Published on
Urgent message: An onsite lab can generate significant revenue for your practice. Lab expert Tim Dumas shows how.
TIM DUMAS, MLT,CLS
Introduction
I have been a lab tech for almost 35 years and serve as advisor to 45 physician office labs around the country. I have seen many changes in that time, most for the better. Thirty—even 20—years ago, a stat CBC with differential was a 15-minute-procedure and required a skilled lab tech to get it right. Today my office labs perform CBC/diffs with an average turn-around-time of five minutes. These labs offer better accuracy and reproducibility and only require a single smart person with the right attitude and a high school diploma to run.
Most advances in laboratory medicine in the past decade have come in the form of computer technology. Blood chemistry analyzers now have the ability to monitor quality control internally. They can notify the operator when there is a problem and when not to accept a result. “Waived” or “kit” tests are made so that it is very difficult to perform a test incorrectly.
As I researched up-to-date statistics relating to lab regulations, registration, lab test usage, or some kind of graph that shows what other urgent cares are doing regarding lab procedures to make my case for onsite labs, I realized that it’s all fluff. What other centers are doing may or may not work for you. So let’s focus on the facts about lab tests—facts that should be well-known but often aren’t. Afterward, you can decide for yourself whether in-house testing is right for your practice.
Why Run Your Own Lab Tests?
The function of lab tests in the clinical setting has always been to assist in the diagnosis of disease and monitor the progress of treatment. Lab tests are one set of tools in the medical tool box that is tough to do without. The quicker a provider can get the result of a lab test, the quicker that provider can make a diagnosis and start treatment—and not waste money and time on unnecessary treatments because the treatment that is offered is based on an accurate lab result when that result is actually needed: not in a day or a week but in minutes. I can think of no better usable setting for the rapid lab results than an urgent care center.
Benefits of In-house Testing
An onsite lab offers numerous benefits to urgent cares:
- You gain the ability to diagnose and treat a patient’s problem while the patient is still in the office.
- The patient starts treatment quicker or can be referred quicker when necessary.
- Your staff does not have to spend time tracking down patient to give her the lab results and/or treatment.
- Many insurance companies now see the benefit of onsite labs to their members. If doctors can provide one-stop services (ie, onsite lab, in-office dispensing), this saves patients from having to make multiple trips to get treatment.
- How many times has a reference lab lost your blood sample and your patient had to be redrawn? Or the wrong test was ordered and/or performed? With an onsite lab, you gain control over specimens.
- If your lab tech is handling the send-out processing to a reference lab, then that individual is, in effect, working for the reference lab, because it is the reference lab that is getting paid.
- The same amount of time spent processing a sendout could have been used to run the test in-house, with your practice retaining the revenue.
What Does It Take to Get an Onsite Lab?
Regulation and oversight are the first considerations in getting a lab into your center. The Clinical Laboratory Improvement Amendments (CLIA; www.cms.gov/CLIA) is the federal regulatory body that oversees all laboratory testing. The purpose of CLIA is to ensure accurate and reliable lab testing for the benefit of your patients. CLIA is controlled by Centers for Medicare & Medicaid Services (CMS).
A CLIA certificate/number is required for billing. Regulatory oversight can also be achieved by several other companies, but they report to CLIA. These are:
- The Commission on Office Laboratory Accreditation (COLA; cola.org), which was established to help physician office labs comply with CLIA regulations. COLA oversight is the most cost-effective way to be compliant.
- The College of American Pathologists (CAP) laboratory accreditation program. The oldest regulatory agency, CAP is better suited to large labs performing highly complex testing.
- The Joint Commission, which is usually used for larger institutions.
CLIA is both the certificate of accreditation and the oversight agency. There is a fee for the inspections; it is paid to whichever agency you choose for oversight.
Applying for a CLIA certificate
To earn accreditation, your lab will need a designated lab director. This position can be filled by a physician with demonstrable lab experience. The best way to meet this regulation is to take the lab director’s course through COLA. It can be completed online or you may want to attend one of COLA’s semi-annual three-day symposia.
For the urgent care setting, two levels of testing certificates are important:
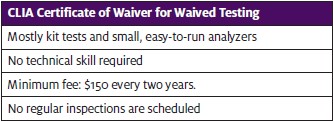
Waived testing is the most basic level of testing. Under CLIA law, waived tests are those tests determined by the Centers for Disease Control and Prevention (CDC) or the Food and Drug Administration (FDA) to be so simple that there is little risk of error. Most offices are already performing waived tests. They include kit tests such as rapid strep, influenza, mono, urine dip stick, and fecal occult blood. Currently, 40 tests have been approved for certificate of waiver status. There are a few chemistries and some immunoassays that can be performed on a waived basis. However, these tests are more expensive to run on a waived analyzer than on a non-waived analyzer. More on that later.
A waived test should be clearly marked “WAIVED.” The package insert provides instructions for the procedure. It indicates the quality controls needed. And it gives details for storage and test limitations. Unfortunately, most clinics don’t read or follow these instructions and that’s where they get into trouble.

Non-waived is the next level of laboratory testing. These tests take a few more steps to perform and include CBCs some chemi stries, and some immuno assays. Running tests on a non-waived analyzer can provide more accurate results as well as being less costly per test. With the right system, this can generate more revenue for the practice. There are a handful of analyzers to choose from and it becomes a job to sort them all out. This is where a distributor’s sales rep or a laboratory consultant can be most beneficial.
How do you know if non-waived testing is right for your center? There are breakeven points for running certain tests. For example, running three to five CBCs tests per day will generally pay for a non-waived analyzer, as would running five or more comprehensive metabolic panels (CMPs) or basic metabolic panels (BMPs) for blood chemistry per day.
You can enroll your laboratory in the CLIA program to get your certificate and number by completing an application (Form CMS-116) available online on the CLIA website. If you are currently running waived testing and would like to add CBCs or any other non-waived test to your lab’s capabilities, you would need to submit this application with your current CLIA information and ask to be upgraded to non-waived status.
Making Your Lab Profitable
I hear from many doctors and office managers that their labs are a drain on the practice. My response is usually the same: “You’re running your lab incorrectly.” Over the years, I have been called in to fix many labs that were losing money or costing too much. A lab is a business and should be run like one. Consider it a business within your business. In fact, some of my physician offices say that the lab brings in as much revenue as office visits.
I have discovered the main source of error to be overhead. Clinics often spend more money to run a test than it returns in reimbursements. I’m amazed at how often I ask for financial information about a lab and the manager doesn’t really know the cost per test or the reimbursement. She just knows the lab is costing money and therefore assumes it is losing money. A business must first know projected revenue before it can start, so let’s take a look.
Financial Feasibility for a Waived Lab
Projecting waived lab test revenue is fairly simple. You need to know this information:
- Cost per reportable. This means the cost per test plus any extra items not included with the kit (eg, swabs, tubes, controls, incubators, etc.). Take the rapid strep test. A kit of 25 tests costs $62.50—or $2.50 per test. The kit includes controls and all the necessary materials to run the test. There are no extras. So the cost per reportable is $2.50.
- Reimbursement. This varies from state to state and from one insurer to another. I have found that a good guide is the “CLIA minimum reimbursement fee schedule” (see How Much Does CLIA Reimburse Per Test? on page 20). Your office can calculate your own average. Many urgent care centers operate on a cash basis. Establish what your set fee for a procedure will be and collect it. For example, the rapid strep Medicare minimum reimbursement is $16.01. The cash price you charge might be $25.
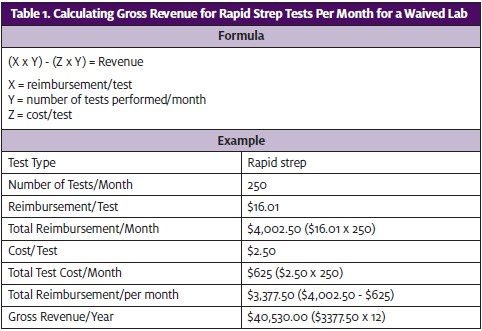
- Number of tests performed. I usually count per month. Volume varies based on time of year. Use this information to determine inventory. Be sure to check the expiration dates on kits and don’t order too many. In the urgent care setting, it is sometimes difficult to predict volume of tests before you open a kit. If this is your situation, aim on the low side. You can always order more kits and receive them the next day. Once you have the ability to average the number of tests per month (eg, 250 rapid strep tests per month), ordering a realistic number gets easier, especially if you use a simple formula in an Excel spreadsheet (Table 1).
Isn’t there more to costs than the cost per test? What about CLIA fees, the cost of a tech’s time to run the tests, regulatory costs, and the cost of lab space?
- This is for a waived lab, so no lab tech is needed. If your volume is high, I recommend that a dedicated staff member run all labs. It’s much more efficient than having the nurses try to do it all. The revenue generated pays for a dedicated individual’s time.
- For a waived lab, the cost of a two-year CLIA/COLA certificate is minimal: $150. The space requirement is also minimal: a countertop and shelves or cabinets for storage.
- Don’t bother adding in tech time, rent, insurance, and other common facility costs in an attempt to calculate net revenue to the penny. You have already have the space, pay the rent, and pay for insurance, so these costs are not really costs from adding a lab.
Financial Feasibility for a Non-waived Lab
Now let’s look at the costs and revenues for a non-waived lab. The most useful test for a non-waived lab in the urgent care setting is the CBC, so let’s use that as an example (Table 2).
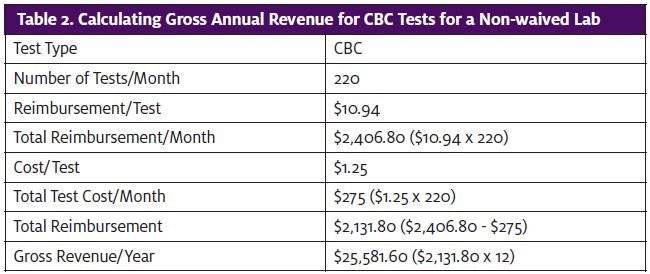
Reimbursement is based on the Medicare minimum ($10.94/test) and will not change much. The only real control we have to increase revenue is to decrease the cost per test. The cost here of $1.25 per test is an average for CBC testing. Cost per test will decrease with higher volume of testing.
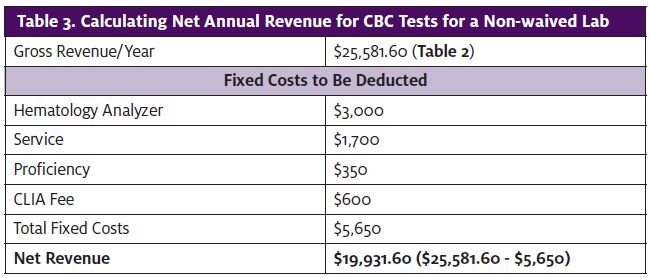
From the gross revenue per year—$25,581.60—subtract your fixed costs (Table 3). I call these “fixed” because no matter how many tests you run, they remain the same. These are the average fixed costs per year:
- Hematology analyzer: $3,000 (estimate: $15,000 leased over five years)
- Service contract: $1,700
- Proficiency testing: $350
- CLIA fee for non-waived testing: approximately $600 per year
Deduct your fixed costs from your gross revenue to calculate your net revenue ($19,931.60 in this example).
Could your urgent care use an extra $20,000 per year in net revenue? Even more important from the standpoint of clinical quality, how valuable is a stat CBC? It would enable you, for example, to diagnose flu vs an infection—with no need to write a prescription or call the patient back when the test result arrives. Most providers I speak to about CBCs say that they would order the tests more often if they were available stat. A sendout CBC result is not much help. Here is where you can factor in the savings from not having to call the patient back or open that chart again to review and comment on the results. It is just better medicine.
While this example is not the whole story, it can be used as a template to determine the feasibility of performing a given test in-house. If you already perform in-house testing but have not calculated revenue, plugging your numbers into this example can help you determine it.
What can be a hidden cost not factored into the example is how well your billing personnel are capturing lab-generated revenue. This is something you really ought to monitor. If you know the projected revenue, then you can compare it to the actual revenue being brought in. Any inconsistencies can then be discovered and corrected.
Other Non-waived Tests
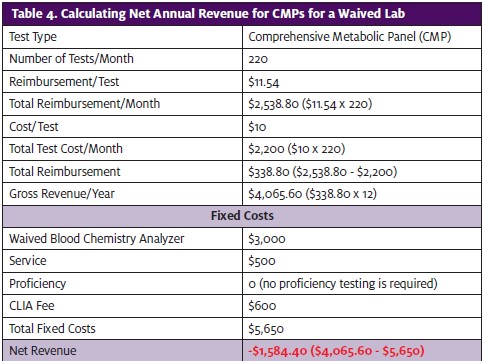
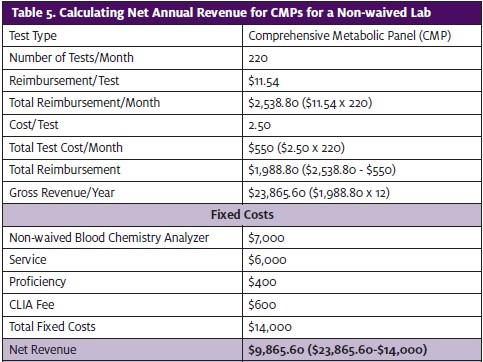
Blood chemistry tests are different from CBCs because there are no waived hematology analyzers (ie, blood cell counters) available. In contrast, blood chemistry analyzers—analyzers that perform CMPs, BMPs, and electrolyte panels (lytes)—are available in both waived and non-waived platforms. Waived chemistry analyzers are more expensive per test/profile and therefore don’t allow for much profit. In fact, this is where most urgent cares lose money on labs (Table 4 and Table 5). Waived test analyzers do not require proficiency testing and the service contract is usually much less expensive compared to non-waived bench-top analyzers.
The high cost per test when performing more complex tests like CMPs in a waived lab vs a non-waived lab ($10 vs $2.50, respectively) makes the profit margin either very small or a negative number for a waived analyzer, and that assumes you collect the full amount you bill.
A better alternative for more complex tests is a non-waived bench-top chemistry analyzer. A nonwaived analyzer can perform multiple tests on multiple patients at one time, perform a larger menu of tests, is usually more accurate, and is less expensive per test than a waived analyzer. On average, a nonwaived bench-top analyzer can perform CMPs for less than $3.
Which specific analyzers to consider is beyond the scope of this article. But comparison-shop and ask lots of questions before making a buying decision.
Challenges to Getting Paid
Even when they master everything just discussed, most physician practices are not getting paid for lab testing by insurers for the simple reason that they haven’t asked to be paid. Like most things with insurers, it’s all about the negotiating.
The insurance company may say they require the office to send the test out to a reference lab. That’s because they have made a deal with that lab for a decreased fee for the tests. It’s good business for the insurer, but this “deal” comes at a cost to the patient and to your urgent care. If the labs could be performed in-house for the same fee as the reference lab, then the practice should get paid.
That’s the basic idea for negotiating with insurers.
You may be surprised at the outcome of just asking to get paid for in-house testing. Don’t assume the worst. Doctors and staff must first understand the benefits of in-house testing. This understanding and belief will enable you to convince an insurer that they can save time, money, and even lives by offering onsite testing. You have the right to provide your patients (their customers) with the high level of quality and convenience that in-house testing can deliver. The importance of in-house testing can be summed up this way:
Negotiating With Insurers
In the past, physicians have assumed that contracts with the insurers were not negotiable. They would not complain for fear that an insurer might not let their clients be a practice’s patients. Insurers rely on that attitude. Physicians must realize that they provide the service that patients seek. It’s a lot easier to find an insurance company than to find a doctor you trust and rely on to make you and your family feel better and healthier. Most patients will pay out of pocket for medical care they can trust. If need be, they will search for insurance that a clinic will accept.
Insurance companies are composed of businesspeople; negotiating is what they do. Don’t give in. Commit to do business. If you aren’t confident about your business abilities, hire a skilled negotiator who is.
When you begin negotiating, make it clear that you are not just asking for money. You must explain the benefits of the testing. Faster results and quicker treatment lead to faster recovery. This is the essence and purpose of both your position and the insurer’s. People today are more educated about their own health than ever before. The Internet has empowered them with information so they know which tests and in some cases even which treatment they should receive. Like it or not, that’s healthcare in the 21st century.
A strong negotiating point is the issue of liability brought on when a patient is misdiagnosed or diagnosed too late due to unavailable or delayed lab reports. Think of the complaints about over-prescribing medications.
Faster Results (Saves Time) = Faster Treatment (Saves Money) = Faster Recovery (Saves Lives)
What’s in it for an insurer? Marketing clout. You are asking to be paid to do a better job of caring for your patients (aka “their clients”). The same Internet that allows patients to discover information about diseases and treatments also allows them to find a provider who has the medical expertise they need—and insurance that supports that provider. It’s good for an insurer to be able to advertise that their network of providers offers in-house testing.
Problems With Billing
The other area to watch for in getting paid for testing is your billing department. In 70% of the labs I have worked with to correct their revenue shortfalls, the problems were coming from the billing department. They include:
- Incorrect CPT codes
- Missing or mismatched ICD-9 codes.
- Tests not billed for at all (too much work to match the codes, tests not checked off on claim forms as performed and reimbursable expenses, etc.)
- Denials of payment not resubmitted
One medical practice failed to collect over $150,000 in lab revenue due to billing errors.
Shopping for Lab Kits and Analyzers
Once you have chosen the test that would be beneficial to your practice, it’s time to buy the equipment you will need. The first place to check is your medical supply vendor. Ask your favorite medical sales rep what he or she offers in that line of testing. And then—very important—find another vendor and pose the same question.
Comparison- shopping is the key to a profitable lab. Let the product sales reps do their job of educating you about the pros and cons of certain test kits and then use a team approach in your urgent care to choose the best ones for your situation. Several distributors may offer the same product. Shop for the best price; the manufacturers are generally brand names offered by all distributors.
One office I worked with discovered they were paying $17 per flu test. Medicare reimburses $16.01. Oops. After shopping around they found a similar kit, which worked just as well, for $9 per test.
Don’t sell yourself short. A difference of $.25 per test adds up over time. Take the rapid strep test used as an example in Table 1. The cost per test is $2.50. If it were just $.25 more expensive, and you were performing 250 tests per month, that cost would balloon to an extra $750 annually ($.25 x 250 x 12).
Concerns About Onsite Labs
Here are some concerns about onsite labs I have encountered, with some perspective:
Concern
Federal regulations are time-consuming and difficult to comply with.
Perspective
The regulations are intended to assure accurate results from your lab. The cost is minimal compared to the benefit and revenue generated. Your staff is responsible for testing and quality control. An ROI analysis can determine whether your staff time is worth the benefit and revenue generated by in-house testing.
Concern
Where will we store all those test kits and reagents?
Perspective
Kits are small boxes, usually shoebox-size or smaller. They contain 25-100 tests per box. Your lab will not usually need more than one or two boxes at a time.
Concern
It’s too expensive to invest in a hematology analyzer.
Perspective
That’s why you need to perform an ROI calculation before you purchase equipment. If you are not sure about the financial/business end of establishing a lab in your urgent care, a consultant who knows the ropes can help. Most of the time this will be well worth the investment.
Concern
We are concerned about the longevity of point-of-care testing (POCT). Some offices are concerned that one day Medicare will not pay for POCT.
Perspective
POCT is here to stay. POCT has been established as good medical practice. Insurers may shift the cost to the patient, but the tests are needed, someone will pay to have them performed, and someone will be paid to do them. Why not you?
Tim Dumas, a Clinical Laboratory Scientist for nearly 35 years, serves as an advisor to 45 physician office labs across the US. His website is www.timdumas.com. He can be reached at (919) 325-2888 or [email protected].


