Published on
Differential Diagnosis
- Polyarteritis nodosa
- Calciphylaxis
- Cryoglobulinemia
- Panniculitis
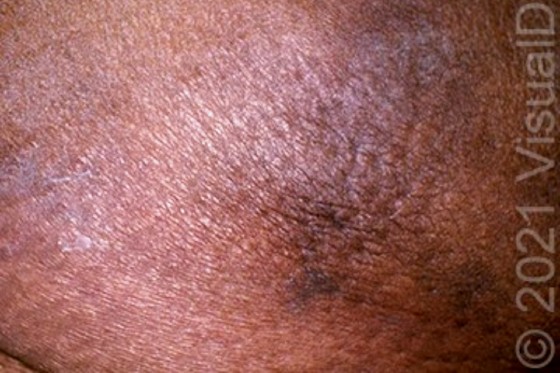
Diagnosis
The correct diagnosis is calciphylaxis, also known as calcific uremic arteriolopathy. This is a microvascular occlusion syndrome thought to occur due to diffuse deposition of insoluble calcium salts in cutaneous blood vessels with associated thrombosis. The process may be triggered by chronic hypocalcemia from decreased intestinal absorption of calcium, leading to increased levels of parathyroid hormone and subsequent recruitment of calcium and phosphate from bone. Hypercoagulable states are also thought to play a possible role
Learnings/What to Look for
- Characteristic pathologic findings include progressive medial calcification of cutaneous blood vessels and subsequent ischemic necrosis of the skin
- Warfarin-associated nonuremic calciphylaxis tends to occur on the lower extremities about 2.5 years after warfarin initiation, does not have associated calcium abnormalities
- Early lesions are extremely painful, violaceous retiform patches and plaques, classically on fat-bearing areas such as the thighs, buttocks, or abdomen. This is followed by necrosis, ulcers, eschar formation, and possibly gangrene. Induration of the surrounding tissues may be present
- Lesions have been reported to be triggered by local trauma, including from insulin or heparin injections, or a skin biopsy
- Incidence of calciphylaxis is increasing and is most commonly associated with chronic renal failure, hemodialysis, and secondary hyperparathyroidism. Other risk factors include female sex, obesity, Northern European descent, and hypoalbuminemia
Pearls for Urgent Care Management
- Mortality from calciphylaxis is high (60%-87%) and is largely secondary to sepsis from large, nonhealing ulcers
- A multidisciplinary approach is likely to be necessary and would include wound care, nephrology, dermatology, and pain management
- The most common intervention is off-label use of intravenous sodium thiosulfate1
- Other treatments described in case reports include bisphosphonates, low-tissue plasminogen activator infusion, LDL-apheresis, vitamin K, and kidney transplant1
Reference
- Nigwekar SU, Kroshinsky D, Nararian RM, et al. Calciphylaxis: risk factors, diagnosis, and treatment. Am J Kidney Dis. 2015;66(1):133-146.
Acknowledgment: Image and case presented by VisualDx (www.VisualDX.com/JUCM).
