Published on
Differential Diagnosis
- Rocky Mountain spotted fever
- Leukocytoclastic vasculitis (LCV)
- Sjögren syndrome
- Acute meningococcemia
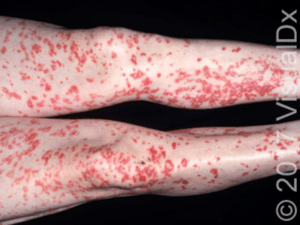
Diagnosis
This patient was diagnosed with leukocytoclastic vasculitis (LCV), a small-vessel vasculitis that predominantly affects postcapillary venules in the dermis.
Learnings/What to Look for
- The clinical hallmark of LCV is palpable purpura; purpuric papules erupt symmetrically on the shins 7-10 days after an inciting factor. Other parts of the lower extremities, including the thighs and dorsal feet, may be involved. Less frequently, the buttocks, upper extremities, and abdomen are involved.
- Purpuric macules seen initially may give way to palpable purpura. In more advanced cases, bullae and ulcers may be seen.
- While the majority of cases are asymptomatic, LCV can be associated with pruritus, pain, or burning.
- Inciting factors may include medications (especially antibiotics, NSAIDs, and diuretics), pathogens (hepatitis viruses, HIV, Epstein-Barr, streptococci), malignancy, inflammatory bowel disease, or connective tissue disease.
- It is important to differentiate skin-limited LCV from systemic vasculitis. The latter should be suspected if fever, myalgias, malaise, lymphadenopathy, abdominal pain, melena, hematochezia, diarrhea, hematuria, lower extremity swelling, or paresthesias are noted.
Pearls for Urgent Care Management and Considerations for Transfer
- Skin-limited LCV does not require treatment beyond rest, elevation of the legs, ice packs, and removal of the inciting factor.
- Treatment of systemic vasculitis may require NSAIDs, oral steroids (prednisone or methylprednisolone), intravenous corticosteroids, or colchicine, depending on severity.
- Inpatient treatment may be required for patients with severe systemic vasculitis syndromes or organ dysfunction.
A 42-Year-Old Male with a New Symmetrical Rash on His Legs
1 2
