Published on
Urgent message: Acute sinusitis poses frequent challenges in urgent care where patient volumes are high and patient satisfaction is valued. An educational session and an algorithmic clinical decision-support tool were implemented in a multisite urgent care quality improvement project which resulted in a statistically significant reduction in antibiotic prescribing for acute sinusitis.
ABSTRACT
Background
Sinusitis is a common upper respiratory condition seen in urgent care centers, as it is in primary care practices and, increasingly of late, telemedicine. Despite a strong body of evidence to support the use of practice guidelines for sinusitis, consistency in diagnosis and treatment of acute sinusitis is lacking. Antibiotics are often prescribed inappropriately, leading to unnecessary side effects, medication interactions, antibiotic resistance, and increased costs. There is evidence that antibiotic stewardship interventions can improve guideline adherence. The purpose of this project was to implement an antibiotic stewardship program and evaluate its effect on antibiotic prescribing for adults with acute sinusitis by urgent care providers.
Methods
Changes in antibiotic prescribing were evaluated for adults with acute sinusitis following provider education on current sinusitis guidelines and implementation of a clinical decision support (CDS) tool at 14 affiliated urgent care centers in an urban and suburban metropolitan area of the Northwest. Number of antibiotic prescriptions, frequency of guideline adherence for diagnosis and drug choice, and use of at least one guideline-recommended supportive measure were assessed with a random sampling of sinusitis charts, pre- and postintervention (n=74 and n=72, respectively).
Results
Antibiotic prescribing rates for acute sinusitis decreased by 20% (p=0.012) in the month following intervention. There were small but insignificant improvements in guideline adherence for diagnosis, drug choice, and supportive measure recommendation.
Discussion
This multisite quality improvement project with a statistically significant reduction in antibiotic prescribing for acute sinusitis shows that a simple educational intervention for providers coupled with an algorithmic CDS tool can be effective. This is a promising approach that could be easily implemented in urgent care and other ambulatory settings.
Background
Sinusitis is a common upper respiratory illness with over 30 million adults in the U.S. diagnosed annually.1 A retrospective cohort study found sinusitis to account for 11.1% of over 2.7 million urgent care visits from a large nationwide database.2 Sinusitis accounts for more than 1 in 5 antibiotic prescriptions for adults, making it the fifth most common diagnosis responsible for antibiotic use and resulting in $5.8 billion in annual healthcare costs. Current trends that emphasize patient satisfaction incentivize providers to prescribe treatments that will meet patients’ expectations, such as antibiotics.
For the purposes of this article, the terms sinusitis and rhinosinusitis are used interchangeably. Rhinosinusitis is an inflammation of the mucosal lining of the nasal passage and paranasal sinuses.3 Symptoms lasting less than 4 weeks can be classified as acute, 4-12 weeks subacute, and more than 12 weeks chronic. Differentiating between acute bacterial rhinosinusitis (ABRS) and viral rhinosinusitis is clinically challenging. Acute rhinosinusitis usually begins after an upper respiratory infection (URI), then inflammation moves into the paranasal sinuses. It is estimated that 90%-98% of acute rhinosinusitis cases are viral, whereas only 2%-10% of cases can be attributed to bacterial causes.3 Prescribing practices should reflect the low rate of bacterial disease. Even when antibiotics are indicated by guideline, the Infectious Diseases Society of America (IDSA) reports that approximately 70% of patients with acute rhinosinusitis improve spontaneously in placebo-controlled randomized clinical trials.2
Unnecessary antibiotic use exposes patients to preventable and potentially serious health problems. The emergence of drug-resistant bacteria is a critical public health threat with a reported 2.8 million antibiotic-resistant infections occurring each year and claiming the lives of 35,000 people in the U.S. each year.4 The CDC estimates that 30% of all antibiotics prescribed in the outpatient setting are unnecessary.5 Urgent care centers have the highest percentage of visits leading to an antibiotic prescription and were much more likely to prescribe antibiotics unnecessarily for respiratory illnesses that don’t require antibiotics.2 Pulia, et al conclude that a global increase in antimicrobial-resistant infections, in combination with limited development of new antibiotics, raises concern for a “post-antibiotic era” with potential catastrophic consequences.6
CLINICAL PRACTICE GUIDELINES
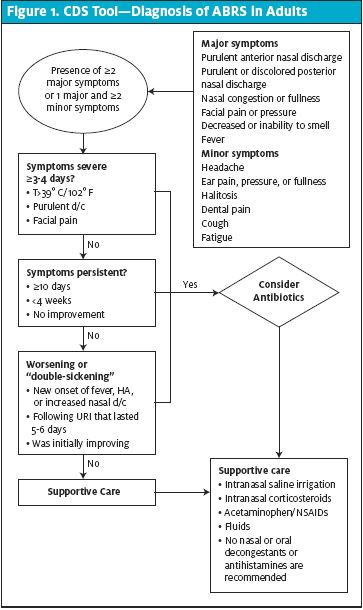
The current guidelines for the diagnosis and treatment of sinusitis were developed by the Infectious Disease Society of America and American Academy of Otolaryngology–Head and Neck Surgery.1,3 Due to their simplicity and clarity, the recommendations from IDSA were used as the primary source for our study. Some recommendations (such as duration of treatment) were integrated from the AAO–HNS guidelines. Diagnosis of ABRS can be differentiated from viral sinusitis when the patient meets any of the three clinical presentations: severe, persistent, or worsening” (Table 1).

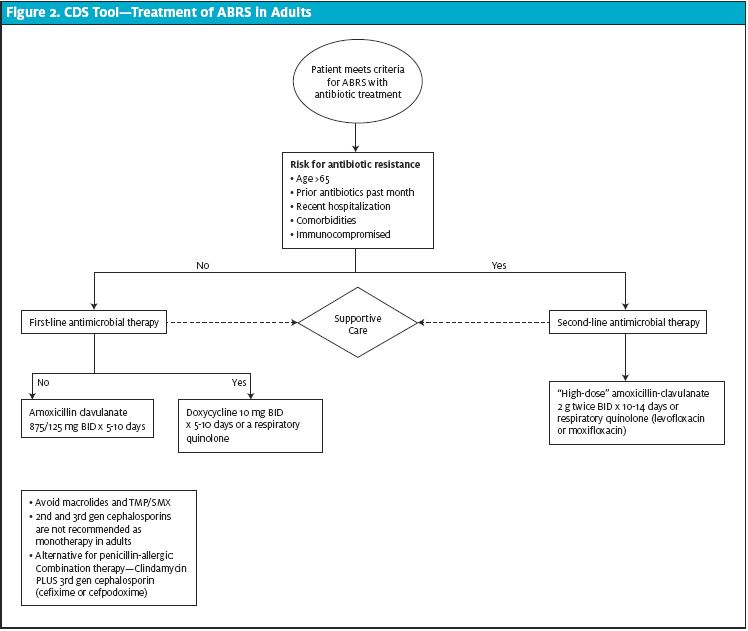
The most common pathogens responsible for ABRS are H influenzae, S pneumoniae, and M catarrhalis. According to the IDSA guidelines, first-line treatment for non-penicillin allergic patients with ABRS is amoxicillin with clavulanate, due to increasing b-lactam resistance in some regions of the United States. Doxycycline may be used as a first-line alternative regimen for adult patients who are penicillin-allergic. Respiratory quinolones (moxifloxacin and levofloxacin) are also options but are not superior to amoxicillin-clavulanate and carry a higher prevalence of adverse effects and increased costs. Macrolides (azithromycin and clarithromycin), TMP/SMX (Bactrim), and second- and third- generation oral cephalosporins are not recommended for empiric therapy.
Supportive measures should be recommended for both ABRS and viral sinusitis. This includes analgesics (acetaminophen and NSAIDS), antipyretics, intranasal saline irrigation, intranasal corticosteroids, and hydration. Neither topical nor oral decongestants or antihistamines are recommended as supportive care treatments due to low efficacy.
METHODS
An antibiotic stewardship program was implemented at 14 urgent care centers using the Plan – Do – Study – Act model for change.7 A clinical decision support (CDS) tool was developed for use at the point-of-care with patients with sinusitis symptoms, using the practice guidelines from the IDSA. To evaluate the program’s effectiveness, a sample of medical records of adult patients seen for sinusitis was audited pre- and postintervention.
SETTING AND PARTICIPANTS
The study was conducted in Legacy GoHealth Urgent Care clinics (n= 14) in the Portland, OR metropolitan area. There were approximately 60 providers: physicians, nurse practitioners, and physician assistants. Each clinic was managed under the same leadership and utilized the same electronic health record (EHR) and protocols. The network of clinics provides care in roughly 13,000 patient encounters each month. During peak seasons, the clinics provide care to over 600 patients a month with acute sinusitis. During the study periods, there were 398 and 177 patients diagnosed with acute sinusitis before and after the program implementation, respectively.
POPULATION
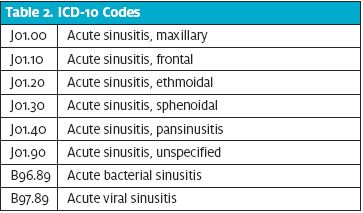
Adult patients being treated for acute sinusitis were included in the study. Inclusion criteria were a) age 18 or older and b) diagnosed with acute sinusitis using the International Classification of Diseases, 10th edition (ICD-10) codes for acute sinusitis. All eight ICD-10 codes for acute sinusitis were used in order to capture the target population (Table 2). Patients were excluded if they a) had symptoms more than 4 weeks, b) were under 18 years of age, c) had had an ear, nose, and throat (ENT) procedure in the past 1 year, d) had had a history of facial or nasal trauma, e) were treated with an antibiotic in the past 30 days, and f) were immunocompromised. These exclusion criteria were congruent with the guideline’s definition of “uncomplicated acute bacterial rhinosinusitis.” Patients were also excluded if they had another concurrent diagnosis requiring antibiotic treatment (eg, acute otitis media, which might influence choice of antibiotic). Identification of these exclusion criteria during data collection was reliant on thorough history taking and documentation by the provider and thus may not have reliably excluded some patients with such histories. Absent such documentation, we presumed these factors were not present.
An educational session was developed to include review of current sinusitis guidelines and introduction of the CDS tool. Education was delivered via a twenty-minute webinar to providers (n=39 in attendance) during a monthly educational meeting and by dissemination of the same content by e-mail to all providers. Attendance at the meeting had an approximate 65% turnout rate. Providers not in attendance were required to view webinar materials and attest to viewing. The CDS tool (see Figure 1 and Figure 2) was created and posted at provider workstations in all 14 clinics and in the online resource portal available to all providers. In-person discussion of the project was held at each of the 14 clinics.
Measures
Pre- and postintervention data were collected through a retrospective review of patient medical records in the EHR. An electronic report was executed by the organizational leadership to identify a list of patients who met inclusion criteria. Charts were obtained for visits during the month before the educational intervention (May 2019) and one month after (July 10, 2019– August 10, 2019), and a random sample was selected. Each included chart was individually reviewed by the DNP student investigator to determine guideline adherence and data were collected in a spreadsheet with a de-identified patient record number.
Data Analysis Preintervention totals of each data point were aggregated and compared to postintervention data, looking specifically at the overall number of antibiotic prescriptions, rates of guideline adherence for diagnosis and drug selection, and frequency of guideline-recommended supportive measure in treatment plan (Table 3). P-value was calculated using the chi squared test with continuity correction withMonte Carlo simulation.
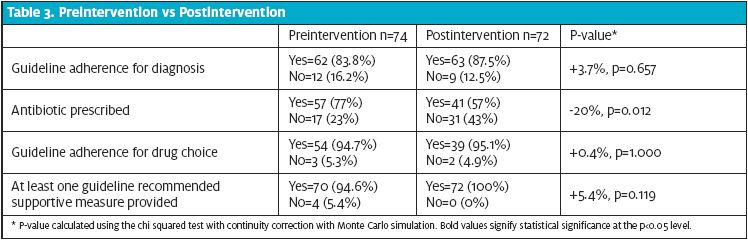
The preintervention audit report consisted of 398 charts of patients diagnosed with acute sinusitis during the month of May. After selecting the sample of every fifth chart, and eliminating patients with exclusion criteria, a total of 78 charts were reviewed manually. Four charts were later eliminated due to the presence of concurrent diagnoses requiring antibiotics, leaving a sample size of 74. From this sample, 77% (n=57) received antibiotic treatment and 83.8% (n=62) met the guidelines for diagnosis. Twelve patients did not meet the guideline criteria for diagnosis (16.2%), which indicates 21% of the antibiotic treatment group received antibiotics inappropriately. Three of the 57 patients treated with antibiotics were given a guideline-deviant drug selection (5.3%).
The postintervention audit report consisted of 177 patient encounters, a reduction of 65% from the preintervention report. For this reason, the sampling was increased. A total of 75 charts were reviewed individually. Three charts were eliminated due to concurrent diagnoses requiring antibiotics leaving a sample size of 72 (Table 3). From this sample, 57% (n=41) received antibiotic treatment and 87.5% (n=63) met guideline criteria for diagnosis. Nine patients (12.5%) did not meet the guideline criteria for diagnosis as determined by lack of documentation of meeting one of the three criteria for diagnosis (Table 1), which indicates 22% of the antibiotic treatment group received antibiotics inappropriately. Only two of the 41 patients treated with antibiotics were given a guideline-deviant drug (4.9%).
ETHICAL CONSIDERATIONS
The project design, CDS tool, and educational materials were approved by clinic leadership and IRB exemption was obtained by the organization. IRB approval was obtained from the Gonzaga University Institutional Review Board. In order to protect individual identities and meet HIPAA regulations, no participants’ names, initials or other identifiers were collected. Individual provider performance was not measured and only group data was reported. This quality improvement project had direct oversight by organizational leaders in all stages of planning and implementation.
DISCUSSION
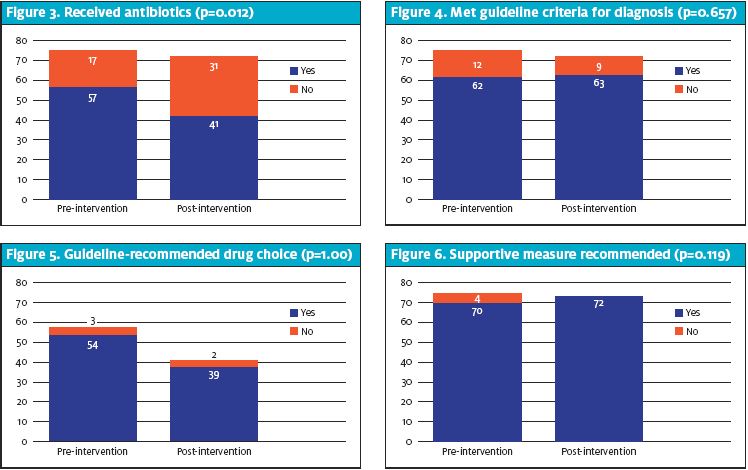
There was a statistically significant reduction in frequency of antibiotic prescribing after the program was implemented (p=0.012) (Figure 3). There were statistically insignificant improvements in the area of guideline adherence for diagnosis (p=0.657) (Figure 4), correct drug choice (p=1.000) (Figure 5), and guideline supportive measure recommendation (p=0.119) (Figure 6). The significant decrease in total patients diagnosed with acute sinusitis during the postintervention period compared to baseline volumes (n=177 vs n=398) is likely due to the seasonality of the illness, with the postintervention time period falling in the summer. This could also be attributed to changes in the use of the acute sinusitis diagnosis codes after the provider education and introduction to the CDS tool.
LIMITATIONS
Some variables could not be accounted for and may have influenced the outcome. The provider mix was an uncontrolled variable that could have made an impact on the outcomes. Providers were not individually identified during the data collection; therefore, the included patients were not limited to the providers who attended the educational session. Despite the low provider turnout at the educational session (65%), each provider was sent the educational materials by email and required to watch the webinar and attest to it by email. The protocol was also made available online, as well as posted at each site. Due to the large number of providers and some level of provider turnover, it is possible that the preintervention patients were seen by a different mix of providers than the postintervention patients, and who might have had different prescribing practices. There was also a challenge in directly connecting with each provider due to number of sites and variability of schedules.
Organization leadership provided informal feedback to the authors. They indicated that most providers did not perceive the guideline education and CDS tool as a significant change in practice. The study was conducted during the summer months when sinusitis and upper respiratory volumes were much lower than in winter, which could have provided more time for provider engagement than during busier months. However, lower volumes could have reduced the focus on quality improvement for this particular diagnosis. Although individual provider feedback was not directly solicited, no negative reactions were expressed. Since patient satisfaction within the organization is highly emphasized, this poses a challenge in that antibiotic prescribing is often perceived as a patient satisfier.
CONCLUSION
In a high-volume urgent care setting, providers face pressure to see patients quickly. Emphasis on patient satisfaction scores and reviews incentivize providers to prescribe treatments that will meet patients’ expectations, such as antibiotics. It is vital for providers to ensure that quality is not sacrificed for convenience in this fast-paced setting. Given the global threat of rising antibiotic resistance, rigorous antibiotic stewardship is becoming increasingly important. This statistically significant 20% reduction in antibiotic prescribing for acute rhinosinusitis shows the value of a simple educational intervention for providers coupled with an algorithmic CDS tool. This is a promising approach that could be easily implemented in urgent care and other ambulatory settings with a similar method. Future directions could include patient education about viral illnesses and adjustment of patient expectations.
References
- Rosenfeld RM, Piccirillo JF, Chandrasekhar SS et al. Clinical practice guideline (update): Adult sinusitis. Otolaryngology–Head and Neck Surgery, 2015;152(2 Suppl), S1-S39.
- Palms DL, Hicks LA, Bartoces M, et al. Comparison of antibiotic prescribing in retail clinics, urgent care centers, emergency departments, and traditional ambulatory care settings in the United States. JAMA Intern Med. 2018. 178(9):1267-1269.
- Chow AW, Benninger MS, Brook I, et al. IDSA clinical practice guideline for acute bacterial rhinosinusitis in children and adults. Clin Infect Dis. 2012. 54(8):e72-e112.
- Centers for Disease Control and Prevention. Antibiotic resistance threats in the United States: 2019.Availablet at: https://www.cdc.gov/drugresistance/pdf/threats-report/2019-ar-threats-report-508.pdf. Accessed Ocober 5, 2020.
- Centers for Disease Control and Prevention. Antibiotic use in the United States, 2018: Progress and opportunities. Available at: https://www.cdc.gov/antibiotic-use/stewardship-report/pdf/stewardship-report-2018-508.pdf. Accessed October 5, 2020.
- Pulia M, Redwood R, May L. Antimicrobial stewardship in the emergency department. Emerg Med Clin North Am. 2018;36(4):853-872.
- Deming WE. Out of the Crisis. Cambridge, MA: The MIT Press. 2018.
Mindy L. Seybold, DNP, ARNP, FNP-C is a primary care Nurse Practitioner in Family Practice at Kaiser Permanente in Longview, WA. Holly Faber Tse, MD is a board-certified internist and pediatrician and the Medical Director of Medical Home at Legacy Health in Portland, OR.
