Nothing hurts a business more than leaving money on the table. It is hard enough to attract business; the last thing you want to do is not get paid once services are rendered. There are a number of steps in the coding and billing process, and errors at any level can lead to bad debt, missed charges, and poor reimbursement. Let’s look at a few I would call the “low-hanging fruit.” Collection at the Time …
Read MoreWriting Off Patient Responsibility, Modifier-51, and More on New vs. Established E/M Codes
DAVID STERN, MD (Practice Velocity) Q. I listened to your UCA coding webinar, and it raised a question. You mentioned that if we bill insurance for a 99051 and the payor denies payment as “patient responsibility,” then we should bill the patient and not write it off. Does that hold true to the S9088, as well? I often see this code either denied or applied to the patient’s coinsurance/deductible. Question submitted by Megan Fontenot, Integrity …
Read More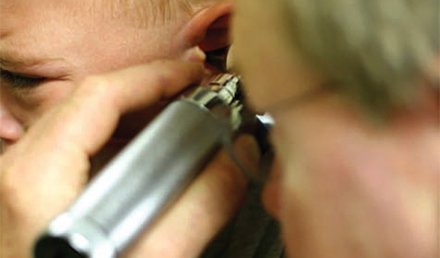
May 2010
Coding X-Rays Ordered by Outside Docs, G-code for Drug Testing, and 99051 for Scheduled Visits
DAVID STERN, MD (Practice Velocity) Q. We have quite a few primary care physicians who regularly send patients to our urgent care center for x-rays. These patients have a prescription for the x-ray service, and they don’t want to be seen by the urgent care doctor. I have several questions related to this service: Should we collect the urgent care copay (or) radiology imaging services copay (which is usually $0)? Should we code S9083 to …
Read More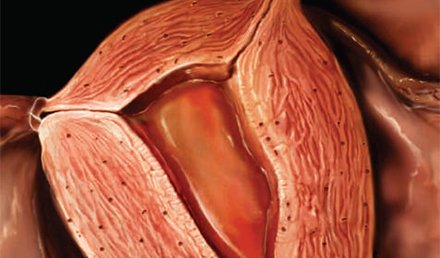
April 2010
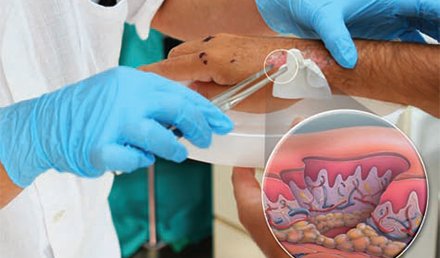
March 2010
Consult Codes, Injection Codes, and Coding for Diabetes Education and In-House Dispensing
Q. My codes for consults seem to suddenly be getting denied as invalid. I checked my CPT book, and the codes are still listed as valid. What’s going on? Question submitted by multiple urgent care billers A. Yes, you are right that the consultation codes (99241-99245, 99251-99255) are still valid per CPT, as published by the AMA. CMS, however, has decided to no longer reimburse for those codes and has now changed the status indicator …
Read MoreCoding for Two Visits in One Day, Billing for Atypical Urgent Care Services, and Billing on the UB-04
Q. The patient in question is a new patient to the urgent care. At 10 a.m., she visited the urgent care with chief complaint of cough, headache, and myalgias. She was discharged home with a final diagnosis of cough and prescription for ibuprofen and cough syrup. At 3 p.m., she retuned with a complaint of headache and was treated with IM headache medications and sent home with a diagnosis of headache with pain meds. How …
Read More
February 2010
Coding by Time, for Emergent Care, and for Nurse Practitioner Visits
Q. How does one determine whether an E/M code can qualify for coding according to time spent? Obviously, any psychiatric counseling would fit the criteria, but what about “teaching” (e.g. how to use an inhaler, how to perform a breast exam), or preventive medicine counseling? – Question submitted by Dr. Kim, Med7 Urgent Care, CA A. The key issues on counting counseling or coordination of care toward the E/M code are: Counseling and/or coordination of …
Read More