Published on
Urgent message: From pregnancy confirmation to the evaluation of bleeding, urgent care centers are often the initial location for management of obstetric-related issues. Careful use of evidence-based guidelines is the key to successful outcomes.
DAVID N. JACKSON, MD, FACOG and PETAR PLANINIC, MD, FACOG
Case Presentation
Urgent care providers are called upon to manage a variety of complaints in pregnancy. Some conditions can be managed at the urgent care center whereas others require stabilization and transport to a center with expert obstetrical capabilities. In all situations, practitioners should consider that a gestational age of fetal viability (many centers now use 23 to 24 weeks) is best served with referral for continuous fetal monitoring if there is bleeding, trauma, significant hypertension, relative hypoxemia (O2 saturation less than 95% for pregnant women), or contractions.
Part 2 of this two part series will discuss:
- Bleeding in pregnancy
- Ectopic gestation
- Trauma and pregnancy
- Acute abdominal pain in pregnancy
- Chronic illness and common medications (anxiety and depression, asthma, cold symptoms, epilepsy, influenza, preeclampsia and eclampsia, thyroid disease)
- Bleeding
Bleeding in Pregnancy
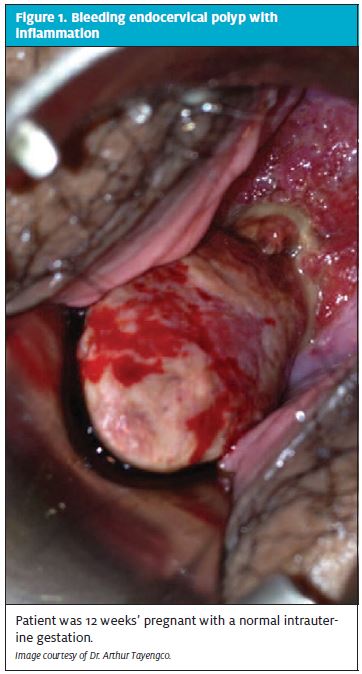
Bleeding in the first trimester is frequent, occurring in 20% to 40% of all pregnancies. Differential diagnosis includes implantation bleeding, threatened to complete abortion, ectopic pregnancy, molar pregnancy, and non- pregnancy sources such as uterine, cervical or vaginal lesions (including inflammation or polyps)
(Figure 1).
Evaluation of vaginal bleeding should follow a systematic process. History of last menses and sexual activity determines the possibility of pregnancy. Be prepared for potential denial answers regarding pregnancy, ranging from “We’ve been ‘careful’,” to “My boyfriend told me he was sterile.” A simple rule would be that every reproductive-age woman with new-onset abnormal vaginal bleeding should be offered evaluation for pregnancy. History should especially include the duration and quality of last menses. If menses are regular, ovulation is predicted on day 14 from the first day of the last menstrual period (LMP). Contraception use should be documented, as well as the quantity and quality of current bleeding (including clots or passage of tissue). The passage of tissue suggests incomplete to complete abortion.
Bleeding that occurs “early” in the cycle, (approximately 18-26 days from the LMP), suggests the possibility of implantation bleeding. It is one of the earliest signs of an intrauterine pregnancy. Implantation bleeding occurs 6 to 12 days post-conception and typically presents as spotting, occasionally with cramping.
The pain that occurs with bleeding gives a clinical suggestion as to pregnancy location. Crampy midline or uterine pain suggests intrauterine gestation with threatened abortion. Discrete lateral pain suggests ectopic gestation, ovarian torsion, or degenerating leiomyomata. Shoulder pain suggests intraabdominal bleeding.
Laboratory evaluation for first-trimester bleeding.
Initial lab assessment includes complete blood count (CBC), Type & screen and human chorionic gonadotropin (hCG). Preferentially ordering a quantitative hCG is helpful to begin serial evaluation to determine if a gestation is viable. Rh (D) immune globulin should be given to all Rh-negative pregnant patients who are bleeding, regardless of the etiology or gestational age.1,2 Rh (D) immunoprophylaxis is currently recommended for women with miscarriage, induced abortion, ectopic pregnancy, and other first-trimester bleeding. Referral by an urgent care provider to obstetrics for treatment with Rh immune globulin based on ACOG guidelines is recommended.3
Physical examination for bleeding in pregnancy.
The maternal physical exam begins with vital signs, looking for tachycardia. Orthostatic changes suggest the need for urgent management of hypovolemia. The maternal abdominal exam should document the presence or absence of peritoneal signs, abdominal distention, rectus rigidity and/or rebound. The fundus of the uterus should be palpable above the symphysis if greater than
12 weeks since the last menses. A fetal heartbeat usually cannot be detected until at least 10 weeks of pregnancy by a handheld Doppler. If the patient is overweight, it may be 12 weeks or more before the heartbeat is rea ily picked up by handheld Doppler.
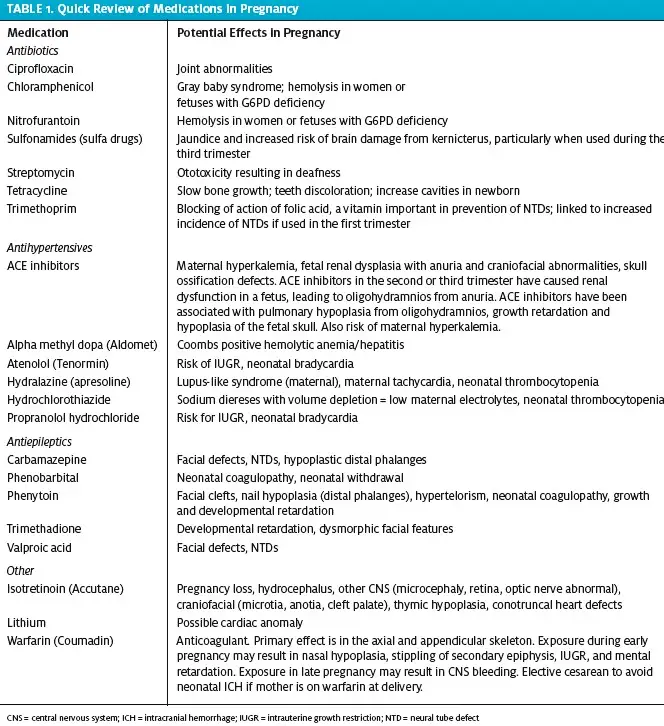
The external vaginal exam notes the amount of bleeding on the labia and perineum. A speculum exam is mandatory to visualize the entire cervix and vagina. Examples of nonpregnancy bleeding include cervical eversion with friability, cervical infection with inflammation, vaginal and cervical lesions and bleeding tumors such as the bleeding “polyp” seen in Figure 1. Visualize the external os to determine any dilatation and to confirm that the bleeding is originating from within the os. Also determine whether trophoblastic tissue is present (Figure 2).
Perform a bimanual exam and gently palpate the uterus and adnexa for size and pain or masses. If an intrauterine pregnancy is confirmed, the following def- initions of bleeding in early pregnancy are based upon physical findings:
Threatened abortion: Cramping and bleeding without passage of tissue. The cervical os is closed.
Inevitable abortion: Cramping and bleeding. The cervical os is open but there is no passage of tissue.
Incomplete abortion: Cramping and bleeding with partial passage of tissue. The cervical os may be open or closed.
Complete abortion: Bleeding and complete passage of tissue. The cervical os is typically closed.
Spontaneous abortion is often associated with advanced maternal age and/or a history of previous miscarriage. Most spontaneous first-trimester losses are associated with fetal or chromosomal abnormalities.
Examination of clot or tissues. One way to determine if a clot contains placental tissue is to suspend the clot in water to look for floating villi. The presence of villi lowers the likelihood of concurrent ectopic pregnancy but it does not prove whether the findings represent a complete or an incomplete spontaneous abortion. Caution: A “decidual cast” may look like rubbery tissue that has passed. It actually represents decidualized endometrium and correlates with an ectopic pregnancy.
Ultrasound evaluation for early pregnancy bleeding. Transvaginal or transabdominal ultrasound should be considered a standard, not optional, recommendation for emergency and urgent care centers evaluating early pregnancy bleeding.4 This is especially true when quantitative hCG levels are at least 1500-2000 IU/L. At this “discriminatory level,” an intrauterine gestational sac should be visualized. If an intrauterine gestational sac is not seen, work up for ectopic pregnancy must continue. For viable pregnancies, if the gestational sac is 20 mm, a yolk sac should be visualized. If the yolk sac is 5 mm, an embryonic pole should be visualized. If the embryonic pole is 5 mm or greater, an embryonic heart beat should be visualized.
Guidance for centers that currently have to send out [3-hCG or that don’t have ultrasound machines on-site is problematic. For these centers, it is prudent to suggest immediate transfer for evaluation with ultrasound if the on-site qualitative pregnancy test is positive and the physical exam suggests ectopic gestation.
Ectopic Pregnancy
Implantation of a developing blastocyst at a site other than the endometrium of the uterine cavity is the most important differential diagnosis an urgent care provider considers in the evaluation of early pregnancy bleeding. Intraabdominal bleeding from ectopic pregnancy remains a cause of pregnancy-related maternal death in the first trimester. Ectopic gestation occurs in 2% of all pregnancies. The patient should be asked about risk factors including prior tubal surgery, prior ectopic pregnancy, previous salpingitis or pelvic infection, assisted reproduction, infertility history, smoking, and regular vaginal douching.
The most common extrauterine location is the fallopian tube, which accounts for 98% of all ectopic gestations. Symptoms of bleeding, pain or both typically occur 6 to 8 weeks after the LMP. Patients classically present with vague or localized pelvic pain, delayed menses, and vaginal spotting/bleeding. However, up to 50% of patients may be asymptomatic until tubal rupture occurs. In fact, 10% of patients with ectopic pregnancy have no pain, 21% have no vaginal bleeding, 29% have no tenderness, and 36% have no palpable adnexal mass. Therefore, the modern diagnosis of ectopic pregnancy requires a combination of quantitative assay for hCG and use of high-resolution transvaginal ultrasonography (TVUS). If a true intrauterine sac is identified, the patient should be managed the same as for a threatened abortion and referred for repeat quantitative hCG in 48 to 72 hours. If no intrauterine sac is seen, an ectopic pregnancy should be suspected, especially if hCG is greater than 1500 to 2000 IU/L. This management requires coordination between imaging and lab analysis. Both must be timely and have opportunity to follow up.
Counseling on First-Trimester Bleeding and Miscarriage
The outcome of ongoing pregnancies with first- trimester threatened abortion is reassuring. Saraswat and colleagues confirmed there is no increase in chromosomal or congenital defects when pregnancies survive early bleeding.5 However, patients with first- trimester bleeding and ongoing pregnancies are more likely to experience preterm premature rupture of membranes (OR 1.78), preterm delivery (OR 2.05), and intrauterine growth restriction (OR 1.54). To date, there are no prospective interventions that reduce these complications.
What is the cause of the bleeding? When miscarriage occurs, patients want to know the etiology. As much as feasible, patients should be reassured that personal issues such as stress, not eating correctly, poor sleep, anxiety, and intercourse do not cause miscarriage. For isolated first trimester loss in which the fetus does not form (anembryonic pregnancy) or does not continue development, chromosomal syndromes are the most likely cause of the loss. If possible, sending products of conception for chromosomal analysis is helpful in future counseling. It is prudent to recommend follow-up counseling with an obstetrical specialist to provide post loss consultation.
Second- and Third-Trimester Issues: Maternal
Positioning
Vena caval obstruction by the uterus decreases preload and can initiate maternal hypotension. Uterine blood flow is not auto-regulated, therefore, a decrease in maternal systolic blood pressure can cause a significant fall in uterine blood flow. A pregnant patient on her back may have sweating, dizziness and hypotension that resolve when she is turned on her side. Prevention begins with positioning all pregnant patients on a rolled-up towel or wedge under the right hip at least 15 degrees. This “left tilt” decreases vena caval obstruction.
Trauma and Pregnancy Outcome
Trauma complicates 6% to 7% of all pregnancies. Pregnant patients who suffer major trauma will likely bypass an urgent care center, but those with minor trauma may be seen. Data on management of minor trauma in pregnancy are limited and conflicting.6 Reports indicate that fetal demise or premature births are increased after even minor trauma to a pregnant patient.7 Monitoring of a viable pregnancy after trauma is typically recommended for 4 to 6 hours. Lab assessment requires CBC, blood type with Rh status, and possibly the Kleihauer- Betke test to determine fetal to maternal bleeding. Any post-trauma patient with symptoms of bleeding, uterine tenderness, contractions, or pain should be referred to a center with obstetrical delivery capabilities for pro- longed monitoring and evaluation of possible placental separation (abruption).8 Patients complaining of unusual falls or seen recurrently for pain should also be screened for abuse and domestic violence.9
Abdominal Pain in Pregnancy
Pain in pregnancy should be categorized as acute or chronic, with or without bleeding, and with or without associated renal or gastrointestinal symptoms. The typical differential includes appendicitis, cholecystitis, fibroid degeneration, adnexal cysts with or without torsion, spontaneous abortion, ectopic pregnancy, amnionitis, and placental abruption. Although rare, ovarian vein thrombosis needs to be considered for acute right-sided pain, especially in postpartum patients. Acute appendicitis is the most common surgical com-lication of pregnancy. It is often suggested by symptoms that initially are confused with pyelonephritis. Shielding of the inflamed appendix by an enlarged uterus may lead to delayed diagnosis, and appendiceal rupture at the time of surgery is more common during pregnancy.
The primary clinical symptoms of appendicitis in pregnancy include decreased appetite, nausea with vomiting, and fever. The focal abdominal pain location will depend on gestational age, and typically rises with the enlarging uterus. Classic signs such as rebound tenderness and leukocytosis may be delayed or absent. Referral for potential surgery is required as soon as a clinical suspicion of appendicitis is developed.
Acute cholecystitis is the second most common surgical complication of pregnancy. Pain is typically upper- right-sided or epigastric. Cholelithiasis is present in 90% of pregnant patients with acute cholecystitis. Elevated white blood cell count, elevated serum amylase, and hyperbilirubinemia are typical. Diagnosis requires ultrasound confirmation. The pregnancy related differential includes severe preeclampsia, acute fatty liver, and placental abruption. The non-pregnancy differential includes pancreatitis, acute appendicitis, and right- lower-lobe pneumonia. Referral for inpatient observation, conservative intravenous therapy, and potential surgery is required.
Adnexal torsion is typically acute and localized to one side of the abdomen. On ultrasound, an adnexal mass without adequate blood flow to the ovaries can be visu- alized. Complications include peritonitis and preterm labor. Surgical management is indicated for patients with signs of acute abdomen.
Degenerating leiomyomata in pregnancy presents as focal, severe, point tenderness. Contractions may be an initial symptom. Imaging is required to confirm the presence of the leiomyomata at the site of a patient’s pain.
Common Medications in Pregnancy
Urgent care centers may make the initial diagnosis of pregnancy. Because urgent care practitioners may be asked by pregnant patients for advice regarding contin- uing chronic medications, they should be aware of which medications are safe in early gestation. An alpha- betized list based on diagnosis is included below and Table 1 provides a summary on common medications in pregnancy.
Anxiety and depression. Initial treatment of anxiety and depression in pregnancy should include expert assessment, psychotherapy, or a combination of psychotherapy and lowest-effective-dose pharmacotherapy. The best medications for anxiety and depression in pregnancy are now controversial, as recent data suggest an increased risk of fetal problems with selective serotonin reuptake inhibitors (SSRIs), tricyclic antidepressants (TCAs), and monoamine oxidase inhibitors (MAOIs).
Antidepressants are generally category C drugs; bupropion is category B. Paroxetine exposure during the first trimester has been associated with an increased risk of birth defects.10 Patients who use SSRIs after the 20th week of pregnancy are 6 times more likely to have persistent pulmonary hypertension.11
In general, tricyclic antidepressants have increased risk over SSRIs, MAOIs should not be used during pregnancy, and benzodiazepines should be avoided in the first trimester.
Warning: Women on antidepressant treatment are 5 times more likely to relapse into major depression during pregnancy if their antidepressant medications are stopped.12 Referral for cognitive-behavioral and interpersonal supportive therapies that involve the family is critical if a patient’s medications are discontinued in pregnancy.
All antidepressants have been shown to be present in breast milk, but sertraline, paroxetine, and nortrypty line are preferred antidepressant treatments in breast- feeding mothers because they result in the lowest drug levels in infants.
Asthma.
Along with influenza and bronchitis, asthma is a common urgent care issue.13 Evaluation and treat-ment in pregnant patients does not differ significantly from that in non-pregnant patients. Typical regimens are short-acting inhaled beta2-agonists, such as albuterol for rescue therapy, and inhaled steroids for maintenance therapy. Although use of fluticasone use is common in women with asthma who are not pregnant, budesonide and beclomethasone are considered the inhaled steroids of choice during pregnancy according to guidelines from the American Congress of Obstetricians and Gynecologists (ACOG). They are the two medicines that have been most studied during pregnancy.14
Urgent care providers managing upper respiratory infections or complicated asthma in pregnancy may be overly concerned about fetal risks associated with chest x-rays. ACOG Guidelines place a limit for maximum elective cumulative fetal dose at 5 rad (1 rad = 1000 mrad =10 mGy = 0.01Gy). A two-view shielded chest x- ray delivers only 0.00007 rad. Therefore, a pregnant patient would have to undergo 71,429 exams to reach the cumulative 5-rad dose limit.
Chronic hypertension.
Antihypertensive monotherapy is typically begun when a patient’s systolic blood pres- sure (BP) is greater than 160 mm Hg and/or diastolic BP is greater than 105 mm Hg. If there is risk of maternal end organ damage, we prefer an upper limit of 140/100 to begin therapy. Referral to obstetrics for treatment is appropriate.
“Cold” symptoms.
Symptomatic relief of rhinitis, sneezing, cough, and throat pain can be attempted with acetaminophen, pseudoephedrine, nasal spray, and chlorpheniramine. Because of the theoretical risks, recommendations are to avoid oral decongestants in the first trimester unless benefits are balanced by theoretical risks of rare birth defects. 15,16 Any pregnant patient who has an upper respiratory infection that lasts more than 7 days should be evaluated for bacterial infection or influenza.
Dental care.
Cavities or infection in pregnant patients must be treated. Cephalosporin and penicillin-based antibiotics are safe to use during pregnancy. Local anesthetics and short-term use of opioid analgesics are also appropriate. Pregnant patients should not be prescribed prolonged antiprostaglandin medications for pain or inflammation because of the fetal renal effects and risk of ductus arteriosus constriction.
Epilepsy or status epilepticus.
Many patients have increased seizure frequency in pregnancy because of stopping medications or taking medications at sub- therapeutic dosages. Concerns are typically over medication-induced fetal embryopathy. The highest risk is with valproic acid (especially if >1100 mg/day) and poly-drug therapy. Lamotrigine may have the safest fetal profile.17 Recurrent seizures in a pregnant patient that result in hypoxia may have a greater negative impact than the potential teratogenic effects of antiepileptic drugs. Therefore, monotherapy at the low- est dose needed to control seizures is recommended.
Status epilepticus is treated with diazepam at 1 mg/min, or up to 250 mg of sodium amobarbital, slowly administered IV. Phenytoin and phenobarbital also can be safely used to prevent recurrent noneclamptic seizures in a pregnant patient. However, IV magnesium sulfate should be immediately used to prevent recurrent seizures associated with eclampsia.
Influenza Vaccine and Treatment
Along with asthma, influenza is one of the most common respiratory conditions complicating pregnancy.18 Influenza is more severe in pregnant women than in other populations. Annual vaccination is recommended for all women who will be pregnant during influenza season (October to May).19 Pregnant women with influenza are more likely to develop severe illness and to die than the general population. Pregnant women are also more likely to be hospitalized for respiratory illnesses than nonpregnant women, especially during influenza season. 20,21 The diagnosis of influenza is made clinically and confirmed with results from rapid influenza diagnostic tests or reverse transcriptase polymerase chain reaction testing.
Typical symptoms of influenza include fever, cough, rhinorrhea, sore throat, headache, shortness of breath and myalgia. Some patients will have vomiting, diarrhea, conjunctivitis, and some have respiratory symptoms without fever.
Pregnant women with suspected influenza require immediate empiric treatment with antiviral medications, even if treatment is initiated more than 2 days after symptom onset.22 The recent influenza virus out- breaks have been responsive to neuraminidase inhibitors such as oseltamiir and zanamivir. These are Category C drugs in pregnancy. Dosing is oseltamivir 75 mg twice faily for 5 days or zanamivir 10 mg (2 inhala- tions) for 5 days. For treatment of pregnant women or women up to 2 weeks postpartum with suspected or confirmed influenza, oseltamivir is currently preferred (see CDC recommendations for frequent updates).
Because prevention is better than treatment, all women who are pregnant or will be pregnant during influenza season should be encouraged to receive the inactivated influenza vaccine, regardless of pregnancy trimester.
Pain Management
Minor pain in pregnant patients can be treated with mas- sage, heat and ice, and acetaminophen. Do not prescribe antiprostaglandin medications as primary agents for pain because of the possible risks of fetal renal impairment or adverse effects on the ductus arteriosus. Pregnant women may get relief from back pain by placing one foot on a stool when standing and placing a pillow between their legs when lying down. Supportive shoes and a pregnancy-based exercise program can be recommended to improve strength and flexibility.
Short-term opioid use can be beneficial for acute relief. Chronic opioid use creates risk for habituation. Referral for physical therapy assessment and chronic pain management services are essential adjuncts for the opioid dependent pain patient who subsequently becomes pregnant.
Preeclampsia and Eclampsia
We have admitted many patients directly from an urgent care center to our obstetrical unit after they have been seen for severe headache in pregnancy. The cerebral and visual disturbances that are typical for preeclampsia may be misdiagnosed as migraine with aura or non-pregnancy CNS pathology. Preeclampsia is new onset of elevated blood pressure and proteinuria (greater than 300 mg in 24 hours or 1+ (30 mg/dL) on at least two random urine dipstick tests after 20 weeks’ gestation.
Patients with preeclampsia and impending eclampsia may have severe headache with visual disturbances, epigastric pain, nausea, and emesis. Delay in diagnosis potentially leads to seizures, abruptio placentae, pul-monary edema, aspiration pneumonitis, cardiac failure, intracranial hemorrhage, and transient blindness. Therefore, any pregnant patient over 20 weeks’ gestation with hypertension or severe headache should be considered at risk of eclampsia until proven otherwise. Warning: Urgent care providers may also see preeclampsia in patients up to 4 weeks postpartum. Basic screening postpartum also includes analysis of symptoms suggestive of organ-specific vasoconstriction (headache, scotomata, elevated LFT, platelets <100,000, elevated uric acid, and proteinuria >1+ on dipstick or >300 mg in 24 hours).
It is critical to initiate therapy with magnesium sul- fate at a 4- to 6-g loading dose over 15 to 20 minutes and 2 g per hour IV maintenance. The ambulance services typically carry these medications.
Thyroid
Women who are on thyroid hormone replacement may require an increase in their dosage by 30% to 50% during pregnancy. Serum concentrations of free T4 and thyroid stimulating hormone are typically used for monitoring thyroid dosing in pregnancy. Ordering a free T4 is necessary because the increase in thyroid-binding globulin associated with pregnancy falsely elevates total T4. TSH is typically unaffected by pregnancy after 16 weeks.
Teratogenic Risks of Common Medications
The fetus is most vulnerable between the 3rd and 8th week after fertilization (5th to 10th week after LMP). Teratogenic drugs taken before the 20th day following conception (5th LMP week) typically have an “all-or- nothing” effect, inducing miscarriage or having no effect at all. Table 1 provides a quick review of medication effects in pregnancy. ■
References
- Griffey RT, Chen BC, Krehbiel Performance in appropriate Rh testing and treat- ment with Rh immunoglobulin in the emergency department. Ann Emerg Med. 2012;59(4):285-293.
- Hannafin B, Lovecchio F, Blackburn Do Rh-negative women with first trimester spon- taneous abortions need Rh immune globulin? Am J Emerg Med. 2006;24(4):487-489.
- American College of Obstetricians and Preventionof Rh D alloimmunization. ACOG Practice Bulletin No. 4. Washington, DC: ACOG; 1999. Reaffirmed 2010.
- Adhikari S, Blaivas M, Lyon Diagnosis and management of ectopic pregnancy using bedside transvaginal ultrasonography in the ED: a 2-year experience. Am J Emerg Med. 2007;25(6):591-596.
- Saraswat L, Bhattacharya S, Maheshwari A, Bhattacharya Maternal and perinatal outcome in women with threatened miscarriage in the first trimester: a systematic review. BJOG. 2010;117(3):245-257
- Cahill AG, Bastek JA, Stamilio DM, et Minor trauma in pregnancy—is the evalua- tion unwarranted? Am J Obstet Gynecol. 2008;198:208.e1-208.e5
- Fischer PE, Zarzaur BL, Fabian TC, Magnotti LJ, Croce Minor trauma is an unrec- ognized contributor to poor fetal outcomes: a population-based study of 78,552 preg- nancies. J Trauma. 2011;71(1):90-93.
- Brown Trauma in pregnancy. Obstet Gynecol. 2009;114(1):147-160.
- Thurston WE, Tutty LM, Eisener AC, Lalonde L, Belenky C, Osborne Implementa- tion of universal screening for domestic violence in an urgent care community health center. Health Promot Pract. 2009;10(4):517-526.
- Kalra S, Born L, Sarkar M, et The safety of antidepressant use in pregnancy. Expert Opinion on Drug Safety. 2005;4:273-283.
- Chambers CD, Hernandez-Diaz S, van Marter LJ, et Selective serotonin-reuptake inhibitors and risk of persistant pulmonary hypertension of the newborn. N Engl J Med. 2006;354:579-587.
- Cohen LS, Altshuler LL, Harlow BL, et al. Relapse of major depression during in women who maintain or discontinue antidepressant JAMA. 2006;295:499- 507.
- Law HZ, Oraka E, Mannino The role of income in reducing racial and ethnic disparities in emergency room and urgent care center visits for asthma-United States, 2001- 2009. J Asthma. 2011;48(4):405-413.
- American College of Obstetricians and Asthma in Pregnancy. ACOG Practice Bulletin No. 90, Washington DC; 2008
- American College of Obstetricians and Gynecologists (ACOG) and The American Col- lege of Allergy, Asthma and Immunology (ACAAI). The use of newer asthma and allergy medications during Position Statement. Ann Allergy Asthma Immunol. 2000;84:475-480.
- Yau WP, Mitchell AA, Lin KJ, Werier MM, Hernandez-Diaz Use of decongestants during pregnancy and the risk of birth defects. Am J Epidemiol. 2013;178(2):198-208.
- Pennell Using current evidence in selecting antiepileptic drugs for use during pregnancy. Epilepsy Curr. 2005;5:45-51.
- Orzechowski KM, Miller Common respiratory issues in ambulatory obstetrics. Clin Obstet Gynecol. 2012;55(3):798-809.
- Fortner KB, Kuller JA, Rhee EJ, Edwards Influenza and tetanus, diphtheria, and acellular pertussis vaccinations during pregnancy. Obstet Gynecol Surv. 2012;67(4):251- 257.
- Neuzil KM, Reed GW, Mitchel EF, Simonsen L, Griffin Impact of influenza on acute cardiopulmonary hospitalizations in pregnant women. Am J Epidemiol. 1998;148:1094-1102.
- Dodds L, McNeil SA, Fell DB, et Impact of influenza exposure on rates of hospi- tal admissions and physician visits because of respiratory illness among pregnant women. CMAJ. 2007;176:463-468.
- Creanga AA, Johnson TF, Graitcer SB, et Severity of 2009 pandemic influenza A (H1N1) virus infection in pregnant women. Obstet Gynecol. 2010;115:717.