of less than .25. To understand the cost associated with having suboptimal reliability, consider that the SCAT3 is only sensitive enough to reliably detect concussion at 24 hours, but not after 8 and 15 days9 (similar limitations have been documented for ImPACT5). Thus, sensitivity is limited to 24-hours postinjury, when symptoms are most pronounced, and much less so when symptoms are subtle. This questions SCAT’s usefulness in cases of mild head injuries, which can be less pronounced symptomatically, but are nonetheless important to diagnose for reasons discussed already, as well as in the case of any return to play decisions made more than a few days after injury. Indeed, concussion symptoms and risk of re-injury are known to last weeks, and in some cases, months after the initial trauma, during which time the SCAT is ineffective in reliably assessing symptoms.
To the credit of their developers, ImPACT and SCAT were innovative in their inclusion of multiple domain testing. Unfortunately, this also compounds problems associated with assessment reliability. When reliability is low, increasing the number of domains tested actually increases the chance of a misdiagnosis. The reason for this is that by including more indices in the battery with low reliability causes over-representation of poor quality (ie, inaccurate or irrelevant) tests and under-representation of good quality measures. Consider the data shown in Figure 1, which illustrates how low reliability results in increasing levels of misclassification with each additional test. As an example, when tests have reliability values of .2, then the use of just five tests will result in a false positive rate of approximately 40%. However, when reliability is high (eg, 0.9), then even the use of 10 tests results in false positive misclassifications of less than 20%.
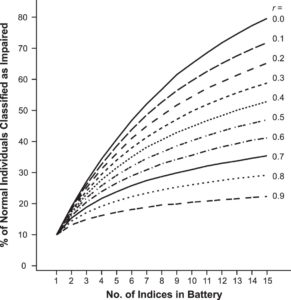
Figure 1. As reliability (r) decreases, including more indices increases the chance of a false positive diagnosis.10
Because research shows that some of the most commonly used tests are not sufficient for accurate concussion diagnoses, medical professionals should consider other more reliable and validated tests—and, ideally, tests that can also be used as reimbursable events in urgent care settings.
Best Practices
Precise measurements of executive abilities such as attention, distractibility, and mental stamina are critical to detecting signs of neurocognitive consequences of concussion. Some of the more useful types of tests are those that are sensitive to subtle cognitive symptoms, such as sustained attention and concentration. For example, trail-making tasks can be used to assess attention and task-switching ability; the Wisconsin Card Sorting Test can examine impulsivity and feedback processing; and the Psychomotor Vigilance Task can measure sustained attention, alertness, and psychomotor skills.
Computerized continuous performance tests can be especially useful in that they not only assess similar cognitive domains, but they can do so in an automated manner to minimize the reliance on the test administration experience of the doctor. Such well-validated tools provide information regarding abilities and functions that are known to be impaired by mTBI. Importantly, research indicates that tests measuring these types of functions are extremely reliable, sensitive to the presence of a concussion, capture remediation curves in adolescents with TBI, and are associated with improved scores as a function of time following mild head trauma.12 Thus, these tests can more reliably and accurately assess the cognitive aspects of concussion as part of a well-constructed assessment battery.
Although all concussed athletes face their own brain and body disruptions, concussions often impair visual-vestibular feedback and sensory-motor control (ie, neuromotor functioning). Neuromotor functioning that supports postural control can be assessed in the form of a balance test or a simple gait analysis. As an illustration, gait functioning is not only an important behavioral consequence of a concussion, but also sensitive for informing return-to-play decisions.
For example, the NIH 4-meter gait test consistently yields some of the highest reliability coefficients of any test, with values of .97.13 Individuals with concussions have shorter stride length and slower gait velocity relative to normal controls, and gait effects have been shown to be remarkably reliable and durable over time.14 The 4-meter gait test has proven to be remarkably reliable, and while it only measures one domain, gait speed is readily and demonstrably indicative of the impairment associated with concussion and mTBI. As a result, when paired with other reliable neurocognitive measures, the 4-meter gait test could prove to be an invaluable part of an updated, more accurate concussion protocol.
Conclusion
Concussions are among the most dangerous and functionally impactful types of traumatic injuries, and they are occurring with increased frequency. Concussions without major symptoms (mTBIs) often go undetected and will compound with reinjury. Importantly, urgent care facilities are uniquely positioned to contribute to the more effective management of concussions because they are accessible (long hours of operation), they have medical professionals who are in a better position to make such decisions (as opposed to parents or coaches), and they have access to professional-grade instruments (eg, neuropsychological tests) that can support decision making.
Indeed, this approach can reflect a favorable step forward for all parties involved, as the patients get a higher level of care and the doctors can be reimbursed (eg, billing code 96118 for neuropsychological testing by an MD) for conducting best practices.
Importantly, these best practices would serve to increase the likelihood that those experiencing subtle mTBI symptoms are identified, medically followed, and referred out to specialists when indicated. Indeed, doctors in urgent care setting can establish a referral network of neurologists and neuropsychologists that can be used when more extensive testing is indicated and/or when neurocognitive rehabilitation is needed. This can occur when a patient is shown to score in the problematic range on some of the neurobehavioral and/or neuromotor tests administered in the urgent care setting or when symptoms persist, suggesting the need for more proactive interventions.
Although some exemplars are herein reviewed, the most important implication of these guidelines is the value of considering the reliability of any selected assessment tool, especially when using multiple assessment tools. Moreover, by understanding the importance of multiple domain testing and selecting tests that are reliable within each domain, better assessment batteries can be selected to support diagnostic and return-to-play decisions. With this understanding of constructs such as reliability and validity, more accurate decisions can be made in the diagnosis and treatment of concussions, thereby creating a safer environment for those experiencing such injuries.
Citation: Lecci L, Hollander J, Key D, Keith J. Concussion management in the urgent care: a primer for implementation. J Urgent Care Med. June 2018. Available at: https://www.jucm.com/concussion-management-in-urgent-care-a-primer-for-implementation/.
References
- Youth Sports Safety Alliance. Preventing sudden death in youth sports. Available at: http://www.swata.org/statistics/. Accessed March 8, 2017.
- Broglio SP, Ferrara MS, Macciocchi SN, et al. Test-retest reliability of computerized concussion assessment programs.J Athl Train. 2007;42(4):509-514.
- Schatz P, Putz BO. Cross-validation of measures used for computer-based assessment of concussion. Appl Neuropsychol. 2006;13(3):151-159.
- McKay CD, Brooks, BL, Meeuwisse WH, et al. The effect of age, sex, and concussion history on preseason ImPACT values of elite Canadian youth ice hockey players. Br J Sports Med. 2013;47(e1).
- Nelson LD, LaRoche AA, Pfaller AY, et al. Prospective, head-to-head study of three computerized neurocognitive assessment tools (CNTs): reliability and validity for the assessment of sport-related concussion. J Int Neuropsychol Soc. 2016;22(1): 24-37.
- Futterman MA. 17-year-old’s death points to flaws in concussion test. Wall St J. April 18, 2017.
- Mayers LB, Redick TS. Clinical utility of ImPACT assessment for postconcussion return-to-play counseling: psychometric issues. J Clin Exp Neuropsychol. 2012;34(3):235-242.
- Hänninen T, Tuominen M, Parkkari J, et al. Sport concussion assessment tool–3rd edition–normative reference values for professional ice hockey players.J Sci Med Sport. 2016;19(8):636-641.
- Chin EY, Nelson LD, Barr WB, et al. Reliability and validity of the Sport Concussion Assessment Tool–3 (SCAT3) in high school and collegiate athletes.Am J Sports Med. 2016;44(9):2276-2285.
- Nelson LD. False-positive rates of reliable change indices for concussion test batteries: a Monte Carlo simulation. J Athl Train. 2015;50(12):1319-1322.
- Riccio CA, Reynolds CR, Lowe P, Moore JJ. The continuous performance test: a window on the neural substrates for attention?Arch Clin Neuropsychol. 2002;17(3):235-272.
- Naunheim RS, Matero D, Fucetola R. Assessment of patients with mild concussion in the emergency department. J Head Trauma Rehabil. 2008;23(2):116–122.
- Peters DM, Fritz SL, Krotish DE. Assessing the reliability and validity of a shorter walk test compared with the 10-meter walk test for measurements of gait speed in healthy, older adults. J Geriatr Phys Ther. 2013;36(1):24-30.
- Parker TM, Osternig LR, van Donkelaar P, Chou LS. Gait stability after a concussion. Med Sci Sports Exerc. 2006;38(6):1031-1040.
- Becker LA. Statistical and clinical significance ─ effect size calculators. Available at: http://www.uccs.edu/lbecker/clinsig.html. Accessed May 16, 2018.
Len Lecci, PhD, MA is Professor of Psychology at the University of North Carolina Wilmington and Director of Clinical Services for MARS Memory-Health Network. Julian Keith, PhD, MS is Professor of Psychology and Department Chairperson at University of North Carolina Wilmington. John Hollander, MA, is a Research Assistant at University of North Carolina Wilmington.

Len Lecci, PhD, MA

John Hollander, MA

