Published on
Urgent message: Impetigo is one of the most common skin infections in children, and can have a variable presentation. As such, it is essential that the urgent care provider be able to recognize this common skin infection, and to know the treatment options.
Aimy T. Patel, MD, FAAP, Allison Burris, MD FAAP, and Nirav Shastri, MD, FAAP, FAMIA, ABMS-CI
CASE PRESENTATION
History
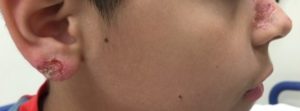
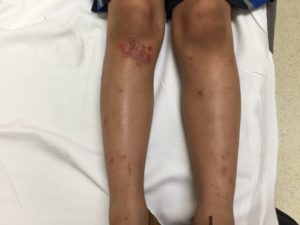
A 9-year-old otherwise healthy boy presents with a 1-week history of an itchy rash on his knee. The rash blistered and burst open, producing clear to yellowish drainage. The rash then spread to his legs, arms, earlobe, and nose with similar appearance and itching. He has no fever or mucous membrane lesions. He has not taken any medications. There are no ill contacts, and he does not have a prior history of similar rashes.
Physical Examination
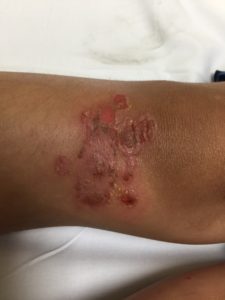
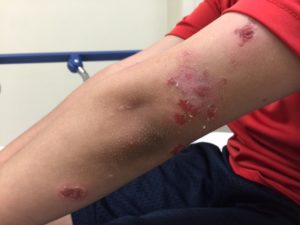
The patient has a very pruritic rash over his bilateral knees, legs, nose, arms, and earlobe (Figures 1 and 2). The rash is erythematous and pruritic with sharply demarcated edges. There is evidence of ruptured bullae showing an underlying erythematous base with yellow dried crust along the edges.
Differential Diagnosis4
- Herpes simplex virus-1 infection
- Bullous impetigo
- Linear IgA dermatosis
- Toxicodendron dermatitis
Herpes simplex virus-1 (HSV-1) lesions usually present as painful vesicular lesions on an erythematous base and can be accompanied by fever with malaise. HSV-1 typically affects the mouth, though it can cause infection at other sites like the genitalia, liver, lung, eye, and central nervous system. It can also be a complication of eczema. Skin lesions associated with HSV-1 tend to be clustered in a single anatomic site, though autoinoculation to distant sites can also occur. Primary lesions tend to last 10-14 days and can occur up to 26 days after inoculation.1
While our patient did have lesions around the nose and earlobe, his rash was not consistent with a primary HSV-1 outbreak because of presentation on various anatomic sites and a lack of pain and systemic symptoms.
Linear immunoglobulin A (IgA) dermatosis is an autoimmune blistering disease that is characterized by the linear deposition of IgA in the basement membrane on direct immunofluorescence. This bullous disease can occur in both adults and children. In children, the bullae are tense rather than flaccid, and can be intensely pruritic.2 New blisters typically arise in a ring surrounding an older lesion, creating a “cluster of jewels” appearance. It is often misdiagnosed initially as bullous impetigo and can improve on antibiotics, though the diagnosis is questioned when the eruption recurs. To differentiate bullous impetigo from this condition in our patient, the bullae were flaccid and not tense. His lesions also cleared with treatment and have not recurred.
Toxicodendron dermatitis (rhus dermatitis) is a result of a type IV hypersensitivity reaction to urushiol, found in sap, roots, and leaves of poison ivy, oak, and sumac. It presents typically as linear erythema with pruritis, leading to papules, vesicles, and bullae with clear or yellow fluid. History will include plant exposure 4 to 96 hours prior to the onset of the rash. If left untreated, the rash can last 1–3 weeks.3 Our patient’s condition is differentiated from toxicodendron dermatitis due to lack of recent poison ivy, poison oak, or poison sumac exposure, lack of linear distribution, and absence of typical papules and vesicles.
DISCUSSION
Impetigo is the most common skin infection. It typically affects children between the ages of 2 and 5 years. The two presentations that can occur are nonbullous and bullous impetigo.
Bullous impetigo accounts for 30% of impetigo cases and is exclusively caused by
Staphylococcus aureus, including methicillin-resistant S aureus (MRSA).4 Impetigo can be further classified as primary (direct bacterial invasion of previously normal skin), or secondary (at sites of minor skin trauma). Minor skin trauma can include abrasions, minor cuts, insect bites, or an underlying skin condition such as eczema.
Nonbullous impetigo is the most common type of impetigo and comprises 70% of the cases. Nonbullous impetigo is primarily caused by S aureus and secondarily group A streptococcus. Nonbullous impetigo presents as papules that progress to vesicles surrounded by erythema. The rash subsequently progresses to pustules that enlarge and rupture to form the classic “honey-colored crusts” that have become pathognomonic for impetigo. Lesions typically occur on the face and extremities. Regional lymphadenitis can occur, but systemic symptoms are unlikely. The rash tends to be localized to one area, but multiple surrounding lesions may occur due to autoinoculation.4
Bullous impetigo lesions are characterized by large, flaccid, fluid-filled bullae that can rupture and ooze yellow, honey-colored fluid. After the bullae rupture, there is a pathognomonic collarette of scales on the periphery with a thin brown crust covering the erosions. Lesions typically occur on the trunk, axilla, and extremities. Patients can spread infection to other body sites via autoinoculation by fingers, towels, or clothing. Systemic symptoms can include fever, fatigue, or diarrhea but are rare.4
Diagnosis of impetigo is made based on clinical findings, and testing is generally not needed. However, if testing is done, gram stain and culture of purulent fluid or exudates can identify whether S aureus or beta-hemolytic streptococcus is the cause.4,5
Treatment of impetigo, either nonbullous or bullous, includes topical antibiotics, oral antibiotics, disinfectant solution, or a combination.6 A Cochrane Review of impetigo interventions was published in 2012 and reflected 68 randomized controlled trials that compared various treatments for impetigo.6 Overall, topical antibiotics were superior to topical placebo. Two topical antibiotics in particular, mupirocin and fusidic acid, were found to be as least as effective as oral antibiotics for mild disease and equally as effective compared with the other. Isolated, small lesions can be treated with topical antibiotics while larger lesions and/or spreading lesions respond well with oral antibiotics.
Mupirocin is readily available but fusidic acid is not currently available in the United States. Parents might ask about OTC topical antibiotic ointments. Per Cochrane Review, bacitracin did not show a significant difference in cure rate compared with placebo8 and was significantly worse than cephalexin.9 One study looked at fusidic acid compared with neomycin/bacitracin10; that showed it was significantly more effective, especially with bullous impetigo. First-line treatment for mild nonbullous disease is mupirocin ointment three times daily for 7-10 days. For extensive nonbullous disease and for bullous impetigo, oral antibiotics or oral plus topical antibiotics are typically recommended. Oral antibiotic treatment options are listed in Table 1. For mild bullous disease that is distributed widely, cephalexin is typically chosen due to cost, general susceptibility, and palatability. If extensive lesions are present or there is a concern for MRSA infection, clindamycin or TMP/SMX should be considered as in this case.
| Table 1. Topical and Oral Antibiotic Therapeutic Options for Impetigo11 | ||
| Pediatric Dosing | Adult Dosing | |
| Topical antibiotics | ||
| Mupirocin | Apply to affected areas TID x 5-7 days | |
| Fusidic acid | Not available in the U.S. | |
| Preferred oral antibiotics | ||
| Cephalexin (Keflex) | 25-50 mg/kg/day in 3-4 divided doses | 250-500 mg 4 times/day |
| Dicloxacillin | 25-50 mg/kg/day in 4 divided doses | 250-500 mg 4 times/day |
| Alternate for penicillin or cephalosporin hypersensitivity | ||
| Erythromycin | 40 mg/kg/day in 304 divided doses | 250 mg 4 times/day |
| Clarithromycin | 15 mg/kg/day in 2 divided doses | 250 mg twice/day |
| If MRSA suspected or confirmed | ||
| Clindamycin | 20 mg/kg/day in 3 divided doses | 300-450 mg 4 times/day |
| Trimethoprim/sulfamethoxazole | 8-12 mg/kg (TMP)/day in 2 divided doses | 1-2 DS tables 2 times/day |
| Doxycyline | 2-4 mg/kg/day in 2 divided doses | 100 mg 2 times/day |
Postinfectious sequelae to consider include poststreptococcal glomerulonephritis and rheumatic fever, in cases caused by S pyogenes.
Additional History
The diagnosis of bullous impetigo was made based on history and physical examination. This patient was started on oral clindamycin and topical mupirocin ointment treatment with resolution of symptoms within a week’s time and no known recurrence of symptoms.
This case highlights the importance of clinical diagnosis and subsequent successful treatment of a common infectious dermatological condition.
Conclusion
The diffuse nature of the rash and the timeline of symptoms at presentation was a challenge for the provider in this case. Bullous impetigo is characterized by large flaccid bullae that can rupture and ooze a yellow honey-colored fluid. Diagnosis is made clinically without need for culture. First-line treatment for mild nonbullous impetigo is topical mupirocin.
First-line treatment for bullous impetigo is an oral antibiotic, such as cephalexin or clindamycin, plus a topical antibiotic, such as mupirocin.

Recognizing common pediatric rash presentations is crucial in an urgent care setting in order to differentiate treatment, avoid unnecessary testing, and to counsel patients on infectivity and expected duration of symptoms.
References
- Cernik C, Gallina K, Brodell RT. The treatment of herpes simplex infections: an evidence based review. Arch Intern Med. 2008;168(11):1137-1144.
- Mintz EM, Morel KD. Clinical features, diagnosis, and pathogenesis of chronic bullous disease of childhood. Dermatol Clin. 2011;29(4):459-462.
- Gladman AC. Toxicodendron dermatitis: poison ivy, oak, and sumac. Wilderness Environ Med. 2006;17(2):120-128.
- Hartman-Adams H, Banvard C, Juckett G. Impetigo: diagnosis and treatment. Am Fam Physician. 2014;90(4):229-235.
- Cole C, Gazewood J. Diagnosis and treatment of impetigo. Am Fam Physician. 2007;75(6):859-864.
- Konig S, van der Sande R, Verhagen AP, et al. Interventions for impetigo. Cochrane Database Syst Rev. 2012;(1):CD003261.
- Feaster T, Singer JI. Topical therapies for impetigo. Pediatr Emerg Care. 2010;26(3):222-227.
- Ruby RJ, Nelson JD. The influence of hexachlorophene scrubs on the response to placebo or penicillin therapy in impetigo. Pediatrics. 1973;52(6):854‐859.
- Bass JW, Chan DS, Creamer KM, et al. Comparison of oral cephalexin, topical mupirocin, and topical bacitracin for treatment of impetigo. Pediatr Infect Dis J. 1997;16(7):708‐710.
- Moraes Barbosa AD. Comparative study between topical 2% sodium fusidate and oral association of chloramphenicol/neomycin/bacitracin in the treatment of staphylococcic impetigo in newborn. Arq Bras Med. 1986;60(6):509-511.
- Stevens DL, Bisno AL, Chambers HF, et al. Practice guidelines for the diagnosis and management of skin and soft tissue infections: 2014 update by the Infectious Diseases Society of America. Clin Infect Dis. 2014;59(2):147-159.
Aimy T. Patel, MD, FAAP is assistant professor of pediatrics at the University of Missouri Kansas City School of Medicine, Children’s Mercy Kansas City. Allison Burris, MD, FAAP is assistant professor of pediatrics, University of Missouri Kansas City School of Medicine, Children’s Mercy Kansas City. Nirav Shastri, MD, FAAP, FAMIA, ABMS-CI is director, informatics and scholarly activities, Department of Pediatrics, Division of Emergency Medicine, Children’s Mercy Kansas City ED. The authors have no relevant financial relationships with any commercial interests.
