Published on
Michael B. Weinstock, MD; Michael Pallaci, DO; Amal Mattu, MD; Cameron Berg, MD; Paul Jhun, MD; and Jeff Riddell, MD.
Urgent message: Patients who present with chest pain but tests indicate there is little risk for a major event can leave providers uncertain as to what next steps are appropriate, and raise concerns for bad outcomes and litigation.
Citation: Weinstock MB, Pallaci M, Mattu A, Berg C, Jhun P, Riddell J. Most Clinicians Are Still Not Comfortable Sending Chest Pain Patients Home with a Very Low Risk of 30-Day Major Adverse Cardiac Event (MACE). J Urgent Care Med. 2021;15(5):17-21.

Introduction
Chest pain is the second-leading cause of presentation to the emergency department, accounting for 4.7% of all ED visits and totaling more than 6.5 million visits per year in 2017.1 Patients presenting with chest pain are evaluated for multiple diagnoses including deadly conditions such as acute coronary syndrome (ACS), pulmonary embolism, and thoracic aortic dissection. However, after these diagnoses have been excluded with bedside evaluation and/or testing, the disposition often represents a clinical conundrum for treating providers; what is the acceptable miss rate for ACS?
In patients presenting with a clear diagnosis of ST elevation myocardial infarction (STEMI) by electrocardiogram or with positive biomarkers indicating myocardial damage (nSTEMI), the medical decision-making pathway is easily established; patients are sent emergently to the cardiac catheterization lab or admitted to a monitored bed. The difficulty in disposition arises when the initial clinical evaluation is reassuring, but subsequent testing reveals unexpectedly positive findings. In an attempt to stratify patients, clinical tools such as the HEART (H=history, E=ECG, A=age, R=risk factors, T=troponin) score have been used to determine additional testing and discharge endpoints.2,3
As with all clinical disposition decisions, the provider weighs the risks, including a missed major adverse coronary event (MACE), defined as death, MI, or revascularization, with the possible risk of harm from over testing and the inherent risks of hospital admission.4 Additionally, there are possible legal implications for the provider; among medical litigation cases in the United States, missed MI is the condition associated with the highest number of claims.5,6
After a negative evaluation for MI, the question present in the mind of the clinician at the bedside is: What level of a MACE is acceptable among practicing providers? The 2018 American College of Emergency Physicians (ACEP) clinical practice guideline estimates an acceptable missed diagnosis rate of 1%–2% for a 30-day MACE in nSTEMI ACS.7 Prior to release of the ACEP statement, this question was posed to participants at the Essentials of Emergency Medicine conference in Las Vegas in 2018. We sought to determine the percent of clinicians who are comfortable with varying degrees of MACE after a negative ED chest pain evaluation.
METHODS
This study was approved by the Adena Health Systems IRB #18-05-024 prior to the poll. Essentials of Emergency Medicine is an annual, 3-day, continuing medical education conference certified by the American Medical Association for Physician’s Recognition Award Category 1 CME credit. During the Essentials of Emergency Medicine conference in 2018, with 1,391 onsite and livestream attendees, a pilot survey was sent to a convenience sample of attendees. Conference participants were asked to download an app to their electronic devices. An invitation to participate in a brief survey was sent to those who downloaded the app. There were also announcements during the conference encouraging conference attendees to complete the survey. The survey consisted of five demographic questions and one clinical opinion question adapted from a similar study by Than, et al.8 The survey was closed on the third day of the conference, before results were revealed to the attendees.

All data was collected electronically and anonymously and compiled on a Microsoft Excel spreadsheet. After collecting demographic data, including practice location, professional role, primary work environment, years of clinical experience, and practice setting, the participants were asked the single question detailed in Figure 1 (identical to the final question in the study by Than, et al8).
Results
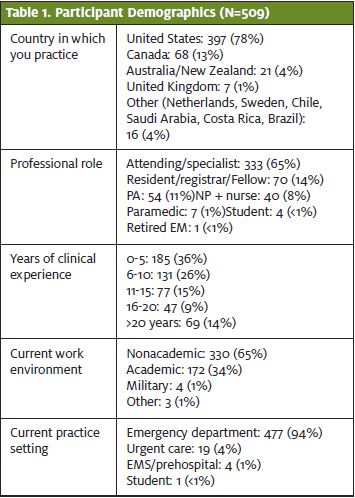
Respondents included practitioners from the United States (78%), Canada (13%), Australia/New Zealand (4%), and other countries (4%). Most participants were attending physicians (65%), with the majority having 0 to 5 years of clinical experience post-residency (36%). A majority of the respondents (65%) were from nonacademic settings. Most respondents worked primarily in emergency medicine (94%), while 4% worked primarily in the urgent care setting. (See Table 1.)
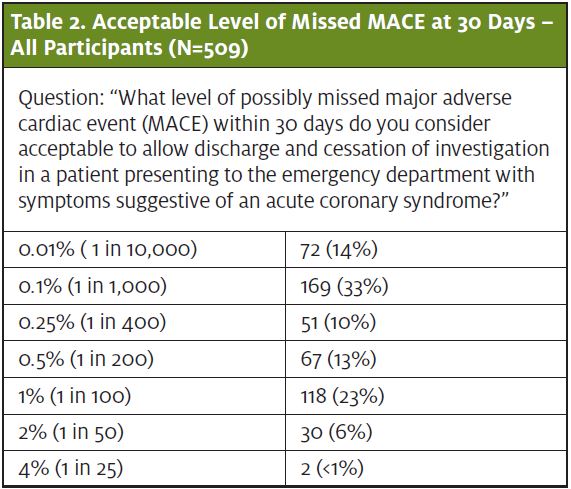
Among the participants, 47% would accept a miss rate of 1/1,000 or 1/10,000 (0.01%–0.1%). Less than 1/3 of participants (29%) would accept a miss rate of 1%–2%. (Table 2).
When looking specifically at the 19 clinicians who work in urgent care (see Table 1), 14 were from the United States, four from Canada, and one from Australia. Attendings/specialists compromised 12, nurse practitioners five, physician assistants one, and EMS one. There were seven clinicians who considered a 1/10,000 (0.01%) level of MACE acceptable, six who considered 1/1,000 (0.1%) acceptable, two at 1/200 (0.25%), one at 1/200 (0.5%), and two at 1/100 (1%), and 1 at 1/50 (2%).
DISCUSSION
Among the participants, almost half (47%) would only accept a miss rate of MACE of 1/1,000 or 1/10,000, far lower than the threshold established by the 2018 ACEP clinical policy7 (released after this study was concluded). In fact, only 29% of the 509 participants in this study were comfortable with the 1%–2% level of MACE deemed to be acceptable by the ACEP statement.
Though the participants who work in the urgent care were a minority of the participants in the study, 13/19 (68%) would only accept a miss rate of MACE of 1/1,000 or 1/10,000, higher than the 47% when looking at all participants in the study.
There is much practice variation in evaluation and management of patients with chest pain, based on the clinician’s comfort with risk,9 the possible risk to the patient (though not necessarily with being involved in a past malpractice action.)10 Concern for malpractice is understandable; a 2010 study of closed malpractice claims, over a 23-year period, involving emergency medicine physicians found acute myocardial infarction (MI) and undifferentiated chest pain to be the two leading reasons for claims with associated indemnity.6 Historically, the rate of missed MI among patients presenting with chest pain to the emergency department is quoted as 2% based on a paper by Pope, et al, in which the authors conclude that those patients discharged with undifferentiated chest pain have higher mortality.11 However, a review of the data in the Pope paper indicated that 19 of the 10,689 patients who were discharged from the ED were subsequently diagnosed with MI, which equates to 0.17% rather than the quoted 2%.12 Additionally, the data are old, collected over a 7-month period of time in 1993 using CK-MB (before the use of conventional or high sensitivity troponin testing).11
More recent data from Backus, et al showed that in patients with a low-risk HEART score, the risk of MACE was 1.7% in the Netherlands.3 An analysis of low-risk HEART patients in North America showed a much lower rate of 0.8%.13 Mahler, et al examined over 8,474 adult chest pain patients and found that those with a low-risk HEART score had a 0.4% risk of MI or death.3,14 Note that Backus, et al used only one troponin for 6-week outcomes and a MACE which included MI and death in addition to percutaneous coronary intervention, coronary artery bypass grafting, or coronary angiography revealing procedurally correctable stenosis managed conservatively.3 Mahler, et al used two troponins performed 3 hours apart with a 30-day MACE outcome defined as MI or death.14
Weinstock, et al examined 7,266 ED with interpretable and nonischemic ECGs, nonconcerning vital signs, and two negative troponin tests admitted to the hospital, and found only four had a clinically relevant adverse cardiac event (CRACE) defined as MI, death, life-threatening arrhythmia, or inpatient STEMI during their hospital course.15
The bedside clinician is forced to grapple with risk assessment and stratification, personal risk threshold of acceptable missed MACE, and the perceived or actual risk of litigation based on case characteristics. The 2018 ACEP clinical practice guideline for management of ED patients with chest pain states that “the majority of patients and providers would agree that a missed diagnosis rate of 1% to 2% for 30-day MACE in NSTE ACS is acceptable.” They further state that there are limitations to diagnostic testing and that there is a need to avoid harms associated with false-positive tests.7
While these ACEP guidelines are available to all (note that this ACEP Clinical Policy was not yet released at the time of the survey), the ultimate decision-maker of acceptable miss rate of MACE is the clinician responsible for the care of the patient. Our poll indicates that despite all of the clinical reference tools, available evidence, and statements from professional organizations, the threshold for what is an acceptable miss rate of MACE is as variable as this patient population.
The authors were surprised by how low the level of acceptable MACE is for many clinicians. In fact, almost half of clinicians would only accept a risk of MACE of 1/1,000 or 1/10,000. If all of these patients were admitted to the hospital, there would be a risk of significant harm. One study showed that 1/164 admitted patients had a preventable adverse event contributing to their deaths, in addition to nonfatal events such as deep vein thrombosis, nosocomial pneumonia, falls resulting in head injuries or hip fractures, sundowning syndrome (acute delirium in elderly hospitalized patients), and false positive tests, as well as expense to patients and the health care system.4
Brooker, et al showed with a hypothetical “acceptable miss rate” of 1%–2%, that 29% of the patients with chest pain in the ED would not be admitted.16 At the bedside in the ED and the urgent care center, there are many techniques available to improve patient and clinician comfort with outpatient management; shared decision-making , demonstrated by Hess, et al in multiple studies, was an effective technique.17-20
This study furthers our current knowledge about the acceptable rate of missed MACE in chest pain patients. Next steps include attempting to discern if the 2018 ACEP policy statement has changed clinician’s perceptions about the acceptable miss rate for MACE with a planned repeat survey at the 2021 EEM conference in Las Vegas.
LIMITATIONS
The attendees of the conference were likely comprised of clinicians motivated enough about their ongoing education to travel to Las Vegas to attend the conference, perhaps providing a sample that is not reflective of urgent care and emergency medicine clinicians nationally. Though the survey was available to everyone who attended the Essentials of Emergency Medicine course in Las Vegas in 2018, slightly more than half of those downloaded the app and completed the survey. This selection bias may limit the external validity of our findings.
There are different definitions and timelines of MACE, depending on whether revascularization is included, such as with the validation HEART study,3 or if only MI and death are included, such as with the 2018 Mahler HEART pathway study.14 If a patient is sent home with and subsequently has a MACE, this does not necessarily mean there was poor care. For example, if a patient is diagnosed with coronary disease and has appropriate follow-up and has a revascularization procedure, this will still be counted as MACE in some studies, even though there was not an adverse outcome.21 It is possible that the participants had varied definitions or did not understand the definition and answered with varied understandings of definition of MACE.
Further research, since publication of the 2018 ACEP guidelines, will be needed to assess whether their recommendation for consideration of a 1%–2% acceptable miss rate leads to changes in practice patterns.
CONCLUSION
Most clinicians are not comfortable when discharging chest pain patients even with a possible 1%–2% rate of MACE.
REFERENCES
- Rui P, Kang K. National Hospital Ambulatory Medical Care Survey: 2017 emergency department summary tables. National Center for Health Statistics. Available at: https://www.cdc.gov/nchs/data/nhamcs/web_tables/2017_ed_web_tables-508.pdf. Accessed January 12, 2021.
- Singer AJ, Than MP, Smith S, et al. Missed myocardial infarctions in emergency department patients prospectively categorized as low risk by established risk score. Am J Emerg Med. 2017;35(5):704-709.
- Backus BE, Six AJ, Kelder JC, et al. A prospective validation of the HEART score for chest pain patients at the emergency department. Int J Cardiol. 2013;168(3):2153–2158.
- James JT. A new, evidence-based estimate of patient harms associated with hospital care. J Patient Saf. 2013;9(3):122-128.
- Ferguson B, Geralds J, Petrey J, Huecker M. Malpractice in emergency medicine—a review of risk and mitigation practices for the emergency medicine provider. J Emerg Med. 2018;55(5):659-665.
- Brown TW, McCarthy ML, Kelen GD, Levy F. An epidemiologic study of closed emergency department malpractice claims in a national database of physician malpractice insurers. Acad Emerg Med. 2010;17(5):553-560.
- American College of Emergency Physicians Clinical Policies Subcommittee (Writing Committee) on Suspected Non–ST-Elevation Acute Coronary Syndromes:, Tomaszewski CA, Nestler D, Shah KH, Sudhir A, Brown MD. Clinical Policy: Critical Issues in the Evaluation and Management of Emergency Department Patients With Suspected Non-ST-Elevation Acute Coronary Syndromes. Ann Emerg Med. 2018;72(5):e65-e106.
- Than MP, Herbert M, Flaws D, et al. What is an acceptable risk of major adverse cardiac event in chest pain patients soon after discharge from the Emergency Department? A clinical survey. Int J Cardiol. 2013;166(3):752-754.
- Smulowitz PB, Barrett O, Hall MM, et al. Physician variability in management of emergency department patients with chest pain. West J Emerg Med. 2017;18(4):592-600.
- Carlson JN, Foster KM, Black BS, et al. Emergency physician practice changes after being named in a malpractice claim. Ann Emerg Med. September 9, 2019. [Epub ahead of print.]
- Pope HJ, Aufderheide TP, Ruthazer R, et all. Missed diagnoses of acute cardiac ischemia in the emergency department. N Engl J Med. 2000;342(16):1163-1170.
- Morgenstern J. Stress test part 1: how often do we miss MI? First 10 EM. 2019. Available at: https://first10em.com/mi-miss-rate/. Accessed January 12, 2021.
- Laureano-Phillips J, Robinson RD, Aryal S, et al. HEART Score Risk Stratification of Low-Risk Chest Pain Patients in the Emergency Department: A Systematic Review and Meta-Analysis. Ann Emerg Med. 2019;74(2):187-203.
- Mahler SA, Lenoir KM, Wells BJ, et al. Safely identifying emergency department patients with acute chest pain for early discharge. Circulation. 2018;138(22):2456-2468.
- Weinstock MB, Weingart S, Orth F, et al. Risk for clinically relevant adverse cardiac events in patients with chest pain at hospital admission. JAMA Intern Med. 2015;175(7):1207-1212.
- Brooker JA, Hastings JW, Major-Monfried H, et al. The association between medicolegal and professional concerns and chest pain admission rates. Acad Emerg Med. 2015;22(7):883-886.
- Hess EP, Knoedler MA, Shah ND, et al. The chest pain choice decision aid. A randomized trial. Circ Cardiovasc Qual Outcomes 2012;5(3):251–259.
- Hess EP, Coylewright M, Frosch DL, Shah ND. Implementation of shared decision making in cardiovascular care: past, present, and future. Circ Cardiovasc Qual Outcomes. 2014;7(5):797–803.
- Hess EP, Grudzen CR, Thomson R, et al. Shared decision-making in the emergency department: respecting patient autonomy when seconds count. Acad Emerg Med. 2015;22(7):856–864.
- Hess EP, Hollander JE, Schaffer JT, et al. Shared decision making in patients with low risk chest pain: prospective randomized pragmatic trial. BMJ. 2016;355:i6165.
- Weinstock MB, Finnerty NM, Pallaci M. Time to move on: redefining chest pain outcomes. J Am Heart Assoc. 201918;8(12):e012542.
Statement from Dr. Weinstock: This author takes responsibility for all aspects of the reliability and freedom from bias of the data presented and their discussed interpretation. There was not funding provided for this study. This study is IRB approved by the Adena Health System IRB.
Author affiliations: Michael B. Weinstock, MD, Adena Health System; Department of Emergency Medicine, Wexner Medical Center at The Ohio State University; Emergency Medicine Reviews and Perspectives (EM RAP); The Journal of Urgent Care Medicine; Urgent Care Reviews and Perspectives (UC RAP); Ohio Dominican University Physician Assistant Studies Program. Michael Pallaci, DO, Adena Health System. Amal Mattu, MD, University of Maryland. Cameron Berg, MD, North Memorial Health Care. Paul Jhun, MD, FAAEM, University of California San Francisco. Jeff Riddell, MD, Keck School of Medicine of the University of Southern California.


