Published on
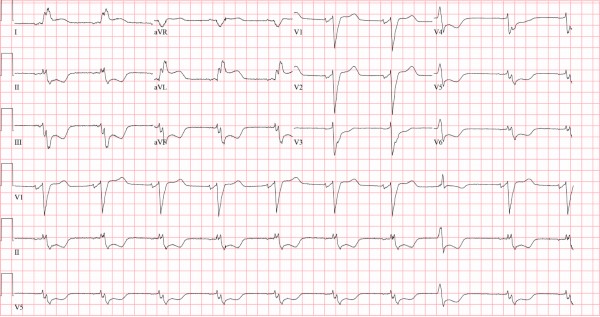
Baseline ECG:
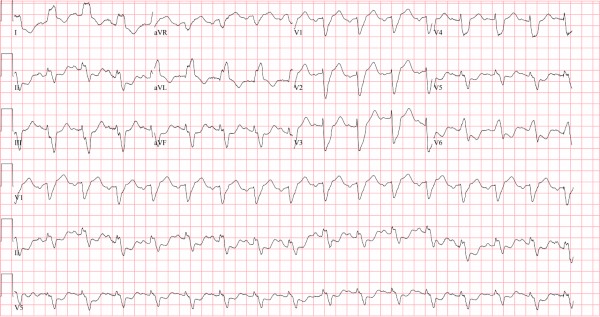
Differential Diagnosis:
- Normal left bundle branch block
- Acute myocardial infarction with left bundle branch block
- Left ventricular hypertrophy
- Hyperkalemia
Diagnosis
This patient was diagnosed with left bundle branch block. The ECG reveals a wide QRS complex (>120 ms) with a dominant S wave in V1 and notched R wave in the lateral leads I, aVL, and V6, indicating the presence of a left bundle branch block. There is concordant ST-elevation in I and aVL—meaning in the same direction as the QRS complex.
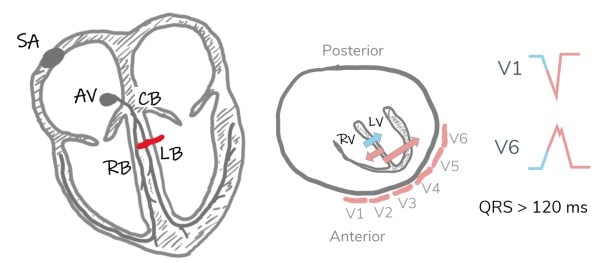
A left bundle branch block occurs when the left bundle no longer conducts, and the signal must pass to the left ventricle via myocyte-to-myocyte conduction. This pattern of conduction is slower than via the specialized conduction system, and results in a wide QRS complex (>120 ms). Conduction disturbances, like bundle branch blocks, result from structural abnormalities of the His-Purkinje system caused by necrosis, fibrosis, calcification, infiltrative disease, electrolyte disturbances, or impaired vascular supply.3 When conduction is impaired to both left ventricular terminals (the left anterior and posterior fascicles), the result is a left bundle branch block (Figure 3).
Normally, a left bundle branch block demonstrates characteristic discordant changes; ST segments tend to deflect in the opposite (ie, discordant) direction from the QRS complex (as demonstrated on the baseline ECG, Figure 2).
For instance, in leads with primarily down-going QRS complexes (ie, V1, V2, V3), slight ST-elevation is expected; and in leads with primarily up-going QRS complexes (ie, I, aVL, V5, V6), slight ST-depression is expected (along with repolarization abnormalities).
For decades, it was believed that the presence of a left bundle branch block obscured findings of acute myocardial infarction on the surface ECG. However, in 1996, Elena Sgarbossa identified electrocardiographic findings that suggested acute myocardial infarction in the presence of left bundle branch block, the so-called “Sgarbossa criteria.”4 The original Sgarbossa criteria heavily relied on the phenomenon of concordance—ST-segment deflection in the same direction as the QRS complex—as a powerful predictor of myocardial infarction, and is an indication for emergent reperfusion.5
In 2015, the original Sgarbossa criteria were modified to the following (as illustrated in Figure 4):6
- Concordant ST-elevation of ≥1 mm
- Concordant ST-depression of ≥1 mm in V1, V2, or V3, or
- Excessively discordant ST-elevation defined as the ST/S ratio >0.25
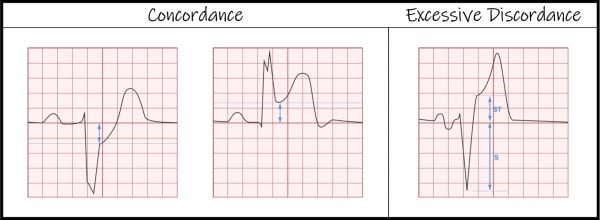
If any single modified Sgarbossa criterion is met, acute myocardial infarction is diagnosed and the emergent reperfusion pathway should be activated.6 The term intraventricular conduction delay describes any disturbance that delays conduction through the ventricles (eg, bundle branch blocks, hyperkalemia, sodium-channel blockade, left ventricular hypertrophy, etc.). It is termed “nonspecific” when bundle branch criteria are not met, which is not the case here. Hyperkalemia can cause all manner of conduction disturbances, but other features to suggest hyperkalemia are absent (eg, peaked T waves, flattened or absent P wave, or PR prolongation). While left ventricular hypertrophy can cause QRS widening, discordant ST changes, and repolarization abnormalities (although all to a lesser extent than left bundle branch block), these changes are better explained by the presence of a left bundle branch block in this case.
Back to the case: This patient was taken to the catheterization lab for emergent percutaneous coronary intervention to the left anterior descending and left circumflex arteries.
Learnings/What to Look for
- The criteria for left bundle branch block are: QRS >120 ms, dominant S wave in V1, broad monophasic or notched R wave in lateral leads (I, aVL, V5, V6), +/- left axis deviation
- Sgarbossa criteria describe ST changes that suggest acute myocardial infarction in the presence of left bundle branch block
- Concordance—ST-segment deflection in the same direction as the QRS complex—is a powerful predictor of myocardial infarction and is an indication for emergent reperfusion
- Excessive discordance describes ST-segment elevation with ST/S ratio greater than 0.25 (Figure 4) and should also be considered an indication for emergent reperfusion
Pearls for Initial Management
- All patients with left bundle branch block and symptoms concerning for acute coronary syndrome should be transferred to a percutaneous coronary intervention-capable facility
- Patients meeting modified Sgarbossa criteria should be immediately transferred via emergency medical services for emergent reperfusion. If capable, activate emergent reperfusion pathways
References
- Kusumoto FM, Schoenfeld MH, Barrett C, et al. 2018 ACC/AHA/HRS Guideline on the Evaluation and Management of Patients With Bradycardia and Cardiac Conduction Delay: A Report of the American College of Cardiology/American Heart Association Task Force on Clinical Practice Guidelines and the Heart Rhyth. Circulation. 2019;140(8):e382-e48
- Da Costa D, Brady WJ, Edhouse J. Bradycardias and atrioventricular conduction block. Br Med J. 2002;324:535-538.
- Surawicz B, Childers R, Deal BJ, Gettes LS. AHA/ACCF/HRS Recommendations for the Standardization and Interpretation of the Electrocardiogram. Part III: Intraventricular Conduction Disturbances A Scientific Statement From the American Heart Association Electrocardiography and Arrhythmias Committee, Council on Clinical Cardiology; the American College of Cardiology Foundation; and the Heart Rhythm Society. J Am Coll Cardiol. 2009;53(11):992-1002.
- Sgarbossa EB, Investigators G-1. Electrocardiographic diagnosis of evolving acute myocardial infarction in the presence of left bundle-branch block. N Engl J Med. 1996;334(8):481-487.
- Ibanez B, James S, Agewall S, et al. 2017 ESC Guidelines for the management of acute myocardial infarction in patients presenting with ST-segment elevation. Eur Heart J. 2018;39(2):119-177.
- Meyers HP, Limkakeng AT, Jaffa EJ, et al. Validation of the modified Sgarbossa criteria for acute coronary occlusion in the setting of left bundle branch block: A retrospective case-control study. Am Heart J. 2015;170(6):1255-1264.
