Published on
In Bouncebacks, we provide the documentation of an actual patient encounter, discuss patient safety and risk-management principles, and then reveal the patient’s bounceback diagnosis. This case is from the book Bouncebacks! Pediatrics, by Michael B. Weinstock, Kevin M. Klauer, Madeline Matar Joseph, and Gregory L. Henry, and is available at www.anadem.com and www.amazon.com.
Introduction
A 16-week-old infant was brought by her parents to the emergency department (ED) of a children’s hospital. Note: The following is the actual documentation by the provider.
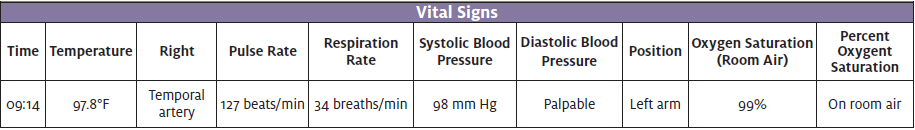
Visit to the Emergency Department
Chief complaint: Bloody vomitus
Triage (at 09:02)
Mother states, “Blood in spit-up. Babysitter put paper towel in baby’s mouth and it came out with blood. Looks like she is gagging.” Parents brought patient in with paper towel that has blood on it that patient’s mother states came from patient’s mouth. Patient does have pink-tinged vomit on the collar of her clothing.
Past Medical History
Allergies: No known allergies
Meds: Axid
Immunizations: The infant’s/child’s immunizations are current
Past medical history: GERD [gastroesophageal reflux disease]
Surgical history: Nothing significant
History of Present Illness (Documented at 13:51)
This child apparently vomited a pinkish fluid today that may have been blood. Child has no significant medical or surgical history except being approximately 10 weeks premature at birth. There is a history of reflux. There have been no black or tarry stools noted at home. Has been no diarrhea or nausea or vomiting. No fever, chills, nausea, blood in stools, constipation.
Physical Examination (Documented at 13:52)
Examination: Exam was unremarkable, with the following notation:
Oral: Posterior pharynx is pink without exudates, erythema. There are two areas that may be a source of bleeding—one is the frenula, and the other is a small area on the mucosa that may have leaked a small amount of blood.
Orders (at 10:44): CBC [complete blood cell count]. [Patient’s] parents refused blood draw after first attempt was unsuccessful.
Progress Notes (Documented at 13:53)
We attempted a blood draw for a CBC [count]. The parents at this time feel the child is okay and that the lesions in the mouth are the source of the bleeding and want to follow up with her pediatrician and are not interested in any more attempts at a blood draw. I let them go at this time.
Diagnosis (at 10:42): GI [gastrointestinal] bleed
Disposition: The patient was discharged to home, carried by parent [and] accompanied by parent/guardian. Aftercare instructions for gastritis/heartburn/peptic ulcer. [Patient] released from ED [emergency department] at 10:52.
The Errors: Risk Management and Patient Safety Issues
Error #1: Nonspecific History
Discussion: This pediatric patient requires a specific neonatal pediatric history.
- Pregnancy history: Was the pregnancy uncomplicated, or was there gestational diabetes, preeclampsia, preterm labor, or other issues?
- Delivery history: Was the patient full term or an early delivery? Any complications with the delivery? Birth weight and current weight?
- Medical history: Any health issues? Any surgeries? Immunizations up to date?
- Social history: Breast-fed or bottle-fed? Smokers in the house? Who are the primary caregivers?
If you commit to having these data on every chart, for patients younger than age 1 year, you will unearth information that was not volunteered, will be prompted to consider important issues and diagnoses, and will generate a more thorough and defensible medical record.
Teaching point: Casting a wide net will often yield important information.
Error #2: Presumption of No Significant Medical History
Discussion: “Child has no significant medical or surgical history except being approximately 10 weeks premature at birth.” This is a significant piece of information, which mandates follow-up questions:
- Why was the patient premature?
- Was the patient on a ventilator and how long?
- How is the family/caregivers responding to the stressors of caring for a premature infant?
As medical providers, we must understand when unexpected data requires additional investigation.
Teaching point: Concerning data often requires further investigation.
Error #3: Two Potential Bleeding Sites in the Mouth Not Investigated
Discussion: The physical examination findings include the possibility that the frenulum and another small mucosal region might be the source of bleeding. If that is true, there would have to be some source of oral trauma. Breast-feeding or bottle-feeding should not cause a mucosal injury. There was no mention of potential trauma or fall in the triage note, HPI, or progress notes.
Teaching point: In nonverbal pediatric patients, it is important to ensure that the mechanism explains the injury.
Error #4: Incomplete Hematologic Evaluation
Discussion: Whether a CBC count was warranted is debatable. However, once ordered, the hematologic evaluation should be completed. The CBC count will check for leukemia, anemia, and thrombocytopenia. If you are going down this pathway, consider coagulation studies to rule out bleeding disorders such as hemophilia. Questions regarding excessive maternal bleeding associated with delivery and requiring blood transfusion, bruises, or blood in the urine or stool will further clarify the medical history.
Teaching point: If you initiate an investigation, finish the thought process.
Error #5: Committing to a Gastrointestinal Source of Bleeding as a Diagnosis
Discussion: What do we really know about the source of the blood? Blood from the patient’s mouth is shown on a paper towel and on the collar of the clothing. The blood could actually be from the nose, mouth, lungs, or stomach, or even from the mother’s nipple. HPI notes specify “no black or tarry stools,” but a rectal examination for occult blood or trauma was not done. It is unlikely that reflux would cause GI bleeding in a neonate. Patients and physicians would all like to have a pinpoint diagnosis in the ED setting; however, that is not always possible. The source of bleeding is GI remains unknown.
Teaching point: Understand the limitations of an evaluation and the ability to make a definitive diagnosis.
Error #6: Lack of a Clear, Unified Story in the Chart
Discussion: A chart narrative must flow from triage to diagnosis. In any medical encounter, the triage and HPI dictates the examination, followed by the appropriate work-up, then medical decision-making, diagnosis, and disposition. In this instance, the triage and HPI concentrate on potential vomiting as the source of blood. The physical examination notes point to potential bleeding from the frenulum and another mucosal region, as does the progress note. The diagnosis then goes back to “GI bleeding,” with aftercare instructions for “gastritis/heartburn/peptic ulcer.”
Teaching point: This chart should tell a single story from beginning to the end.
The Bounceback
The infant was brought back 12 days later to the ED of the children’s hospital.
- Chief complaint: Eyes rolled back
- Vital signs:
- Afebrile
- Pulse rate, 148 beats/min
- Respirations, 40 breaths/min
- Blood pressure, 108/53 mm Hg
- Triage: Put baby down for nap—baby rolled from back to belly and was unresponsive
- Examination:
- General: Consolable, alert
- Head: Atraumatic
- Ears: No hemotympanum
- Respiratory: No respiratory distress
- Cardiology: RRR [regular rate and rhythm] without murmur
- Abdomen: Nontender
- Extremities: Normal
- Neurology: No sensory or motor deficit
- Results
- CT [computed tomography] results: New and old subdural hematomas
- XR [x-ray] results: Negative left wrist XR
- MDM [medical decision-making]:
- Concern for abuse by PMD [private medical doctor], so sent to ED for evaluation. Abuse concern due to previous injuries at babysitter[’s home] that cannot be adequately explained.
- Diagnosis:
- Subdural hematoma, alleged physical abuse
Discussion
The Differential Diagnosis
In this case, the patient is a 16-week-old, born prematurely at 30 weeks’ gestation, and blood has been noted in the patient’s mouth. What is the etiology of this bleeding? A generic differential diagnosis may include the following:
- Trauma: force-feeding, drop, fall, abuse
- Environmental temperature or humidity (dry or cracked lips or oral mucosa)
- Bleeding dyscrasia caused by a low platelet count, hemophilia, or von Willebrand disease
- Neonatal leukemias or cancer
- Vitamin K deficiency bleeding of the newborn occurs in the first 2 weeks of life. Late deficiency bleeding may also occur, a some point between 2 and 12 weeks, in infants who are breast-fed (i.e., receiving no formula) or who have malabsorption due to diarrhea, intestinal bacterial overgrowth, hepatitis, cholestatic jaundice, celiac disease, or cystic fibrosis.1
- Vitamin C deficiency and an increased histamine level may occur with hyperemesis gravidarum, malnutrition, surgery, or infection, in the pregnant patient. Subdural hemorrhages have been diagnosed by antepartum ultrasonography. Barlow disease or infantile scurvy can be considered in cases with bruising, broken bones, and subdural hematoma.2
- Glutaric acidemia, a genetic disorder caused by a missing or decreased-function enzyme called glutaryl-CoA dehydrogenase, which breaks down certain amino acids, results in acidemia and causes a myriad of symptoms, including cerebral edema and cerebral hemorrhage.3 It is clinically important to be aware that this genetic disorder does not predispose the patient to fractures.
- Hemorrhagic pulmonary edema from suffocation or strangulation, with bloody fluid in the mouth
- Blood in the mouth of an infant being breast-fed is often from cracks in the nipples of the mother, although the findings in this case were not consistent with that situation.
Subdural Hematoma in Children
Though head injuries in children may be caused by accidental trauma, inflicted head trauma is the most common cause of death in children who are younger than 1 year. Of patients with head trauma, 45% of those in whom it is inflicted have permanent neurologic damage, whereas only 5% of those in whom it is accidental have damage.
In a prospective, longitudinal study by Ewing-Cobbs et al4 of children including newborns and children up to age 6 years who were hospitalized for traumatic brain injury (TBI), a comparison of inflicted TBI and accidental TBI showed the following:
- Of patients with inflicted TBI,70% were younger than 1 year of age.
- Of patients with inflicted TBI, 50% had no reported history of trauma. Of those with accidental TBI, all had a reported history of trauma.
- Subdural hematomas occur in greater frequency with inflicted TBI (80%) than with accidental TBI (45%).
- Epidural hematomas (20%) and shear injuries (20%) were seen only in the group with accidental TBI.
- Retinal hemorrhages occurred in 70% of patients with inflicted TBI but in none with accidental TBI.
- Subsequent seizures occurred more often in patients with inflicted TBI (65%) than in those with accidental TBI (20%).
- Mental deficiency was occurred more often in the patients with inflicted TBI (45%) than in those with accidental TBI (5%).
- There were no differences in motor skills scores in the two groups.
Risk Factors for Child Abuse
The World Health Organization has published a comprehensive list of risk factors for child maltreatment.5 This is a condensed list:
- Risk factors for parents or caregivers: difficulty bonding with the child, maltreatment of the parent or caregiver as a child, lack of awareness of typical child development or unrealistic developmental expectations, lack of parenting skills, disciplining of child with physical punishment, presence of physical/mental/cognitive health issues, lack of self-control, alcohol and or drug abuse, criminal activity, social isolation
- Risk factors for the child: unwanted baby, has high needs (premature, disabled, chronic illness), crying and difficult to comfort, mental-health issues, part of a birth of multiples, many siblings
- Relationship factors: lack of parent–child bonding, family breakdown, violence in the family, disrespect in the family, isolation in the community, lack of support network
- Community factors: violence, gender and social inequality, lack of housing and support services, unemployment, poverty, and alcohol and/or drug abuse
- Societal factors: social, economic, health, and education policies that cause a poor standard of living or socioeconomic inequality or instability, and social or cultural norms of violence toward others
Work-Up in Patients with Suspected Child Abuse
A multidisciplinary approach should be used when investigating alleged abuse, to include some or all of the following:
- Pediatrician
- Pediatric neurosurgeon, for management of any intracranial injury
- Pediatric neurologist, for examination and optimization of outcomes
- Orthopedist, for fracture management
- Ophthalmology, for the complete eye examination and confirmation of retinal hemorrhages
- Forensic pathologist, in the case of death, for classification of the timing and mechanism of injury
- Social services, including child protective services
- Police
Laboratory studies may include a CBC count, prothrombin time, partial thromboplastin time, bleeding time, vitamin K and vitamin C levels, and histamine levels.
Radiographic Studies
- Noncontrast brain CT is the initial screen for subdural hematoma, subarachnoid hemorrhage, cerebral contusion, cerebral edema, infarction, and white matter changes.
- Diffusion-weighted magnetic resonance imaging may distinguish between acute and chronic cerebral infarction.
- An initial skeletal survey will pinpoint occult fractures. Rib fractures and long bone fractures are more prevalent in children with inflicted traumatic injuries, with rib fractures having the highest probability (70%) for abuse as a cause. There is a high correlation between multiple fractures and abuse. Eighty percent of inflicted fractures are seen in children who are younger than 18 months of age.
- A bone scan will identify subperiosteal hemorrhage and early fracture healing.
- If a genetic bone disease such as osteogenesis imperfecta or mineralization defect is suspected, then screens for calcium, magnesium, phosphorus, and vitamin D levels are indicated.
Incidence of Child Abuse
Child maltreatment or abuse is underreported because it often is not considered, recognized, or detected. Child maltreatment is divided into four categories:
- Neglect
- Physical abuse
- Emotional abuse
- Sexual abuse
Neglect is the most common child maltreatment, with physical abuse being the second most common. Physical abuse affects all cultures and socioeconomic groups, with an incidence that is similar for male and for female children. This risk of abuse increases with age, but fatal and serious injuries are most common in children younger than 2 years.6,7
Mandatory Reporting of Child Abuse
Physician, nurses, and health-care workers are mandatory reporters of suspected child abuse and neglect, as are school professionals, social workers, mental-health professionals, childcare providers, medical examiners and coroners, and law-enforcement officers. The exact requirements for mandatory reporting vary from state to state. A report must be made if the reporter “suspects or has a reason to believe that a child has been abused or neglected” or “has knowledge of, or observes a child be subjected to, conditions that should reasonably result in harm to the child.”8 The report of child abuse or neglect can be made to child protective services or to law-enforcement agencies. Many states have a telephone hotline or internet mechanism for reporting.
A report made in good faith means that the reporter had actual knowledge or reason to believe that the child was subjected to abuse or neglect. There is immunity, both for mandatory and voluntary reports of child abuse or neglect, when made in good faith.9 There are penalties for the failure to report child abuse or neglect, including felony charges and state charges, the latter of which vary and include misdemeanor charges, monetary fines, jail terms, or civil liability for any subsequent damages.
Conclusion
Abuse does escalate. Therefore, it is imperative to make the diagnosis early (bleeding gums in this case), before the infant sustains a more serious injury or dies.
References
- American Academy of Pediatrics Committee on Fetus and Newborn. Controversies concerning vitamin K and the newborn. Pediatrics. 2003;112(1 pt 1):191–192.
- Clemetson Capillary fragility as a cause of subdural hemorrhage in infants. Med Hypotheses Res. 2004;1:121–129.
- Morris AAM, Hoffmann GF, Naughten ER, et al. Glutaric aciduria and suspected child abuse. Arch Dis Child. 1999;80:404–405.
- Ewing-Cobbs L, Kramer L, Prasad M, et al. Neuroimaging, physical, and developmental findings after inflicted and noninflicted traumatic brain injury in young children. Pediatrics. 1998;102:300–307.
- World Health Organization and International Society for Prevention of Child Abuse and Neglect. Preventing child maltreatment: a guide to taking action and generating evidence. Geneva, Switzerland: World Health Organization; © 2006. Available from: http://apps.who.int/iris/bitstream/10665/43499/1/9241594365_eng.pdf
- Kellogg ND; American Academy of Pediatrics Committee on Child Abuse and Neglect. Evaluation of suspected child physical abuse. Pediatrics. 2007;119:1232–1241.
- Hussey JM, chang JJ, Kotch JB. Child maltreatment in the United States: prevalence, risk factors, and adolescent health consequences. Pediatrics. 2006;118:933–942.
- Child Welfare and Information Gateway. Mandatory reporters of child abuse and neglect. Washington DC: U.S. Department of Health and Human Services, Children’s Bureau. © 2016. Available from: https://www.childwelfare.gov/pubPDFs/manda.pdf
- Child Welfare and Information Gateway. Immunity for reporters of child abuse and neglect. Washington DC: U.S. Department of Health and Human Services, Children’s Bureau. © 2016. Available from: https://www.childwelfare.gov/pubPDFs/immunity.pdf

